 Back
BackBlood Collection Equipment and Additives: Principles and Applications in Microbiology and Clinical Laboratory Science
Study Guide - Smart Notes

Blood Collection Equipment for Venipuncture and Capillary Specimens
Introduction to Blood Collection Equipment
Blood collection is a fundamental procedure in clinical laboratories, including microbiology, for diagnostic and research purposes. The equipment used must ensure specimen integrity, patient safety, and accurate test results. Blood can be collected via venipuncture, skin puncture, or arterial puncture (the latter typically performed by specialized personnel).
Venipuncture: Collection of blood from a vein, most common for laboratory testing.
Skin puncture: Collection from a finger or infant’s heel, used when venipuncture is not feasible.
Arterial puncture: Used for arterial blood gases, typically by nurses or IV teams.
Essential Venipuncture Equipment
Vacuum tubes (evacuated tubes)
Safety-needle collection devices (adapter, holder)
Tourniquet
Antiseptic supplies (70% alcohol, chlorhexidine gluconate)
Labeling supplies (permanent marker, labels)
Gloves
Transport trays
Gauze, wraps, tape, bandages
Sharps container for safe disposal
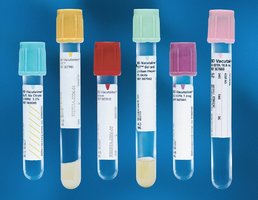
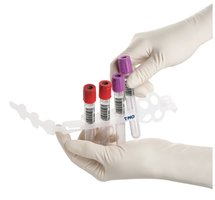
Vacuum (Evacuated) Tube System
Principle and Components
The vacuum tube system is the most direct, efficient, and safest method for obtaining blood specimens. It consists of an evacuated tube, a double-pointed needle, and a safety plastic holder (adapter). One end of the needle enters the vein, while the other pierces the tube cap, allowing the vacuum to aspirate blood into the tube.
Advantages: Minimizes exposure to blood, reduces contamination risk, and allows for multiple samples with one puncture.
Common brand: BD Vacutainer.
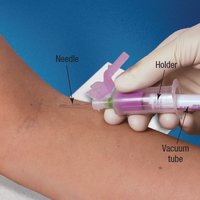
Needle Shielding Safety Devices
Active devices: Require manual activation (e.g., covering the needle or pressing a button).
Passive devices: Automatically shield the needle after blood collection, enhancing safety.

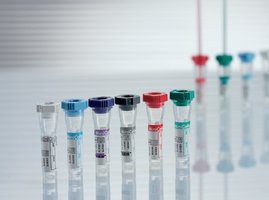
Blood Collection Tubes and Additives
Tube Sizes and Materials
Size: Defined by external diameter, length (mm), and maximum volume (mL; typically 1.8–10 mL).
Material: Most tubes are plastic to reduce breakage risk; all are sterile inside.
Color Coding: Tube caps are color-coded according to additive, following Clinical Laboratory Standards Institute (CLSI) guidelines.
Filling and Handling
Premeasured vacuum ensures precise blood volume; tubes must be filled to the indicated line to maintain correct blood-to-additive ratio.
Loss of vacuum can occur due to expiration, improper handling, or storage issues.
Specimens may be processed as serum, plasma, or whole blood, depending on the test.
Additives in Blood Collection Tubes
Additives: Substances added to alter the specimen for laboratory analysis or handling (e.g., gels, clot activators, anticoagulants).
Anticoagulants: Prevent blood clotting by various mechanisms; must be mixed immediately after collection (5–8 gentle inversions).
Preservatives: Extend the lifespan and metabolic activity of cells in the sample.
Types of Anticoagulants and Their Mechanisms
ACD (acid citrate-dextrose): Used for blood donations; preserves RBC function.
Oxalates, citrates, EDTA: Prevent clotting by binding calcium; not suitable for calcium assays.
EDTA: Prevents platelet aggregation; preserves cell morphology for hematology.
Heparin: Inactivates thrombin and Factor X; used for plasma/whole blood assays.
Color Codes and Applications of Blood Collection Tubes
Tube Color | Additive | Common Use |
|---|---|---|
Yellow | SPS or ACD | Blood cultures, HLA typing, paternity, organ transplant compatibility |
Light Blue | Sodium citrate | Coagulation studies (PT, APTT) |
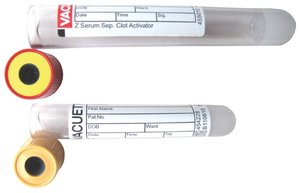
Red | None | Serum collection |
Gold/Speckled | Polymer gel | Serum separation |
Green | Heparin | Plasma/whole blood assays |
Purple/Lavender | EDTA | Hematology, molecular diagnostics |
Pink | EDTA | Blood bank, viral studies |
Gray | Potassium oxalate, sodium fluoride | Glucose testing (glycolytic inhibition) |
Royal Blue | None or EDTA | Trace elements, toxicology |
Tan | EDTA | Lead testing |
Black | Buffered sodium citrate | ESR (erythrocyte sedimentation rate) |
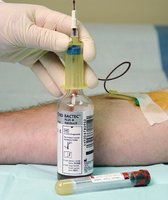


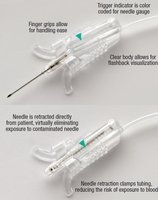
Safety Syringes and Needle Devices
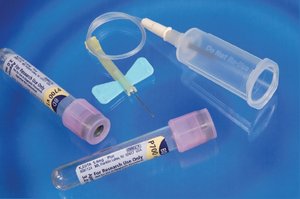
Safety Syringes
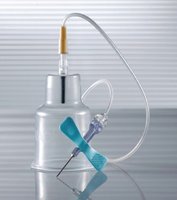
Safety syringes are used for patients with fragile veins or for blood collection from central venous catheters. They consist of a needle, safety cover, hub, barrel, and plunger. After collection, the needle is shielded and disposed of in a sharps container. Blood is transferred to tubes using a blood-transfer device.


