 Back
Backunit 5 lecture 2
Study Guide - Smart Notes

Herd Immunity and Pathogen Eradication
Herd Immunity
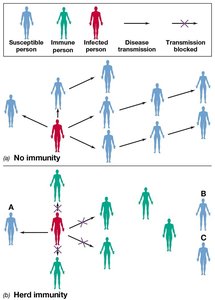
Herd immunity refers to the resistance of a population to the spread of an infectious disease when a sufficiently high proportion of individuals are immune, either through vaccination or previous infection. This concept is crucial for limiting disease transmission, especially for highly infectious diseases.
Definition: Herd immunity is achieved when enough individuals are immune to an infection, thereby indirectly protecting non-immune individuals by interrupting transmission chains.
Threshold: The required percentage of immune individuals varies by disease and is higher for more infectious pathogens.
Mechanisms: Immunity can be acquired through vaccination, natural infection, or innate resistance.
Public Health Importance: Herd immunity is a key strategy in disease control and eradication efforts.
Basic Reproduction Number (R0) and Herd Immunity Thresholds
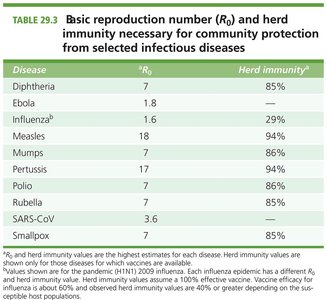
The basic reproduction number, R0, represents the average number of secondary infections produced by one infected individual in a fully susceptible population. The higher the R0, the greater the proportion of the population that must be immune to achieve herd immunity.
Calculation: Herd immunity threshold can be estimated as 1 - (1/R0).
Examples: Measles (R0 = 18) requires about 94% immunity; Influenza (R0 = 1.6) requires about 29%.
Disease | R0 | Herd Immunity (%) |
|---|---|---|
Diphtheria | 7 | 85% |
Ebola | 1.8 | 44% |
Influenza | 1.6 | 29% |
Measles | 18 | 94% |
Mumps | 17 | 94% |
Pertussis | 17 | 94% |
Polio | 7 | 86% |
Rubella | 7 | 85% |
SARS-CoV | 3.6 | 72% |
Smallpox | 7 | 85% |
Pathogen Eradication
Pathogen eradication is the complete elimination of a pathogen from all reservoirs, preventing new cases from occurring. This is a challenging goal, often requiring coordinated global efforts, surveillance, and vaccination campaigns.
Criteria: Easier for pathogens with only human reservoirs (e.g., smallpox).
Examples: Smallpox has been eradicated worldwide; polio eradication efforts are ongoing.
Challenges: Animal reservoirs, asymptomatic carriers, and incomplete vaccination coverage can hinder eradication.

