 Back
BackHealth Systems Quality and Quality Improvement in Healthcare
Study Guide - Smart Notes

Health Systems Quality
Introduction to Health Systems Quality
Health systems quality refers to the degree to which health services for individuals and populations increase the likelihood of desired health outcomes and are consistent with current professional knowledge. It is a foundational concept in personal and public health, ensuring that care is safe, effective, patient-centered, timely, efficient, and equitable.
Definition: Quality in health care is measured by how well health services increase the likelihood of desired health outcomes and adhere to current professional standards.
Importance: High-quality health systems reduce harm, improve patient outcomes, and ensure efficient use of resources.
Canada Health Act Principles: Public administration, comprehensiveness, universality, portability, and accessibility are key pillars guiding Canadian health care quality.
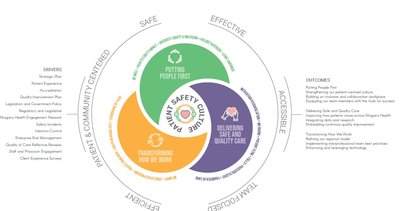
Dimensions of Health Care Quality
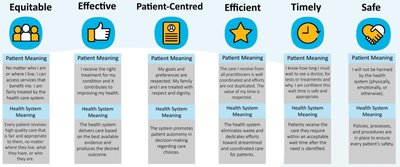
Quality in health care is multi-dimensional, encompassing several domains that collectively define a high-performing health system.
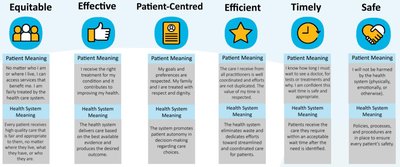
Safe: Avoiding harm to patients from care that is intended to help them.
Effective: Providing services based on scientific knowledge to all who could benefit.
Patient-Centered: Providing care that is respectful of and responsive to individual patient preferences, needs, and values.
Timely: Reducing waits and sometimes harmful delays for both those who receive and those who give care.
Efficient: Avoiding waste, including waste of equipment, supplies, ideas, and energy.
Equitable: Providing care that does not vary in quality because of personal characteristics such as gender, ethnicity, geographic location, and socioeconomic status.
Why is Quality Improvement Important?
Patient Safety and Harm in Health Care
Patient safety incidents are a significant concern in health care systems. Unintended harm can occur frequently, making quality improvement (QI) essential for reducing adverse events and improving outcomes.
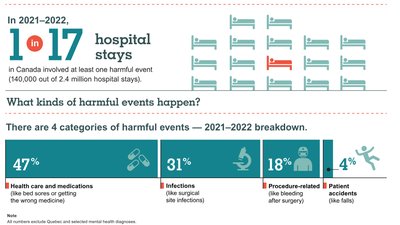
Statistics: In Canada, 1 in 17 hospital stays involved at least one harmful event in 2021–2022.
Types of Harmful Events: Health care and medication errors, infections, procedure-related issues, and patient accidents.
Impact: Patient safety incidents are the third leading cause of death in Canada.
Medical Errors and the Need for a Culture of Safety
Medical errors are a major public health problem, often resulting from system failures rather than individual negligence. Establishing a culture of safety and continuous improvement is critical.
System Failures: Most errors are due to flaws in processes, not individual mistakes.
Reporting Systems: Encouraging error reporting helps identify and address safety issues.
Standardization: Simplifying and standardizing procedures can reduce errors.
Leadership: Accountability and leadership at all levels are necessary for safety improvement.

