 Back
BackCirculation and Blood: Structure, Function, and Regulation
Study Guide - Smart Notes

Circulatory System Structure and Evolution
Heart Chambers and Blood Flow
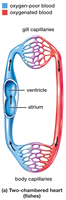
The vertebrate heart has evolved from a simple two-chambered structure in fish to a complex four-chambered organ in mammals and birds. This evolution allows for increasingly efficient separation of oxygenated and deoxygenated blood, supporting higher metabolic rates.
Two-chambered heart: Found in fish; consists of one atrium and one ventricle. Blood flows in a single circuit from the heart to the gills and then to the body.
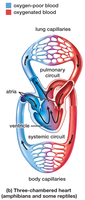
Three-chambered heart: Found in amphibians and some reptiles; consists of two atria and one ventricle. Partial separation of oxygenated and deoxygenated blood occurs.
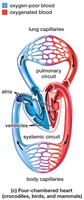
Four-chambered heart: Found in crocodilians, birds, and mammals; consists of two atria and two ventricles, allowing complete separation of oxygen-rich and oxygen-poor blood.
Human Heart Structure and Function
Heart Anatomy and Valves
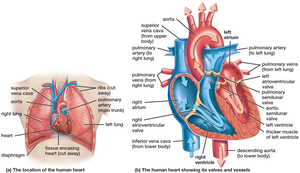
The human heart is a muscular organ divided into four chambers: two atria (upper chambers) and two ventricles (lower chambers). Valves ensure unidirectional blood flow and prevent backflow during contraction cycles.
Atrioventricular (AV) valves: Separate atria from ventricles (tricuspid and bicuspid/mitral valves).
Semilunar valves: Located at the exits of the ventricles (pulmonary and aortic valves).
The "lub-dub" sounds of the heartbeat are produced by the closing of these valves: "lub" (AV valves closing), "dub" (semilunar valves closing).
Cardiac Cycle and Electrical Conduction
The cardiac cycle consists of coordinated contractions (systole) and relaxations (diastole) of the atria and ventricles, regulated by an intrinsic conduction system and modulated by the nervous and endocrine systems.
Atrial systole: Atria contract, pushing blood into ventricles.
Ventricular systole: Ventricles contract, ejecting blood into arteries (normal pressure: 120 mm Hg).
Diastole: Heart muscle relaxes, chambers fill with blood (normal pressure: 80 mm Hg).
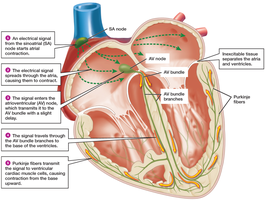
Conduction system: The sinoatrial (SA) node initiates the heartbeat, followed by the atrioventricular (AV) node, AV bundle, bundle branches, and Purkinje fibers.
Heart rate and force are influenced by the parasympathetic and sympathetic nervous systems, as well as hormones.
Blood: Composition and Function
Major Components of Blood
Blood is a connective tissue with two main components: plasma (liquid) and formed elements (cells and cell fragments). It serves as the transport medium for gases, nutrients, wastes, and signaling molecules.
Plasma: Makes up 55–60% of blood volume; primarily water with dissolved proteins, ions, nutrients, hormones, and wastes.
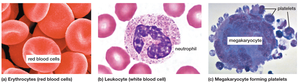
Formed elements: Include red blood cells (erythrocytes), white blood cells (leukocytes), and platelets (thrombocytes).
Plasma Proteins and Functions
Plasma proteins are essential for maintaining osmotic balance, immune defense, and blood clotting.
Albumin: Maintains osmotic pressure of blood.
Globulins: Include antibodies for immune response.
Fibrinogen: Precursor to fibrin, essential for blood clotting.
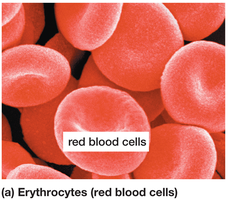
Red Blood Cells (Erythrocytes)
Red blood cells are specialized for oxygen transport. They lack nuclei and mitochondria in mammals, maximizing space for hemoglobin.
