 Back
BackDigestive System Infections: Microbiology Study Notes
Study Guide - Smart Notes

Digestive System Infections
Overview of the Digestive System
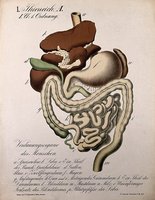
The digestive system is composed of the gastrointestinal (GI) tract and accessory organs. It is responsible for the breakdown and absorption of nutrients, as well as the elimination of waste. The GI tract extends from the mouth to the anus and is divided into upper and lower sections. Accessory organs include the salivary glands, liver, gallbladder, and pancreas.
Upper GI tract: Mouth, pharynx, esophagus, stomach
Lower GI tract: Small and large intestines, rectum, anus
Accessory organs: Salivary glands, liver, gallbladder, pancreas
Defenses of the GI Tract
The GI tract is protected by several barriers that limit microbial colonization and infection.
Lysozyme in saliva: Enzyme that breaks down bacterial cell walls
Acidity of gastric juices: Destroys many ingested microbes
Bile salts: Disrupt bacterial membranes
Mucus lining: Physical barrier to pathogens
Mucosa-associated lymphoid tissue (MALT): Immune surveillance
Normal gut microbiota: Compete for nutrients and surfaces, produce antimicrobial substances
Digestive System Microbiome
Composition and Distribution
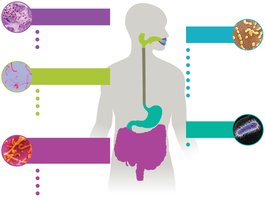
The digestive tract harbors the most diverse and dense population of microbes in the human body. Different regions support distinct microbial communities.
Mouth: Prevotella, Porphyromonas, Veillonella, Streptococcus
Gums: Neisseria, Haemophilus, Streptococcus
Teeth: Streptococcus, Porphyromonas, Veillonella, Prevotella, Actinomyces, Corynebacterium, Neisseria
Stomach: Helicobacter pylori
Small and large intestines: Lactobacillus, Bacteroides, Streptococcus, Gemella
Transmission, Causes, and Prevention of Digestive System Infections
Transmission
Most intestinal pathogens are transmitted via the fecal–oral route, primarily through contaminated food or water. Poor hygiene, inadequate water sanitation, and insufficient food-handling regulations increase risk.
Prevention
Hand washing
Sewer management
Water sanitation practices
Food processing regulations
Diagnostic Tools for GI Infections
Diagnosis of digestive system infections involves several laboratory and clinical techniques:
Fecal sample collection for culturing on selective and differential media
Molecular diagnostic analysis
Microscopic examination for parasites/eggs
Endoscopy (upper GI or colonoscopy) to observe tissue damage
Viral Infections of the GI Tract
Mumps
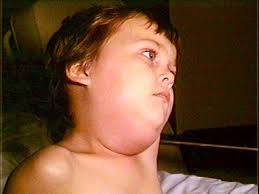
Mumps is caused by an enveloped RNA virus and is transmitted via respiratory droplets or direct contact with infected saliva. The incubation period is 2–3 weeks. Adults are more likely to experience severe complications.
Signs and symptoms: Swelling of the parotid salivary glands (parotitis), dry mouth, fever, headache, fatigue
Treatment: Symptomatic therapy
Complications: Orchitis (testicular inflammation), hearing loss
Hepatitis
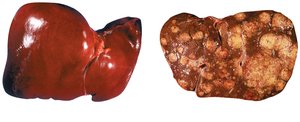
Hepatitis refers to inflammation of the liver and can be caused by several viruses, including hepatitis A, B, and C. Each type can be acute or chronic.
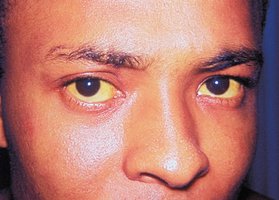
Hepatitis A: Single-stranded RNA virus, transmitted via fecal–oral route. Symptoms include low-grade fever, nausea, vomiting, abdominal pain, fatigue, and jaundice. Usually self-limiting; prevention includes good hygiene and vaccination.
