 Back
BackNeurons, Nervous System, and Circulatory System: Structure and Function
Study Guide - Smart Notes

Neurons and Nervous System Organization
Structure and Function of Neurons
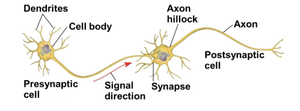
Neurons are specialized cells responsible for transmitting information throughout the body. Their structure is adapted for efficient communication, consisting of dendrites, a cell body, and a single axon. Dendrites receive signals, while the axon transmits them to other cells. The synapse is the junction where the axon communicates with the postsynaptic cell, often via neurotransmitters. Glial cells support and maintain neurons, outnumbering them significantly.
Dendrites: Highly branched extensions that receive signals.
Cell body: Contains most organelles of the neuron.
Axon: Long extension transmitting signals to other cells.
Synapse: Junction for signal transmission to postsynaptic cells.
Neurotransmitters: Chemical messengers passing information between neurons.
Glial cells: Support and outnumber neurons.
Stages of Nervous System Information Processing
The nervous system processes information in three main stages: sensory input, integration, and motor output. Sensory neurons transmit information about stimuli, interneurons analyze and interpret this input, and motor neurons send signals to effectors such as muscles or glands.
Sensory input: Detection of external or internal stimuli.
Integration: Analysis and interpretation by interneurons.
Motor output: Transmission of signals to effectors.
Central and Peripheral Nervous Systems
The Central Nervous System (CNS) consists of the brain and spinal cord, responsible for integration. The Peripheral Nervous System (PNS) includes nerves and ganglia, transmitting information to and from the CNS. Bundles of PNS neurons form nerves.
CNS: Brain and spinal cord, site of integration.
PNS: Nerves and ganglia, transmission of information.
Nerves: Bundles of PNS neurons.
Membrane Potential and Action Potentials
Membrane Potential and Ion Channels
The membrane potential is the electrical potential difference across the neuron's plasma membrane, with the inside being negatively charged relative to the outside. The resting potential is maintained by sodium-potassium pumps, which use ATP to create sodium and potassium gradients. Ion channels convert chemical potential energy to electrical potential energy.
Resting potential: Membrane potential when neuron is not signaling.
Sodium-potassium pump: Maintains ion gradients using ATP.
Ion channels: Allow ions to flow, changing membrane potential.
Action Potential: Stages and Properties
An action potential is a rapid, all-or-none change in membrane voltage, triggered by depolarization. It consists of several stages: resting potential, depolarization, rising phase, falling phase, and undershoot. The refractory period prevents immediate reactivation.
Resting potential: Most voltage-gated channels closed.
Depolarization: Some sodium channels open.
Rising phase: Threshold crossed, rapid increase in membrane potential.
Falling phase: Sodium channels inactivated, potassium flows out.
Undershoot: Potassium permeability high, then returns to rest.
Equation for membrane potential: (Nernst equation for equilibrium potential)
Circulatory System: Structure and Function
Blood Flow and Capillary Exchange
The circulatory system transports nutrients, gases, and wastes. The aorta provides blood to the heart via coronary arteries. Diffusion of O2 and CO2 occurs in capillary beds throughout the body. Blood returns to the heart through the superior and inferior vena cava, entering the right atrium.
Aorta: Main artery supplying blood to the heart.
Capillary beds: Sites of gas exchange.
Vena cava: Returns blood to the heart.


The Cardiac Cycle
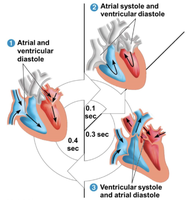
The cardiac cycle consists of alternating contraction (systole) and relaxation (diastole) phases. During systole, the heart pumps blood; during diastole, chambers fill with blood. Coordination of these phases ensures efficient circulation.
Systole: Contraction phase, blood pumped out.
Diastole: Relaxation phase, chambers fill with blood.
Cardiac cycle: Complete sequence of pumping and filling.
Heart Valves and Blood Flow Regulation
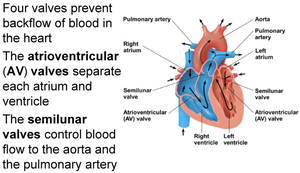
Four valves prevent backflow of blood in the heart. The atrioventricular (AV) valves separate atria and ventricles, while semilunar valves control blood flow to the aorta and pulmonary artery.
AV valves: Separate atria and ventricles.
Semilunar valves: Control flow to aorta and pulmonary artery.
Electrical Activity and Pacemaker Function
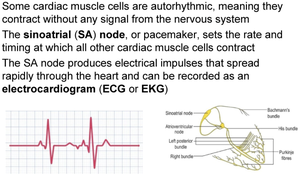
Some cardiac muscle cells are autorhythmic, contracting without nervous input. The sinoatrial (SA) node acts as the pacemaker, setting the rate and timing of contraction. Electrical impulses from the SA node spread rapidly and can be recorded as an electrocardiogram (ECG).
SA node: Pacemaker, initiates electrical impulses.
ECG: Records electrical activity of the heart.
Conduction Pathways in the Heart
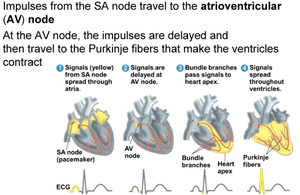
Impulses from the SA node travel to the atrioventricular (AV) node, where they are delayed before moving to the Purkinje fibers, causing ventricular contraction. This pathway ensures coordinated contraction of the heart chambers.
AV node: Delays impulses, coordinates contraction.
Purkinje fibers: Distribute impulses for ventricular contraction.
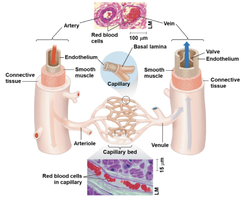
Blood Vessel Structure and Capillary Beds
Arteries, veins, and capillaries have distinct structural features. Arteries have thick walls to withstand high pressure, veins have valves to prevent backflow, and capillaries have thin walls for efficient exchange of materials.
Arteries: Thick walls, high pressure.
Veins: Valves, lower pressure.
Capillaries: Thin walls, exchange of gases and nutrients.
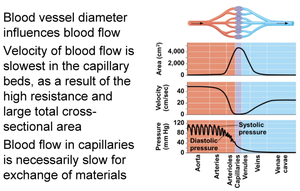
Blood Flow Dynamics and Pressure
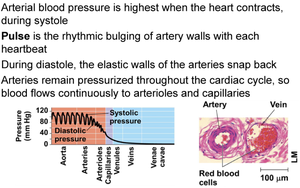
Blood vessel diameter influences blood flow. Velocity is slowest in capillary beds due to high resistance and large cross-sectional area, allowing for material exchange. Blood pressure is highest during systole and lowest during diastole.
Velocity: Slowest in capillaries.
Pressure: Highest during systole, lowest during diastole.
Pulse: Rhythmic bulging of artery walls.
Summary Table: Nervous and Circulatory System Components
Component | Function |
|---|---|
Neuron | Transmits electrical signals |
Glial cell | Supports and maintains neurons |
SA node | Pacemaker of the heart |
AV node | Delays and coordinates heart impulses |
Artery | Carries blood away from heart |
Vein | Returns blood to heart |
Capillary | Site of gas and nutrient exchange |
Additional info: The notes expand on the original content by providing definitions, examples, and context for each topic, ensuring completeness and academic quality for exam preparation.
