Back
BackHost-Microbe Interactions and Pathogenesis: Study Guide
Study Guide - Smart Notes

Host-Microbe Interactions and Pathogenesis
Host-Microbe Interactions
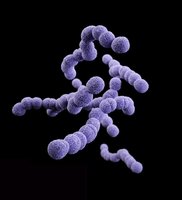
Host-microbe interactions encompass the complex relationships between humans and the microorganisms that colonize their bodies. Not all interactions are harmful; many are mutualistic, contributing to health and homeostasis. Disruption of these relationships can lead to disease.
Normal Microbiota: Microorganisms that colonize nearly every part of the human body, often providing benefits such as protection against pathogens and aiding digestion.
Mutualism: Both host and microbe benefit from the relationship.
Dysbiosis: Disruption of normal microbiota, which can compromise health and increase susceptibility to infection.
Example: Antibiotic therapy can reduce normal gut microbiota, allowing pathogens to establish infection.
Host Factors
Host factors, such as immune status and age, influence whether a microbe is pathogenic. Some microbes are harmless in one host but cause disease in another.
Example: Group B Streptococci (GBS) is a commensal in adult women but can cause severe infections in newborns due to their immature immune systems.
Tropism
Tropism refers to a pathogen's preference for a particular host or tissue. Changes in tropism can lead to new infectious diseases.
Estimated 60-80% of new infectious diseases in humans result from changes in tropism.
Virulence
Virulence and Pathogenicity
Pathogenicity is the ability of a microbe to cause disease, while virulence is the degree of disease caused. Virulence factors are mechanisms that help pathogens overcome host defenses.
Virulence Factors: Include toxins, adhesins, invasins, and mechanisms to evade immunity.
Example: Influenza virus strains vary in virulence; some cause mild disease, others cause widespread mortality.
Host Factors & Virulence
Host properties, such as age and immune response, affect the outcome of infection. Some virulence factors directly damage host cells, while others provoke immune responses.
Example: The 1918 influenza pandemic was more virulent in young adults, likely due to overstimulation of the immune system.
Transmission
Pathogens with less aggressive or asymptomatic infections often transmit more readily. Transmission is quantified by reproduction numbers.
Basic reproduction number (R0): Expected number of cases directly generated by one case in a susceptible population.
Effective reproduction number (Re): Changes as host-pathogen interactions evolve.
Environment and Evolution of Virulence
Pathogens evolve new virulence factors in response to environmental pressures, such as antibiotic use. Removal of selective pressure can lead to loss of resistance.
Example: Salmonella typhi resistance to ampicillin decreased after the drug was no longer used.
Attenuation: Pathogens grown in cell culture often lose virulence factors.
Exposure Dose
The infectious dose-50 (ID50) and lethal dose-50 (LD50) are quantitative measures of pathogen infectivity and toxicity.
ID50: Number of cells or virions needed to infect 50% of exposed hosts.
LD50: Amount of toxin needed to kill 50% of untreated hosts.
Toxins
Toxins are molecules produced by microbes that cause adverse effects in hosts. Toxigenic microbes produce toxins, and toxemia refers to the presence of toxins in the blood.
Example: Bacillus cereus produces a heat-stable toxin causing food poisoning.
Endotoxins
Endotoxins are lipid A components of lipopolysaccharide (LPS) in Gram-negative bacteria, released when bacteria die or divide. They can cause septic shock, and there are no vaccines or therapies against them.
Exotoxins
Exotoxins are toxic soluble proteins produced by both Gram-positive and Gram-negative bacteria. They are classified based on their target or mechanism.
Neurotoxins: Affect nervous system
Enterotoxins: Affect gastrointestinal tract
Hepatotoxins: Affect liver
Nephrotoxins: Affect kidneys
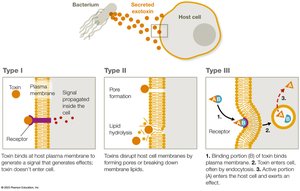
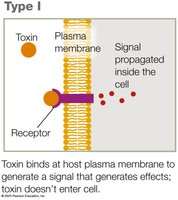
Type I Exotoxins
Type I exotoxins act on the cell membrane by binding to specific receptors and triggering signaling cascades without entering the cell. Superantigens are examples that overstimulate the immune system.
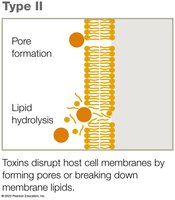
Type II Exotoxins
Type II exotoxins damage host cell membranes by forming pores or breaking down membrane lipids, leading to cell lysis.
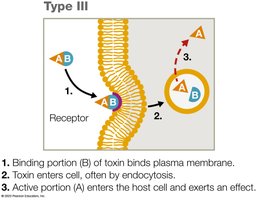
Type III Exotoxins
Type III exotoxins are intracellular toxins (AB toxins). The B portion binds to a cell receptor, and the A portion enters the cell to exert its effects.
Example: Botulinum toxin produced by Clostridium botulinum.
Steps to Infection
Establishing an Infection
Pathogens follow a series of steps to establish infection: entry, adhesion, invasion, replication, and transmission.
Enter the host
Adhere to host tissues
Invade tissues and obtain nutrients
Replicate while evading immune defenses
Transmit to a new host
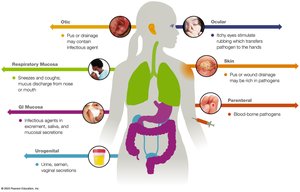
Step 1: Entering the Host
Pathogens use specific portals of entry, which are often sites of disease development.
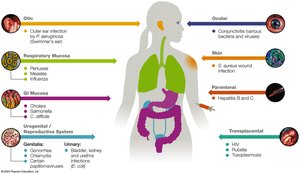
Integumentary System
The skin, hair, nails, and glands form the largest body system. Pathogens can enter via wounds, otic entry, conjunctiva, or parenteral routes.
Other Portals of Entry
Respiratory tract: Most common portal; entry via droplets, aerosols, or dust.
Gastrointestinal tract: Fecal-oral transmission; invasion of mucosal surfaces.
Urogenital tract: Sexually transmitted pathogens; vertical transmission from mother to fetus.
Step 2: Adhere to Host Tissues
Initial adhesion is often nonspecific, followed by specific interactions using adhesins. Adhesins are virulence factors that facilitate attachment to host cells.
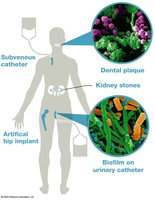
Biofilms and Quorum Sensing
Biofilms provide a platform for adhesion and enhance virulence. Quorum sensing regulates biofilm formation and dispersal.
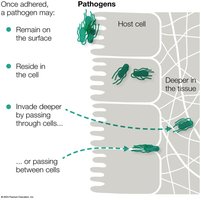
Step 3: Invade Tissues and Obtain Nutrients
After adhesion, pathogens may remain on the surface, invade deeper tissues, or reside within cells as intracellular pathogens.
Invasins
Invasins are local-acting factors, such as extracellular enzymes and surface molecules, that enable tissue invasion.
Obtaining Nutrients
Siderophores: Molecules that extract iron from transferrin.
Extracellular enzymes: Break down nutrients in the local environment, aiding pathogen survival and damaging host tissues.
Examples: Lipases and proteases.
Cytopathic Effects
Pathogens cause cytopathic effects, which may kill (cytocidal) or damage (noncytocidal) host cells. Some pathogens are oncogenic, transforming normal cells into cancer cells. Immune-mediated damage can also occur.
Step 4: Evade Host Defenses
Pathogens use various strategies to evade host immunity, including hiding within biofilms, entering a latent state, and altering antigenic features.
Antigenic masking: Concealing antigenic features.
Antigenic mimicry: Imitating host cells.
Antigenic variation: Altering surface molecules.

