Back
BackAdaptive Immunity: Specific Defenses of the Host
Study Guide - Smart Notes

Adaptive Immunity: Specific Defenses of the Host
Introduction to Adaptive Immunity
Adaptive immunity refers to the body's ability to mount a specific response to particular pathogens after exposure. This system distinguishes between "self" and "nonself" and is activated when innate defenses are insufficient. Adaptive immunity is acquired through infection or vaccination and is characterized by a primary response (first exposure) and a more rapid, effective secondary response due to immunological memory.
Dual Nature of the Adaptive Immune System
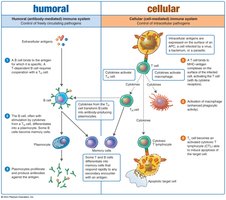
Humoral Immunity
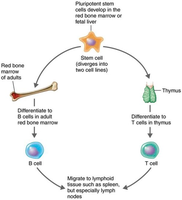
Humoral immunity involves the production of antibodies by B lymphocytes (B cells), which are created and mature in the red bone marrow. These cells recognize antigens and produce antibodies, primarily targeting extracellular pathogens and toxins.
B cells mature in the bone marrow and reside in blood and lymphoid organs.
Named after the bursa of Fabricius in birds.
Effective against extracellular bacteria, toxins, and viruses before they enter host cells.
Cellular Immunity (Cell-Mediated Immunity)
Cellular immunity is mediated by T lymphocytes (T cells), which mature in the thymus. T cells recognize antigenic peptides presented by phagocytic cells and secrete cytokines to coordinate the immune response, rather than producing antibodies. This branch is most effective against virus-infected cells and intracellular bacteria.
T cells mature in the thymus and reside in blood and lymphoid organs.
T cell receptors (TCRs) recognize antigens and trigger cytokine release.
Targets antigens already inside cells, such as viruses and some bacteria.
Cytokines: Chemical Messengers of Immune Cells
Cytokines are protein messengers produced in response to stimuli, facilitating communication between immune cells. Overproduction can lead to a cytokine storm, which is harmful.
Interleukins (ILs): Communication between leukocytes.
Chemokines: Induce migration of leukocytes.
Interferons (IFNs): Interfere with viral infections.
Tumor necrosis factor alpha: Involved in inflammation and autoimmune diseases.
Hematopoietic cytokines: Control development of blood cells.
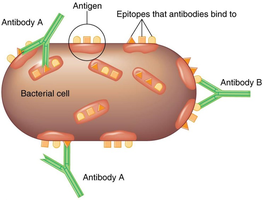
Antigens and Epitopes
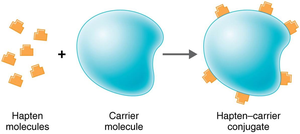
Antigens are substances that provoke an immune response, usually components of microbes or foreign substances. Antibodies interact with specific regions called epitopes (antigenic determinants). Haptens are small molecules that become antigenic only when attached to larger carrier molecules.
Examples: Capsules, cell walls, flagella, toxins, viral capsids, pollen.
Haptens require carrier molecules to elicit an immune response.
Humoral Immunity: Antibodies (Immunoglobulins)
Structure and Classes of Antibodies
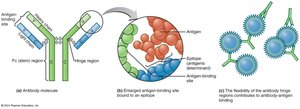
Antibodies, or immunoglobulins (Ig), are compact, soluble proteins that recognize and bind specific antigens. Each antibody has a valence, indicating the number of antigen-binding sites. The basic structure consists of two identical heavy chains and two identical light chains, forming a Y shape. The variable regions bind epitopes, while the constant (Fc) region determines the antibody class.
Five classes: IgG, IgM, IgA, IgD, IgE
Valence: Bivalent antibodies have two binding sites.
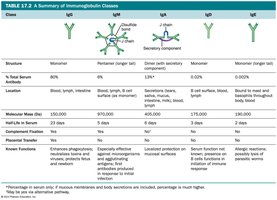
Summary of Immunoglobulin Classes
Class | Structure | Serum % | Location | Functions |
|---|---|---|---|---|
IgG | Monomer | 80% | Blood, lymph, intestine | Crosses placenta, activates complement, enhances phagocytosis, neutralizes toxins/viruses |
IgM | Pentamer | 6% | Blood, lymph, B cell surface | First antibody produced, agglutination, activates complement |
IgA | Dimer (secretions), Monomer (serum) | 13% | Secretions, blood, lymph | Protects mucosal surfaces |
IgD | Monomer | 0.02% | Blood, lymph, B cell surface | Role in B cell activation |
IgE | Monomer | 0.002% | Bound to mast cells, basophils, blood | Allergic reactions, lysis of parasitic worms |
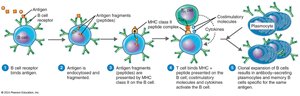
Humoral Immune Response Process
Clonal Selection and Expansion
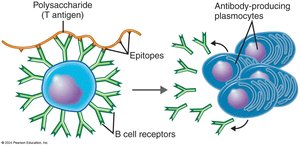
B cells interact with antigens in lymphoid organs. Each B cell has many surface immunoglobulins (B cell receptors, BCRs) that bind specific antigens. Upon activation (clonal selection), the B cell proliferates and differentiates into antibody-secreting plasma cells and memory B cells.
T-dependent antigens: Require help from T helper cells for B cell activation.
T-independent antigens: Activate B cells without T cell help (often polysaccharides).
Major Histocompatibility Complex (MHC)
MHC molecules are cell surface proteins essential for antigen presentation. Class I MHC is found on all nucleated cells and identifies "self." Class II MHC is found on antigen-presenting cells (APCs) such as B cells, macrophages, and dendritic cells, and is crucial for activating T helper cells.
