 Back
BackChapter 3 - Observing Microorganisms Through a Microscope: Staining and Microscopy Techniques
Study Guide - Smart Notes

Observing Microorganisms Through a Microscope
Introduction to Light Microscopy
Light microscopy is a fundamental technique in microbiology, allowing for the visualization of microorganisms and their cellular structures. Proper specimen preparation and staining are essential for enhancing contrast and distinguishing cellular components.
Purpose: To observe microorganisms and their structures using magnification and illumination.
Key Components: Objective lenses, light source, condenser, specimen holder, and focusing knobs.
Application: Used in clinical and research laboratories for identification and study of microbes.

Preparation of Specimens for Light Microscopy
Specimens must be properly prepared to ensure accurate observation. This involves creating a smear, fixing it to the slide, and applying stains to enhance visibility.
Smear Preparation: A thin film of microorganisms is spread over a slide and allowed to air dry.
Fixation: The smear is fixed to the slide, often by heat, which kills the microorganisms and attaches them to the slide.
Importance: Fixing prevents loss of sample during staining and preserves cellular morphology.


Staining Techniques in Microbiology
Understanding Stains and Dyes
Stains, or dyes, are salts composed of a colored ion (chromophore) and an uncolored ion. They are used to enhance contrast and highlight specific structures within cells.
Basic Dyes: Chromophore is in the cation; stains the entire cell. Examples: crystal violet, safranin, methylene blue.
Acidic Dyes: Chromophore is in the anion; stains the background, leaving cells colorless (negative staining). Examples: eosin, nigrosin, india ink.
Simple Staining
Simple staining uses a single basic dye to color all cells, making it easier to observe cell shape and arrangement.
Procedure: Apply dye to a fixed smear; often use a mordant to intensify the stain.
Purpose: To visualize cell morphology and arrangement.
Differential Staining Techniques
Differential stains distinguish between different types of bacteria based on structural differences. The most common are the Gram stain and acid-fast stain.
Gram Stain
The Gram stain is a critical technique for classifying bacteria into Gram-positive and Gram-negative groups based on cell wall structure.
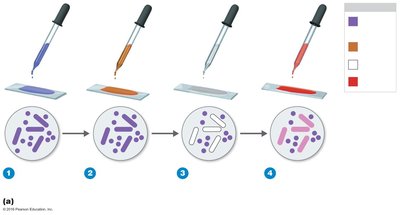
Procedure:
Apply crystal violet (primary stain).
Add iodine (mordant).
