 Back
BackUrinary System: Structure, Function, and Regulation
Study Guide - Smart Notes

Urinary System Overview
Functions of the Urinary System
The urinary system is essential for maintaining homeostasis by removing waste products and regulating the composition of blood. Its primary function is the excretion of metabolic wastes, excess ions, and water, which occurs in the kidneys. Other structures serve mainly for storage and transport of urine.
Excretion: Removal of ions (Na+, K+, Ca2+, Cl-, HPO42-, H+), water, nitrogenous wastes (NH3, urea), drugs, toxins, and hormones.
Hormone Production: Kidneys produce renin (regulates blood pressure), calcitriol (regulates Ca2+ levels), and erythropoietin (stimulates red blood cell production).
Gluconeogenesis: Kidneys can synthesize glucose from amino acids during starvation.
Anatomy of the Urinary System
Gross Anatomy
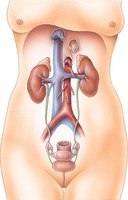
The urinary system consists of the kidneys, ureters, bladder, and urethra. The kidneys are retroperitoneal, meaning they are located behind the peritoneum. They are protected and held in place by the renal capsule, adipose capsule, and renal fascia.
Renal Capsule: Dense irregular connective tissue surrounding the kidney.
Adipose Capsule: Fatty layer that cushions and stabilizes the kidney.
Renal Fascia: Anchors the kidney to surrounding structures.
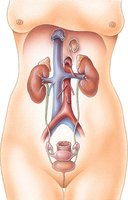
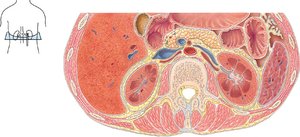
Internal Anatomy of the Kidney
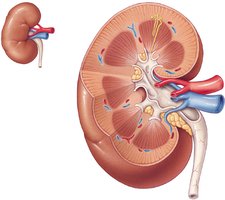
The kidney is divided into the renal cortex (outer region) and renal medulla (inner region, containing pyramids). The functional unit of the kidney is the nephron, with about 1 million nephrons per kidney.
Renal Cortex: Site of filtration and initial urine formation.
Renal Medulla: Contains renal pyramids, involved in urine concentration.
Nephron: Functional unit responsible for urine formation.
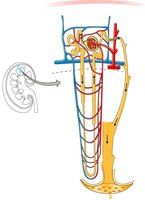
Nephron Anatomy
Structure of the Nephron
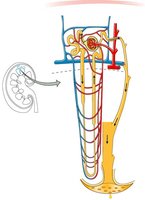
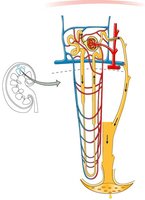
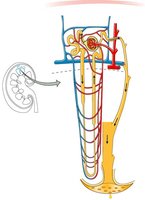
Each nephron consists of two main parts: the renal corpuscle and the renal tubule. The renal corpuscle includes the glomerulus and Bowman’s capsule, while the renal tubule is composed of the proximal convoluted tubule, loop of Henle, and distal convoluted tubule.
Renal Corpuscle: Site of filtration; includes glomerulus (capillary network) and Bowman’s capsule (surrounds glomerulus).
Renal Tubule: Proximal convoluted tubule, loop of Henle, distal convoluted tubule; all are one cell thick.
Types of Nephrons
There are two types of nephrons: cortical and juxtamedullary. Cortical nephrons are more common and have short loops of Henle, producing dilute urine. Juxtamedullary nephrons have long loops of Henle and produce concentrated urine.
Cortical Nephrons: 80–85% of nephrons; short loops; dilute urine.
Juxtamedullary Nephrons: Long loops; concentrated urine.
Nephron Function
Urine Formation Processes
Urine is formed by three main processes: filtration, reabsorption, and secretion. Filtration occurs in the renal corpuscle, reabsorption and secretion occur along the tubule.
Filtration: Plasma moves into the capsular space; 150–180 liters/day, most reabsorbed.
Reabsorption: Water and solutes are reclaimed from filtrate.
Secretion: Additional wastes are added to filtrate.
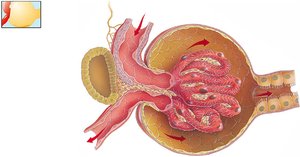
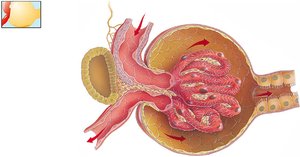
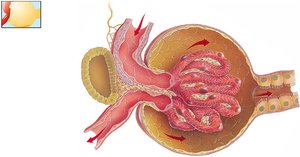
Glomerular Filtration
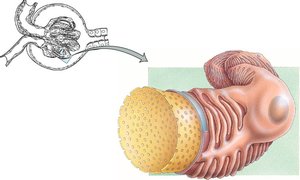
The glomerulus is designed to retain large proteins and blood cells while allowing water, glucose, vitamins, amino acids, small proteins, NH3, urea, and ions to pass. Filtration is facilitated by fenestrated capillaries, basal lamina, and podocytes.