Landmark Studies and Adverse Events
Research such as the "To Err is Human" report and the Canadian Adverse Events Study have highlighted the prevalence and preventability of medical errors.
Adverse Event: An unintended injury or complication caused by health care management, not the patient's underlying disease, leading to death, disability, or prolonged hospital stay.
Prevalence: Studies show that a significant percentage of hospital admissions involve preventable errors.
Quality Improvement (QI) in Healthcare
Definition and Scope of QI
Quality Improvement in healthcare involves systematic, data-driven efforts to enhance the quality, safety, and value of health services. QI is a continuous process that engages all staff and stakeholders in identifying and implementing effective changes.
QI Activities: Range from small-scale interventions to large organizational changes.
Continuous Process: QI should be ongoing and integrated into daily practice.
Goal: To reliably and sustainably meet patient and community needs.
Models and Approaches to QI
Several models guide QI efforts in healthcare, including the Model for Improvement and the Juran Trilogy.
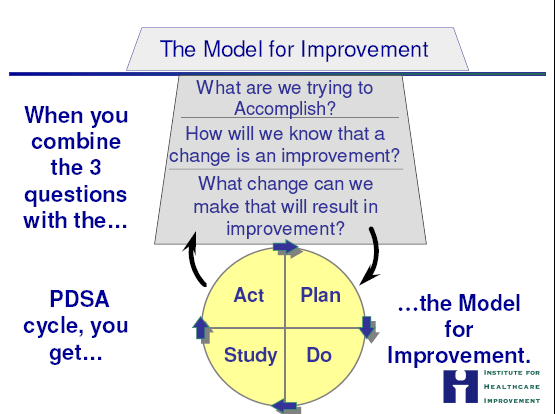
Model for Improvement: Focuses on three key questions: What are we trying to accomplish? How will we know a change is an improvement? What change can we make that will result in improvement? Uses the Plan-Do-Study-Act (PDSA) cycle.
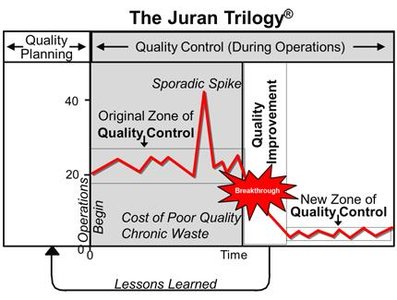
Juran Trilogy: Emphasizes quality planning, quality control, and quality improvement as stages in managing quality.

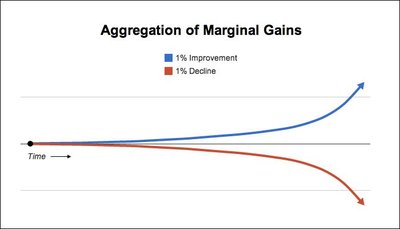
Marginal Gains and Incremental Improvement
The concept of marginal gains suggests that small, incremental improvements in multiple areas can lead to significant overall enhancement in quality and outcomes.
Aggregation of Marginal Gains: Consistent 1% improvements can compound over time to produce substantial benefits.
Application: Used in both healthcare and high-performance fields like sports and engineering.
Examples and Outcomes of QI in Healthcare
Case Studies and Measured Improvements
Quality improvement initiatives have demonstrated measurable benefits in various healthcare settings.
Reduced Readmission Rates: Follow-up calls and coaching reduced heart failure readmissions by 20%.
Reduced Falls: Implementing risk assessments reduced falls by 40%.
Improved Antibiotic Use: Amending pre-operative orders increased appropriate antibiotic use by 36%.
Hierarchy of Effectiveness in QI Interventions
QI interventions can be classified by their leverage and effectiveness, from low-leverage (education, rules) to high-leverage (automation, forcing functions).
System-Based Interventions: More effective but may be less feasible to implement.
Person-Based Interventions: Easier to implement but generally less effective.
Quality Oversight and Governance
Structures Supporting Quality
Oversight bodies and legislation play a crucial role in maintaining and improving health system quality.
Quality Oversight: Includes annual quality improvement plans, patient and staff surveys, and linking executive compensation to quality outcomes.
Key Organizations: Health Quality Ontario, Institute for Healthcare Improvement, and Healthcare Excellence Canada.


Conclusion: The Role of Everyone in Quality
Quality is the responsibility of all healthcare professionals, regardless of their role. Continuous improvement, collaboration, and a focus on patient safety are essential for advancing health system quality and achieving better health outcomes for all.