Diversity and Results of Antigen–Antibody Interaction
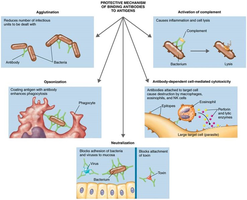
Antibody diversity is generated by gene rearrangement, allowing the immune system to recognize a vast array of antigens. Clonal deletion removes self-reactive B cells. When antibodies bind antigens, they form antigen–antibody complexes, leading to:
Agglutination
Opsonization
Antibody-dependent cell-mediated cytotoxicity
Neutralization
Complement activation
Cellular Immunity Response Process
T Cell Maturation and Activation
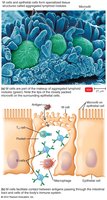
T cells mature in the thymus, where thymic selection eliminates self-reactive cells. Mature T cells migrate to lymphoid tissues and recognize antigens via T cell receptors (TCRs). Pathogens entering the gastrointestinal tract are sampled by M cells over Peyer's patches, which transfer antigens to lymphocytes and APCs.
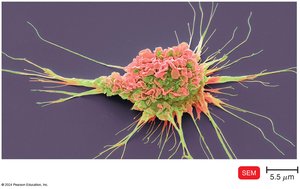
Antigen-Presenting Cells (APCs)
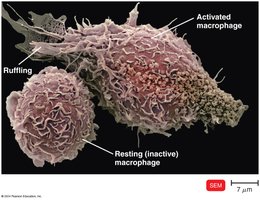
APCs include dendritic cells, macrophages, and B cells. Dendritic cells engulf and degrade microbes, presenting antigens to T cells. Macrophages are activated by cytokines or antigen ingestion and present antigens to T cells in lymph tissue.
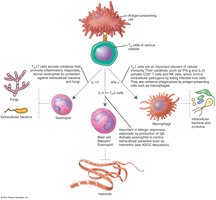
Classes of T Cells
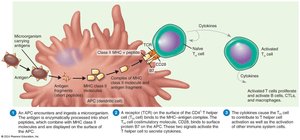
T Helper Cells (CD4+ T Cells)
T helper cells are activated when their TCR binds to antigen-MHC class II complexes on APCs. They secrete cytokines that activate B cells, other T cells, and macrophages. Subsets include Th1, Th2, and Th17, each with specialized functions in immunity and inflammation.
T Regulatory Cells
T regulatory cells (a subset of CD4+ cells) suppress immune responses against self, protect beneficial intestinal bacteria, and help prevent fetal rejection during pregnancy.
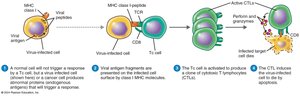
Cytotoxic T Lymphocytes (CD8+ T Cells)
CD8+ T cells (CTLs) recognize antigens presented by MHC class I molecules on infected or abnormal cells. Upon activation, CTLs release perforin and granzymes, inducing apoptosis in target cells, which prevents the spread of infection.
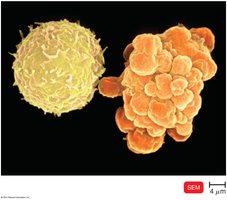
Nonspecific Cells and Extracellular Killing
Natural Killer (NK) Cells
NK cells destroy virus-infected cells, tumor cells, and large extracellular parasites. They do not require antigen stimulation and target cells lacking MHC class I molecules, inducing apoptosis via pore formation.
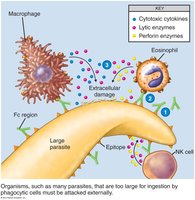
Antibody-Dependent Cell-Mediated Cytotoxicity (ADCC)
ADCC is used to destroy pathogens too large for phagocytosis, such as protozoans and helminths. Antibodies coat the target, and immune cells (NK cells, macrophages, eosinophils) bind to the Fc region, releasing cytotoxic substances to lyse the target.
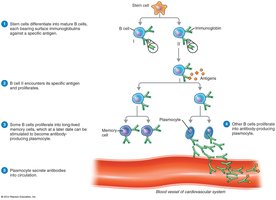
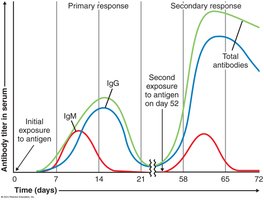
Immunological Memory
Primary immune response occurs upon first exposure to an antigen, with IgM produced first, followed by IgG. Secondary (anamnestic) response is faster and stronger due to memory cells, with class switching to IgG, IgE, or IgA. Antibody titer measures the concentration of antibodies in serum.
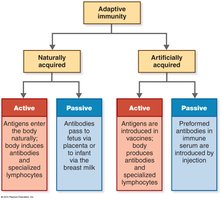
Types of Adaptive Immunity
Adaptive immunity can be acquired naturally or artificially, and can be active (body produces its own antibodies) or passive (antibodies are received from another source).
Naturally acquired active immunity: Infection-induced antibody production.
Naturally acquired passive immunity: Antibodies transferred via placenta or breast milk.
Artificially acquired active immunity: Vaccination-induced antibody production.
Artificially acquired passive immunity: Injection of preformed antibodies.
Summary: Dual Nature of the Adaptive Immune System
The adaptive immune system consists of humoral and cellular branches, each with specialized cells and mechanisms for targeting pathogens. Humoral immunity is mediated by B cells and antibodies, while cellular immunity is mediated by T cells. Both branches interact and are essential for effective immune defense.