 Back
BackThe Gastrointestinal System: Digestion, Absorption, and Disorders
Study Guide - Smart Notes

The Gastrointestinal System
Introduction to the Gastrointestinal Tract (GIT)
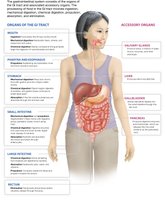
The gastrointestinal tract (GIT) is a series of organs that work together to digest food, absorb nutrients, and eliminate waste. The GIT includes both major organs, through which food passes, and accessory organs, which assist in digestion but do not directly contact food.
Major Organs: Mouth, pharynx, esophagus, stomach, small intestine, large intestine, rectum.
Accessory Organs: Salivary glands, liver, gallbladder, pancreas.
Sphincters: Muscular valves that regulate the passage of material between organs.
Major Functions of the GIT
Digestion: Breakdown of food into smaller components via mechanical and chemical methods.
Absorption: Uptake of nutrients into the circulatory system.
Fermentation: Gut microbiota break down soluble fibers.
Excretion: Removal of waste products in stool.
Digestion: Physical and Chemical Processes
The Mouth
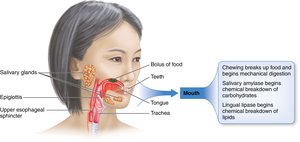
Digestion begins in the mouth, where both mechanical and chemical processes start breaking down food.
Mechanical Digestion: Chewing breaks food into smaller pieces.
Chemical Digestion: Salivary amylase begins carbohydrate digestion; lingual lipase starts lipid digestion.
Pharynx and Esophagus
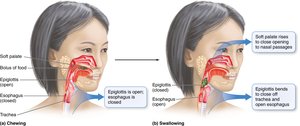
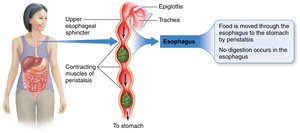
Food moves from the mouth to the pharynx and then the esophagus. The epiglottis prevents food from entering the trachea during swallowing. Peristalsis, a series of muscular contractions, moves food toward the stomach.
Bolus: The chewed mass of food that is swallowed.
Peristalsis: Involuntary muscle contractions that propel food.
Gastroesophageal Sphincter: Separates esophagus from stomach.
The Stomach
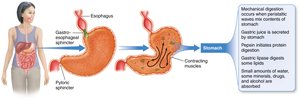
The stomach mixes, digests, and stores food. Mechanical digestion mixes food with gastric juice to form chyme. Chemical digestion of proteins and fats occurs here.
Gastric Juice: Contains hydrochloric acid (HCl), intrinsic factor, pepsin, and gastric lipase.
Chyme: Semi-liquid mass of partially digested food.
Minimal Absorption: Only small amounts of water, alcohol, and some drugs are absorbed.
The Small Intestine
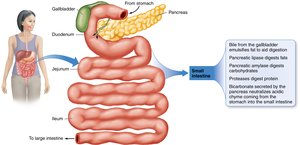
The small intestine is the primary site for digestion and absorption. Chyme is released from the stomach through the pyloric sphincter. Enzymes from the pancreas and bile from the gallbladder aid in digestion.
Sections: Duodenum, jejunum, ileum.
Enzymes: Pancreatic amylase (carbohydrates), pancreatic lipase (fats), proteases (proteins).
Bile: Emulsifies fats for digestion.
Mechanical Digestion: Segmentation and peristalsis mix and move food.
The Large Intestine
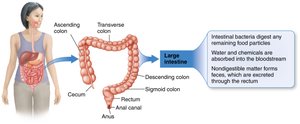
Undigested food passes into the large intestine, where water and some nutrients are absorbed. Bacterial fermentation of fiber occurs, and waste is stored before elimination.
Sections: Cecum, colon (ascending, transverse, descending, sigmoid), rectum, anus.
Functions: Absorption of water, formation of feces, bacterial fermentation.
Accessory Organs
Salivary Glands: Produce saliva containing salivary amylase.
Liver: Produces bile for fat digestion.
Gallbladder: Stores and releases bile.
Pancreas: Produces digestive enzymes and bicarbonate to neutralize stomach acid.
Actions of the GIT
Mechanical Digestion
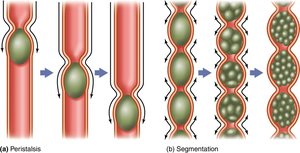
Mechanical digestion involves the physical breakdown and movement of food. Peristalsis propels food, while segmentation mixes it with digestive enzymes.
Peristalsis: Wavelike contractions moving food through the GIT.
Segmentation: Rhythmic contractions in the small intestine that mix food.

