 Back
BackControlling Microbial Growth in the Environment: Principles and Methods
Study Guide - Smart Notes

Controlling Microbial Growth in the Environment
Basic Principles of Microbial Control
Microbial control is essential for preventing infection and contamination in medical, laboratory, and everyday settings. Understanding how microbes are killed or inhibited is foundational to microbiology and public health.
Microbial Death: Defined as the permanent loss of reproductive ability under ideal environmental conditions.
Microbial Death Rate: The rate at which a microbial population is killed, often constant under specific conditions. This is typically expressed as a logarithmic decline, meaning a constant percentage of the population dies per unit time.
Action of Antimicrobial Agents: Agents may target cell walls, membranes, proteins, or nucleic acids, leading to cell death or inhibition of growth.
Damage Mechanisms: Disruption of cell walls/membranes causes leakage of cellular contents; denaturation of proteins and nucleic acids halts essential cellular functions.
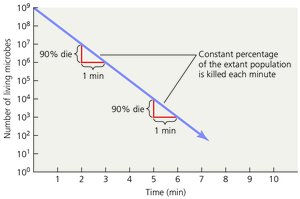
Terminology of Microbial Control
Microbial control methods are classified based on their effectiveness and the types of organisms they target.
Sterilization: The complete removal or destruction of all microbes, including endospores and viruses.
Disinfection: The use of physical or chemical agents to destroy most microbes on inanimate objects.
Antisepsis: Reduction of microbes on living tissue.
Sanitization: Lowering microbial counts to safe public health levels.
Degerming: Mechanical removal of microbes from a limited area.
Selection of Microbial Control Methods
The choice of microbial control method depends on the situation, the nature of the item or area to be treated, and the type of microbes present.
Ideal Agents: Should be inexpensive, fast-acting, stable during storage, and harmless to humans, animals, and objects.
Factors Affecting Efficacy:
Site to be Treated: Some methods are unsuitable for living tissues or delicate materials.
Relative Susceptibility: Microbes vary in resistance to control methods. Prions and bacterial endospores are among the most resistant, while enveloped viruses are most susceptible.
Environmental Conditions: Temperature, pH, and presence of organic matter can influence the effectiveness of antimicrobial agents.

Biosafety Levels
Laboratories handling infectious agents are classified into four biosafety levels (BSL) based on the risk posed by the microbes.
BSL-1: For agents not known to cause disease in healthy humans.
BSL-2: For moderately hazardous agents.
BSL-3: For agents that can cause serious or potentially lethal disease via inhalation; requires safety cabinets.
BSL-4: For dangerous and exotic agents that pose a high risk of aerosol-transmitted infections and life-threatening disease; requires full-body, air-supplied suits and specialized facilities.

Physical Methods of Microbial Control
Heat-Related Methods
Heat is one of the most common and effective methods for controlling microbial growth. It works by denaturing proteins, disrupting membranes, and damaging nucleic acids.
Thermal Death Point (TDP): The lowest temperature that kills all cells in a broth in 10 minutes.
Thermal Death Time (TDT): The time required to sterilize a volume of liquid at a set temperature.
Decimal Reduction Time (D value): The time required to kill 90% of the microbes in a sample at a specific temperature.
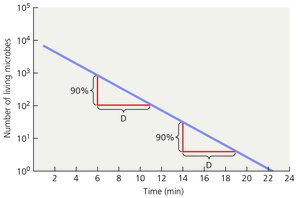
Moist Heat
Boiling: Kills most vegetative cells, fungi, protozoa, and most viruses, but not endospores or some viruses.
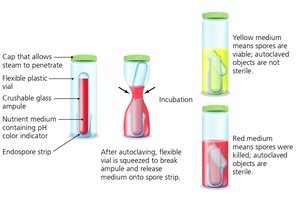
Autoclaving: Uses pressurized steam (121°C, 15 psi, 15 min) to achieve sterilization, effective against endospores.
Pasteurization: Reduces microbial load in heat-sensitive liquids (e.g., milk, juice) without sterilizing; heat-tolerant microbes may survive.
Ultra-high-temperature Sterilization: Exposes liquids to 140°C for 1–3 seconds, allowing storage at room temperature.

