 Back
BackDigestion and Absorption in the Small and Large Intestine
Study Guide - Smart Notes

The Small Intestine
Gross Anatomy
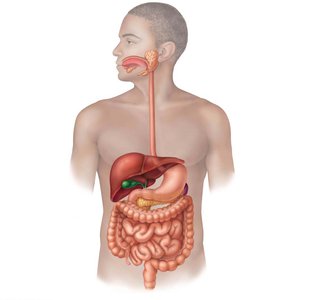
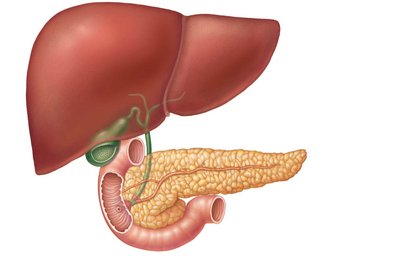
The small intestine is the primary site for digestion and absorption of nutrients. It extends from the pyloric sphincter to the ileocecal valve, measuring 2–4 meters in length and 2.5–4 cm in diameter. It is subdivided into three regions: the duodenum, jejunum, and ileum. The duodenum receives digestive secretions from the liver, gallbladder, and pancreas, which are essential for digestion.
Duodenum: First section, about 25 cm long, curves around the pancreas.
Jejunum: Middle section, about 2.5 m long, attached by mesentery.
Ileum: Last section, about 3.6 m long, joins the large intestine at the ileocecal valve.
Blood and Nerve Supply
Blood supply: Superior mesenteric artery supplies blood; veins drain into the hepatic portal vein and then to the liver.
Nerve supply: Parasympathetic (vagus nerve) and sympathetic (thoracic splanchnic nerves) innervation regulate intestinal activity.
Microscopic Anatomy
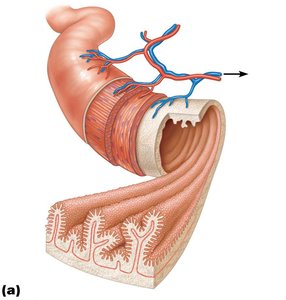
The small intestine is highly specialized for absorption, with structural modifications that increase its surface area approximately 600-fold to about 200 m2 (the size of a tennis court). These modifications include:
Circular folds: Permanent folds (~1 cm deep) that force chyme to spiral, increasing absorption time.
Villi: Fingerlike projections (~1 mm high) containing capillaries and a lymphatic vessel (lacteal) for nutrient absorption.
Microvilli: Cytoplasmic extensions forming the brush border, which contains enzymes for final digestion of carbohydrates and proteins.
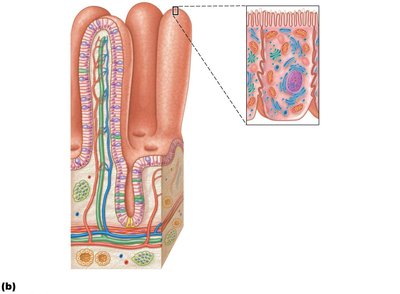
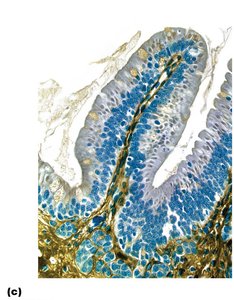
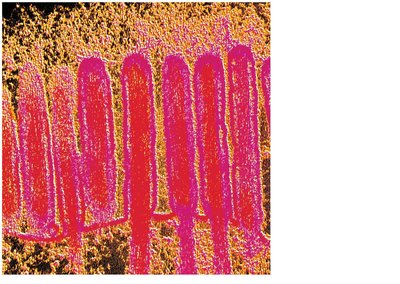
Cell Types in the Small Intestine
Enterocytes: Absorptive cells with microvilli; absorb nutrients and electrolytes.
Goblet cells: Secrete mucus for lubrication and protection.
Enteroendocrine cells: Release hormones (e.g., CCK, secretin) that regulate digestion.
Paneth cells: Secrete antimicrobial agents (defensins, lysozyme) to protect against bacteria.
Stem cells: Continuously divide to renew the epithelium every 2–4 days.
Intestinal Juice
1–2 L secreted daily in response to distension or irritation.
