 Back
BackBlood Components: Structure, Function, and Clinical Relevance
Study Guide - Smart Notes

Blood Components and Their Functions
Overview of Blood Composition
Blood is a specialized connective tissue in vertebrates, consisting of cells suspended in a liquid matrix called plasma. It plays essential roles in transport, exchange, and defense. Blood can be separated into plasma (about 55% of blood volume) and cellular elements (about 45%).
Plasma: The liquid component containing water, ions, proteins, nutrients, wastes, gases, and hormones.
Cellular Elements: Includes erythrocytes (red blood cells), leukocytes (white blood cells), and platelets.
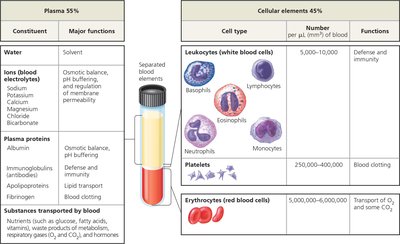
Plasma
Plasma is the straw-colored, liquid portion of blood. It serves as the medium for transporting substances and maintaining homeostasis.
Water: Acts as a solvent for carrying other substances.
Ions (Electrolytes): Such as sodium, potassium, calcium, and chloride, are crucial for osmotic balance, pH buffering, and regulation of membrane permeability.
Plasma Proteins:
Albumin: Maintains osmotic balance and buffers pH.
Immunoglobulins (Antibodies): Provide immune defense.
Apolipoproteins: Transport lipids in the blood.
Fibrinogen: Functions in blood clotting.
Other Substances: Nutrients, metabolic wastes, respiratory gases (O2, CO2), and hormones are transported in plasma.
Cellular Elements
The cellular elements of blood include erythrocytes, leukocytes, and platelets, each with specialized functions.
Erythrocytes (Red Blood Cells): Transport oxygen (O2) and some carbon dioxide (CO2).
Leukocytes (White Blood Cells): Defend the body against infection and disease. There are five major types: neutrophils, lymphocytes, monocytes, eosinophils, and basophils.
Platelets: Cell fragments involved in blood clotting.
Specialized Functions of Blood Cells
Erythrocytes (Red Blood Cells)
Erythrocytes are the most numerous blood cells, specialized for oxygen transport. Their biconcave shape increases surface area for gas exchange. They lack nuclei and mitochondria, maximizing space for hemoglobin, the iron-containing protein that binds O2.
Hemoglobin: Each erythrocyte contains about 250 million hemoglobin molecules, each binding up to four O2 molecules.
Sickle-Cell Disease: Caused by abnormal hemoglobin (HbS), leading to distorted, sickle-shaped cells that can block blood flow and reduce O2 delivery.
Leukocytes (White Blood Cells)
Leukocytes are less numerous than erythrocytes but are essential for immune defense. They can leave the circulatory system to patrol tissues and lymphatic fluid.
Phagocytic Leukocytes: Engulf and digest pathogens and debris (e.g., neutrophils, monocytes).
Lymphocytes: B cells and T cells mount specific immune responses.
Leukocyte Count: Increases during infection; normal range is 5,000–10,000 per μL of blood.
Platelets
Platelets are small, anucleate cell fragments derived from bone marrow cells. They play a critical role in blood clotting by forming plugs and releasing clotting factors.
Blood Cell Formation and Regulation
Hematopoiesis: Blood Cell Formation
All blood cells originate from multipotent stem cells in the red bone marrow. These stem cells differentiate into two main progenitor lines: lymphoid and myeloid.
Lymphoid Progenitors: Give rise to lymphocytes (B cells and T cells).
Myeloid Progenitors: Give rise to erythrocytes, platelets, and other leukocytes.
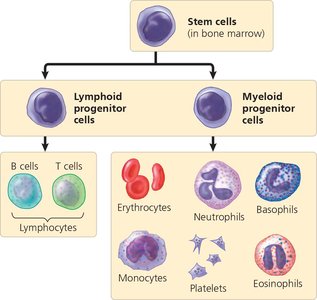
Erythrocyte production is regulated by erythropoietin (EPO), a hormone released by the kidneys in response to low O2 levels. EPO stimulates the production of more erythrocytes.
