 Back
BackHost–Microbe Interactions and Pathogenesis: Core Concepts and Clinical Implications
Study Guide - Smart Notes

Basics of Host–Microbe Interactions
Introduction to Host–Microbe Interactions
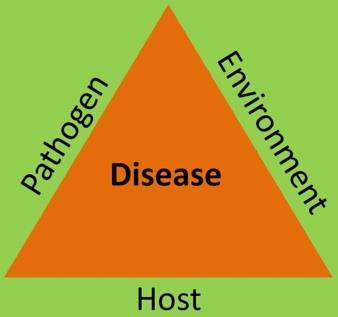
Host–microbe interactions are fundamental to understanding how microorganisms coexist with, benefit, or harm their hosts. These interactions can foster health or lead to disease, depending on the balance between the host, the microbe, and environmental factors.
Microbiota: The community of microorganisms (bacteria, archaea, protists, fungi, and viruses) that reside in a specific environmental niche, such as the human body.
Microbiome: The microbiota plus their collective genetic material and gene products within an environment.
Symbiotic Relationships: These include commensalism (benign coexistence), mutualism (both host and microbe benefit), and pathogenicity (microbe causes disease).
Dysbiosis: Disruption of the normal microbiota balance, which can compromise health and increase the risk for infections and disease.
Pathogen: A microorganism capable of causing disease.
Opportunistic Pathogen: Normally harmless but can cause disease in a compromised host or when introduced to an unusual site.
Emerging Pathogen: A newly identified or previously rare pathogen increasing in incidence.
Example: Clostridioides difficile (C. difficile) is a major healthcare-associated infection (HAI) that arises when antibiotics disrupt the normal gut microbiota, allowing C. difficile to flourish.
Normal Human Microbiota and Health
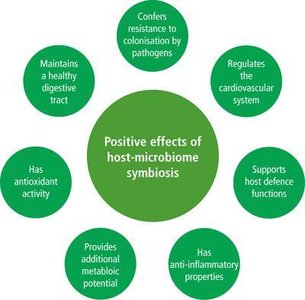
The human microbiota, also known as normal flora, consists of resident microbes on the skin, respiratory, genitourinary, and digestive systems. The composition and function of the microbiota are influenced by factors such as mode of delivery, diet, antibiotics, and environment.
Microbiota develops and evolves throughout life, playing a critical role in health.
Shifts in microbiota levels or location can promote disease.
Commensal organisms in one host may be pathogenic in another.
Example: Early antibiotic use in children is associated with increased risk of asthma and allergies due to impaired immune system development.
Dysbiosis and Disease
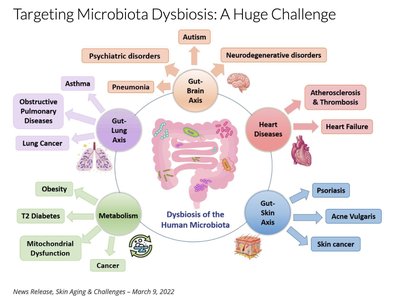
Dysbiosis refers to an imbalance in the normal microbiota, which can lead to increased susceptibility to infections and chronic diseases. The gut microbiome, in particular, is linked to metabolic, neurological, and immune-related disorders.
Factors affecting dysbiosis include antibiotics, diet, stress, genetics, and environmental exposures.
Dysbiosis is correlated with diseases such as asthma, obesity, diabetes, and autoimmune disorders.
Introduction to Virulence
Pathogenicity and Virulence
Pathogenicity is the ability of a microbe to infect a host and/or cause disease. Virulence refers to the degree or extent of disease/damage caused by a pathogen. Host–microbe interactions, including host immune fitness and microbiota balance, influence both pathogenicity and virulence.
Virulence Factors: Mechanisms or components that enable pathogens to infect, invade, damage host tissues, overcome defenses, or transmit to new hosts.
Virulence is an evolving property, shaped by selective pressures and host responses.
Pathogens may become attenuated (weakened) in the lab, losing virulence factors but remaining infectious.
Toxins as Virulence Factors
Toxins are substances produced by microbes that have adverse effects on the host. They are classified as endotoxins or exotoxins.
Endotoxins: Lipid A portion of lipopolysaccharide (LPS) in Gram-negative bacteria; released upon cell lysis and cause systemic inflammation (e.g., septic shock).
Exotoxins: Proteins (often enzymes) secreted by both Gram-positive and Gram-negative bacteria; highly potent and often immunogenic.
Toxigenic: Microbes that produce toxins.
Toxemia: Presence of toxins in the bloodstream.
