 Back
BackControl of Microbial Growth: Principles, Methods, and Applications
Study Guide - Smart Notes

Control of Microbial Growth
Introduction
The control of microbial growth is a fundamental aspect of microbiology, essential for preventing infection, ensuring food safety, and maintaining sterile environments in clinical and laboratory settings. This module explores the principles, terminology, and methods used to control microbial populations, including both physical and chemical approaches.
Microbial Presence in Everyday Environments
Microbial Contamination in Cars
Microbes are ubiquitous and can be found in various environments, including vehicles. Studies have shown that frequently touched surfaces, such as the center console and door latch, harbor the highest concentrations of microbial colony-forming units (CFUs). Maintaining basic hygiene is important to reduce microbial load, but complete sterility is rarely achieved outside specialized settings.

Hygiene and Immune System Development
While cleanliness is important, excessive sterilization may impact immune system development, especially in children. Epidemiological data suggest that exposure to moderate levels of environmental microbes, such as through outdoor play and contact with pets, can help train the immune system and reduce allergy risk. Regular handwashing with soap and water is sufficient for most situations; antimicrobial soaps are generally unnecessary unless advised by a healthcare provider.
Microbial Control Terminology
Definitions
Sterilization: The complete elimination or destruction of all forms of microbial life, including endospores.
Disinfection: The elimination of most pathogenic microorganisms (excluding endospores) on inanimate objects.
Antisepsis: The reduction of microbial load on living tissue.
Sanitization: The reduction of microbial populations to safe levels as determined by public health standards.
Degerming: The mechanical removal of microbes from a limited area, such as skin before injection.
Principles of Microbial Control
Microbial Death Rates
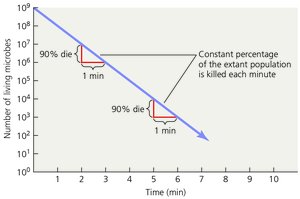
Microbial death is defined as the permanent loss of reproductive ability under ideal environmental conditions. The death rate is often constant for a given microorganism under specific conditions, and when plotted on a semilogarithmic graph, it produces a straight line. This concept is crucial for understanding the effectiveness of sterilization and disinfection processes.
Action of Antimicrobial Agents
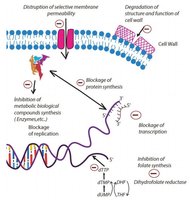
Antimicrobial agents act by:
Altering cell walls and membranes: Damage to the cell wall can cause cells to burst due to osmotic effects, while damage to the cytoplasmic membrane leads to leakage of cellular contents.
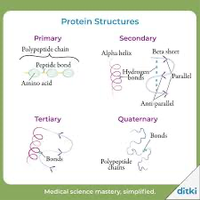
Interrupting cellular metabolism and reproduction: Agents may denature proteins or destroy nucleic acids, halting protein synthesis and producing fatal mutants.
Selection of Microbial Control Methods
Criteria for Choosing Methods
Ideal microbial control agents should be inexpensive, fast-acting, stable during storage, and harmless to humans, animals, and objects. However, no single method meets all criteria, so several factors are considered:
Site to be treated: The nature of the site (e.g., human tissue, medical instruments) determines the method used.
Relative susceptibilities of microbes: Microbes vary in their resistance to antimicrobial agents. For example, bacterial endospores and prions are highly resistant, while enveloped viruses are most susceptible.

Environmental Conditions
Temperature, pH, and the presence of organic materials can affect microbial death rates and the efficacy of antimicrobial methods. Organic materials may interfere with the penetration of heat, chemicals, and radiation, and can inactivate disinfectants.
Biosafety Levels
Laboratory Safety Levels
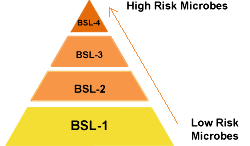
Laboratories handling pathogens are classified into four biosafety levels (BSL-1 to BSL-4), based on the risk posed by the microbes and the required safety precautions. BSL-1 is for low-risk microbes, while BSL-4 is for highly dangerous pathogens requiring full containment.



Physical Methods of Microbial Control
Heat-Related Methods
High temperatures denature proteins, disrupt cell membranes and walls, and damage nucleic acids. Key concepts include:
Thermal Death Point (TDP): Lowest temperature that kills all cells in a broth in 10 minutes.
Thermal Death Time (TDT): Minimum time required to sterilize a volume of liquid at a set temperature.
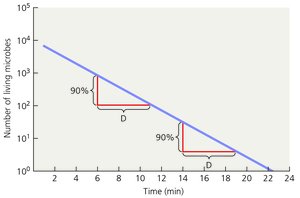
Decimal Reduction Time (D): Time required to reduce a microbial population by 90% at a given temperature.