Alcohol wash (decolorizer).
Apply safranin (counterstain).
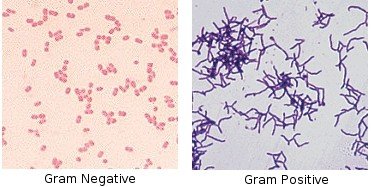
Results:
Gram-positive: Retain crystal violet, appear purple/blue.
Gram-negative: Lose crystal violet, take up safranin, appear red/pink.
Clinical Importance: Guides antibiotic treatment and identification of pathogens.
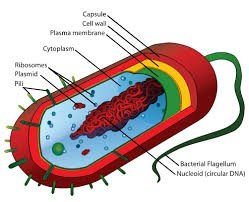
Bacterial Cell Wall Structure and Gram Stain Mechanism
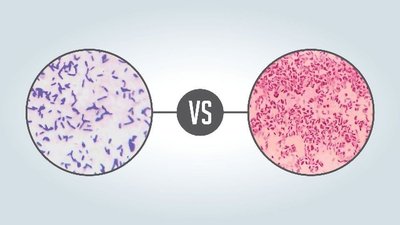
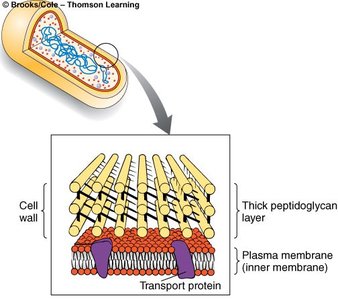
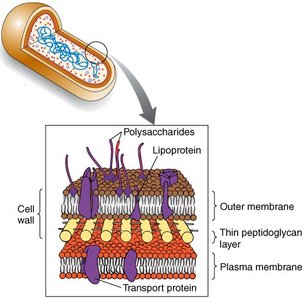
The cell wall composition determines the outcome of the Gram stain. Gram-positive bacteria have a thick peptidoglycan layer, while Gram-negative bacteria have a thin peptidoglycan layer and an outer membrane.
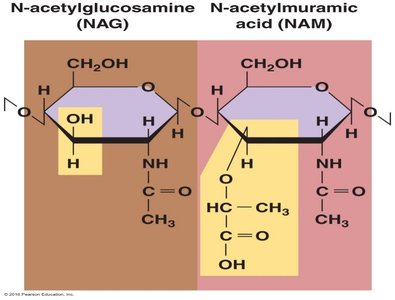
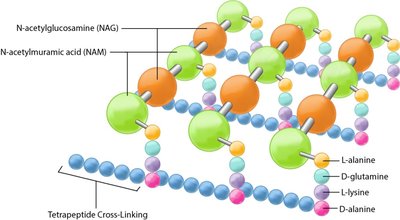
Peptidoglycan: A polymer of N-acetylglucosamine (NAG) and N-acetylmuramic acid (NAM) linked by β-1,4 bonds.
Gram-positive: Thick peptidoglycan, no outer membrane.
Gram-negative: Thin peptidoglycan, outer membrane present.
Comparison Table: Gram-Positive vs Gram-Negative Cell Walls
Feature | Gram-Positive | Gram-Negative |
|---|---|---|
Peptidoglycan Layer | Thick | Thin |
Outer Membrane | Absent | Present |
Stain Color | Purple/Blue | Red/Pink |
Clinical Relevance | Often more susceptible to antibiotics | Often more resistant due to outer membrane |
Acid-Fast Stain
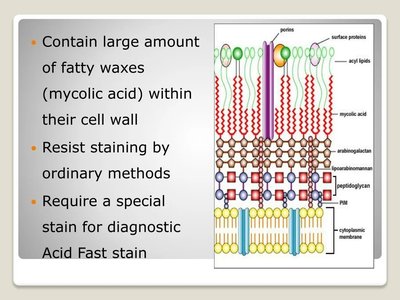
The acid-fast stain is used to identify bacteria with waxy cell walls containing mycolic acid, such as Mycobacterium and Nocardia.
Procedure:
Apply carbolfuchsin (primary stain).
Decolorize with acid-alcohol.
Counterstain with methylene blue.
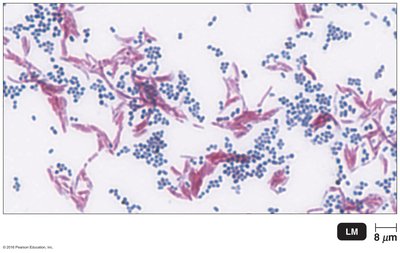
Results:
Acid-fast bacteria: Red
Non-acid-fast bacteria: Blue
Clinical Importance: Used for diagnosis of tuberculosis and leprosy.
Special Stains: Capsule, Endospore, and Flagella
Capsule Staining
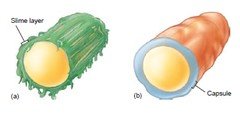
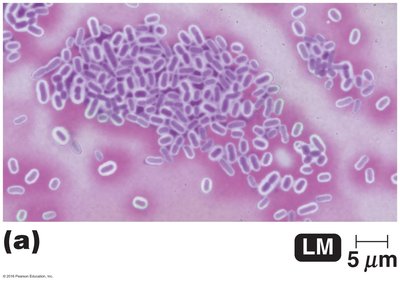
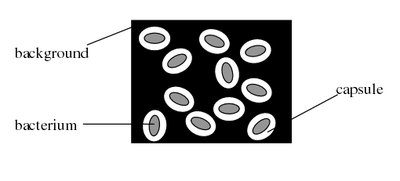
Capsule stains are used to visualize the glycocalyx, a gelatinous layer external to the cell wall. Capsules contribute to virulence by preventing phagocytosis and aiding in adherence.
Types: Capsule (organized, firmly attached) and slime layer (unorganized, loosely attached).
Stains Used: Acidic stains such as india ink and nigrosin for negative staining.
Clinical Relevance: Capsules are important in biofilm formation and immune evasion.

