 Back
BackHost Resistance to Viral Infections: Mechanisms and Immune Responses
Study Guide - Smart Notes

Host Resistance to Viral Infections
Overview of Host Resistance
Host resistance to viral infections refers to the ability of an organism to limit or prevent viral replication, spread, and disease. This resistance is achieved through a multi-layered defense system, including both innate (nonspecific) and adaptive (specific) immunity. The effectiveness of these defenses varies among individuals and species, influenced by genetic, immunological, and environmental factors.
Resistance: Reduces viral burden by eliminating or controlling the pathogen.
Tolerance: Minimizes tissue damage caused by infection, even if the virus is not cleared.
Mechanisms of Host Resistance
Innate Immunity (Nonspecific Defenses)
Innate immunity provides the first line of defense against viral infections, acting rapidly and without prior exposure to the pathogen. It includes physical barriers, chemical defenses, and cellular responses.
Physical and Chemical Barriers
Skin: Acts as a physical barrier, preventing entry of viruses, bacteria, and toxins.
Mucus and Saliva: Trap and help eliminate pathogens from mucosal surfaces.
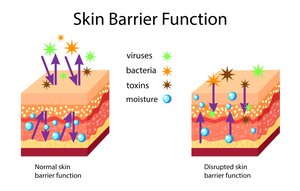
Cellular and Molecular Responses
Interferons (IFNs): Signaling proteins released by infected cells to alert neighboring cells and inhibit viral replication.
Natural Killer (NK) Cells: Immune cells that identify and destroy infected cells.
Antigen-Presenting Cells (APCs): Cells such as dendritic cells and macrophages that present viral antigens to initiate adaptive immunity.
Interferons and the Antiviral State
Interferons are crucial for establishing an antiviral state in cells. They are released by infected and neighboring cells, warning the immune system and activating antiviral defenses.
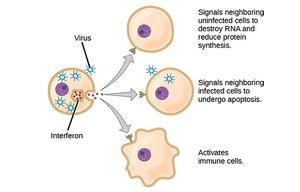
Induction of Interferon-Stimulated Genes (ISGs): IFNs signal neighboring cells to upregulate ISGs, which encode proteins that disrupt various stages of the viral life cycle.
Examples of ISG Actions: Degradation of viral RNA, inhibition of viral protein synthesis.
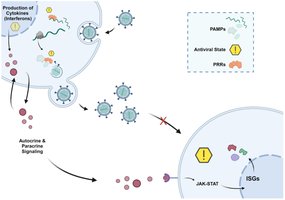
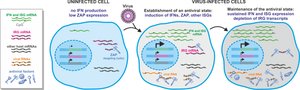
Natural Killer (NK) Cells
NK cells are a vital component of innate immunity, providing rapid responses to virally infected cells. They kill infected cells directly and secrete cytokines to coordinate the immune response.
Cytotoxic Killing: NK cells release perforin and granzymes to induce lysis of infected cells.
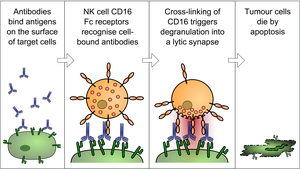
Antibody-Dependent Cell-Mediated Cytotoxicity (ADCC): NK cells recognize antibody-coated infected cells and induce apoptosis.
Cytokine Production: NK cells secrete cytokines that enhance antiviral immunity and modulate other immune cells.
Immunopathology: Excessive NK cell activity can cause tissue damage, highlighting the need for immune balance.
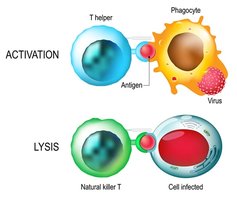
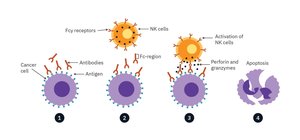
Antigen-Presenting Cells (APCs)
APCs, such as dendritic cells and macrophages, bridge innate and adaptive immunity. They ingest viruses, process antigens, and present them on MHC molecules to activate T cells in lymph nodes.
Dendritic Cells: Located in tissues exposed to the environment (e.g., skin, mucosa), they present antigens to T helper cells via MHC II molecules.
