 Back
BackUrinary System: Structure, Function, and Renal Filtration
Study Guide - Smart Notes

Urinary System Overview
Organs of the Urinary System
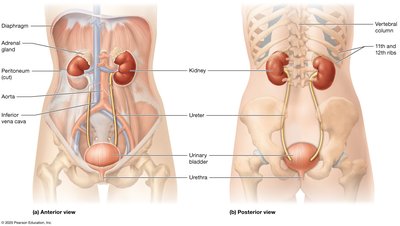
The urinary system is responsible for filtering blood, removing waste, and maintaining homeostasis of fluids, electrolytes, and acid-base balance. The main organs include the kidneys, ureters, urinary bladder, and urethra.
Kidneys: Filter blood and produce urine.
Ureters: Transport urine from kidneys to the bladder.
Urinary bladder: Stores urine until excretion.
Urethra: Conducts urine out of the body.
Functions of the Urinary System
Excretion of metabolic waste (especially nitrogenous wastes like urea).
Regulation of fluid, electrolyte, and acid-base balance.
Blood pressure regulation via fluid volume and hormone secretion.
Regulation of erythropoiesis (red blood cell production) through erythropoietin.
Metabolic functions such as gluconeogenesis and activation of vitamin D for calcium absorption.
Kidney Anatomy
External Anatomy of the Kidney
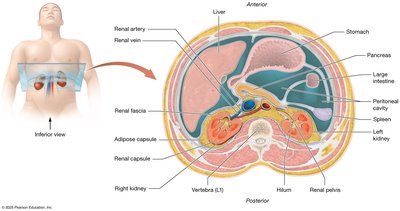
The kidneys are retroperitoneal organs protected and anchored by three connective tissue layers:
Renal fascia: Anchors the kidney to the peritoneum and posterior abdominal wall.
Adipose capsule: Cushions and stabilizes the kidney.
Renal capsule: Thin, tough layer protecting against infection and trauma.
Internal Anatomy of the Kidney
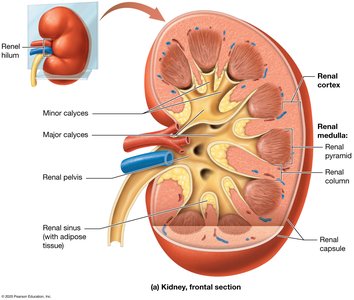
Renal cortex: The outer region containing renal corpuscles and parts of nephrons.
Renal medulla: Inner region with renal pyramids and columns.
Renal pyramids: Cone-shaped tissues that drain urine into minor calyces.
Renal pelvis: Central collecting region for urine before it enters the ureter.
Blood Supply of the Kidney
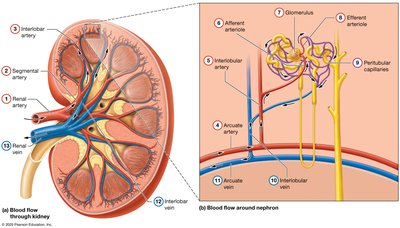
The kidneys receive blood from the renal arteries, which branch into smaller arteries and arterioles, eventually forming the glomerulus. Blood is filtered and then exits via the renal veins.
Renal artery → segmental arteries → interlobar arteries → arcuate arteries → interlobular arteries → afferent arteriole → glomerulus → efferent arteriole → peritubular capillaries/vasa recta → interlobular veins → arcuate veins → interlobar veins → renal vein
Nephron Structure and Function
Nephron Overview
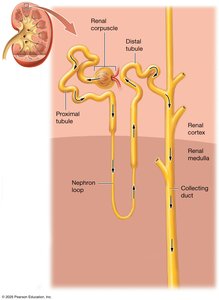
The nephron is the functional unit of the kidney, responsible for filtering blood and forming urine. Each nephron consists of a renal corpuscle and a renal tubule.
Renal corpuscle: Includes the glomerulus and glomerular (Bowman's) capsule; site of blood filtration.
