Back
BackAdaptive Immunity: Specific Defenses of the Host – Study Notes
Study Guide - Smart Notes

Adaptive Immunity: Specific Defenses of the Host
Overview of Adaptive Immunity
Adaptive immunity is a highly specialized defense system that targets specific pathogens after exposure. It distinguishes "self" from "nonself" and is activated when innate defenses fail. Adaptive immunity is acquired through infection or vaccination and is characterized by a primary response (first exposure) and a secondary response (subsequent exposures), which is faster and more effective due to immunological memory.
Comparison of Adaptive and Innate Immunity
Innate Immunity: Non-specific, immediate response, includes barriers and phagocytes.
Adaptive Immunity: Specific, delayed response, involves lymphocytes and memory formation.
Dual Nature of the Adaptive Immune System
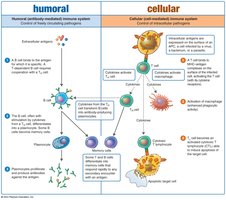
The adaptive immune system consists of two main branches: humoral and cellular immunity.
Humoral Immunity: Mediated by B cells and antibodies; combats extracellular pathogens and toxins.
Cellular Immunity: Mediated by T cells; combats intracellular pathogens such as viruses and some bacteria.
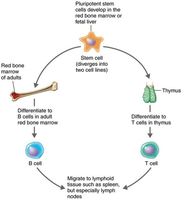
Humoral Immunity
B cells mature in the red bone marrow and reside in blood and lymphoid organs.
They recognize antigens and produce antibodies.
Cellular Immunity
T cells mature in the thymus and reside in blood and lymphoid organs.
T cell receptors (TCRs) recognize antigenic peptides processed by phagocytic cells.
T cells secrete cytokines instead of antibodies.
Cytokines: Chemical Messengers of Immune Cells
Cytokines are protein messengers produced in response to stimuli and regulate immune responses.
Interleukins (ILs): Communication between leukocytes.
Chemokines: Induce migration of leukocytes.
Interferons (IFNs): Interfere with viral infections.
Tumor Necrosis Factor (TNF): Involved in inflammation and autoimmune diseases.
Hematopoietic Cytokines: Control stem cell development into blood cells.
Antigens and Antibodies
Antigens
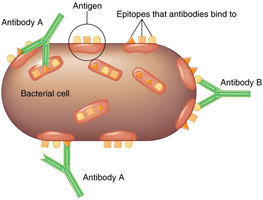
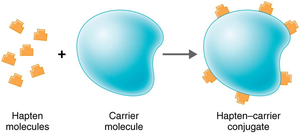
Antigens are substances that provoke an immune response, usually components of microbes or foreign substances. Antibodies interact with specific regions called epitopes (antigenic determinants). Haptens are small molecules that become antigenic only when attached to carrier molecules.
Antibody Structure and Function
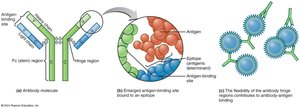
Antibodies (immunoglobulins, Ig) are compact, soluble proteins that recognize and bind to specific antigens. Each antibody has a valence (number of antigen-binding sites), typically two (bivalent).
Composed of two identical light chains and two identical heavy chains joined by disulfide bonds.
Variable (V) regions at the ends bind epitopes; constant (Fc) region is the stem.
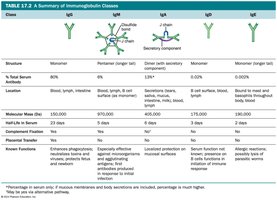
Five classes: IgG, IgM, IgA, IgD, IgE.
Classes of Antibodies
IgG: Monomer; 80% of serum antibodies; crosses placenta, triggers complement, enhances phagocytosis, neutralizes toxins/viruses.
IgM: Pentamer; 6% of serum antibodies; causes agglutination, activates complement, first response to infection.
IgA: Monomer in serum, dimer in secretions; 13% of serum antibodies; protects mucous membranes.
IgD: Monomer; 0.02% of serum antibodies; function not well-defined, may initiate immune response on B cells.
IgE: Monomer; 0.002% of serum antibodies; involved in allergic reactions and defense against parasitic worms.
Class | Structure | Total Serum Antibody (%) | Location | Known Functions |
|---|---|---|---|---|
IgG | Monomer | 80% | Blood, lymph, intestine | Enhances phagocytosis; neutralizes toxins and viruses; protects fetus and newborn |
IgM | Pentamer | 6% | Blood, lymph, B cell surface | Effective against microorganisms; agglutinating antigens; first produced in response to infection |
IgA | Dimer | 13% | Secretions, blood, lymph | Localized protection on mucosal surfaces |
IgD | Monomer | 0.02% | B cell surface, blood, lymph | Initiation of immune response |
IgE | Monomer | 0.002% | Mast cells, basophils, blood | Allergic reactions; lysis of parasitic worms |
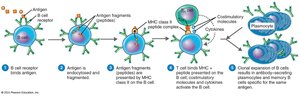
Humoral Immunity Response Process
Clonal Selection and Expansion
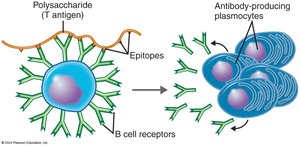
B cells interact with antigens in lymphoid organs. Each B cell has surface immunoglobulins as antigen receptors. Clonal selection occurs when a B cell receptor binds its antigen, leading to clonal expansion and differentiation into plasmocytes (antibody-secreting cells) and memory B cells.
