 Back
Backlec 23:Biofilms: Structure, Function, and Clinical Relevance
Study Guide - Smart Notes

Biofilms: Structure, Function, and Clinical Relevance
Definition and Importance of Biofilms
Biofilms are organized communities of microorganisms, such as bacteria or fungi, that adhere to surfaces and are embedded within a self-produced matrix of extracellular polymeric substances (EPS). This matrix provides protection, enhances survival under adverse conditions, and significantly increases resistance to antimicrobial agents and host immune responses.
Biofilm Matrix: Composed of polysaccharides, proteins, and extracellular DNA (eDNA).
Antibiotic Resistance: Biofilm-associated cells can be up to 1,000 times more resistant to antibiotics than planktonic (free-floating) cells.
Clinical Relevance: Biofilms are implicated in chronic infections and device-related complications.
Where Biofilms Are Found
Biofilms are ubiquitous and can form on nearly any surface exposed to water or moisture, including biological tissues and medical devices.
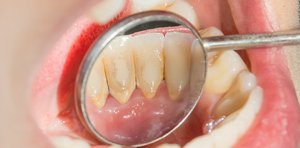
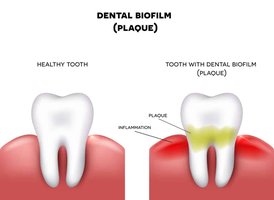
Human Body: Dental plaque, mucosal surfaces (respiratory tract, gut, vagina), and medical implants (catheters, heart valves, pacemakers, artificial joints).
Beneficial Biofilms: Lactobacilli in the vagina protect against pathogenic microbes.
Harmful Biofilms: Chronic lung infections in cystic fibrosis patients, persistent device-related infections.
Biofilm Life Cycle
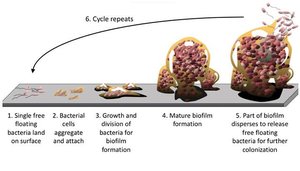
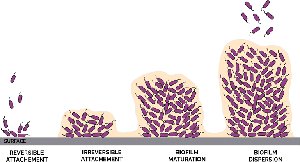
The formation and development of a biofilm follow a highly organized, multi-stage process, often described as a microbial city with division of labor and communication.
Stage 1: Initial Attachment (Reversible) – Free-floating bacteria land on a surface and loosely attach using structures like pili or flagella.
Stage 2: Irreversible Adhesion – Bacteria firmly attach and begin producing EPS, anchoring themselves and each other.
Stage 3: Maturation I (Microcolony Formation) – Bacteria multiply, forming microcolonies and initiating quorum sensing for coordinated growth.
Stage 4: Maturation II (3D Structure) – Biofilm develops complex architecture with water channels for nutrient and waste transport; protective matrix thickens.
Stage 5: Dispersion – Cells are released to colonize new surfaces, restarting the cycle.
Biofilm Differentiation and Communication
Within a biofilm, cells differentiate into specialized roles and communicate via chemical signals, enabling coordinated behavior and survival.
Division of Labor:
Fast-growing cells: Located on the periphery, focus on expansion.
Matrix producers: Synthesize EPS for structural integrity and protection.
Persister cells: Deep within the biofilm, enter dormancy and exhibit high antibiotic resistance.
Disperser cells: Facilitate biofilm spread under changing conditions.
Quorum Sensing (QS): Cell-to-cell communication using autoinducers to coordinate gene expression and group behaviors.
Quorum Sensing Signaling Molecules
Acyl-homoserine lactones (AHLs): Used by Gram-negative bacteria; synthesized by LuxI, detected by LuxR.
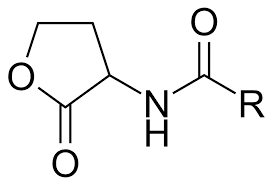
Autoinducing peptides (AIPs): Used by Gram-positive bacteria; processed and released to trigger gene expression.
AI-2 (Autoinducer-2): Universal signal for interspecies communication.
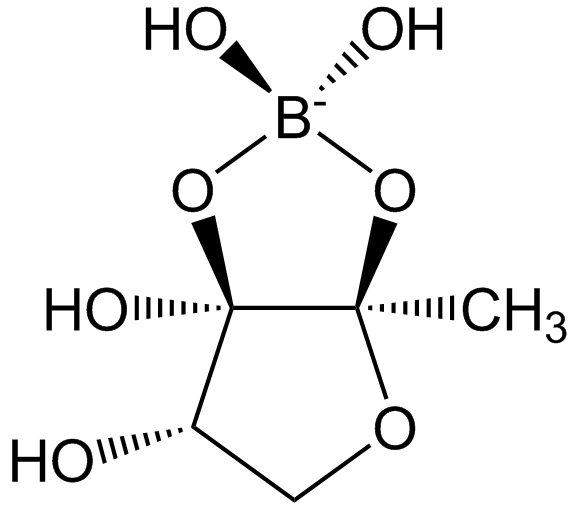
Quorum Sensing Feedback Loop
Basal production: Bacteria release small amounts of signals.
Accumulation: Signals build up as population grows.
Threshold (quorum): Once a critical concentration is reached, bacteria detect the signal.
