 Back
BackControl of Microbial Growth: Principles, Methods, and Applications
Study Guide - Smart Notes

Control of Microbial Growth
Introduction
The control of microbial growth is a fundamental aspect of microbiology, essential for preventing infection, ensuring food safety, and maintaining sterile environments in clinical and laboratory settings. This topic covers the principles, terminology, and methods used to reduce or eliminate microbial populations.
Microbial Presence in Everyday Environments
Microbes are ubiquitous, colonizing various surfaces and environments, including vehicles, homes, and workplaces. Even frequently cleaned areas can harbor significant microbial populations.
Colony-Forming Units (CFUs): A measure of viable microbial cells capable of forming colonies.
Frequently touched surfaces: These often have higher microbial loads due to repeated contact.
Example: The center console of a car can have the highest CFUs due to spilled drinks and frequent handling.

Hygiene, Cleanliness, and Immune System Development
Maintaining basic hygiene is important, but excessive cleanliness may impact immune system development, especially in children. Exposure to environmental microbes can help train the immune system and reduce allergy risks.
Handwashing: Regular soap and water are sufficient for most situations; antimicrobial soaps are rarely needed.
Household Cleanliness: Basic hygiene is recommended, but some exposure to dirt is beneficial.
Pets: Early exposure to healthy pets may reduce allergy risk and strengthen immunity.
Microbial Death Rates and Principles of Control
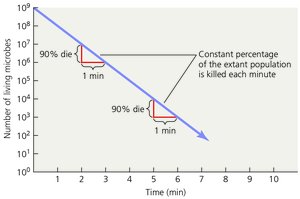
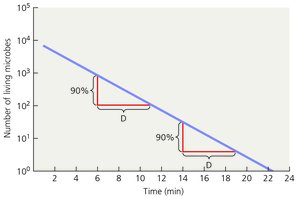
Microbial death is defined as the permanent loss of reproductive ability under ideal conditions. The rate of microbial death is often constant under specific conditions and can be plotted as a straight line on a semilogarithmic graph.
Microbial Death Rate: The percentage of microbes killed per unit time remains constant.
Decimal Reduction Time (D): The time required to reduce a microbial population by 90%.
Action of Antimicrobial Agents
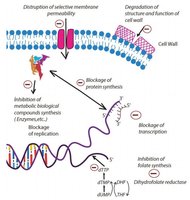
Antimicrobial agents act by disrupting cellular structures or interfering with metabolic processes. Their modes of action include:
Alteration of cell walls and membranes: Damaged cell walls lead to cell lysis; damaged membranes cause leakage of cellular contents.
Interference with proteins and nucleic acids: Denaturation of proteins and destruction of nucleic acids halt metabolism and reproduction.
Nonenveloped viruses: These are more resistant to harsh conditions than enveloped viruses.
Selection of Microbial Control Methods
Choosing an appropriate microbial control method depends on several factors:
Site to be treated: Some methods are unsuitable for living tissues or delicate objects.
Relative susceptibilities of microbes: Microbes vary in resistance to antimicrobial agents.
Environmental conditions: Temperature, pH, and organic materials can affect efficacy.
Microbe Type | Relative Resistance |
|---|---|
Prions | Most resistant |
Bacterial endospores | Very resistant |
Enveloped viruses | Most susceptible |
Vegetative bacteria | Low resistance |
Fungal spores | Intermediate resistance |
Protozoan cysts | High resistance |
Mycobacteria | High resistance |
Gram-positive bacteria | Low resistance |
Gram-negative bacteria | Intermediate resistance |

Biosafety Levels
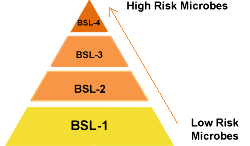
Laboratories are classified into four biosafety levels (BSL) based on the risk posed by the microbes handled:
BSL-1: Basic, for low-risk microbes (e.g., E. coli).
BSL-2: Moderate, for pathogens like Salmonella.
BSL-3: High, for airborne diseases like tuberculosis.
BSL-4: Maximum, for deadly viruses (e.g., Ebola).

Physical Methods of Microbial Control
Heat-Related Methods
Heat is a widely used method for microbial control, acting by denaturing proteins, disrupting membranes, and destroying nucleic acids.
Thermal Death Point (TDP): Lowest temperature that kills all cells in 10 minutes.
Thermal Death Time (TDT): Minimum time to sterilize at a set temperature.
Decimal Reduction Time (D): Time to reduce population by 90%.

Moist Heat Methods
Moist heat is more effective than dry heat for microbial control. Common methods include:
Boiling: Kills most vegetative cells, but not endospores or some viruses.
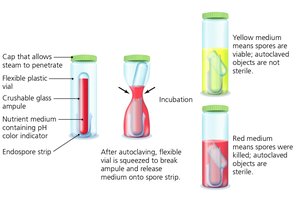
Autoclaving: Uses pressurized steam (121°C, 15 psi, 15 min) to achieve sterilization.
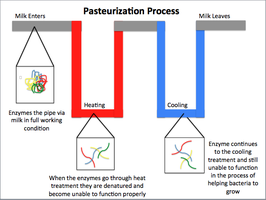
Pasteurization: Reduces microbial load in food and beverages without sterilizing.
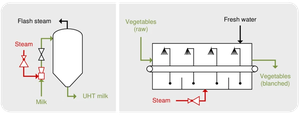
Ultra-high-temperature sterilization (UHT): 140°C for 1–3 seconds, allows storage at room temperature.






