 Back
BackThe Skeletal System: Structure, Function, and Maintenance
Study Guide - Smart Notes

The Skeletal System: Structure, Function, and Maintenance
Overview of the Skeletal System
The skeletal system is a complex framework of bones and connective tissues that provides support, protection, and movement for the human body. It consists of bones, ligaments, and cartilage, each with specialized roles in maintaining structural integrity and facilitating motion.
Bones: Hard elements that form the skeleton.
Ligaments: Dense fibrous connective tissues that attach bones to other bones.
Cartilage: Specialized connective tissue that cushions vertebrae and reduces friction in joints.
Classification and Organization of Bones
Bones are classified by their shapes and are organized into two main groupings within the skeleton.
Types of Bones:
Long bones: Found in limbs and fingers.
Short bones: Found in the wrist.
Flat bones: Found in the cranium, sternum, and ribs.
Irregular bones: Found in the vertebrae and coxal bones.
Axial Skeleton: The midline of the body, including the skull, sternum, ribs, and vertebral column.
Appendicular Skeleton: Bones of the appendages and their attachments, including the pectoral and pelvic girdles, arms, and legs.
Functions of the Skeleton
The skeleton serves several essential functions:
Support: Provides a framework for soft organs.
Protection: Shields vital organs such as the brain, heart, and lungs.
Movement: Joints and muscles enable flexible movement.
Blood Cell Formation: Occurs in red bone marrow.
Mineral Storage: Stores calcium and phosphate.
Bone Structure and Composition
Bone Textures: Compact and Spongy Bone
Bones have two main textures: compact bone and spongy bone. Compact bone forms the dense outer layer, while spongy bone (also called diploë in flat bones) is found inside and has a porous, lattice-like structure.
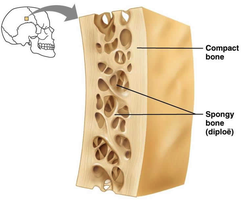
Microscopic Anatomy of Bone
Bones are living tissues containing several types of cells involved in bone formation and remodeling:
Osteogenic cells: Bone stem cells.
Osteoblasts: Cells that build new bone.
Osteocytes: Mature bone cells that maintain bone tissue.
Bone lining cells: Regulate calcium movement.
Osteoclasts: Cells that break down bone (resorption).
Structure of a Long Bone
Long bones have a characteristic structure:
Diaphysis: The shaft, composed of compact bone.
Epiphyses: The ends, containing spongy bone and red marrow.
Medullary cavity: Central cavity containing yellow marrow (fat storage).
Periosteum: Outer membrane covering the bone.
Articular cartilage: Covers joint surfaces to reduce friction.
Connective Tissues of the Skeleton
Ligaments
Ligaments are dense fibrous connective tissues that attach bone to bone, providing joint stability while allowing movement.
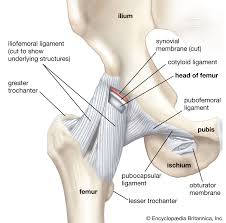
Cartilage
Cartilage provides support under pressure and reduces friction in joints. There are three main types:
Fibrocartilage: Found in intervertebral disks and menisci of the knee.
Hyaline cartilage: Forms embryonic structures, covers ends of long bones, and reduces friction.
Elastic cartilage: Flexible, found in the outer ear, nose, and epiglottis.
Bone Development, Growth, and Remodeling
Bone Development (Ossification)
Bone development begins in the embryo with cartilage models formed by chondroblasts. Later, osteoblasts replace cartilage with bone by secreting osteoid and enzymes that crystalize calcium phosphate. Osteoblasts mature into osteocytes, which maintain the bone matrix.
Bone Growth in Childhood and Adolescence
Long bones lengthen at the growth (epiphyseal) plate. Chondroblasts produce cartilage on the outer surface, while osteoblasts replace cartilage with bone on the inner surface. Bones also grow in diameter as osteoblasts deposit bone beneath the periosteum.
Bone Remodeling and Repair
Mature bone undergoes constant remodeling, changing shape, size, and strength in response to stress, diet, exercise, age, and hormones. Remodeling depends on the balance between osteoblast and osteoclast activity. Weight-bearing exercise increases bone mass and strength. Osteoporosis results from prolonged imbalance, leading to bone loss.
Bone Repair
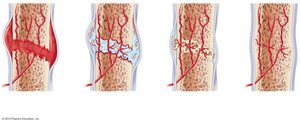
Bone repair after a fracture involves several stages:
Hematoma formation (clotted blood at the fracture site).
Fibrocartilaginous callus formation (fibroblasts and chondroblasts create a tough callus).
Bony callus formation (osteoblasts deposit new bone).
Bone remodeling (restoration of original shape and structure).
Joints (Articulations)
Classification of Joints
Joints connect bones and are classified by their degree of movement:
Fibrous joints: Immovable (e.g., skull sutures).
Cartilaginous joints: Slightly movable, connected by cartilage (e.g., intervertebral discs).
Synovial joints: Freely movable, bones separated by a fluid-filled cavity, stabilized by ligaments and tendons.
Types of Synovial Joints and Movements
Hinge joints: Allow movement in one plane (e.g., knee, elbow).
Ball and socket joints: Permit a wide range of movement (e.g., shoulder, hip).
Movements: Gliding, angular (flexion, extension, abduction, adduction), and rotation.
Ligaments, Tendons, and Muscles in Joint Stability
Ligaments: Attach bone to bone, providing stability.
Tendons: Attach muscle to bone, aiding movement and stability.
Muscles: Further stabilize joints and enable movement.
Diseases and Disorders of the Skeletal System
Common Disorders
Sprains: Stretched or torn ligaments, slow to heal due to poor blood supply.
Bursitis and tendinitis: Inflammation of bursae or tendons.
Osteoporosis: Excessive bone loss, increasing fracture risk.
Arthritis: Inflammation of joints, including osteoarthritis (degenerative) and rheumatoid arthritis (autoimmune).
Summary Table: Cells Involved in Bone Development and Maintenance
Cell Type | Function |
|---|---|
Osteogenic cells | Stem cells that differentiate into osteoblasts |
Osteoblasts | Build new bone matrix |
Osteocytes | Maintain bone tissue |
Bone lining cells | Regulate calcium and phosphate movement |
Osteoclasts | Break down bone (resorption) |
Hormonal Regulation of Bone Cells
Parathyroid hormone (PTH): Increases when blood calcium is low, stimulates osteoclasts to release calcium from bone.
Calcitonin: Increases when blood calcium is high, stimulates osteoblasts to deposit calcium in bone.
Additional info: Bone health is influenced by nutrition (calcium, vitamin D), physical activity, and hormonal balance. Disorders such as osteoporosis and arthritis can significantly impact mobility and quality of life.