Major stimulus: hypertonic or acidic chyme.
Slightly alkaline, isotonic with blood plasma, mainly water and mucus.
Digestive Processes in the Small Intestine
Chyme from the stomach contains partially digested carbohydrates and proteins, and undigested fats. The small intestine completes digestion and absorbs nutrients over 3–6 hours. Enzymes from the pancreas and bile from the liver aid in digestion, while brush border enzymes complete the breakdown of nutrients.
Segmentation: Most common motion after a meal, mixing and moving chyme toward the ileocecal valve.
Peristalsis: Occurs between meals, moving remnants toward the large intestine.
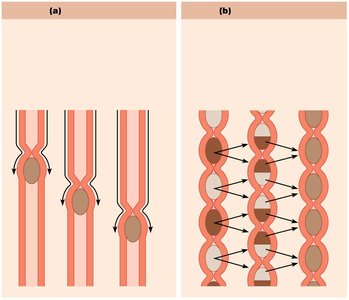
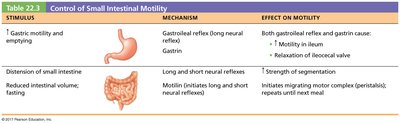
Control of Small Intestinal Motility
Stimulus | Mechanism | Effect on Motility |
|---|---|---|
Gastric motility and emptying | Gastroileal reflex (long neural reflex), Gastrin | Increased motility in ileum, relaxation of ileocecal valve |
Distension of small intestine | Long and short neural reflexes | Increased strength of segmentation |
Reduced intestinal volume (fasting) | Motilin (initiates migrating motor complex) | Initiates peristaltic waves until next meal |
The Large Intestine
Gross Anatomy
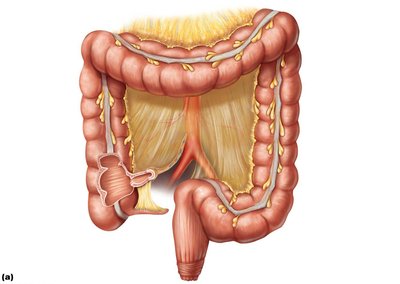
The large intestine absorbs remaining water, electrolytes, and vitamins produced by bacteria, and compacts indigestible food into feces. It is characterized by three unique features: teniae coli (longitudinal muscle bands), haustra (pouches), and epiploic appendages (fat-filled pouches).
Cecum: First part, receives chyme from the ileum.
Appendix: Contains lymphoid tissue, may store beneficial bacteria.
Colon: Ascending, transverse, descending, and sigmoid regions.
Rectum: Stores feces; three valves prevent passage of feces with gas.
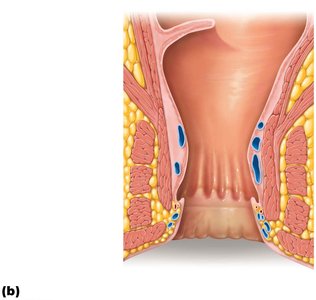
Anal canal: Opens to the exterior; contains internal (smooth muscle) and external (skeletal muscle) sphincters.
Microscopic Anatomy
Thicker mucosa with simple columnar epithelium (except anal canal, which is stratified squamous).
Deep crypts with many goblet cells for mucus secretion.
Anal columns and sinuses aid in emptying and protect the mucosa.
Bacterial Flora
Over 1000 species of bacteria, outnumbering human cells 10:1.
Functions: ferment indigestible carbohydrates, synthesize B vitamins and vitamin K, suppress pathogenic bacteria, and influence health and disease susceptibility.
Digestive Processes in the Large Intestine
Residue remains for 12–24 hours; no further food breakdown except by bacteria.
Absorbs vitamins, water, and electrolytes; propels feces toward the anus for defecation.
Motility includes haustral contractions (slow segmenting movements) and mass movements (powerful peristaltic waves).
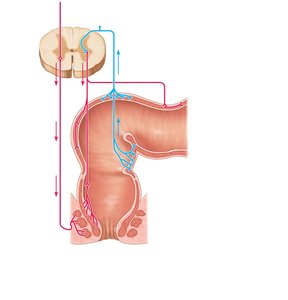
Defecation Reflex
Mass movements force feces into the rectum, stretching the wall and initiating the spinal defecation reflex.
