 Back
BackHost–Microbe Interactions and Pathogenesis: Core Concepts and Clinical Implications
Study Guide - Smart Notes

Host–Microbe Interactions and Pathogenesis
Basics of Host–Microbe Interactions
Host–microbe interactions are fundamental to understanding how microorganisms can both support health and contribute to disease. The balance between the host, the microbe, and the environment determines the outcome of these interactions.
Microbiota: The community of microorganisms (bacteria, archaea, protists, fungi, and viruses) that inhabit a specific environmental niche, such as the human body.
Microbiome: The microbiota plus their collective genetic material and gene products within an environment.
Symbiotic Relationships: These include commensalism (microbes coexist without harming the host), mutualism (both host and microbe benefit), and pathogenicity (microbes cause disease).
Dysbiosis: Disruption of the normal microbiota balance, which can compromise health and increase susceptibility to infections and disease.
Pathogen: A microorganism capable of causing disease.
Opportunistic Pathogen: Normally harmless microbes that can cause disease under certain conditions, such as immune suppression or microbiota imbalance.
Emerging Pathogen: Microbes that are newly identified or increasing in incidence.
The human microbiome is dynamic, evolving throughout life, and is influenced by factors such as diet, antibiotics, genetics, and environment. It plays a critical role in health, including immune system development, nutrient metabolism, and protection against pathogens.
Dysbiosis and Disease
Dysbiosis can lead to increased risk for infections, metabolic disorders, autoimmune diseases, and allergies. For example, early antibiotic use is associated with increased incidence of asthma and allergic diseases.
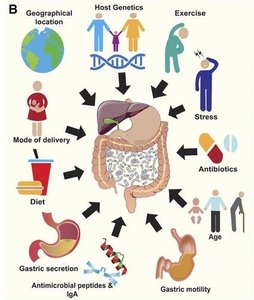
Factors Affecting the Microbiome
Mode of delivery (C-section vs. vaginal birth)
Feeding patterns (breastfeeding vs. formula)
Diet, antibiotics, stress, age, genetics, and environmental exposures
Microbiota and Immune System Development
Exposure to diverse microbes in childhood is necessary for proper immune system development. Dysbiosis impairs immune function and increases the risk of chronic diseases.
Introduction to Virulence
Virulence refers to the degree of pathogenicity of a microbe, or its ability to cause disease. Pathogenicity is the ability to infect and/or damage a host. Virulence factors are microbial mechanisms or components that enable infection, invasion, immune evasion, and transmission.
Virulence Factors: Include toxins, adhesins, invasins, immune evasion mechanisms, and nutrient acquisition systems.
True Pathogen: Causes disease in healthy hosts.
Attenuated Pathogen: Weakened form, often used in vaccines.
Toxin: A substance produced by microbes that causes damage to the host.
Toxigenic: Microbes that produce toxins.
Toxemia: Presence of toxins in the bloodstream.
Septic Shock: Life-threatening condition caused by systemic inflammatory response to infection, often due to endotoxins.
Endotoxins vs. Exotoxins
Property | Endotoxins | Exotoxins |
|---|---|---|
Made of | Lipid (Lipid A of LPS) | Protein |
Made by | Gram-negative bacteria | Gram-negative and Gram-positive bacteria |
Released from | G- cell wall when bacteria divide or die (in OM) | Actively growing bacteria (produced & secreted; released) or lysis |
Vaccines | No | Yes (immunogenic, neutralized) |
Fever/Symptoms | Yes (inflammatory)/general malaise (all produce same effects) | Sometimes (certain superantigens)/ specific for a particular cell or body function |
Can be neutralized in patient? | No | Yes (some) |
Toxicity | Less toxic (but can cause septic shock and organ failure in high concentrations) | Highly toxic (small amounts, usually targets specific type of cell) |
Infectious Dose (ID50) and Lethal Dose (LD50)
ID50: Number of pathogens required to infect 50% of exposed hosts.
Lower ID50 indicates higher infectivity.
Highly infectious does not equal especially dangerous
LD50: Amount of pathogen or toxin needed to kill 50% of affected hosts.
Lower LD50 = higher virulence (death).
