 Back
BackConnective Tissue, Bone, Skin, and Blood: Structure and Function
Study Guide - Smart Notes

Connective Tissue Overview
Definition and Types
Connective tissue is characterized by having relatively few cells dispersed within an abundance of extracellular material. It serves structural, supportive, and transport functions throughout the body.
Loose connective tissue: Attaches epithelial tissue to underlying structures.
Tendons: Connect muscle to bone (covered in previous lectures).
Bone: Provides structural support and protection.
Blood: Functions as a transport medium for various substances.
Cells within connective tissue produce structural molecules (e.g., elastin) that are secreted into the extracellular matrix.
Bone: Structure and Growth
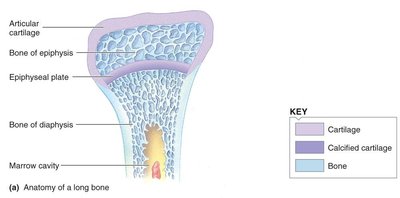
Anatomy of a Long Bone
Bones are specialized connective tissues composed of cells and an extracellular organic matrix (osteoid) produced by osteoblasts. The matrix is hardened by the deposition of calcium phosphate crystals, giving bone its strength and lightness.
Articular cartilage: Covers the ends of bones at joints, reducing friction.
Epiphysis: The rounded end of a long bone, containing spongy bone.
Epiphyseal plate: Region of cartilage where bone growth occurs in length.
Diaphysis: The shaft of the bone, composed mainly of compact bone.
Marrow cavity: Central cavity containing bone marrow.
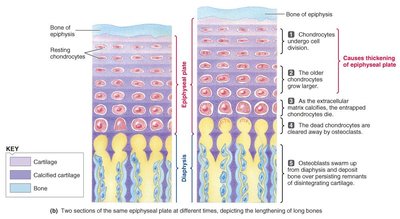
Bone Growth: Thickness and Length
Bone growth occurs by two mechanisms: appositional (thickness) and longitudinal (length) growth.
Thickness: Osteoblasts deposit new bone on the outer surface, while osteoclasts resorb bone on the inner surface near the marrow cavity.
Length: Occurs at the epiphyseal plate through the proliferation and maturation of chondrocytes (cartilage cells), followed by ossification.
Bone Cells and Remodeling
Osteoblasts: Bone-forming cells that secrete osteoid.
Osteocytes: Mature bone cells derived from osteoblasts, involved in calcium exchange.
Osteoclasts: Bone-resorbing cells that break down bone matrix.
Bone is a dynamic tissue, constantly remodeled by the balanced activity of osteoblasts and osteoclasts. This process is regulated by hormones such as parathyroid hormone (PTH), which increases plasma Ca2+ levels by stimulating bone resorption.
Hormonal Regulation of Bone Growth
Growth hormone (GH) and insulin-like growth factor 1 (IGF-1) stimulate the proliferation of epiphyseal cartilage, promoting bone growth in both length and thickness. The epiphyseal plate remains cartilaginous during growth, but ossifies (closes) at the end of adolescence, halting further lengthening.
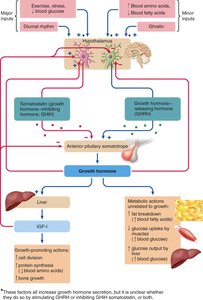
Abnormal Growth Hormone Secretion
Excess GH in childhood: Leads to gigantism (excessive height).
Excess GH in adulthood: Causes acromegaly (enlargement of extremities and facial features).
GH deficiency: Results in pituitary dwarfism if it occurs in childhood.
These conditions illustrate the importance of hormonal regulation in normal skeletal development.
Functions of the Skeleton
Provides structural support and protection for internal organs.
Facilitates movement by serving as attachment points for muscles.
Acts as a reservoir for minerals, especially calcium and phosphate.
Houses bone marrow for blood cell production.
Calcium Homeostasis and Bone Remodeling
About 99% of the body's Ca2+ is stored in bone. Plasma Ca2+ is tightly regulated (2.2–2.6 mmol/L) and is essential for:
Neuromuscular activity
Muscle contraction
Blood clotting
Cell signaling (second messenger)
Structural integrity of bone and teeth
Bone remodeling involves a balance between deposition (by osteoblasts) and resorption (by osteoclasts). PTH increases plasma Ca2+ by stimulating bone resorption.
Osteoporosis
Osteoporosis is a condition characterized by decreased bone density due to reduced deposition of the bone's organic matrix. It is especially common in peri- and post-menopausal women, increasing the risk of fractures and associated complications. Prevention includes maintaining physical activity and adequate calcium intake throughout life.
Skin: Structure and Function
Layers of the Skin
The skin is composed of three main layers, each with distinct structures and functions:
Epidermis: Outermost layer, consisting of multiple layers of epithelial cells. The inner layer contains living, dividing cells, while the outer layer is composed of dead, keratinized cells. The epidermis is avascular and provides a barrier to the environment.
Dermis: Connective tissue layer containing elastin, collagen, blood vessels, and specialized nerve endings. It supports the epidermis and houses sensory receptors and exocrine glands.
Hypodermis (subcutaneous tissue): Anchors the skin to underlying tissues and contains fat cells for insulation and energy storage.
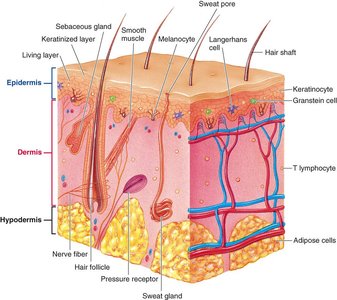
Specialized Cells and Functions
Keratinocytes: Produce keratin, forming the tough, protective outer layer.