Property | Endotoxins | Exotoxins |
|---|---|---|
Made of | Lipid (Lipid A of LPS) | Protein |
Produced by | Gram-negative bacteria | Gram-negative and Gram-positive bacteria |
Release | Upon cell lysis | Secreted by living cells |
Vaccines | No | Yes (toxoid vaccines) |
Toxicity | Less toxic (but can cause septic shock) | Highly toxic (small amounts) |
Infectious Dose (ID50) and Lethal Dose (LD50)
These metrics quantify the infectiousness and lethality of pathogens:
ID50: Number of pathogens required to infect 50% of exposed hosts. Lower ID50 indicates higher infectivity.
LD50: Amount of pathogen/toxin needed to kill 50% of affected hosts. Lower LD50 indicates higher virulence.
Example: Agent 1 with ID50 = 100 is more infectious than Agent 2 with ID50 = 10,000.
Steps to Infection
Five Steps to Infection
To establish an infection, a pathogen must complete five general tasks:
Enter the host (portal of entry)
Adhere to host tissues (adhesins, pili, tissue tropism)
Obtain nutrients and/or invade (invasins, biofilm formation)
Replicate while evading immune defenses
Transmit to a new host (portal of exit, reservoirs)
Adhesion and Tropism
Adhesion is mediated by surface molecules called adhesins, which bind to specific host cell receptors. Tropism refers to the preference of a pathogen for a specific host or tissue, determined by these interactions.
Pili (fimbriae) and other adhesins facilitate attachment.
Altering or blocking adhesins/receptors can prevent infection.
Biofilm Formation
Biofilms are multicellular communities of microbes encased in a protective extracellular polymeric substance (EPS) matrix. Biofilm formation enhances microbial survival, antibiotic resistance, and persistence in chronic infections.
Biofilms are common on medical devices and tissues.
Quorum sensing enables coordinated behavior within biofilms.
Invasion and Nutrient Acquisition
Pathogens use invasins (enzymes or proteins) to invade host tissues and obtain nutrients. Examples include:
Flagella: Enhance motility and spread.
Collagenases: Break down collagen for tissue invasion.
Neuraminidases: Disrupt host cell communication.
Coagulases/Kinases: Manipulate blood clotting to protect or spread pathogens.
Siderophores: Scavenge iron from host proteins.
Immune Evasion
Pathogens employ various strategies to evade host immune defenses:
Antigen masking, mimicry, and variation: Alter or hide antigens to avoid detection.
Latency: Remain dormant to escape immune response.
Intracellular lifestyle: Survive within host cells.
Suppression of immune function: Target immune cells, break down antibodies, or block immune signals.
Avoidance of phagocytosis: Produce capsules, block phagosome-lysosome fusion, or neutralize enzymes.
Transmission and Reservoirs
Transmission to a new host or reservoir is essential for pathogen survival. Reservoirs can be animate (humans, animals) or inanimate (soil, water, fomites). Portals of exit often match portals of entry and are associated with symptoms that facilitate spread (e.g., coughing, diarrhea).
Biosafety and Standard Precautions in Health Care
Biosafety Levels (BSL)
Biosafety levels (BSL-1 to BSL-4) are assigned based on the infectivity, disease severity, transmission mode, and availability of treatments for pathogens. BSL dictates laboratory and clinical safety practices.
BSL-1: Well-characterized agents, rarely cause disease in healthy people.
BSL-2: Pathogens causing treatable or preventable human disease.
BSL-3: Cause serious or lethal disease, often untreatable.
BSL-4: Exotic, lethal pathogens with no cures or treatments.
Infection Control Practices
Infection control teams implement strategies to limit infection risks in healthcare settings. Practices include:
Standard Precautions: Universal measures for all patients (hand hygiene, gloves, PPE, disinfection, proper waste management).
Transmission Precautions: Additional measures for specific infectious agents (contact, droplet, airborne precautions).
Summary Table: Key Terms and Concepts
Term | Definition |
|---|---|
Microbiota | Community of microorganisms in a niche |
Microbiome | Microbiota plus genetic material |
Dysbiosis | Disruption of normal microbiota balance |
Pathogen | Microbe capable of causing disease |
Virulence | Degree of pathogenicity |
Endotoxin | Lipid A of LPS in Gram-negative bacteria |
Exotoxin | Secreted protein toxin |
ID50 | Infectious dose for 50% of hosts |
LD50 | Lethal dose for 50% of hosts |
Reservoir | Natural habitat of a pathogen |
BSL | Biosafety level |