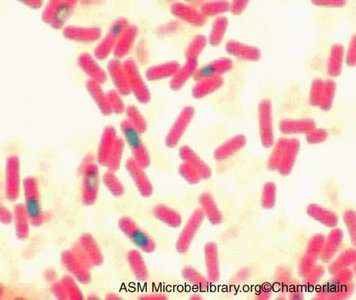
Endospore Staining
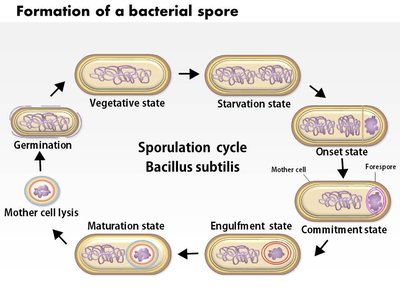
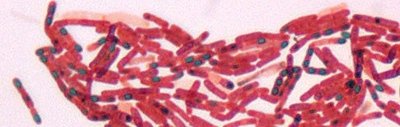
Endospores are highly resistant, dormant structures formed by certain bacteria, such as Bacillus and Clostridium. They require special staining techniques due to their impermeable coats.
Shaeffer-Fulton Method:
Stain with malachite green (with heat).
Decolorize with water.
Counterstain with safranin.
Results: Endospores appear green within red/pink vegetative cells.
Clinical Importance: Endospores are resistant to harsh conditions and are important in disease transmission.

Flagella Staining
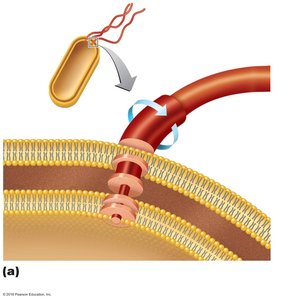
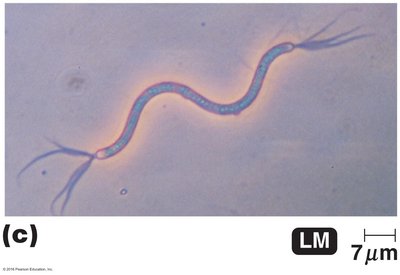
Flagella are locomotor structures that are not visible without special staining. The staining procedure uses carbolfuchsin and a mordant to increase the diameter of the flagella for observation.
Structure: Filament, hook, and basal body.
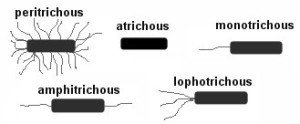
Arrangement: Can be monotrichous, lophotrichous, amphitrichous, or peritrichous.
Clinical Importance: Flagella contribute to motility and pathogenicity.

Summary Table: Staining Techniques
Stain | Purpose | Key Reagents | Result |
|---|---|---|---|
Simple Stain | Cell morphology | Basic dye | All cells colored |
Gram Stain | Cell wall classification | Crystal violet, iodine, alcohol, safranin | Gram-positive: purple; Gram-negative: pink |
Acid-Fast Stain | Identify acid-fast bacteria | Carbolfuchsin, acid-alcohol, methylene blue | Acid-fast: red; Non-acid-fast: blue |
Capsule Stain | Visualize capsule | India ink, nigrosin | Capsule appears as clear halo |
Endospore Stain | Identify endospores | Malachite green, safranin | Endospore: green; Vegetative cell: red |
Flagella Stain | Visualize flagella | Carbolfuchsin, mordant | Flagella visible |
Check Your Understanding
Why is the Gram stain so useful? It differentiates bacteria based on cell wall structure, guiding diagnosis and treatment.
Which stain would be used to identify microbes in the genera Mycobacterium and Nocardia? Acid-fast stain.
How do unstained endospores appear? Stained endospores? Unstained endospores are colorless; stained endospores appear green within red/pink cells.
Why doesn't a negative stain color a cell? The stain is repelled by the cell, coloring only the background.
Why is fixing necessary for most staining procedures? It attaches cells to the slide and preserves their structure.
Case Study Application
Gram stain results from a bronchial lavage can reveal whether the infecting organism is Gram-positive or Gram-negative, and its shape (coccus, bacillus, spirilli, comma). This information is critical for diagnosis and treatment of bacterial infections.