Melanocytes: Synthesize melanin, the pigment responsible for skin color and protection against UV radiation.
Langerhans cells: Immune cells involved in defense mechanisms.
Granstein cells: Recently discovered immune cells with unclear functions.
The skin also synthesizes vitamin D in response to sunlight, which is essential for calcium absorption in the digestive tract.
Blood: Composition and Function
Components of Blood
Blood is a specialized connective tissue that transports gases, nutrients, wastes, and hormones throughout the body. It consists of plasma and three types of cellular elements:
Erythrocytes (red blood cells): Transport oxygen and carbon dioxide.
Leukocytes (white blood cells): Defend against pathogens and participate in immune responses.
Platelets (thrombocytes): Involved in blood clotting (hemostasis).
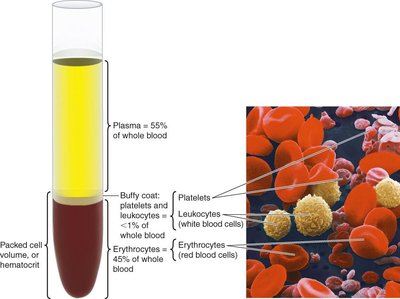
Plasma and Plasma Proteins
Plasma is the liquid component of blood, containing water, electrolytes, nutrients, wastes, gases, hormones, and plasma proteins. The main plasma proteins are:
Albumins: Maintain osmotic pressure and transport substances.
Globulins: Alpha and beta globulins transport substances; gamma globulins are antibodies.
Fibrinogen: Precursor to fibrin, essential for blood clotting.
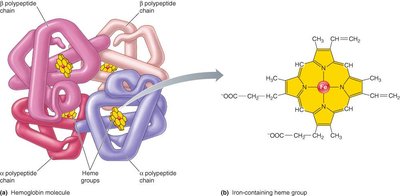
Erythrocytes and Hemoglobin
Erythrocytes are biconcave, flexible cells lacking nuclei and organelles, optimized for gas transport. Each erythrocyte contains millions of hemoglobin (Hb) molecules, which bind oxygen, carbon dioxide, hydrogen ions, carbon monoxide, and nitric oxide.
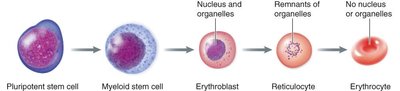
Erythropoiesis
Erythropoiesis is the process of red blood cell production, occurring in the bone marrow. It involves the differentiation of pluripotent stem cells into mature erythrocytes through several stages:
Pluripotent stem cell → Myeloid stem cell → Erythroblast → Reticulocyte → Erythrocyte
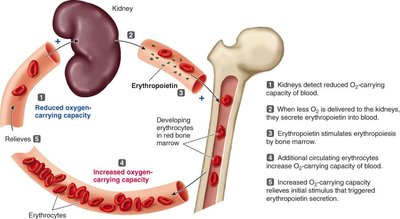
Regulation of Erythropoiesis
Erythropoiesis is regulated by erythropoietin (EPO), a hormone produced by the kidneys in response to reduced oxygen-carrying capacity of the blood. EPO stimulates the bone marrow to increase red blood cell production.
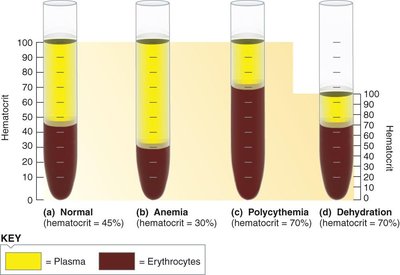
Hematocrit and Blood Disorders
Hematocrit is the percentage of blood volume occupied by erythrocytes. Normal values are about 45% for men and 42% for women. Changes in hematocrit can indicate anemia (low RBCs) or dehydration (reduced plasma volume).
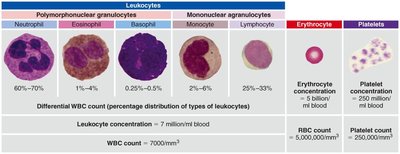
Leukocytes: Types and Functions
Leukocytes are divided into granulocytes (neutrophils, eosinophils, basophils) and agranulocytes (monocytes, lymphocytes). Each type has distinct roles in immune defense:
Neutrophils: Phagocytose bacteria and debris.
Eosinophils: Attack parasitic worms; involved in allergic reactions.
Basophils: Release histamine and heparin; involved in inflammation and allergic responses.
Monocytes: Differentiate into macrophages for phagocytosis.
Lymphocytes: B cells produce antibodies; T cells mediate cellular immunity.
Platelets and Hemostasis
Platelets are cell fragments essential for hemostasis, the process that prevents blood loss from damaged vessels. Hemostasis involves three steps:
Vascular spasm (vasoconstriction)
Formation of a platelet plug
Blood coagulation (clotting)
Platelets contain actin, myosin, and secretory granules, enabling them to contract and release factors necessary for clot formation.

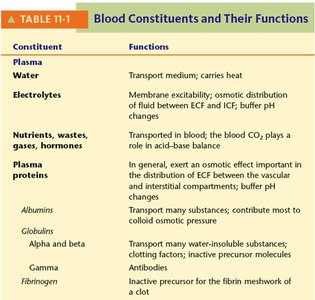
Summary Table: Blood Constituents and Their Functions
Constituent | Function |
|---|---|
Water | Transport medium; carries heat |
Electrolytes | Membrane excitability; osmotic distribution; buffer pH changes |
Nutrients, wastes, gases, hormones | Transported in blood; CO2 plays a role in acid-base balance |
Albumins | Transport substances; maintain colloid osmotic pressure |
Globulins (alpha, beta, gamma) | Transport, clotting, antibodies |
Fibrinogen | Precursor for fibrin meshwork of a clot |
