 Back
BackImmune Disorders: Hypersensitivities, Autoimmune Diseases, and Immunodeficiencies
Study Guide - Smart Notes

Immune Disorders
Overview of Immune Disorders
Immune disorders arise when the immune system malfunctions, leading to exaggerated, insufficient, or misdirected immune responses. These disorders are classified into hypersensitivities, autoimmune diseases, and immunodeficiencies.
Hypersensitivities
Definition and Types
Hypersensitivity refers to any immune response against a foreign antigen that is exaggerated beyond the norm. There are four main types:
Type I (Immediate)
Type II (Cytotoxic)
Type III (Immune Complex–Mediated)
Type IV (Delayed or Cell-Mediated)
Type I (Immediate) Hypersensitivity
This type involves a rapid, localized or systemic reaction resulting from the release of inflammatory molecules in response to an antigen (allergen). Commonly called allergies, these reactions develop within seconds or minutes after exposure.
Allergens: Antigens that trigger allergic reactions.
Two-step process:
Sensitization: Initial exposure to allergen leads to IgE production.
Degranulation: Subsequent exposure causes sensitized cells to release inflammatory mediators.
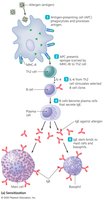
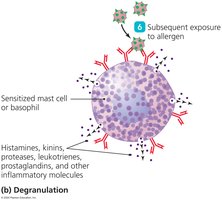
Cells Involved in Type I Hypersensitivity
Mast Cells: Found throughout connective tissue; release histamine, kinins, proteases, leukotrienes, and prostaglandins upon degranulation.
Basophils: Least numerous leukocytes; degranulate like mast cells when encountering allergens.
Eosinophils: Accumulate in blood during allergic responses; release leukotrienes, increasing severity of reactions.
Clinical Manifestations
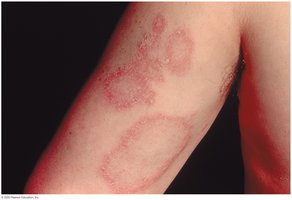
Localized reactions: Mild, site-dependent (e.g., hay fever, asthma, hives/urticaria).
Systemic reactions: Massive degranulation can cause acute anaphylaxis or anaphylactic shock, requiring immediate treatment with epinephrine.

Diagnosis, Prevention, and Treatment
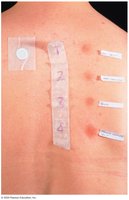
Diagnosis: Detection of allergen-specific IgE (e.g., ImmunoCAP test) or skin tests.
Prevention: Avoidance of allergens, elimination diets, immunotherapy (allergy shots).
Treatment: Antihistamines, glucocorticoids, bronchodilators, and epinephrine for severe reactions.
Type II (Cytotoxic) Hypersensitivity
Type II hypersensitivity results when cells are destroyed by an immune response, often involving complement and antibodies. It is a component of many autoimmune diseases.
Examples:
Destruction of blood cells after incompatible blood transfusion (ABO system).
Hemolytic disease of the newborn (Rh system).
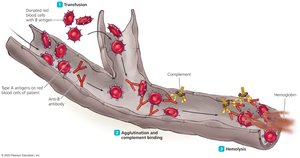
The ABO System and Transfusion Reactions
Blood group antigens (A, B, AB, O) are surface molecules on red blood cells.
Transfusion of incompatible blood leads to antibody-mediated destruction of donor cells.
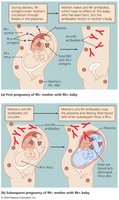
The Rh System and Hemolytic Disease of the Newborn
Rh antigen is present in 85% of humans (Rh+).
Rh− mothers carrying Rh+ fetuses may develop antibodies that attack fetal red blood cells in subsequent pregnancies.
Prevention: Administration of anti-Rh immunoglobulin (RhoGAM).
Type III (Immune Complex–Mediated) Hypersensitivity
This type is caused by the formation of immune complexes that trigger inflammation. It can cause localized or systemic reactions.
Localized reactions: Hypersensitivity pneumonitis, glomerulonephritis.
Systemic reactions: Systemic lupus erythematosus (SLE), rheumatoid arthritis (RA).

