 Back
BackConcepts of Infectious Disease: Host-Microbe Interactions, Pathogenesis, and Epidemiology
Study Guide - Smart Notes

Concepts of Infectious Disease
Introduction to Host-Microbe Relationships
Infectious diseases arise from complex interactions between hosts (animals, plants, or humans) and microorganisms. These interactions can be beneficial, neutral, or harmful, depending on the nature of the microbe and the host's response.
Host: An organism that provides a living environment for microorganisms.
Microbiota: The community of normal microbes living in and on the host, often contributing to health.
Pathogens: Microbes that cause disease by exploiting host resources and damaging tissues.
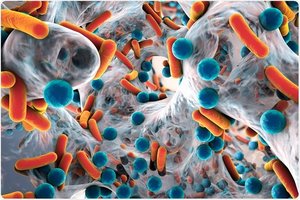
Host-Microbe Relationship (Microbiota)
Normal microbiota engage in mutualistic or commensal relationships with the host, providing essential functions and protection against pathogens.
Mutualism: Both host and microbe benefit (e.g., vitamin production, immune regulation).
Commensalism: Microbes benefit without affecting the host.
Colonization Resistance: Normal microbiota prevent pathogen colonization by competing for resources and producing inhibitory substances.
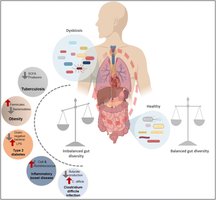
Host-Pathogen Relationship (Infection & Disease)
Pathogens establish parasitic relationships, benefiting at the host's expense and often causing disease. The outcome depends on pathogen virulence and host defenses.
Parasitism: Pathogen benefits, host is harmed.
Pathogenesis: The process by which pathogens cause disease, involving entry, replication, spread, and evasion of host defenses.
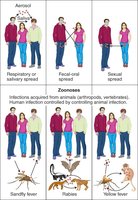
Portals of Entry for Infectious Agents
Major Routes of Entry
Microbes enter the host through specific anatomical sites, each associated with characteristic diseases.
Respiratory tract: Inhalation of aerosolized droplets (e.g., influenza, rhinovirus).
Gastrointestinal tract: Ingestion of contaminated food or water (e.g., typhoid, cholera).
Genital tract: Sexual transmission (e.g., HIV, herpes simplex virus).
Conjunctiva: Infection of the eye surface (e.g., conjunctivitis, Zika virus).
Parenteral route: Direct entry via breaks in the skin (e.g., insect bites, needle punctures).
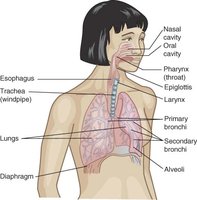
Respiratory Tract Entry
The respiratory tract is the most common portal of entry for airborne pathogens, which are inhaled into the lungs.
Examples: Rhinoviruses, coronaviruses, influenza viruses.
Gastrointestinal Tract Entry
Pathogens enter via ingestion and must survive harsh stomach acidity and digestive enzymes.
Examples: Salmonella typhi (typhoid), norovirus.

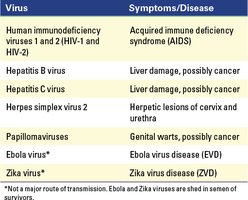
Genital Tract Entry
Sexually transmitted infections enter through abrasions or mucosal surfaces of the reproductive tract.
Examples: HIV, herpes simplex virus, papillomaviruses.
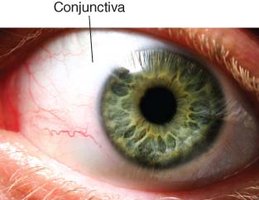
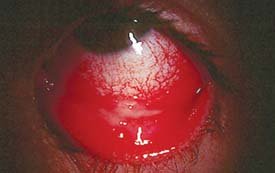
Conjunctiva Entry
The conjunctiva is a thin membrane covering the eye, susceptible to infection by various pathogens.
Diseases: Conjunctivitis (pink eye), epidemic keratoconjunctivitis, Zika virus-associated eye disease.
Mechanisms of Pathogenesis
Stages of Pathogenesis
Pathogenesis involves a series of steps by which a pathogen enters, establishes, and spreads within the host, ultimately causing disease.
Entry: Access to the host via a portal of entry.
Adhesion: Attachment to host cells using adhesins.
Invasion: Penetration and spread within host tissues.
Infection and Damage: Multiplication and tissue injury.
Evasion of Host Defenses: Avoidance of immune responses.
Exit and Transmission: Shedding and spread to new hosts.
Adhesion
Pathogens use specific molecules (adhesins) to bind to host cell receptors, enabling colonization and tissue targeting.
Example: Uropathogenic Escherichia coli use fimbriae to adhere to urinary tract epithelium.
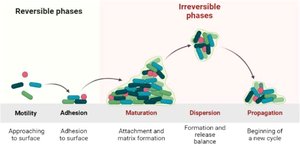
Invasion
After adhesion, pathogens may invade deeper tissues or enter host cells, often using enzymes to break down barriers.
Example: Streptococcus pyogenes produces hyaluronidase to degrade connective tissue.
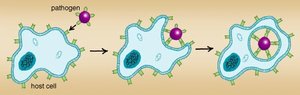
Infection and Damage
Pathogens multiply and cause tissue injury through direct cell destruction, toxin production, or immune-mediated damage.
Direct damage: Viral lysis of host cells.
Toxins: Diphtheria toxin inhibits protein synthesis.
Immune-mediated: Excessive inflammation (cytokine storm).
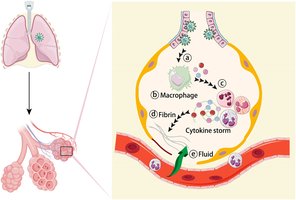
Evasion of Host Defenses
Pathogens employ strategies to avoid immune detection and destruction, such as capsules, antigenic variation, and intracellular survival.
Example: Neisseria gonorrhoeae changes surface proteins to evade antibodies.
Exit and Transmission
Pathogens exit the host via portals such as the respiratory tract (coughing/sneezing), gastrointestinal tract (feces), or skin, facilitating transmission to new hosts.