ID50 AND LD50 change based on
Species affected
host's immune fitness
route of exposure
Five Steps to Infection
To establish an infection, a pathogen must complete five steps:
Entry: Pathogen enters the host via specific portals (e.g., respiratory, GI, urogenital, skin, parenteral, transplacental).
most common: mucous membranes
Maybe where disease develops
Some pathogens have >1 portal of entry
PORTALS OF ENTRY
Respiratory mucosa (including ocular)
▪ Most common portal of entry
▪ Microbes transmitted by CONTACT with mucosa of mouth/eyes/nose or INHALATION of respiratory droplets, aerosols, or dust particles
▪ May infect other area(s)
Skin
▪ Largest body system
▪ Physical protective barrier
▪ Has to be penetrated for infection to occur
GI Mucosa
▪ Infections frequently due to fecal-oral transmission via contaminated food, water or fingers
▪ Disease may occur elsewhere
Urogenital Systems
▪ Most STIs acquired through the mucosa; some through skin
▪ Urinary tract infections often normal flora
Parental
▪ Introduced directly into bloodstream intravenously or by injection
Transplacental
▪ Some pathogens exhibit vertical transmission
▪ Spread from mother to developing child in utero
Adhesion: Pathogen attaches to host tissues using adhesins (e.g., pili, surface proteins).
Pili (fimbriae) are bacterial adhesions that assemble into hair-like appendages and extend from the cell surface; other adhesions are directly associated with the microbial cell surface
species and tissue tropism is due to specificity for attachment to a particular host cell surface marker.
Colonization involves biofilm formation
1. Bacteria alternate between two distinct life phases: planktonic (free-floating) and biofilm-associated (multicellular communities of attached sessile cells)
2. Planktonic bacterial attachment and colonization of surfaces is critical during for the development of a sustainable, persistent population within a mature biofilm
3. Biofilms are cooperative communities of adherent microbes encased in a protective, sticky, slimy, matrix layer
Multiple layers develop; residents of the innermost layers are highly protected
Can form on almost any surface, especially prevalent in aqueous enviroments
Share nutrients, protected from environmental stressors
4. Microbes within the biofilm periodically detach and are released as free-growing planktonic cells; results in recurrence of disease and/or spread to new areas to begin process again
Invasion/Nutrient Acquisition: Pathogen invades tissues and obtains nutrients using invasins and extracellular enzymes.
Immune Evasion: Pathogen evades host immune defenses through antigenic variation, latency, intracellular lifestyle, and immune suppression.
Antigen masking, mimicry, and variation
Latency (dormancy)
Intracellular lifestyle- reside, multiply, and survive inside host cells (pirates)
Suppression of immune function
Avoidance of phagocytosis (e.g., capsules, inhibition of phagosome-lysosome fusion)
Transmission: Pathogen exits the host via portals of exit (e.g., respiratory droplets, feces, blood, urine) to infect new hosts.
1. The last crucial step in a pathogen’s success is transmission to a new host or back into natural reservoir for propagation/persistence
2. Reservoir– habitat where pathogen is typically found
Animate or inanimate source when pathogen is normally lives and reproduces (human, non-human animal, plant, environmental niche, fomite)
Identification useful in preventing disease and stopping large outbreaks
▪Control disease by eliminating/protecting against exposure to pathogen’s reservoir
Biosafety and Standard Precautions in Health Care
Biosafety levels (BSL-1 to BSL-4) are assigned based on the infectivity, disease severity, transmission mode, and availability of treatments for pathogens. Standard precautions are universal measures to prevent transmission of infectious agents in healthcare settings, including hand hygiene, use of personal protective equipment (PPE), and proper waste management. Transmission-based precautions (contact, droplet, airborne) are used for specific pathogens.
Biosafety Levels
BSL | Description |
|---|---|
BSL-1 | Agents not known to cause disease in healthy adults |
BSL-2 | Agents associated with human disease; moderate hazard |
BSL-3 | Agents that may cause serious or potentially lethal disease via inhalation |
BSL-4 | Dangerous/exotic agents with high risk of life-threatening disease |
– BSL-1 & -2 = most laboratories, hospitals, health care settings
– BSL-3 & -4 = restricted to approved clinical/research facilities
Standard Precautions
Hand hygiene before and after patient contact
Use of gloves, gowns, masks, and face shields as needed
Proper handling and disposal of sharps and biohazardous waste
Disinfection of surfaces and equipment
Transmission Precautions
Contact: wound/skin infections spread by direct or indirect contact (e.g., MRSA, C. difficile)
Droplet: For pathogens spread by respiratory droplets (e.g., influenza, pertussis)- coughing/sneezing
Airborne: For pathogens spread by airborne particles (e.g., tuberculosis, measles)
Summary Table: Key Terms and Concepts
Term | Definition |
|---|---|
Microbiota | Community of microorganisms in a specific environment |
Microbiome | Microbiota plus their genetic material |
Dysbiosis | Disruption of normal microbiota balance |
Pathogen | Microbe capable of causing disease |
Virulence | Degree of pathogenicity |
Virulence Factor | Microbial component that aids infection |
Endotoxin | Lipid A of LPS in Gram-negative bacteria |
Exotoxin | Secreted protein toxin |
ID50 | Infectious dose for 50% of hosts |
LD50 | Lethal dose for 50% of hosts |