Dry Heat Methods
Dry heat is used for materials that cannot be sterilized with moist heat. It requires higher temperatures and longer times.
Incineration: Ultimate means of sterilization.
Direct flaming: Used for glass slides, scalpels, and culture tube mouths.
Hot air sterilization: Used for glassware and metal instruments.


Refrigeration and Freezing
Low temperatures slow microbial metabolism and growth. Refrigeration halts most pathogens, but some microbes can multiply in cold environments.
Slow freezing: More effective than quick freezing.
Organisms vary in susceptibility to freezing.
Desiccation and Lyophilization
Desiccation (drying) inhibits microbial growth by removing water. Lyophilization (freeze-drying) is used for long-term preservation, preventing ice crystal formation.
Filtration
Filtration removes microbes from liquids and gases by passing them through a filter with defined pore size.
Membrane filters: Trap microbes larger than the pore size.
HEPA filters: Used in biological safety cabinets, operating rooms, and isolation rooms.
Osmotic Pressure
High concentrations of salt or sugar create hypertonic environments, causing cells to lose water and inhibiting growth. Fungi are more resistant than bacteria to these conditions.
Radiation
Radiation is used to control microbial growth by damaging cellular components.
Ionizing radiation: Includes electron beams, gamma rays, and X-rays; creates ions that disrupt DNA and proteins.
Nonionizing radiation: Includes UV light; causes DNA damage (pyrimidine dimers) and is suitable for disinfecting surfaces and air.
Chemical Methods of Microbial Control
Categories of Antimicrobial Chemicals
Chemical agents are used as antiseptics and disinfectants. Major categories include:
Surfactants: Reduce surface tension; soaps and detergents are common examples.
Heavy metals: Denature proteins; examples include silver nitrate and copper.
Aldehydes: Cross-link functional groups to denature proteins and inactivate nucleic acids.
Gaseous agents: Used in closed chambers; examples include ethylene oxide.
Enzymes: Used for specific microbial control.
Phenol and phenolics: Disrupt cell membranes and denature proteins.
Alcohols: Denature proteins and disrupt membranes; not effective against spores.
Halogens: Damage enzymes; examples include iodine and chlorine.
Oxidizing agents: Kill by oxidation; examples include hydrogen peroxide and ozone.
Surfactants
Surfactants are surface-active chemicals that reduce surface tension, aiding in the removal of microbes from surfaces.
Soaps: Good degerming agents but not antimicrobial.
Detergents: Positively charged; disrupt cellular membranes.
Quaternary ammonium compounds (quats): Low-level disinfectants, safe for many applications.
Heavy Metals
Heavy-metal ions denature proteins and act as low-level bacteriostatic and fungistatic agents.
Silver nitrate: Used to prevent eye infections in newborns.
Copper: Controls algal growth in water systems.
Phenol and Phenolics
Phenol and phenolics denature proteins and disrupt cell membranes. They remain active in the presence of organic matter and are commonly used in healthcare settings.
Alcohols
Alcohols are intermediate-level disinfectants that denature proteins and disrupt membranes. They are more effective than soap for hand hygiene but do not kill spores.
Halogens
Halogens are intermediate-level antimicrobial chemicals that damage enzymes by denaturation. They are widely used for water treatment and disinfection.
Oxidizing Agents
Oxidizing agents kill microbes by oxidizing enzymes. Hydrogen peroxide, ozone, and peracetic acid are examples.
Aldehydes
Aldehydes cross-link functional groups to denature proteins and inactivate nucleic acids. Glutaraldehyde and formalin are commonly used.
Gaseous Agents
Gaseous agents are used in closed chambers to sterilize items. Ethylene oxide is a common example, used for heat-sensitive instruments.
Case Study: Foodborne Infection
Campylobacter jejuni and Raw Dairy Products
Consumption of raw (unpasteurized) milk and cheese can lead to foodborne infections, such as those caused by Campylobacter jejuni. This pathogen is commonly associated with raw dairy and can cause gastrointestinal illness.
Symptoms: Fever, abdominal cramps, diarrhea, sometimes with blood.
Diagnosis: Stool sample analysis.
Prevention: Pasteurization of dairy products.

Why Pasteurization is Important
Pasteurization is a heat treatment process that reduces microbial load in food and beverages, preventing foodborne illnesses. It is especially important for dairy products, which can harbor pathogens if consumed raw.
Summary Table: Physical and Chemical Methods of Microbial Control
Method | Mechanism | Application |
|---|---|---|
Heat (Moist/Dry) | Denatures proteins, disrupts membranes | Sterilization of lab equipment, food safety |
Filtration | Physical removal of microbes | Sterilization of heat-sensitive liquids |
Radiation | Damages DNA and proteins | Food preservation, surface sterilization |
Surfactants | Reduce surface tension, disrupt membranes | Hand hygiene, surface cleaning |
Heavy Metals | Denature proteins | Antimicrobial creams, water treatment |
Alcohols | Denature proteins, disrupt membranes | Skin antisepsis |
Halogens | Damage enzymes | Water disinfection, wound cleaning |
Oxidizing Agents | Oxidize enzymes | Surface sterilization, water treatment |
Aldehydes | Cross-link proteins and nucleic acids | Instrument sterilization |
Gaseous Agents | Cross-link proteins and DNA | Sterilization of heat-sensitive items |
Additional info: These notes expand on the original content by providing definitions, examples, and context for each method, making them suitable for exam preparation and self-study in a college microbiology course.