Dry Heat
Used for materials that cannot be sterilized with moist heat (e.g., powders, oils).
Requires higher temperatures and longer times than moist heat.
Incineration is the ultimate means of sterilization.
Refrigeration and Freezing
Low temperatures decrease microbial metabolism, growth, and reproduction. Most pathogens do not grow at refrigeration temperatures, but some can survive or even multiply.
Refrigeration: Halts growth of most pathogens.
Freezing: Slow freezing is more effective than quick freezing due to formation of ice crystals that damage cells.
Desiccation and Lyophilization
Desiccation (drying) inhibits microbial growth by removing water, while lyophilization (freeze-drying) is used for long-term preservation of microbial cultures by preventing ice crystal formation.

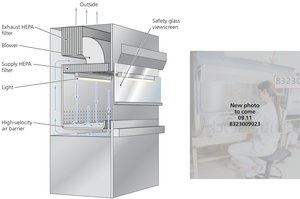
Filtration
Filtration physically removes microbes from liquids or air using filters with pores small enough to retain microorganisms. This method is essential for sterilizing heat-sensitive solutions and maintaining sterile environments.
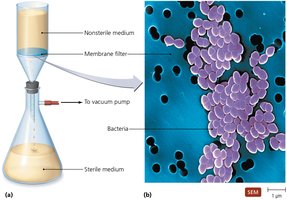
Osmotic Pressure
High concentrations of salt or sugar create hypertonic environments, causing cells to lose water and inhibiting microbial growth. Fungi are generally more resistant to osmotic pressure than bacteria.
Radiation
Ionizing Radiation: (e.g., gamma rays, X-rays) Ejects electrons from atoms, creating ions that damage DNA and proteins. Used for sterilizing medical supplies and food.
Nonionizing Radiation: (e.g., UV light) Causes formation of thymine dimers in DNA, inhibiting replication. Used for disinfecting air, surfaces, and transparent fluids.

Chemical Methods of Microbial Control
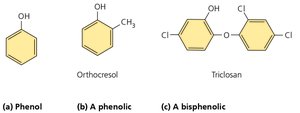
Phenol and Phenolics
Phenolics are compounds derived from phenol that disrupt cell membranes and denature proteins. They are effective in the presence of organic matter and remain active for prolonged periods.
Alcohols
Alcohols are intermediate-level disinfectants that denature proteins and disrupt membranes. They are commonly used for skin antisepsis and surface disinfection but are not effective against endospores or some viruses.
Halogens
Halogens (e.g., iodine, chlorine, bromine) are intermediate-level antimicrobial chemicals that damage enzymes by denaturation. They are widely used for disinfecting water, surfaces, and medical equipment.
Oxidizing Agents
Oxidizing agents such as hydrogen peroxide, ozone, and peracetic acid kill microbes by oxidizing their enzymes. They are high-level disinfectants and are used for sterilizing surfaces and equipment.
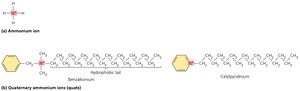
Surfactants
Surfactants, including soaps and detergents, reduce surface tension and aid in the mechanical removal of microbes. Quaternary ammonium compounds (quats) are low-level disinfectants that disrupt cell membranes.
Heavy Metals
Heavy-metal ions (e.g., silver, mercury, copper) denature proteins and are used as low-level bacteriostatic and fungistatic agents. Examples include silver nitrate for preventing neonatal blindness and copper for controlling algal growth.

Aldehydes
Aldehydes (e.g., glutaraldehyde, formalin) are high-level disinfectants that cross-link functional groups in proteins and nucleic acids, inactivating them. Used for sterilizing medical equipment and preserving biological specimens.
Gaseous Agents
Gaseous agents such as ethylene oxide are used in closed chambers to sterilize heat-sensitive items. They denature proteins and DNA but are highly toxic and potentially carcinogenic.
Enzymes
Antimicrobial enzymes, such as lysozyme, break down microbial cell walls. They are used in food preservation and to remove prions from medical instruments.
Antimicrobial Drugs
Antibiotics, semisynthetic, and synthetic drugs are primarily used to treat infectious diseases but can also be used for microbial control outside the body.
Evaluating Disinfectants and Antiseptics
The efficacy of disinfectants and antiseptics can be measured using the phenol coefficient, which compares their effectiveness to phenol. A value greater than 1.0 indicates greater efficacy than phenol.