Chemical Digestion
Chemical digestion uses enzymes and acids to break down food into absorbable molecules. Enzymes are specific to substrates and require optimal pH and co-factors.
Enzymes: Proteins that catalyze chemical reactions.
Acid-Base Conditions: pH affects enzyme activity.
Regulation of Digestion
Digestion is regulated by the nervous and endocrine systems. Hormones and nerves coordinate the release of digestive juices and enzymes.
Nervous System: Relays messages between the GIT and brain.
Hormones: Ghrelin (stimulates hunger), cholecystokinin (CCK, satiety), leptin (satiety).
Absorption
Absorptive Structures
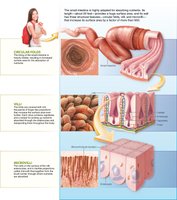
The small intestine is specialized for absorption, with folds, villi, and microvilli increasing surface area. Enterocytes line the villi and facilitate nutrient uptake.
Folds: Increase surface area.
Villi: Finger-like projections containing capillaries and lacteals.
Microvilli: Microscopic projections that trap nutrients.
Absorptive Mechanisms
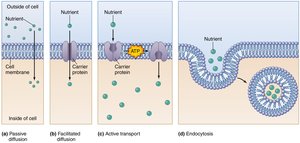
Nutrients are absorbed by several mechanisms:
Passive Diffusion: Movement from high to low concentration without energy or carrier proteins (e.g., water, lipids).
Facilitated Diffusion: Movement from high to low concentration with a carrier protein (e.g., fructose).
Active Transport: Movement from low to high concentration using energy and a carrier protein (e.g., glucose, amino acids).
Endocytosis: Cell engulfs nutrient molecules.
Transport of Nutrients
Water-Soluble Nutrients: Enter the portal vein and go to the liver.
Fat-Soluble Nutrients: Enter lymphatic vessels and then the bloodstream.
Gut Microbiome
Functions of the Gut Microbiome
The gut microbiome consists of beneficial bacteria, fungi, and other microbes that aid digestion, synthesize vitamins, inhibit harmful organisms, and support immune function.
Fermentation: Produces short-chain fatty acids, gases, and vitamins (biotin, vitamin K).
Protective Role: May reduce risk of colorectal cancer.
Probiotics, Prebiotics, and Synbiotics
Probiotics: Live microorganisms that confer health benefits (e.g., yogurt, kefir, kimchi).
Prebiotics: Dietary components that promote growth of beneficial microbes (e.g., inulin, resistant starch).
Synbiotics: Combination of probiotics and prebiotics (e.g., yogurt with fruit).
Disorders of the GIT
Heartburn and GERD
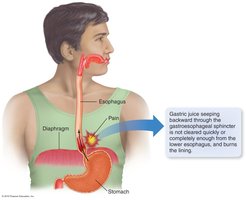
Heartburn is caused by stomach acid entering the esophagus due to a weakened lower esophageal sphincter. GERD is chronic, persistent heartburn.
Symptoms: Chest pain, burning sensation.
Aggravating Factors: Coffee, alcohol, nicotine.
Treatment: Smaller meals, avoid lying down after eating, medications.
Ulcers
Ulcers are erosions of the stomach or duodenal lining, often caused by Helicobacter pylori infection. Not caused by stress, but worsened by it.
Symptoms: Pain 1-3 hours after meals.
Treatment: Antibiotics to eradicate H. pylori.
Diarrhea
Diarrhea involves frequent, watery stools and can result from food intolerances, infections, stress, or bowel disorders. It can cause dehydration, especially in children and the elderly.
Treatment: Address underlying cause, maintain hydration.
Constipation and Hemorrhoids
Constipation is characterized by infrequent, hard, and difficult-to-pass stools, often due to low fiber intake. Hemorrhoids are swollen veins in the rectum and anus, sometimes resulting from constipation.
Treatment: High-fiber diet, adequate fluids, exercise.
Leaky Gut (Intestinal Barrier Dysfunction)
Leaky gut is caused by degradation of the gut microbiome, often due to antibiotics, poor diet, alcohol, or stress. It is linked to various GI disorders and chronic diseases.
Treatment: Diet rich in prebiotics and probiotics.
Irritable Bowel Syndrome (IBS)
IBS is a functional disorder affecting colon function, more common in women. Symptoms include abdominal cramps, bloating, and alternating diarrhea or constipation. A low-FODMAP diet may help reduce symptoms.
Celiac Disease
Celiac disease is an autoimmune disorder triggered by gluten, leading to damage of the small intestine and poor nutrient absorption. Requires a strict gluten-free diet.
Symptoms: Malabsorption, GI distress.
Diagnosis: Blood tests, biopsy.
Treatment: Gluten-free diet.