Renal tubule: Modifies the filtrate through reabsorption and secretion. Segments include the proximal tubule, nephron loop (Loop of Henle), distal tubule, and collecting duct.
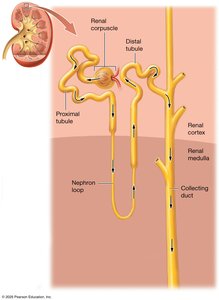
Renal Tubule Segments
Proximal tubule: Simple cuboidal epithelium with microvilli for reabsorption.
Nephron loop (Loop of Henle): Descending and ascending limbs; important for concentrating urine.
Distal tubule: Simple cuboidal epithelium with fewer microvilli; involved in selective reabsorption and secretion.
Collecting duct: Receives filtrate from multiple nephrons; final site for water reabsorption and urine concentration.
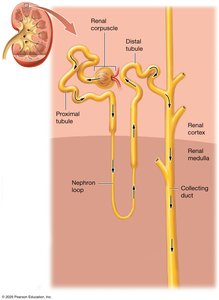
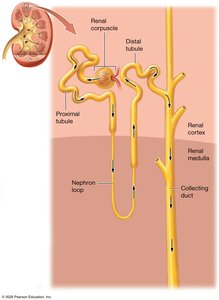
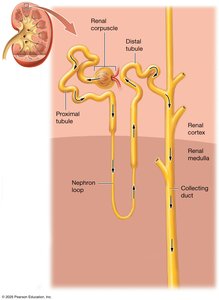
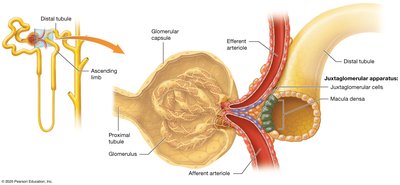
Juxtaglomerular Apparatus (JGA)
The JGA is a specialized structure where the distal tubule contacts the afferent and efferent arterioles. It regulates blood pressure and glomerular filtration rate (GFR).
Juxtaglomerular cells: Modified smooth muscle cells that secrete renin.
Macula densa: Distal tubule cells that sense sodium and chloride concentration in filtrate.
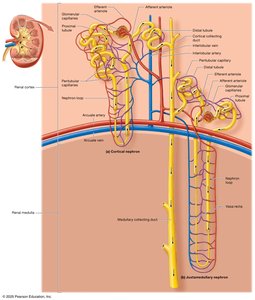
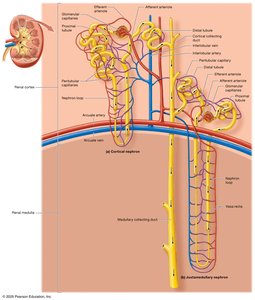
Types of Nephrons
Cortical nephrons: 80% of nephrons; located mainly in the cortex; short nephron loops; peritubular capillaries supply blood.
Juxtamedullary nephrons: 20% of nephrons; long nephron loops extend into the medulla; vasa recta capillaries supply blood; crucial for urine concentration.
Urine Formation
Three Processes of Urine Formation
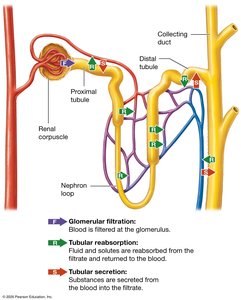
Glomerular filtration: Blood pressure forces water and solutes from glomerular capillaries into the glomerular capsule, forming filtrate.
Tubular reabsorption: Most water and solutes are reabsorbed from the filtrate back into the blood, mainly in the proximal tubule and nephron loop.
Tubular secretion: Additional substances are secreted from the blood into the filtrate to maintain homeostasis.