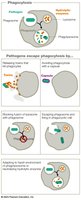
Undermining Host Immune Response
Pathogens interfere with phagocytosis and immune responses using capsules, proteases, and other mechanisms.
Escape from phagosomes
Prevent fusion of phagosome and lysosome
Neutralize enzymes
Thrive in harsh environments
Suppress immune system
Step 5: Transmission to New Host
Pathogens exit the host via specific portals of exit and maintain reservoirs for continued transmission.
Safety
Biosafety Levels
Biosafety levels (BSLs) are rankings that guide safety practices in laboratories and healthcare settings. Levels are determined by infectivity, disease severity, transmission mode, and availability of treatments.
BSL-1: Agents rarely cause disease in healthy individuals (e.g., Bacillus subtilis, E. coli K12).
BSL-2: Pathogens cause disease but are preventable or treatable (e.g., Staphylococcus aureus, herpes simplex viruses).
BSL-3: Agents cause serious or lethal diseases, some with airborne transmission (e.g., Mycobacterium tuberculosis).
BSL-4: Dangerous, exotic pathogens with no cures (e.g., Ebola virus).
Infection Control
Standard Precautions
Standard precautions are applied to all patients to prevent transmission of infectious agents. These include hand hygiene, use of gloves, barrier gowns, and disinfection.

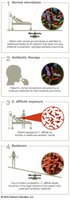
Transmission Precautions
Transmission precautions are additional measures taken when a specific infectious agent is suspected or known. They include contact, droplet, and airborne precautions, each with specific protocols.