 Back
BackEpidemiology: Tracking Infectious Diseases
Study Guide - Smart Notes

Epidemiology
Introduction to Epidemiology
Epidemiology is the scientific discipline concerned with studying how diseases are distributed within populations and the factors that influence or determine this distribution. It is fundamental to understanding, preventing, and controlling infectious diseases in communities.
Epidemiology investigates patterns, causes, and effects of health and disease conditions.
It provides the basis for public health interventions and policy decisions.
Key focus: infectious disease transmission, outbreak detection, and disease prevention.

Basic Concepts of Epidemiology
Several foundational concepts help explain how infectious diseases behave within populations:
Incidence: The rate at which new cases occur in a population over a specific period.
Prevalence: The total number of existing cases in a population at a given time.
Infectivity: The ability of a pathogen to enter and multiply in a host.
Pathogenicity: The ability of a pathogen to cause clinical disease after infection.
Virulence: The degree of severity of the disease produced by the pathogen.
Epidemiologic Triad
Agent, Host, and Environment
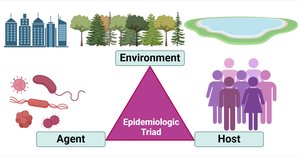
The Epidemiologic Triad is a traditional model for understanding infectious disease. It consists of three components:
Agent: The pathogen (bacteria, virus, fungus, parasite) responsible for causing disease.
Host: The susceptible person who can become infected.
Environment: External factors that bring the agent and host together, such as climate, urbanization, and water sources.
Chain of Infection
Steps in Disease Transmission
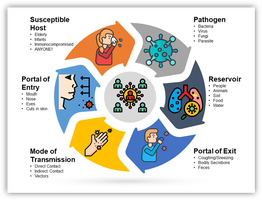
The Chain of Infection describes the sequence of events required for a disease to spread:
Pathogen: The infectious agent (bacteria, virus, etc.).
Reservoir: Where the pathogen lives (people, animals, soil, water).
Portal of Exit: How the pathogen leaves the reservoir (coughing, sneezing, bodily secretions).
Mode of Transmission: How the pathogen is transferred (direct contact, indirect contact, vectors).
Portal of Entry: How the pathogen enters a new host (nose, mouth, skin).
Susceptible Host: Individuals at risk (elderly, infants, immunocompromised).
Core Epidemiological Tools
Descriptive and Analytic Epidemiology
Epidemiologists use specific methodologies to gather data and test hypotheses:
Descriptive Epidemiology: Organizes data by person (who is ill), place (where they are), and time (when they became ill) to identify patterns.
Analytic Epidemiology: Uses comparison groups to test hypotheses about the link between exposure and disease, often through cohort studies or case-control studies.
Surveillance Systems: Continuous, systematic collection and analysis of health data to monitor disease trends and detect outbreaks early.
Reproductive Number (Rt or R0)
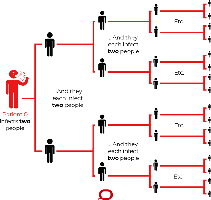
The Reproductive Number is a metric estimating the average number of new infections caused by one infected person:
Rt > 1.0: Indicates an increasing epidemic.
Rt < 1.0: Indicates a declining epidemic.
Formula:
Tracing Infectious Diseases
Disease Emergence
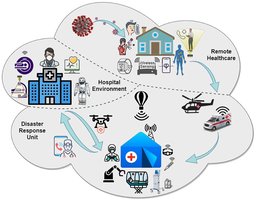
New infectious diseases often emerge when pathogens cross from animals to humans or adapt to new environments. Their spread is accelerated by global connectivity, and rapid detection relies on advanced molecular tools and digital surveillance.
Zoonotic Spillover: Most emerging infectious diseases (EIDs) are zoonotic, originating in animals before jumping to humans. Examples: HIV (chimpanzees to humans), SARS (wild animals to humans).
Ecological Changes: Human activities like deforestation and urbanization increase contact with wildlife, leading to new diseases (e.g., Lyme disease).
Pathogen Adaptation: Microbes can evolve to become more dangerous or drug-resistant. Pandemic influenza arises when flu strains "reassort" in animals, creating new viruses.
Spread: Globalization and Connectivity
Modern factors allow diseases to spread globally in record time:
Global Travel: Humans can travel worldwide in under 36 hours, turning localized outbreaks into global epidemics (e.g., SARS in 2003).
Vector Movement: Climate and trade changes move disease-carrying insects to new areas (e.g., Zika virus spread).
Detection: Advanced Surveillance and Rapid Testing
Molecular Tools
Early detection is critical for stopping outbreaks before they become pandemics. Molecular techniques like real-time PCR allow scientists to identify a pathogen's genetic material within hours, even for new variants.

Digital and Genomic Surveillance
Automated systems scan global news, social media, and online reports to find early signals of disease outbreaks. Metagenomic sequencing of viral genomes reveals how diseases move through regions in real-time.
Environmental Monitoring
Scientists use advanced digital PCR to detect pathogens in environmental samples, such as soil, to warn communities of potential infection hotspots before outbreaks peak.

Summary Table: Key Epidemiological Concepts
Concept | Definition | Example |
|---|---|---|
Incidence | Rate of new cases in a population | New COVID-19 cases per week |
Prevalence | Total existing cases in a population | Total HIV cases in a country |
Infectivity | Ability to enter and multiply in host | Norovirus in cruise ships |
Pathogenicity | Ability to cause clinical disease | Streptococcus causing strep throat |
Virulence | Severity of disease produced | Ebola virus |
R0 | Average number of new infections per case | Measles R0 ≈ 15 |