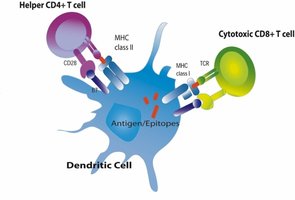
Adaptive Immunity (Specific Defenses)
Overview of Adaptive Immunity
Adaptive immunity develops more slowly but is highly specific to the infecting virus. It involves B cells (antibody production) and T cells (cell-mediated responses), and generates immunological memory for faster responses upon re-exposure.
B Cells: Produce antibodies that neutralize viruses and mark them for destruction.
T Cells: Include helper T cells (coordinate immune responses) and cytotoxic T cells (kill infected cells).
Immunological Memory: Memory B and T cells enable rapid, robust responses to future infections by the same virus.
Time Course of Immune Responses
Innate defenses act rapidly after infection, while adaptive responses (antibodies and T cells) take days to weeks to develop.
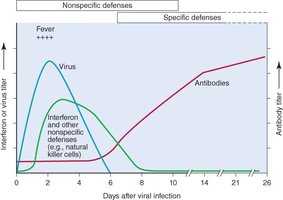
Humoral Response: Antibody Production
B cells are activated by viral antigens and differentiate into plasma cells that secrete antibodies. These antibodies neutralize viruses and facilitate their clearance.
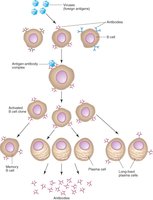
Neutralization: Antibodies bind to viral particles, blocking their attachment and entry into host cells.
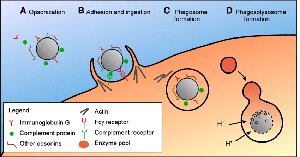
Opsonization: Antibodies coat viruses, marking them for phagocytosis by macrophages.
ADCC: Antibodies bound to infected cells recruit NK cells to induce apoptosis.
Cell-Mediated Response: T Cells
T cells are essential for eliminating viruses that have already infected host cells. There are two main subtypes: cytotoxic T cells (CD8+) and helper T cells (CD4+).
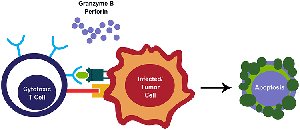
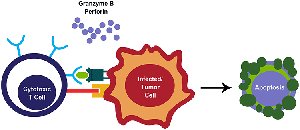
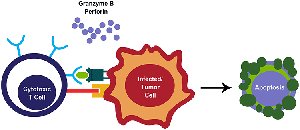
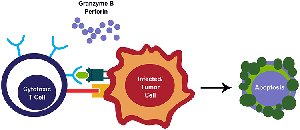
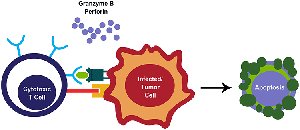
Cytotoxic T Cells (CD8+): Recognize viral antigens presented on MHC I molecules of infected cells and induce apoptosis via perforin and granzymes.
Helper T Cells (CD4+): Recognize antigens on MHC II molecules of APCs, secrete cytokines to activate B cells, cytotoxic T cells, and innate immune cells.
Helper T Cells (CD4+)
Antigen Presentation: Recognize viral antigens on MHC II molecules of APCs.
Activation of B Cells: Stimulate B cell maturation and antibody production.
Enhancement of Cytotoxic T Cells: Secrete cytokines (e.g., IFN-γ, IL-2) to promote cytotoxic T cell proliferation.
Boosting Innate Immunity: Activate macrophages and NK cells for enhanced antiviral activity.
Factors Influencing Host Resistance
Genetic Factors: Genes, especially those in the major histocompatibility complex (MHC), influence immune responses.
Physiological Factors: Age, nutrition, stress, and health status affect resistance to viral infections.
Co-evolution: Viruses evolve mechanisms to evade host defenses, leading to an evolutionary arms race.
Distinction Between Resistance and Tolerance
Resistance: Reduces the viral load by eliminating the pathogen.
Tolerance: Limits tissue damage without necessarily reducing viral burden.
Example: The body may minimize tissue damage even if the virus persists.