Blood Clotting Mechanism
Coagulation Cascade
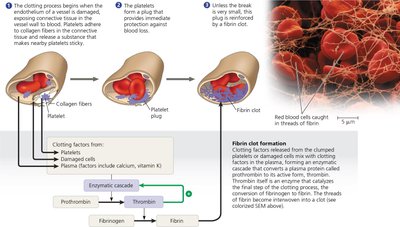
Blood clotting (coagulation) is a complex process that prevents blood loss after injury. It involves a cascade of enzymatic reactions leading to the conversion of fibrinogen (inactive) to fibrin (active), which forms a mesh to stabilize the clot.
Platelet Plug Formation: Platelets adhere to exposed collagen at the injury site and release clotting factors.
Enzymatic Cascade: Clotting factors activate prothrombin to thrombin, which then converts fibrinogen to fibrin.
Positive Feedback: Thrombin accelerates its own production, ensuring rapid clot formation.
Hemophilia: Genetic disorders that impair clotting, leading to excessive bleeding.
Cardiovascular Disease
Atherosclerosis, Heart Attacks, and Stroke
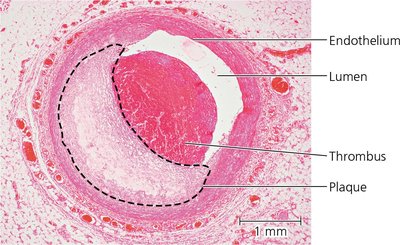
Cardiovascular diseases are major causes of mortality. Atherosclerosis is the buildup of fatty plaques in arteries, leading to reduced blood flow and increased risk of heart attack and stroke.
Atherosclerosis: Involves cholesterol accumulation, inflammation, and plaque formation in arterial walls.
Thrombus: A blood clot that forms within a vessel, potentially blocking blood flow.
Heart Attack (Myocardial Infarction): Occurs when blood flow to heart muscle is blocked, causing tissue death.
Stroke: Death of brain tissue due to blocked or ruptured arteries in the brain.
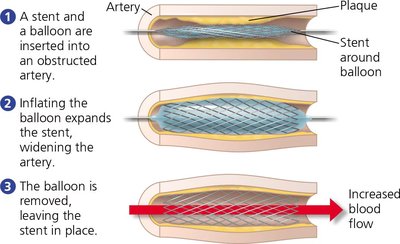
Treatment of Obstructed Arteries
Obstructed arteries can be treated by inserting a stent, a mesh tube that widens the artery and restores blood flow.
Cholesterol and Cardiovascular Risk
Cholesterol is transported in the blood by lipoproteins. Low-density lipoprotein (LDL) delivers cholesterol to cells, while high-density lipoprotein (HDL) removes excess cholesterol. A high LDL/HDL ratio increases cardiovascular risk. Genetic and lifestyle factors influence cholesterol levels.
Scientific Skills: Interpreting Histograms in Cardiovascular Research
Genetic Influence on LDL Cholesterol
Research on the PCSK9 gene shows that individuals with an inactivating mutation have lower LDL cholesterol levels, reducing cardiovascular risk. Histograms are used to compare LDL levels between study and control groups.
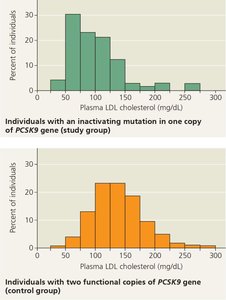
Interpretation: The study group (with the mutation) has a higher percentage of individuals with low LDL levels compared to the control group.
Conclusion: Inactivating PCSK9 mutations lower LDL cholesterol and may protect against heart disease.
Clinical and Lifestyle Considerations
Risk Factors and Prevention
Risk Factors: High LDL/HDL ratio, smoking, poor diet, lack of exercise, and genetic predisposition.
Prevention: Lifestyle changes (diet, exercise, quitting smoking), medications (statins, aspirin), and surgical interventions (stents, bypass surgery).
Hypertension: Chronic high blood pressure damages arteries and promotes plaque formation. Defined as systolic > 140 mm Hg or diastolic > 90 mm Hg.
Summary Table: Blood Components and Functions
Component | Major Functions |
|---|---|
Plasma | Solvent, osmotic balance, pH buffering, transport of nutrients, wastes, gases, and hormones |
Erythrocytes | Transport of O2 and some CO2 |
Leukocytes | Defense and immunity |
Platelets | Blood clotting |
Key Equations
Oxygen Carrying Capacity:
Blood Pressure: Additional info: Cardiac output and peripheral resistance are key determinants of blood pressure.