Glomerular Filtration
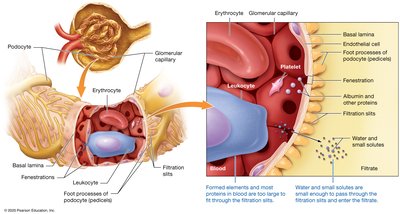
Filtration Membrane
The filtration membrane consists of three layers:
Fenestrated glomerular capillary endothelium
Basal lamina
Podocytes (visceral layer of glomerular capsule)
Only small molecules (e.g., water, glucose, electrolytes, amino acids) pass through; large proteins and cells are retained in the blood.
Glomerular Filtration Rate (GFR)
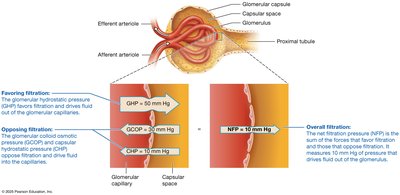
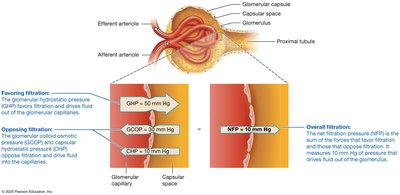
GFR is the amount of filtrate formed by both kidneys per minute. In healthy adults, GFR is about 125 mL/min (180 L/day), meaning plasma is filtered about 60 times per day.
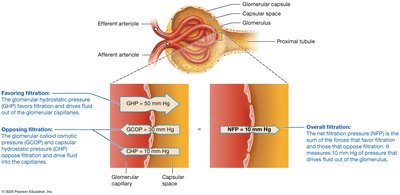
Glomerular hydrostatic pressure (GHP): Favors filtration by pushing fluid out of capillaries.
Glomerular colloid osmotic pressure (GCOP): Opposes filtration by drawing water back into capillaries due to plasma proteins.
Capsular hydrostatic pressure (CHP): Opposes filtration due to pressure from accumulated filtrate in the capsule.
Regulation of Glomerular Filtration Rate (GFR)
Autoregulation
Myogenic mechanism: Smooth muscle in afferent arteriole responds to stretch; constricts if blood pressure rises (decreases GFR), dilates if blood pressure falls (increases GFR).
Tubuloglomerular feedback: Macula densa cells sense Na+ and Cl- in filtrate; release ATP/adenosine to constrict afferent arteriole if GFR is too high, or signal JG cells to release renin if GFR is too low.
Hormonal Regulation
Natriuretic peptides: Released by the heart in response to increased blood volume; dilate afferent arterioles and constrict efferent arterioles, increasing GFR and promoting fluid loss to lower blood pressure.
Renin-angiotensin-aldosterone system (RAAS): Activated by low blood pressure or low Na+/Cl- in filtrate; increases Angiotensin-II, which constricts arterioles, increases GFR, and stimulates aldosterone release for Na+ retention.
Neural Regulation
Sympathetic nervous system: Releases norepinephrine, causing vasoconstriction. Low stimulation maintains GFR; high stimulation (e.g., during shock) greatly reduces GFR to conserve fluid.
Types of Capillaries
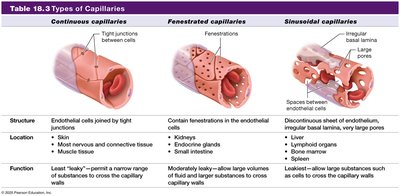
Type | Structure | Location | Function |
|---|---|---|---|
Continuous | Tight junctions | Most nervous and connective tissue, muscle tissue | Least leaky; restricts passage of most substances |
Fenestrated | Fenestrations (pores) | Kidneys, endocrine glands, small intestine | Moderately leaky; allows large volumes of fluid and small solutes to cross |
Sinusoidal | Discontinuous endothelium, large pores | Liver, lymphoid organs, bone marrow | Most leaky; allows large substances to cross |
Summary Table: Control of Glomerular Filtration Rate
See Table 24.1 in your textbook for a summary of the mechanisms controlling GFR, including autoregulation, hormonal, and neural influences.
Additional info: The micturition reflex (urination) and regulation of urine concentration are covered in subsequent lessons.
