 Back
BackChapter 7: The Control of Microbial Growth – Study Notes
Study Guide - Smart Notes

Chapter 7: The Control of Microbial Growth
7.1 The Terminology of Microbial Control
This section introduces essential terms and concepts related to the control of microbial growth, which are foundational for understanding sterilization, disinfection, and related practices in microbiology.
Sepsis: Refers to bacterial contamination. Common causative agents include Staphylococcus aureus, Streptococcus pyogenes, Klebsiella spp., Escherichia coli, and Pseudomonas aeruginosa. Sepsis is a life-threatening systemic response to infection.
Asepsis: The absence of significant contamination. Aseptic techniques are crucial in surgery to prevent microbial contamination of wounds.

Sterilization: The removal or destruction of all microbial life. Commercial sterilization targets Clostridium botulinum endospores in canned goods but may not achieve complete sterilization.
Disinfection: The destruction of only harmful microorganisms, typically on inanimate objects.
Antisepsis: The destruction of harmful microorganisms on living tissue.
Degerming: Mechanical removal of microbes from a limited area (e.g., alcohol swab before injection).
Sanitization: Lowering microbial counts on eating utensils to safe levels (e.g., high-heat dishwasher).
Biocide (Germicide): Agents that kill microbes; the suffix -cide means to kill.
Bacteriostasis: Inhibition, not killing, of microbes; the suffix -stat means to inhibit.
Aseptic Technique: Procedures that prevent contamination by unwanted microorganisms.





7.2 The Rate of Microbial Death
Understanding how microbial populations decline under antimicrobial treatment is essential for effective microbial control in clinical, industrial, and laboratory settings.
Effectiveness of Treatment Depends On:
Number of microbes present
Environmental factors (organic matter, temperature, biofilms)
Time of exposure
Microbial characteristics (e.g., endospore formation, cell wall structure)
Exponential Death Rate: Bacterial populations typically die at a constant rate when exposed to heat or chemicals.
Death Curve: Logarithmic plotting of microbial death shows a straight line, aiding in understanding sterilization and preservation processes.
Actions of Microbial Control Agents:
Alteration of membrane permeability
Damage to proteins (enzymes)
Damage to nucleic acids


7.4 Physical Methods of Microbial Control
Physical methods are widely used to control microbial growth in medical, laboratory, and food industry settings. These methods include heat, filtration, low temperature, high pressure, desiccation, and radiation.
Heat
Heat Denatures Enzymes: Leading to microbial death.
Thermal Death Point (TDP): Lowest temperature at which all cells in a liquid culture are killed in 10 minutes.
Thermal Death Time (TDT): Minimal time for all bacteria in a liquid culture to be killed at a given temperature.
Decimal Reduction Time (DRT): Time (in minutes) to kill 90% of a population at a given temperature.


Moist Heat Sterilization
Boiling: Kills vegetative forms of bacteria, viruses, and fungi within 10 minutes.
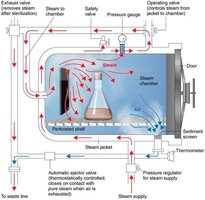
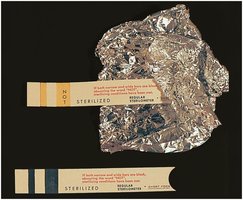
Autoclaving: Uses pressurized steam (121°C, 15 psi) to achieve sterilization. Large containers require longer times; test strips indicate sterility.
Pasteurization: High-temperature short-time (HTST, 72°C for 15 sec) reduces spoilage organisms and pathogens; ultra-high-temperature (UHT, 140°C for 4 sec) allows storage at room temperature.




Dry Heat Sterilization
Kills by Oxidation: Methods include flaming, incineration, and hot-air sterilization.

Filtration
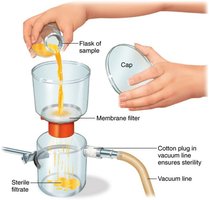
Filtration: Physical removal of microbes by passage through a filter. Used for heat-sensitive materials. HEPA filters remove microbes >0.3 μm; membrane filters can remove viruses and large proteins.
Other Physical Methods
Low Temperature: Bacteriostatic effect (refrigeration, deep-freezing, lyophilization).
High Pressure: Denatures proteins; endospores are resistant.
Desiccation: Absence of water prevents metabolism.
Osmotic Pressure: High salt/sugar concentrations cause plasmolysis.