Regional Elimination in the United States
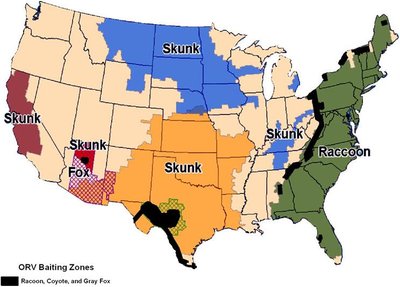
Several diseases have been regionally eliminated in the US, primarily through vaccination and public health measures. However, outbreaks can still occur due to imported cases or declining vaccination rates.
Eliminated Diseases: Yellow fever, smallpox, polio, malaria, measles, rubella, diphtheria.
Ongoing Efforts: Rabies control in wildlife, syphilis, tuberculosis.
Surveillance and Vaccination: Essential for maintaining elimination status.
Control of Microbial Growth
Terminology of Microbial Control
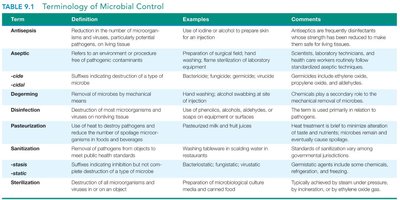
Understanding the terminology of microbial control is essential for selecting appropriate methods in clinical, laboratory, and public health settings.
Term | Definition | Example | Comment |
|---|---|---|---|
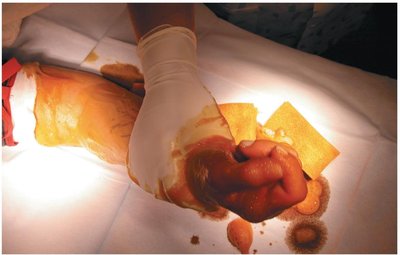
Antisepsis | Reduction of microorganisms on living tissue | Use of iodine on skin | Safe for living tissues |
Aseptic | Environment/procedure free of pathogens | Surgical field preparation | Prevents contamination |
Degerming | Removal by mechanical means | Handwashing | Chemical plays secondary role |
Disinfection | Destruction of most microorganisms on nonliving tissue | Use of phenolics, alcohols | Not all microbes killed |
Pasteurization | Use of heat to destroy pathogens in food/drink | Milk, fruit juices | Not sterilization |
Sanitization | Removal of pathogens to meet public health standards | Washing tableware | Some microbes remain |
-cide/-cidal | Destruction of a type of microbe | Bactericide, fungicide | Kills target organism |
-stasis/-static | Inhibition of microbe growth | Bacteriostatic | Does not kill, just inhibits |
Sterilization | Destruction/removal of all microorganisms | Preparation of microbiological culture media | Absolute removal |
Microbial Death Rates
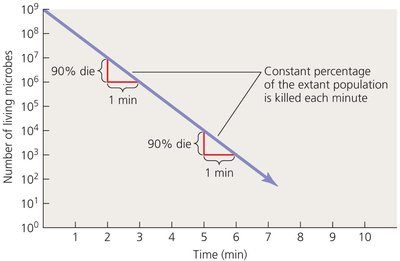
Microbial death rates describe the rate at which microorganisms are killed under specific conditions. The death rate is typically constant for a given organism and condition, and is used to determine the effectiveness of sterilization methods.
Decimal Reduction Time (D-value): The time required to kill 90% of the microbial population under specific conditions.
Application: Used to design sterilization protocols in healthcare and food industries.
Equation: Where is the number of surviving microbes at time , is the initial number, and is the decimal reduction time.
Physical Methods of Microbial Control: Heat
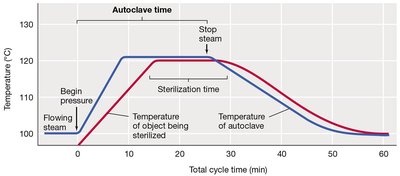
Heat is one of the most effective physical methods for controlling microbial growth. Both moist and dry heat can be used, but moist heat is generally more effective due to better heat penetration and protein denaturation.
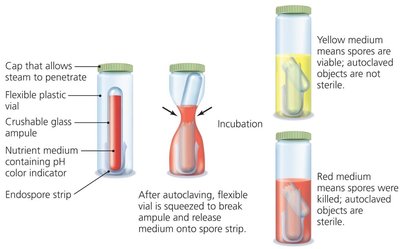
Autoclaving: Uses pressurized steam at 121°C to sterilize liquids and solids, including killing endospores.
Boiling: Effective for disinfection but not sterilization (does not kill all endospores).
Dry Heat: Used for sterilizing glassware and metal instruments (e.g., hot air oven, Bunsen burner).
Pasteurization
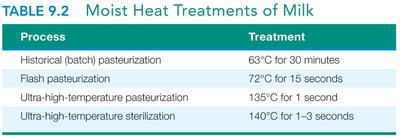
Pasteurization is a heat treatment process that reduces the number of viable pathogens in liquids such as milk, juice, and eggs, thereby increasing shelf life without significantly affecting taste or nutritional value.
Historical Pasteurization: 63°C for 30 minutes.
Flash Pasteurization: 72°C for 15 seconds.
Ultra-High Temperature (UHT): 135–140°C for 1–3 seconds (can achieve sterilization).
Outcome: Most, but not all, microbes are killed; surviving microbes are generally non-pathogenic.
Process | Treatment |
|---|---|
Historical (batch) pasteurization | 63°C for 30 minutes |
Flash pasteurization | 72°C for 15 seconds |
Ultra-high-temperature pasteurization | 135°C for 1 second |
Ultra-high-temperature sterilization | 140°C for 1–3 seconds |
Cold Temperatures and Desiccation
Cold temperatures (refrigeration and freezing) and desiccation (drying) are commonly used to slow or stop microbial growth, especially in food preservation.
Refrigeration/Freezing: Slows metabolism of most microbes; psychrophiles may still grow.
Desiccation: Removal of water inhibits microbial metabolism; adding solutes like salt or sugar enhances this effect.
Limitations: Some molds and spores can survive low moisture conditions.