Examples
Hypersensitivity pneumonitis: Inhaled antigens form immune complexes in the lungs.
Glomerulonephritis: Immune complexes deposit in kidney glomeruli, causing inflammation and potential kidney failure.
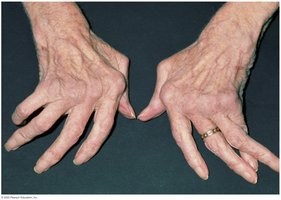
Rheumatoid arthritis (RA): Immune complexes in joints cause inflammation and joint distortion.
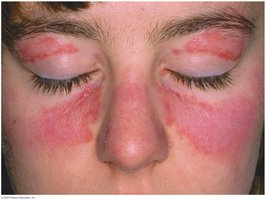
Systemic lupus erythematosus (SLE): Autoantibodies against DNA and other cell components cause widespread inflammation and tissue damage.
Type IV (Delayed or Cell-Mediated) Hypersensitivity
Type IV hypersensitivity is mediated by T cells and occurs 12–24 hours after antigen exposure. It involves inflammation due to the actions of antigen-presenting cells and T cells.
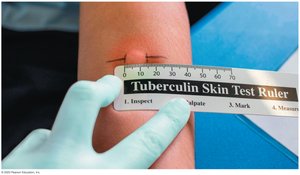
Tuberculin response: Skin reaction to tuberculin injection in individuals previously exposed to Mycobacterium tuberculosis.
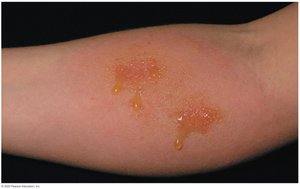
Allergic contact dermatitis: Skin rash caused by contact with allergens like poison ivy, latex, or chemicals.
Graft rejection: Immune response against transplanted tissues or organs due to foreign MHC proteins.
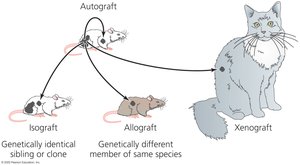
Graft-versus-host disease: Donated bone marrow cells attack recipient tissues if MHC mismatch exists.
Donor-recipient matching: Tissue typing and immunosuppressive drugs are used to reduce rejection risk.
Autoimmune Diseases
Causes of Autoimmune Diseases
Autoimmune diseases occur when the immune system attacks the body's own cells. They are more common in the elderly and in women. Causes include hormonal influences, genetic factors, environmental triggers, molecular mimicry, and failure of immune regulation.
Estrogen may stimulate cytotoxic T cell activity.
Maternal or fetal cells crossing the placenta may trigger autoimmunity.
Viral infections and certain MHC genes increase risk.
Self-antigens normally hidden may be exposed to T cells.
Examples of Autoimmune Diseases
Systemic autoimmune diseases: Affect multiple organs (e.g., SLE, RA).
Single-organ autoimmune diseases: Target specific organs (e.g., blood cells, endocrine glands, nervous tissue).
Autoimmune hemolytic anemia: Antibodies against red blood cells cause anemia.
Type 1 diabetes mellitus: Immune attack on pancreatic islets leads to insulin deficiency.
Graves’ disease: Autoantibodies stimulate thyroid hormone production, causing goiter.
Multiple sclerosis (MS): Cytotoxic T cells destroy myelin sheaths in the CNS, impairing function.
Immunodeficiency Diseases
Types of Immunodeficiency Diseases
Immunodeficiency diseases result from defective immune mechanisms and are classified as primary (congenital) or acquired.
Primary immunodeficiency diseases: Genetic or developmental defects, manifest in infants and children.
Acquired immunodeficiency diseases: Develop later in life due to aging, stress, malnutrition, or infections (e.g., AIDS).
Acquired immunodeficiency syndrome (AIDS) is characterized by opportunistic infections, low CD4 cells, and HIV infection.
Additional info: For all hypersensitivity types, the underlying mechanisms involve inappropriate or excessive immune responses, which can be targeted by specific therapies or prevented by avoiding triggers. Autoimmune diseases often require immunosuppressive treatment, while immunodeficiencies may need supportive care or immune reconstitution.