Fenestrated Capillaries: Large pores allow passage of most substances except blood cells.
Basal Lamina: Retains large proteins.
Podocytes: Filtration slits form the final barrier.
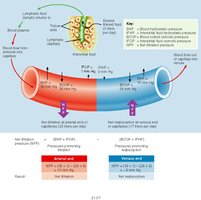
Net Filtration Pressure
Filtrate formation depends on the pressure gradient across the glomerulus. Three pressures affect filtration: glomerular blood hydrostatic pressure (GBHP), capsular hydrostatic pressure (CHP), and blood colloid osmotic pressure (BCOP).
Net Filtration Pressure (NFP):
Large volume of filtrate is due to the length and leakiness of glomerular capillaries and the small efferent vessel increasing glomerular blood pressure.
Regulation of Glomerular Filtration Rate (GFR)
GFR is regulated to remain constant despite changes in blood pressure. This is achieved by renal autoregulation, neural regulation, and hormonal regulation.
Renal Autoregulation:
Myogenic Mechanism: Smooth muscle contraction in afferent arteriole in response to stretching.
Tubuloglomerular Feedback: Juxtaglomerular apparatus constricts afferent arteriole as GFR increases.
Neural Regulation: Sympathetic stimulation causes vasoconstriction, reducing GFR.
Hormonal Regulation:
Angiotensin II: Vasoconstricts afferent/efferent arterioles, decreases GFR.
Atrial Natriuretic Peptide: Increases surface area, increases GFR.
Tubule Function: Reabsorption and Secretion
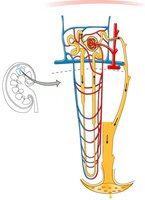
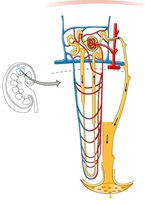
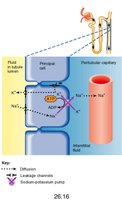
Most filtrate is reabsorbed along the nephron tubule. The proximal convoluted tubule (PCT) reabsorbs large amounts of water and solutes, mainly driven by Na+ movement. Glucose and amino acids are reabsorbed via Na+ symporters.
PCT: 65% of water and Na+ reabsorbed; 100% of glucose and amino acids; H+ secreted.
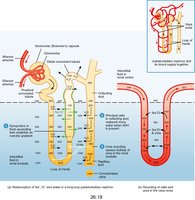
Loop of Henle: Descending limb reabsorbs water; ascending limb reabsorbs Na+, K+, Cl- (impermeable to water).
DCT and Collecting Duct: Na+ and Cl- reabsorbed; water reabsorption regulated by hormones; K+ may be secreted or reabsorbed.
Hormonal Regulation of Tubule Function
Renin-Angiotensin-Aldosterone System (RAAS)
Low blood pressure stimulates renin release, which converts angiotensinogen to angiotensin I, then II. Angiotensin II causes vasoconstriction and enhances Na+ and Cl- reabsorption, stimulating aldosterone secretion. Aldosterone increases Na+ and Cl- reabsorption in the DCT, increasing water reabsorption.
Antidiuretic Hormone (ADH)
ADH is released by the posterior pituitary in response to decreased blood pressure or volume. It increases water permeability in the collecting duct, promoting water reabsorption and concentrating urine.
Atrial Natriuretic Peptide (ANP)
ANP is secreted by the heart in response to increased blood pressure. It decreases ADH and aldosterone production, inhibits Na+ reabsorption in PCT and DCT, and decreases water reabsorption.
Other Components of the Urinary System
Ureters, Bladder, and Urethra
Urine is transported from the kidneys to the bladder via the ureters by gravity, hydrostatic pressure, and peristaltic contractions. The bladder is a muscular, extensible sac that can hold 700–800 ml of urine. The urethra is shorter in females (1.5 inches) than in males (6–8 inches).
Micturition Reflex and Incontinence
The micturition reflex is triggered by stretch receptors in the bladder, with the micturition center located in the sacral spinal cord. Conscious control is exerted via the external urethral sphincter. Incontinence is the lack of voluntary control over urination.
Diuretics and Dialysis
Diuretics decrease water reabsorption in the kidneys, increasing urination. Examples include alcohol (inhibits ADH), caffeine (inhibits Na+ reabsorption), and drugs for hypertension. Dialysis is used to remove waste products from the blood in cases of kidney failure, either via hemodialysis or peritoneal dialysis.
Salt Water and Urine Concentration
Human urine can only reach about 2% salt concentration, while seawater is about 3.5%. The kidneys cannot excrete enough salt to safely drink seawater.
Summary Table: Urinary System Functions
Function | Location | Key Points |
|---|---|---|
Excretion | Kidneys | Removes wastes, excess ions, water |
Hormone Production | Kidneys | Renin, Calcitriol, Erythropoietin |
Gluconeogenesis | Kidneys | Glucose synthesis during starvation |
Storage/Transport | Ureters, Bladder, Urethra | Urine storage and elimination |
Additional info: Academic context was added to clarify nephron structure, urine formation, and regulatory mechanisms. All included images directly reinforce anatomical and physiological explanations.