Filtration
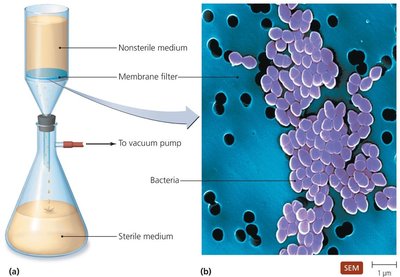
Filtration is a physical method used to remove microbes from heat-sensitive liquids and air. Membrane filters with defined pore sizes can exclude bacteria and larger organisms, but not viruses.
Applications: Sterilizing solutions containing proteins, antibiotics, or other heat-labile substances.
Mechanism: Liquid is forced through a filter; microbes are trapped on the membrane.

Radiation
Radiation is used to control microbial growth by damaging cellular components, especially DNA. There are two main types: ionizing and non-ionizing radiation.
Ionizing Radiation: (e.g., gamma rays, X-rays) produces ions and reactive molecules that damage DNA and proteins. Used for sterilizing medical supplies, food, and pharmaceuticals.
Non-Ionizing Radiation: (e.g., UV light) causes DNA mutations and is useful for sterilizing surfaces, air, and transparent fluids.
Limitations: UV light does not penetrate solids; ionizing radiation is more penetrating and effective for bulk items.

Chemical Methods of Microbial Control
Chemical agents are widely used to control microbial growth on surfaces, in liquids, and on living tissues. Their effectiveness depends on the agent, concentration, and target organism.
Protein Denaturation: Most chemical agents (e.g., phenols, alcohols, halogens, heavy metals, aldehydes) denature proteins, leading to cell death.
Membrane Disruption: Some chemicals disrupt cell membranes (e.g., alcohols, surfactants).
Other Mechanisms: Gases like ethylene oxide can sterilize equipment by penetrating materials.
Food Preservation Strategies
Food preservation relies on physical and chemical methods to limit microbial growth and extend shelf life.
Physical Methods: Refrigeration, freezing, desiccation, and irradiation.
Chemical Preservatives: Salt, sugar, nitrites, and potassium sorbate inhibit microbial growth by reducing water activity or interfering with metabolism.
Summary Table: Methods of Microbial Growth Control
Method | Mechanism | Example/Application |
|---|---|---|
Degerming | Mechanical removal | Handwashing before surgery |
Disinfection | Chemical destruction of most pathogens | Bleach on surfaces |
Sterilization | Destruction/removal of all microbes | Autoclaving surgical tools |
Pasteurization | Heat to kill most pathogens in liquids | Milk pasteurization |
Filtration | Physical removal by size exclusion | Filtering antibiotics solutions |
Radiation | DNA damage | UV sterilization of surfaces |
Desiccation | Removal of water | Dried fruits, jerky |
Cold Temperatures | Slows metabolism | Refrigerated foods |
Additional info: These notes integrate foundational concepts from Ch. 9 and Ch. 10 of a standard microbiology curriculum, focusing on the principles and applications of microbial growth control and public health strategies for infectious disease management.