Epidemiology: Distribution and Control of Infectious Diseases
Introduction to Epidemiology
Epidemiology is the scientific study of disease distribution and determinants in populations. It informs public health interventions and policies.
Objectives: Identify health problems, determine causes, evaluate interventions, and guide resource allocation.

Key Epidemiological Terms
Endemic: Disease constantly present at low levels in a region.
Sporadic: Irregular, infrequent disease occurrence.
Epidemic: Sudden increase in cases above normal expectations.
Pandemic: Worldwide epidemic.
Morbidity: Illness or disease state.
Mortality: Deaths caused by a disease.
Incidence: Number of new cases in a time period.
Prevalence: Total number of cases at a given time.
Etiological agent: The causative pathogen.
Case definition: Criteria for identifying disease cases.
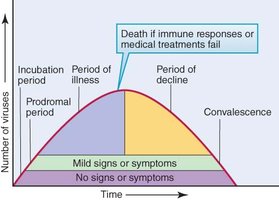
Incubation period: Time from infection to symptom onset.
Prodromal period: Early, mild symptoms.
Communicable period: Time when an individual is contagious.
Convalescence: Recovery phase after illness.
Mode of transmission: How disease spreads (direct/indirect).
Zoonosis: Disease transmissible from animals to humans.
Infectious dose: Minimum number of microbes needed to cause disease.
Virulence: Severity of disease caused by a pathogen.
Pathogenicity: Ability to cause disease.
R-nought (R0): Basic reproduction number, indicating transmission potential.
Modes of Transmission
Direct transmission: Physical contact (e.g., touching, kissing, sexual contact).
Indirect transmission: Via intermediates such as air, vectors (insects), vehicles (fomites), or ingestion.
Chain of Infection
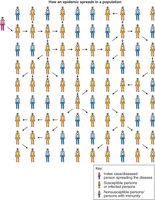
The chain of infection describes the sequence of events allowing infection to spread, including portals of exit and entry. Breaking the chain at any point can prevent disease transmission.
Concept of Herd Immunity
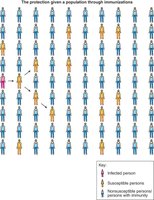
Herd immunity occurs when a large proportion of a population is immune (via vaccination or prior infection), reducing the likelihood of disease spread and protecting susceptible individuals.
Prevention and Containment of Contagious Diseases
Quarantine: Separation of exposed but healthy individuals to prevent disease spread.
Isolation: Separation of ill/infected individuals from healthy individuals.

Summary Table: Portals of Entry and Associated Diseases
Portal of Entry | Example Disease |
|---|---|
Respiratory tract | Influenza, COVID-19 |
Gastrointestinal tract | Typhoid, Cholera |
Genital tract | HIV, Herpes simplex |
Conjunctiva | Conjunctivitis, Zika virus |
Parenteral (skin break) | Rocky Mountain spotted fever, Hepatitis B/C |
Key Equations
Incidence Rate:
Prevalence Rate:
Basic Reproduction Number (R0):
Additional info: These notes integrate foundational concepts from microbiology, including host-microbe interactions, mechanisms of pathogenesis, and epidemiological principles, providing a comprehensive overview for exam preparation.
