 Back
BackControl of Microbial Growth: Methods and Principles
Study Guide - Smart Notes

Control of Microbial Growth
Key Terms and Definitions
Understanding the terminology is essential for discussing microbial control methods in microbiology.
Sterilization: The complete destruction or removal of all forms of microbial life, including endospores.
Disinfection: The destruction or removal of vegetative pathogens but not bacterial endospores, usually on inanimate objects.
Antisepsis/Degerming: The destruction or inhibition of microorganisms on living tissue (antisepsis) or mechanical removal of microbes from a limited area (degerming).
Sanitization: Lowering microbial counts on eating utensils to safe levels as determined by public health standards.
Bactericide: An agent that kills bacteria.
Bacteriostatic: An agent that inhibits the growth of bacteria without necessarily killing them.

Types of Microbes and Their Resistance
Relative Resistance of Microbial Forms
Microorganisms vary in their resistance to physical and chemical control methods. Understanding these differences is crucial for selecting appropriate sterilization or disinfection strategies.
Most Resistant: Bacterial endospores (e.g., Bacillus, Clostridium species)
Fairly Resistant: Mycobacterium, Staphylococcus, Pseudomonas, cysts, naked (non-enveloped) viruses
Least Resistant: Most vegetative cells (especially actively growing cells), enveloped viruses (exception: Hepatitis B virus)
Microbial Death
Definition and Kinetics
Microbial death refers to the permanent loss of reproductive capability under ideal growth conditions. Death occurs exponentially, meaning a constant proportion of cells die per unit time when exposed to a lethal agent.
Decimal Reduction Time (D-value): The time required to kill 90% of a microbial population at a given temperature.
Factors Affecting Microbial Death
Key Influencing Factors
Several factors influence the effectiveness of antimicrobial treatments:
Population Size: Larger populations require longer treatment times.
Population Composition: Different species and life stages (e.g., spores vs. vegetative cells) vary in susceptibility.
Concentration or Intensity of Agent: Higher concentrations or intensities generally increase effectiveness.
Duration of Exposure: Longer exposure increases microbial death.
Temperature: Higher temperatures often enhance the activity of chemical agents.
Local Environment: Presence of organic matter, pH, and other environmental factors can affect efficacy.
Physical Methods of Microbial Control
Temperature-Based Methods
Temperature is a critical factor in controlling microbial growth. Both high and low temperatures are used for different purposes.
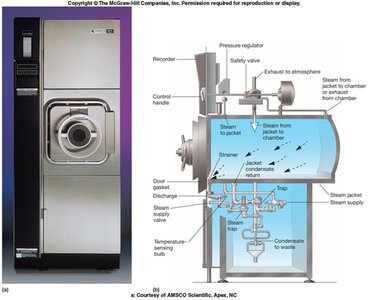
Autoclave: Uses pressurized steam (typically 121°C at 15 psi for 15-20 minutes) to achieve sterilization. Effective against all microbes, including endospores.
Pasteurization: Uses mild heat to reduce microbial load in food and beverages without damaging the product. Common protocols include 72°C for 15 seconds (HTST).
Dry Heat: Includes incineration and hot-air ovens. Incineration is used for sterilizing inoculating loops; hot-air ovens are used for glassware.
Boiling Water: Kills most vegetative cells and viruses but not endospores.
Low Temperatures: Refrigeration and freezing slow microbial growth but do not kill most microbes.

Filtration
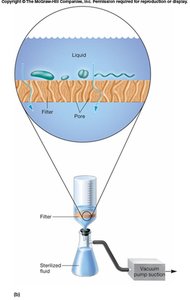
Filtration is used to physically remove microbes from liquids or air, especially for heat-sensitive materials.
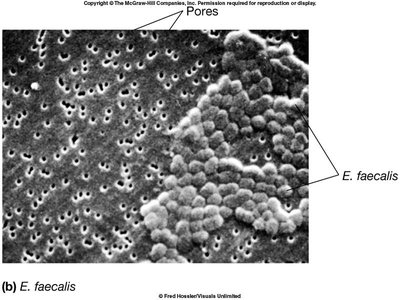
Membrane Filtration: Liquids are passed through filters with pores small enough to retain bacteria and larger microbes.
HEPA Filters: High-Efficiency Particulate Air filters are used in biological safety cabinets to remove airborne particles.