Radiation
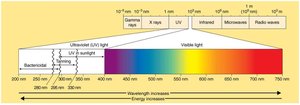
Ionizing Radiation: (X-rays, gamma rays, electron beams) damages DNA by causing lethal mutations.
Nonionizing Radiation: (UV, 260 nm) damages DNA by creating thymine dimers.
Microwaves: Kill by heat, not especially antimicrobial.
7.5 Chemical Methods of Microbial Control
Chemical agents are widely used to control microbial growth on surfaces, in solutions, and on living tissues. Their effectiveness depends on several factors and can be evaluated by laboratory tests.
Principles of Effective Disinfection
Concentration of disinfectant
Presence of organic matter
pH of the environment
Time of exposure
Use-Dilution and Disk-Diffusion Tests
Use-Dilution Test: Measures effectiveness of disinfectants against selected microbes.
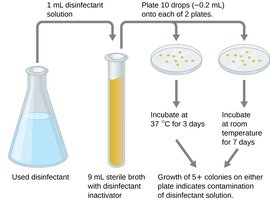
Disk-Diffusion Method: Filter paper disks with chemicals are placed on agar plates inoculated with bacteria; zones of inhibition indicate effectiveness.

Major Classes of Chemical Disinfectants and Antiseptics
Phenol and Phenolics: Disrupt plasma membranes and remain active in the presence of organic matter.

Bisphenols: Derivatives of phenol with two phenol groups; effective against gram-positive bacteria (e.g., hexachlorophene, triclosan).
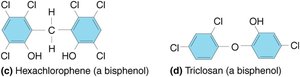
Biguanides: Broad-spectrum, especially effective against gram-positive bacteria (e.g., chlorhexidine).

Essential Oils: Plant-derived, primarily active against gram-positive bacteria due to phenolics and terpenes.
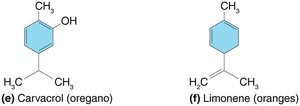

Halogens: Iodine (tincture, iodophor) and chlorine (bleach, chloramine) are strong oxidizing agents that disrupt proteins and membranes.


Alcohols: Denature proteins and dissolve lipids; ineffective against endospores and nonenveloped viruses. Common types: ethanol, isopropanol.
Heavy Metals: Oligodynamic action; denature proteins (e.g., silver nitrate, mercuric chloride, copper sulfate, zinc chloride).


Surface-Active Agents: Soaps and detergents mechanically remove microbes; quaternary ammonium compounds (quats) are bactericidal against gram-positive bacteria.



Chemical Food Preservatives: Sulfur dioxide, organic acids (sorbic, benzoic, calcium propionate), and nitrites/nitrates prevent spoilage and endospore germination.

Antibiotics: Bacteriocins (e.g., nisin, natamycin) prevent spoilage in cheese.


Aldehydes: Inactivate proteins by cross-linking; used for preserving specimens and sterilizing medical equipment (e.g., glutaraldehyde, formaldehyde).

Chemical Sterilization
Gaseous Sterilants: Ethylene oxide and formaldehyde gas sterilize heat-sensitive materials by alkylation (cross-linking nucleic acids and proteins).
Plasma Sterilization: Uses electrically excited gas (e.g., H2O2 plasma) to generate free radicals that destroy microbes; suitable for tubular instruments.
Supercritical Fluids: Combine properties of gases and liquids; used for sterilizing medical implants.
Peroxygens: Oxidizing agents (e.g., hydrogen peroxide, peracetic acid) used for surfaces and food packaging.
7.6 Microbial Characteristics and Microbial Control
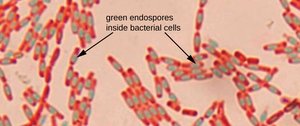
The effectiveness of chemical and physical methods depends on the type of microbe. Endospores and mycobacteria are particularly resistant, while gram-negative bacteria are more resistant to chemical biocides than gram-positive bacteria due to their outer membrane structure.
Summary Table: Key Terms in Microbial Control
Term | Definition | Example/Application |
|---|---|---|
Sterilization | Destruction/removal of all microbial life | Autoclaving surgical instruments |
Disinfection | Destruction of harmful microbes on surfaces | Bleach on countertops |
Antisepsis | Destruction of harmful microbes on living tissue | Alcohol swab on skin |
Degerming | Mechanical removal of microbes | Handwashing |
Sanitization | Lowering microbial counts to safe levels | Dishwasher cleaning utensils |
Biocide/Germicide | Agent that kills microbes | Phenol, chlorine |
Bacteriostasis | Inhibiting, not killing, microbes | Refrigeration |
Asepsis | Absence of contamination | Sterile surgical field |
Additional info: This guide expands on the original notes with definitions, examples, and context for each method and term, ensuring a comprehensive and self-contained study resource for microbiology students.
