 Back
BackGram-Negative Bacilli: Structure, Pathogenicity, and Clinical Relevance
Study Guide - Smart Notes

Gram-Negative Bacilli
Overview and Clinical Relevance
Gram-negative bacilli are a diverse group of rod-shaped bacteria that are significant in clinical microbiology due to their role as causative agents of many diseases. Their pathogenicity is attributed to various virulence factors, including toxins, enzymes, and their ability to evade the host immune system.
Virulence Factors: Include exotoxins, endotoxins, enzymes that degrade host tissues, siderophores for iron acquisition, and biofilm formation.
Biofilm Formation: Enables resistance to immune attacks and antibiotics.
Immune Evasion: Mechanisms such as capsules and efflux pumps help bacteria survive in hostile environments.
Definition: Virulent refers to the degree to which a microorganism can cause disease.

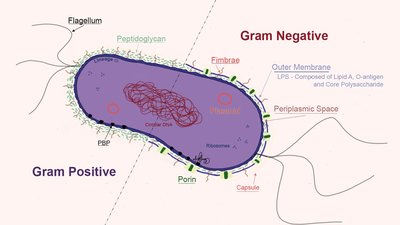
Structural Features of Gram-Negative Bacilli
Gram-negative bacilli possess unique structural features that contribute to their pathogenicity and resistance to treatment.
Cell Wall: Thin peptidoglycan layer surrounded by an outer membrane containing lipopolysaccharide (LPS).
Outer Membrane: Acts as a barrier to many antibiotics and contains porins for selective permeability.
Fimbriae and Pili: Facilitate attachment to host cells and surfaces.
Flagella: Provide motility, often polar (located at one or both ends).
Capsule: Protects against phagocytosis and enhances virulence.

Pseudomonas aeruginosa
Ecology and Structural Characteristics
Pseudomonas aeruginosa is commonly found in soil, water, and moist environments such as bathtubs and sinks. It is notable for its motility, environmental adaptability, and presence in hospital settings.
Polar Flagella: Located at one or both ends, enabling motility.
Fimbriae: Aid in attachment to surfaces and host tissues.
Biofilm Formation: Contributes to persistence and resistance.
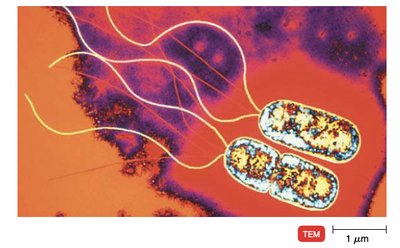
Metabolic Versatility
Pseudomonas aeruginosa synthesizes a wide variety of enzymes, allowing it to metabolize uncommon substances, including pesticides and soap residues. Its ability to grow in low-moisture environments and utilize unusual carbon sources makes it a formidable environmental and clinical pathogen.
Enzyme Production: Enables decomposition of complex chemicals.
Growth in Soap Residues: Can survive in environments hostile to most bacteria.
Biofilm Strength: Forms robust biofilms, especially in hospital settings.

Opportunistic Pathogenicity
Pseudomonas aeruginosa is an opportunistic pathogen, posing a primary risk to immunocompromised patients, such as those with cystic fibrosis, cancer, AIDS, or indwelling medical devices. It is a leading cause of death in cystic fibrosis patients and is responsible for a significant proportion of healthcare-associated infections (HAIs).
Antibiotic Resistance: Due to cell wall porins and efficient efflux pump systems.
Biofilm Formation: Enhances resistance to treatment.
Cystic Fibrosis: Thick, sticky mucus traps bacteria, impairing ciliary clearance.
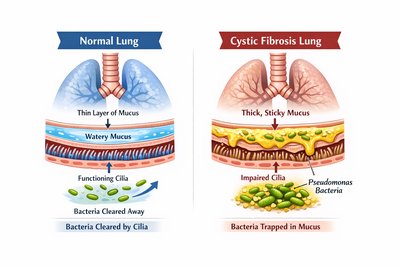
Extracellular Pigments and Virulence
Pseudomonas aeruginosa produces extracellular, water-soluble pigments that serve as virulence factors and aid in laboratory identification.
Pigment | Color / Appearance | Main Function(s) | Clinical Relevance |
|---|---|---|---|
Pyocyanin | Blue-green | Generates reactive oxygen species (ROS); antimicrobial; damages host tissues | Characteristic color in infections |
Pyoverdine | Yellow-green, fluorescent | Siderophore; chelates iron; promotes virulence | Fluorescent under UV; lab identification |

Haemophilus influenzae
Ecology and Growth Requirements
Haemophilus influenzae inhabits the mucous membranes of the upper respiratory tract and is transmitted via respiratory droplets. It is a fastidious organism, requiring blood in its culture medium to acquire essential growth factors.
Culture Medium: Grows on chocolate agar, which contains lysed blood cells.
Transmission: Spread by coughing and sneezing.