Moist Heat Methods
Moist heat is more effective than dry heat for microbial control. Methods include:
Boiling: Kills most vegetative cells and viruses, but not endospores or some viruses. Boiling time varies with elevation.
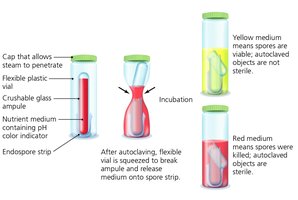
Autoclaving: Uses pressurized steam (121°C, 15 psi, 15 min) to achieve sterilization.
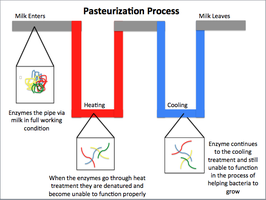
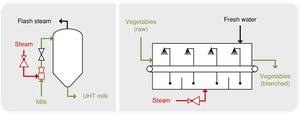
Pasteurization: Reduces microbial load in foods and beverages without sterilizing. Methods include batch, flash, and ultra-high-temperature (UHT) pasteurization.
Ultra-high-temperature sterilization: 140°C for 1–3 seconds, allowing treated liquids to be stored at room temperature.






Dry Heat Methods
Dry heat is used for materials that cannot be sterilized with moist heat. It denatures proteins and oxidizes chemicals, requiring higher temperatures and longer times. Incineration is the ultimate means of sterilization.


Refrigeration and Freezing
Low temperatures decrease microbial metabolism and growth. Refrigeration halts most pathogens, but some microbes can multiply in refrigerated foods. Slow freezing is more effective than quick freezing.
Desiccation and Lyophilization
Desiccation (drying) inhibits microbial growth by removing water. Lyophilization (freeze-drying) is used for long-term preservation, preventing damaging ice crystal formation.
Filtration
Filtration removes microbes from liquids and gases by passing them through filters with defined pore sizes. Modern filters can trap even viruses and are used to sterilize heat-sensitive materials.
Osmotic Pressure
High concentrations of salt or sugar create hypertonic environments, causing cells to lose water and inhibiting growth. Fungi are more resistant to osmotic pressure than bacteria.
Radiation
Ionizing radiation: Includes electron beams, gamma rays, and X-rays. It creates ions that disrupt DNA and other molecules, effectively killing microbes.
Nonionizing radiation: Includes UV light, which causes DNA damage (pyrimidine dimers) and is suitable for disinfecting air, fluids, and surfaces.
Chemical Methods of Microbial Control
Categories of Antimicrobial Chemicals
Surfactants: Reduce surface tension; soaps are good degerming agents, while detergents (quats) disrupt membranes.
Heavy Metals: Denature proteins; used as low-level bacteriostatic and fungistatic agents.
Phenol and Phenolics: Denature proteins and disrupt membranes; effective in presence of organic matter.
Alcohols: Intermediate-level disinfectants; denature proteins and disrupt membranes.
Halogens: Damage enzymes by denaturation; used in water treatment and antiseptics.
Oxidizing Agents: Kill by oxidation of enzymes; include peroxides, ozone, and peracetic acid.
Aldehydes: Cross-link functional groups to denature proteins and inactivate nucleic acids.
Gaseous Agents: Used in closed chambers; denature proteins and DNA.
Enzymes: Used for specific microbial control applications.
Case Study: Foodborne Infection
Campylobacter jejuni and Raw Dairy Products
Consumption of raw (unpasteurized) milk and cheese is a common source of foodborne infections, such as those caused by Campylobacter jejuni. Outbreaks often lead to public health investigations and temporary cessation of product sales until the contamination source is identified.

Summary Table: Relative Susceptibility of Microbes
Most Resistant | Most Susceptible |
|---|---|
Prions | Enveloped viruses |
Bacterial endospores | Most Gram-positive bacteria |
Cysts of Cryptosporidium (protozoan) | Large nonenveloped viruses |
Mycobacteria | Vegetative fungi |
Cysts of other protozoa | Fungal spores |
Small nonenveloped viruses | Active-stage protozoa (trophozoites) |
Active-stage protozoa (trophozoites) | Most Gram-negative bacteria |
Fungal spores |