Parasympathetic signals stimulate contraction of the rectum and relaxation of the internal anal sphincter.
Voluntary relaxation of the external anal sphincter allows defecation.
Mechanisms of Digestion and Absorption
Enzymatic Hydrolysis
Digestion is a catabolic process that breaks down macromolecules into monomers small enough for absorption. Enzymes from intrinsic and accessory glands carry out hydrolysis, adding water to break chemical bonds.
Absorption Mechanisms
Absorption moves substances from the gut lumen into the body, primarily through enterocytes.
Lipid molecules are absorbed passively; other nutrients require active transport.
Most absorption occurs before chyme reaches the ileum.
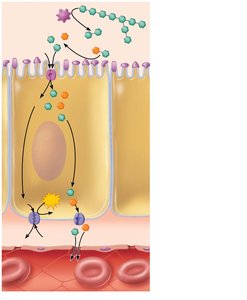
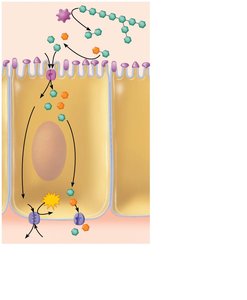
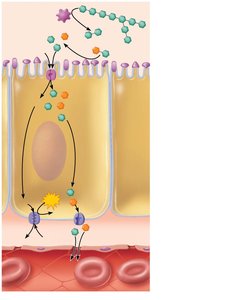
Digestion and Absorption of Carbohydrates
Only monosaccharides (glucose, fructose, galactose) are absorbed.
Starch and disaccharides are broken down by salivary and pancreatic amylase, then by brush border enzymes into monosaccharides.
Monosaccharides are absorbed via cotransport with Na+ (secondary active transport) and facilitated diffusion.
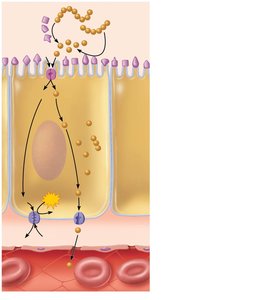
Digestion and Absorption of Proteins
Proteins are digested by pepsin in the stomach, then by pancreatic proteases (trypsin, chymotrypsin, carboxypeptidase) and brush border enzymes in the small intestine.
Amino acids are absorbed via cotransport with Na+ or H+ and exit by facilitated diffusion.
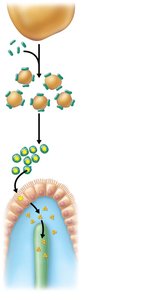
Digestion and Absorption of Lipids
Emulsification by bile salts increases surface area for pancreatic lipase action.
Lipase breaks triglycerides into monoglycerides and free fatty acids, which form micelles with bile salts.
Lipid products diffuse into enterocytes, are reassembled into triglycerides, and packaged as chylomicrons for transport via lymphatics.
Digestion and Absorption of Nucleic Acids
Pancreatic nucleases and brush border enzymes break down DNA and RNA into nitrogenous bases, pentose sugars, and phosphate ions.
These are absorbed by active transport into the blood.
Absorption of Vitamins, Electrolytes, and Water
Vitamins: Fat-soluble vitamins (A, D, E, K) are absorbed with micelles; water-soluble vitamins by diffusion or active transport; vitamin B12 requires intrinsic factor.
Electrolytes: Most ions are actively absorbed; iron and calcium absorption is regulated by need.
Water: About 95% is absorbed in the small intestine by osmosis; the rest in the large intestine.
Clinical Considerations
Lactose intolerance: Deficiency of lactase leads to osmotic diarrhea and gas production.
Malabsorption syndromes: Can result from impaired bile or pancreatic juice delivery, or damaged mucosa (e.g., celiac disease).
Appendicitis: Inflammation of the appendix, potentially leading to peritonitis if ruptured.
Antibiotic-associated diarrhea: Overgrowth of Clostridium difficile can cause severe colitis.
Diverticulosis/diverticulitis: Outpouchings of the colon wall, which can become inflamed or rupture.
Irritable bowel syndrome: Functional disorder with abdominal pain, stool changes, and bloating, often triggered by stress.