Structural Features and Pathogenicity
Haemophilus influenzae is a coccobacillus with no flagella but possesses pili (fimbriae) for attachment to epithelial cells. The presence of a capsule, especially type b (Hib), increases virulence and is associated with invasive diseases such as meningitis.
Capsule: Type b capsule is highly virulent; non-encapsulated strains cause localized infections.
Fimbriae: Essential for attachment to host cells.
Diseases: Meningitis, bacteremia, epiglottitis (encapsulated); otitis media, sinusitis, bronchitis, pneumonia (non-encapsulated).
Vaccination: Prevents type B H. influenzae infections.
Legionella pneumophila
Ecology and Transmission
Legionella pneumophila is found in water systems such as lakes, rivers, plumbing, and hot tubs. Infections occur through inhalation of aerosols containing the bacteria.
Pili/Fimbriae: Aid in attachment.
Polar Flagella: Provide motility.
Intracellular Pathogenicity
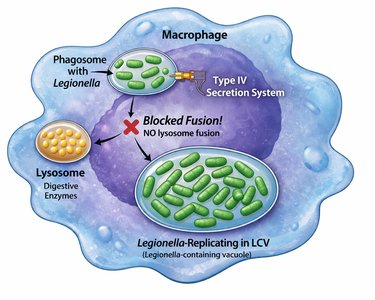
Legionella pneumophila infects lung macrophages, surviving and multiplying inside a specialized vacuole (Legionella-containing vacuole, LCV) by using a Type IV secretion system to inject proteins and block lysosome fusion. This leads to macrophage bursting and pneumonia symptoms in Legionnaires’ disease.
Type IV Secretion System: Injects proteins into macrophages.
Intracellular Survival: Replicates inside LCV, evading host defenses.
Macrophage Bursting: Releases bacteria and inflammatory signals.
Risk Factors and Immune Response
Smoking and immunocompromised states increase susceptibility to Legionella infection. Smoking damages cilia and impairs macrophage function, while weak T-cell responses hinder clearance of this intracellular pathogen.
Smoking: Damages cilia, impairs clearance.
Immunocompromised: Weak T-cell response reduces macrophage activation.
Bordetella pertussis
Structural Features and Pathogenicity
Bordetella pertussis is a small coccobacillus that is not considered an opportunistic pathogen. It possesses fimbriae and adhesion proteins for strong attachment, and virulent strains have a capsule. Several toxins are produced, including tracheal cytotoxin and pertussis toxin, which damage ciliated cells and disrupt immune signaling.
Fimbriae & Adhesion Proteins: Enable strong attachment to respiratory epithelium.
Capsule: Increases virulence.
Toxins: Tracheal cytotoxin and pertussis toxin.
Whooping Cough (Pertussis)
Pertussis is primarily a childhood disease, highly contagious and spread through airborne droplets. The disease progresses through three stages: catarrhal (resembles a cold), paroxysmal (severe coughing fits), and convalescence (gradual recovery). Early antibiotic treatment is effective; later stages require supportive care. Vaccination (DTaP/Tdap) is essential for prevention.
Catarrhal Stage: Initial, mild symptoms.
Paroxysmal Stage: Severe coughing, compromised ciliary action, mucus accumulation.
Convalescence Stage: Gradual recovery, may last months.
Vaccination: DTaP for children, Tdap for adults.
Enteric Bacteria
Overview and Clinical Relevance
Enteric bacteria are gut bacteria, many of which are normal flora but can act as opportunistic pathogens. Notable genera include Salmonella, Shigella, Enterobacter, Escherichia, and Citrobacter. Their structural features, such as capsules, fimbriae, and flagella, are closely related to their virulence.
Normal Flora: Many are harmless in the gut but can cause disease if displaced.
Opportunistic Pathogens: Cause infections in immunocompromised hosts.
Virulence Structures: Capsules, fimbriae, flagella enhance pathogenicity.
Summary Table: Gram-Negative Bacilli
Genus | Habitat | Virulence Factors | Clinical Relevance |
|---|---|---|---|
Pseudomonas | Soil, water, hospitals | Biofilm, pigments, enzymes, efflux pumps | HAIs, cystic fibrosis, burns |
Haemophilus | Respiratory tract | Capsule, fimbriae | Meningitis, otitis media |
Legionella | Water systems | Type IV secretion, intracellular survival | Legionnaires’ disease |
Bordetella | Respiratory tract | Fimbriae, toxins, capsule | Whooping cough |
Enteric bacteria | Gut | Capsule, fimbriae, flagella | GI infections, opportunistic |