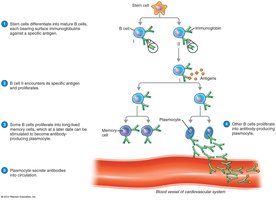
T-Dependent and T-Independent Antigens
T-Dependent Antigens: Require T helper cell assistance; usually proteins.
T-Independent Antigens: Do not require T cell help; often polysaccharides.
Antibody Diversity
Humans can produce millions of different antibodies due to gene segment rearrangement in immunoglobulin genes. Clonal deletion removes self-reactive B cells.
Results of Antigen–Antibody Interaction
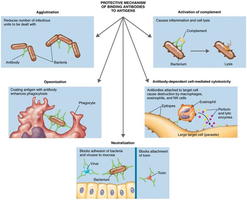
Protective Mechanisms
Antigen–antibody complexes protect the host by tagging foreign molecules for destruction. Key outcomes include:
Agglutination: Clumping of antigens.
Opsonization: Coating antigens to enhance phagocytosis.
Antibody-dependent cell-mediated cytotoxicity: Destruction by immune cells.
Neutralization: Blocking pathogen attachment.
Activation of complement: Leads to inflammation and cell lysis.
Cellular Immunity Response Process
T Cell Functions and Antigen-Presenting Cells (APCs)
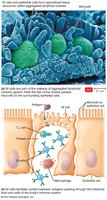
T cells combat intracellular pathogens and abnormal cells. They mature in the thymus and migrate to lymphoid tissues. Pathogens entering the gastrointestinal tract pass through M cells, which transfer antigens to lymphocytes and APCs.
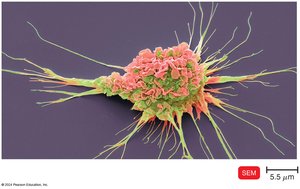
Types of Antigen-Presenting Cells
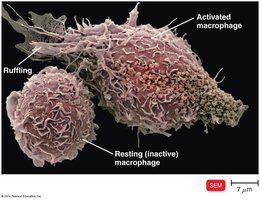
Dendritic Cells: Engulf and degrade microbes, display antigens to T cells.
Macrophages: Activated by cytokines or antigen ingestion, present antigens to T cells.
B Cells: Also act as APCs.
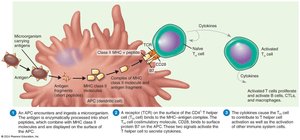
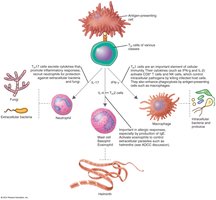
Classes of T Cells
T Helper Cells (CD4+): Activate B cells, other T cells, and macrophages via cytokines.
Cytotoxic T Lymphocytes (CTL, CD8+): Kill infected or abnormal cells by inducing apoptosis.
T Regulatory Cells: Suppress immune responses against self, protect intestinal bacteria and fetus.
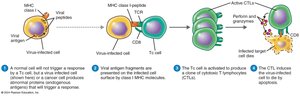
Cytotoxic T Lymphocyte Mechanism
CTLs recognize infected cells via MHC class I and antigenic peptide, then induce apoptosis using perforin and granzymes.
Nonspecific Cells and Extracellular Killing
Natural Killer (NK) Cells
Destroy virus-infected cells, tumor cells, and large parasites.
Not antigen-specific; detect cells lacking MHC class I.
Induce apoptosis by forming pores in target cells.
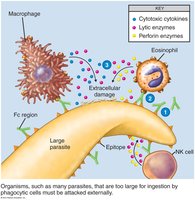
Antibody-Dependent Cell-Mediated Cytotoxicity (ADCC)
Protozoans and helminths are too large for phagocytosis. Antibodies coat the target cell, and immune cells (NK cells, macrophages, eosinophils) attach to Fc regions, releasing chemicals to lyse the target.
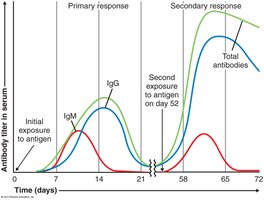
Immunological Memory
Primary vs. Secondary Immune Response
The primary response occurs on first exposure to an antigen, while the secondary (anamnestic) response is faster, stronger, and longer-lasting due to memory cells. Class switching from IgM to IgG, IgE, or IgA occurs during secondary response. Antibody titer reflects the intensity of the humoral response.
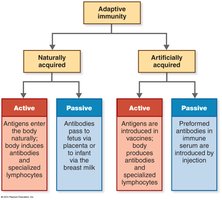
Types of Adaptive Immunity
Four Types of Adaptive Immunity
Naturally Acquired Active Immunity: Resulting from infection.
Naturally Acquired Passive Immunity: Antibodies passed from mother to fetus or infant.
Artificially Acquired Active Immunity: Injection of vaccination.
Artificially Acquired Passive Immunity: Injection of antibodies.
Summary: Dual Nature of Adaptive Immune System
The adaptive immune system consists of humoral and cellular branches, each controlling different types of pathogens. Humoral immunity targets freely circulating pathogens, while cellular immunity controls intracellular pathogens. Both branches involve memory cell formation for rapid secondary responses.