Needle Gauge and Length
Gauge: Indicates needle diameter; lower gauge = larger diameter.
16–18 gauge: Used for blood donation.
21–23 gauge: Used for routine laboratory blood collection.
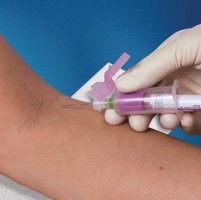
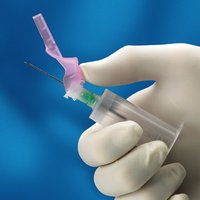

Butterfly Needle (Blood Collection Set)
Also known as a safety winged infusion set, the butterfly needle is commonly used for intravenous access, especially in small or fragile veins. It features a safety shield that covers the needle after use.
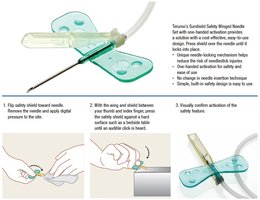
Sharps Disposal
All needles and sharps must be discarded in rigid, leak-proof, plastic containers (usually orange or red) and treated as biohazardous waste.

Tourniquets and Vein Location Devices
Tourniquets
Used to slow venous blood flow and aid in vein location.
Types: Pliable strap, Velcro, or blood pressure cuff (less common due to cleaning challenges).
Nonlatex disposable tourniquets are preferred; reusable tourniquets must be disinfected regularly.

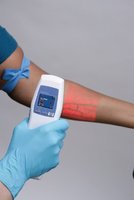
Vein Finders
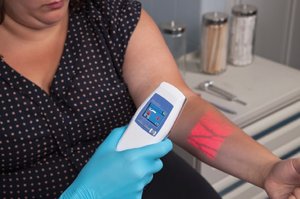
Venoscope: Noninvasive device to visualize veins for blood collection.
AccuVein: Portable, handheld device that projects vein patterns onto the skin for easier access.


Gloves, Antiseptics, and Other Supplies
Gloves
Mandatory for all blood collection procedures.
Do not use powdered gloves; change gloves between patients and never reuse.
Antiseptics, Gauze, and Bandages
Essential for site preparation and post-collection care.
Common antiseptics: 70% isopropyl alcohol, iodine, chlorhexidine (especially for blood cultures).
Microcollection Equipment
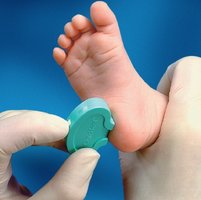
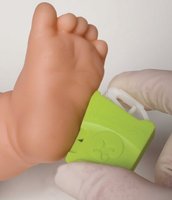
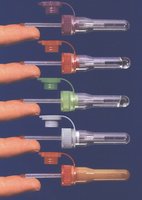
Skin Puncture Devices
Used primarily for infants or when venipuncture is not feasible.
Penetration depth for infant heel sticks should be less than 2.0 mm to avoid bone injury.
Common devices: BD Quikheel, BD Microtainer, Terumo Capiject, Tenderlett, Sarstedt Safety Lancet, Greiner Bio-One, Natus Medical NeatNick.


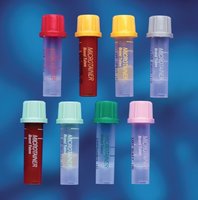
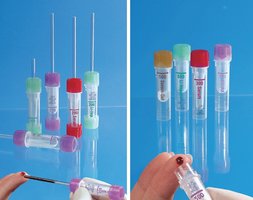
Microcontainers and Capillary Tubes
Plastic microhematocrit capillary tubes (red band = heparin, blue band = none).
Microcollection containers are color-coded to match vacuum tube protocols.
Brands: BD Microtainer, SAFE-T-FILL, Microvette, CAPIJECT, Greiner Bio-One MiniCollect, RNA Medical Safe-Wrap Combo.
BMP LeukoChek Microdilution System
Used for leukocyte and platelet counting.
Disposable, self-filling pipette with premeasured buffered ammonium oxalate solution.
Blood-Drawing Chairs and Specimen Collection Trays
Blood-Drawing Chairs
Designed for patient safety and comfort; features may include adjustable armrests, recliner options, and safety locks.
Specimen Collection Trays
Contain all necessary equipment for blood collection rounds.
Home health care trays must be enclosed, lockable, and labeled with a biohazard symbol.


Summary Table: Common Blood Collection Tubes and Their Uses
Tube Color | Additive | Primary Use |
|---|---|---|
Yellow | SPS/ACD | Blood cultures, HLA typing |
Light Blue | Sodium citrate | Coagulation studies |
Red | None | Serum chemistry |
Gold/Speckled | Polymer gel | Serum separation |
Green | Heparin | Plasma chemistry |
Purple/Lavender | EDTA | Hematology |
Pink | EDTA | Blood bank |
Gray | Potassium oxalate, sodium fluoride | Glucose/lactate |
Royal Blue | None/EDTA | Trace elements |
Tan | EDTA | Lead testing |
Black | Buffered sodium citrate | ESR |
Key Points for Microbiology Students
Proper selection and handling of blood collection equipment is critical for accurate laboratory results, including microbiological assays (e.g., blood cultures for septicemia).
Understanding tube additives and their mechanisms is essential to avoid test interference and ensure specimen integrity.
Safety protocols, including use of gloves, sharps disposal, and antiseptics, protect both patient and healthcare worker.
Additional info: Knowledge of blood collection equipment and additives is foundational for clinical microbiology, as specimen quality directly impacts the detection and identification of pathogens.