Hepatitis B: Double-stranded DNA virus, transmitted via blood, sexual contact, or vertically from mother to child. Symptoms include abdominal pain, dark urine, fever, fatigue, and jaundice. Chronic infection can lead to cirrhosis, liver failure, and hepatocellular carcinoma. Prevention includes vaccination.
Bacterial Infections of the GI Tract
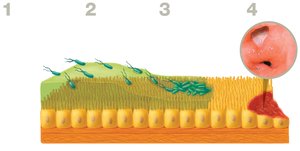
Helicobacter pylori and Stomach Ulcers
Helicobacter pylori is a Gram-negative, vibrio-shaped bacterium that infects the stomach lining. It is transmitted via the fecal–oral route and is associated with gastritis and peptic ulcers.
Pathology: Produces urease and burrows into the stomach lining, causing inflammation and ulcers.
Diagnosis: Detection of antigens in stool, antibodies in blood, urea breath test, or biopsy during endoscopy.
Treatment: Antibiotics and proton pump inhibitors.
Bacterial Food Poisoning
Food poisoning (intoxication) results from ingestion of preformed bacterial toxins (enterotoxins) in food. Common agents include Staphylococcus aureus, Clostridium perfringens, and Bacillus cereus.
S. aureus: Linked to mayonnaise salads, dairy, poultry, and meat products. Transmission is often via unwashed hands.
C. perfringens: Spore-forming, found in animal intestines and raw meat. Associated with gravy and meat left at room temperature.
B. cereus: Spore-forming, present in soil and produce. Spores survive cooking and germinate if food is left at room temperature.

Bacterial Food Infections
Foodborne bacterial infections result from ingestion of live pathogens that colonize and infect the GI tract. Common agents include Shigella species, Escherichia coli O157:H7, Salmonella enterica, and Vibrio cholerae.
Shigella: Causes shigellosis (dysentery), transmitted via fecal–oral route. Produces exotoxins that damage intestinal cells.
E. coli O157:H7: Shiga toxin–producing strain, infectious dose as low as 10–100 cells. Causes bloody diarrhea and can lead to hemolytic uremic syndrome (HUS).
Salmonella enterica: Causes salmonellosis and typhoid fever. Transmitted via contaminated food, water, or contact with animals. Typhoid fever is human-specific and can cause severe systemic illness.
Vibrio cholerae: Causes cholera, characterized by profuse watery diarrhea ("rice-water stools"). Can lead to rapid dehydration and death if untreated.
Clostridioides difficile Infections
Clostridioides difficile is a spore-forming, Gram-positive anaerobe that causes antibiotic-associated diarrhea and colitis. Transmission is via fecal–oral route, often in healthcare settings.
Virulence factors: Exotoxins A and B
Treatment: Withdrawal of antibiotics, rehydration, vancomycin, or fecal transplant
Prevention: Limit unnecessary antibiotic use
Protozoan Infections of the GI Tract
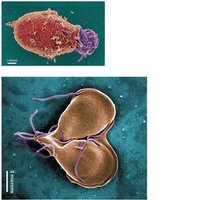
Giardiasis
Caused by Giardia lamblia, which exists as cysts (resistant to disinfection) and trophozoites. Transmission occurs via ingestion of cysts in contaminated water or food.
Symptoms: Diarrhea, flatulence, vomiting
Treatment: Usually self-limiting; metronidazole for severe cases
Prevention: Boil or filter water; chlorine is ineffective against cysts
Amebiasis
Caused by Entamoeba histolytica, prevalent in tropical regions. Transmission is fecal–oral. Most infections are asymptomatic, but invasive disease can cause ulcers and systemic abscesses.
Treatment: Metronidazole
Prevention: Same as giardiasis
Cryptosporidiosis
Caused by Cryptosporidium species, which reside in the intestines of humans and animals. Oocysts are resistant to chlorine and can contaminate surface water.
Symptoms: Mild diarrhea in healthy individuals; severe, chronic infection in immunocompromised
Treatment: Anti-protozoan medications, hydration
Prevention: Proper water treatment (filtration and UV radiation)