Autoinduction: Triggers synchronized gene expression and further signal production.
Critical Tasks Managed by Quorum Sensing
Matrix construction
Structural organization
Virulence factor production
Dispersion
Quorum Quenching: Disrupting Bacterial Communication
Quorum quenching (QQ) strategies aim to interfere with bacterial communication, reducing virulence and biofilm formation without directly killing bacteria.
Signal degradation: Enzymes break down autoinducers.
Receptor blockers: Molecules prevent signal detection.
Natural inhibitors: Compounds from garlic, turmeric, and clove oil disrupt QS.
Pseudomonas aeruginosa and Quorum Sensing
Pseudomonas aeruginosa is a model organism for studying biofilm formation and QS, especially in chronic infections such as those affecting cystic fibrosis patients.
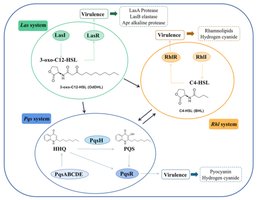
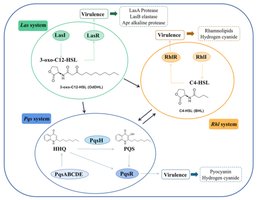
Multi-layered QS Network: Four interconnected systems regulate virulence and biofilm formation: Las, Rhl, PQS, and IQS.
Las system: Master regulator using 3-oxo-C12-HSL and LasR.
Rhl system: Controls chronic infection factors using C4-HSL and RhlR.
PQS system: Links Las and Rhl, regulates biofilm and iron uptake.
IQS system: Responds to environmental stress.
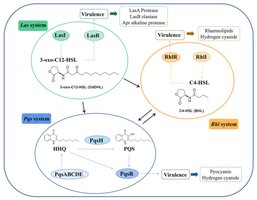
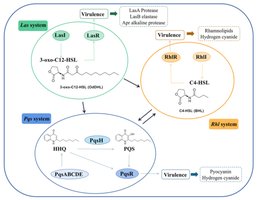
Host Interaction and Immune Evasion
Signal integration: Detects host molecules to enhance QS.
Immune evasion: QS molecules can weaken host defenses and damage tissues.
Treatment Strategies for Pseudomonas aeruginosa Biofilms
Biofilms formed by P. aeruginosa are highly resistant to treatment, requiring combined approaches.
Physical disruption: Removal or debridement of infected tissue or devices.
Enzymatic "slime breakers": Enzymes like DNase degrade the biofilm matrix.
Combination antibiotics: High-dose or inhaled antibiotics, often used together.
Topical treatments: Acetic acid and medical-grade honey disrupt biofilms.
Biofilms and "Permastink" in Synthetic Fabrics
Biofilms contribute to persistent odors in synthetic fabrics by forming protected microbial communities within fibers, resistant to normal washing.
Coordinated defense: QS triggers EPS production, anchoring bacteria to fibers.
Metabolic switch: QS induces breakdown of sweat into smelly molecules (e.g., isovaleric acid).
Re-stink effect: Residual bacteria reactivate upon wearing, causing odor recurrence.
Synthetic fabric properties: Oil-trapping and microstructure favor biofilm formation.
Strategies to Remove Biofilms from Fabrics
Biofilm disruptors: Enzyme-based laundry products break down EPS, allowing detergents to remove bacteria and residues.

High temperature: Washing at elevated temperatures helps degrade biofilm proteins.

Acidic rinses: White vinegar dissolves oils and weakens biofilm structure.

Summary Table: Biofilm Life Cycle Stages
Stage | Description |
|---|---|
Initial Attachment | Reversible binding of bacteria to surface |
Irreversible Adhesion | Firm attachment and EPS production |
Maturation I | Microcolony formation and quorum sensing |
Maturation II | 3D structure development, water channels |
Dispersion | Release of cells to colonize new surfaces |
Key Equations and Concepts
Quorum Sensing Threshold:
Biofilm Resistance:
Additional info:
Biofilm formation is a major topic in microbial cell structure, microbial growth, microbial regulatory systems, and microbial infection/pathogenesis.
Understanding biofilms is critical for developing new antimicrobial strategies and improving clinical outcomes in chronic and device-related infections.