Radiation
Radiation methods are used for sterilization and disinfection, especially for heat-sensitive items.
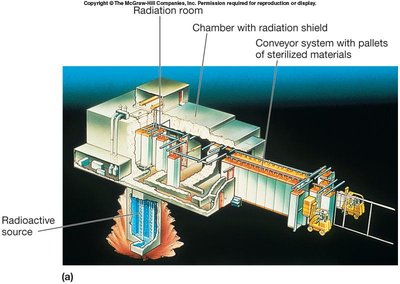
Ionizing Radiation: (e.g., X-rays, gamma rays) causes DNA damage and is highly penetrating. Used for sterilizing pharmaceuticals and medical supplies.
Non-ionizing Radiation: (e.g., UV light) causes DNA mutations but has poor penetration. Used for surface disinfection and air sterilization.

Summary Table: Physical Methods
The following table summarizes the main physical methods used to control microbial growth, their mechanisms, and preferred uses.
Method | Mechanism of Action | Comment | Preferred Use |
|---|---|---|---|
Moist heat (boiling, autoclaving, pasteurization) | Protein denaturation | Kills most pathogens; autoclaving is most effective | Media, glassware, food, beverages |
Dry heat (incineration, hot-air oven) | Oxidation, burning | Very effective for sterilization | Inoculating loops, glassware |
Filtration | Physical removal | Useful for heat-sensitive liquids | Culture media, antibiotics |
Low temperature | Decreased metabolism | Bacteriostatic | Food preservation |
Radiation | DNA damage | Ionizing for deep sterilization; UV for surfaces | Medical supplies, air, surfaces |

Chemical Methods of Microbial Control
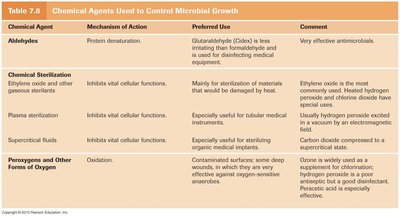
Major Classes of Chemical Agents
Chemical agents are widely used for disinfection, antisepsis, and sterilization. Selection depends on the target microbe, application, and safety considerations.
Phenolics: Disrupt plasma membranes and denature proteins. Used for surfaces and instruments.
Alcohols: Denature proteins and dissolve lipids. Effective against bacteria and fungi, not endospores.
Halogens: (e.g., iodine, chlorine) Oxidize cellular components. Used for water, skin, and surfaces.
Heavy Metals: (e.g., silver, mercury) Denature proteins. Used in antiseptics and preservatives.
Quaternary Ammonium Compounds: Disrupt membranes. Used for surface disinfection.
Aldehydes: Inactivate proteins by cross-linking. Used for medical equipment sterilization.
Ethylene Oxide: Gaseous sterilant for heat-sensitive materials.



Considerations for Disinfectant Use
When choosing and using disinfectants, several factors must be considered:
Nature of Microbes: Some microbes are more resistant than others.
Presence of Organic Matter: Organic material can inactivate disinfectants; cleaning is required before disinfection.
Concentration: The effectiveness of a disinfectant often depends on its concentration.
Application: Consider toxicity, compatibility with the item, temperature, and pH.
Summary of Microbial Control Methods
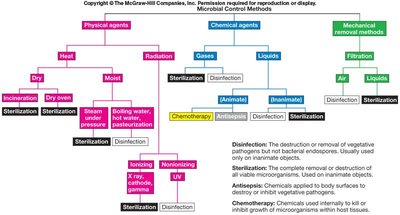
Classification of Methods
Microbial control methods can be classified as physical, chemical, or mechanical. The following diagram summarizes these approaches and their applications.

Decision: Sterilize or Disinfect?
Choosing the Appropriate Method
The choice between sterilization and disinfection depends on the intended use of the item, the risk of infection, and the resistance of potential contaminants. Critical items (e.g., surgical instruments) require sterilization, while non-critical items may only require disinfection.
Conclusion
Effective control of microbial growth is essential in healthcare, laboratory, and food industry settings. Understanding the principles, methods, and factors influencing microbial control enables the selection of appropriate strategies to ensure safety and prevent infection.