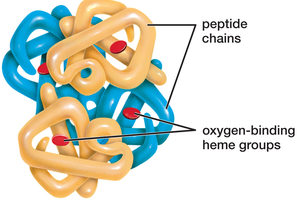
Hemoglobin: Iron-containing protein that binds oxygen; each molecule can carry four O2 molecules.
Hemoglobin gives blood its red color when oxygenated and a darker color when deoxygenated.
Red blood cells are produced in bone marrow and live about 120 days.
Regulation of Red Blood Cell Production
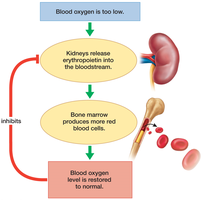
Red blood cell numbers are regulated by negative feedback involving the hormone erythropoietin, produced by the kidneys in response to low oxygen levels.
Erythropoietin: Stimulates bone marrow to increase RBC production.
Low oxygen can result from blood loss, high altitude, or lung dysfunction.
When oxygen levels normalize, erythropoietin secretion decreases.
White Blood Cells (Leukocytes)
White blood cells defend the body against pathogens and foreign substances. They are larger than RBCs and can move through capillary walls into tissues.
Five main types: neutrophils, eosinophils, basophils, lymphocytes, and monocytes.
Monocytes become macrophages in tissues, engulfing pathogens and debris.
Leukocytes make up less than 1% of blood cells but are vital for immunity.
Platelets and Blood Clotting
Platelets are cell fragments derived from megakaryocytes in bone marrow. They play a central role in blood clotting, which prevents excessive blood loss after injury.
Platelets form a temporary plug at injury sites and release chemicals that trigger the clotting cascade.
Fibrinogen is converted to fibrin, forming a mesh that stabilizes the clot.
Clotting disorders, such as hemophilia, result from deficiencies in clotting factors.
Blood Vessels: Structure and Function
Types of Blood Vessels
Blood circulates through a closed system of vessels, each adapted for specific functions in the transport and exchange of substances.
Arteries: Carry blood away from the heart; thick, elastic walls withstand high pressure.
Arterioles: Small branches of arteries that regulate blood flow to capillaries.
Capillaries: Microscopic vessels where exchange of gases, nutrients, and wastes occurs; walls are one cell thick.
Venules: Collect blood from capillaries and transport it to veins.
Veins: Return blood to the heart; thinner walls and valves prevent backflow.
Capillary Exchange and Fluid Balance
Capillaries allow for the exchange of substances between blood and interstitial fluid. Fluid movement is regulated by blood pressure and osmotic pressure.
Most cells are within 100 micrometers of a capillary, ensuring efficient diffusion.
Precapillary sphincters regulate blood flow into capillary beds.
About 85% of fluid lost from capillaries is reabsorbed; the remainder is returned by the lymphatic system.
Venous Return and Valves
Veins rely on skeletal muscle contractions and one-way valves to return blood to the heart, especially from the lower body. Prolonged inactivity can lead to pooling of blood and varicose veins.
The Lymphatic System and Its Role in Circulation
Lymphatic System Functions
The lymphatic system is a network of vessels and organs that returns excess interstitial fluid to the bloodstream, transports fats, and supports immune function.
Returns fluid to the venous system, preventing edema.
Transports absorbed fats from the small intestine via lacteals.
Filters blood and lymph, exposing pathogens to immune cells in lymph nodes and the spleen.
Lymphatic Vessels and Organs
Lymphatic vessels resemble veins and capillaries but are more permeable and have one-way valves. Primary lymphatic organs include bone marrow and thymus; secondary organs include lymph nodes, tonsils, and spleen.
Lymph nodes filter lymph and house lymphocytes and macrophages.
The spleen filters blood, breaks down old erythrocytes, and stores blood.
Clinical Connection: Lymphatic Disorders
Blockage of lymphatic vessels, such as in elephantiasis caused by parasitic infection, leads to severe swelling due to fluid accumulation.
Summary Table: Blood Components and Their Functions
Component | Main Function |
|---|---|
Plasma | Transports nutrients, wastes, hormones; maintains osmotic balance |
Red Blood Cells (Erythrocytes) | Transport oxygen and some carbon dioxide |
White Blood Cells (Leukocytes) | Defend against pathogens; immune response |
Platelets | Blood clotting |
