 Back
BackImmune Disorders: Hypersensitivity and Autoimmunity
Study Guide - Smart Notes

Immune Disorders
Overview of Immune Disorders
Immune disorders arise when the immune system malfunctions, leading to exaggerated, misdirected, or uncontrolled immune responses. These disorders include hypersensitivity reactions and autoimmune diseases, which can cause significant tissue damage and pathology.
Hypersensitivity Reactions
Definition and Classification
Hypersensitivity refers to any immune response against a foreign antigen that is exaggerated beyond the norm. There are four major types of hypersensitivity reactions, each with distinct mechanisms, time courses, and clinical manifestations.
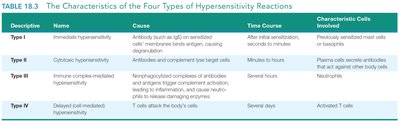
Type | Name | Cause | Time Course | Characteristic Cells Involved |
|---|---|---|---|---|
I | Immediate hypersensitivity | Antibody (mainly IgE) on sensitized cells interacts with antigen, causing degranulation | After initial sensitization, seconds to minutes | Previously sensitized mast cells or basophils |
II | Cytotoxic hypersensitivity | Antibodies and complement lyse target cells | Minutes to hours | Plasma cells secrete antibodies that act against other body cells |
III | Immune complex-mediated hypersensitivity | Nonphagocytized complexes of antibody and antigen trigger complement activation, inflammation, and neutrophil damage | Several hours | Neutrophils |
IV | Delayed (cell-mediated) hypersensitivity | T cells attack the body's cells | Several days | Activated T cells |
Type I (Immediate) Hypersensitivity
Type I hypersensitivity, also known as anaphylactic hypersensitivity, is a rapid, localized or systemic reaction resulting from the release of inflammatory molecules in response to an antigen. The antigens that trigger this response are called allergens. Common examples include pollen, dust mites, and certain foods.
Mechanism: Develops within seconds or minutes after exposure to an allergen.
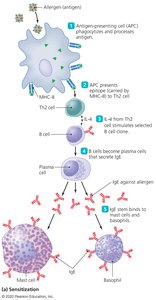
Two-step process:
Sensitization: Initial exposure to allergen leads to IgE production and binding to mast cells or basophils.
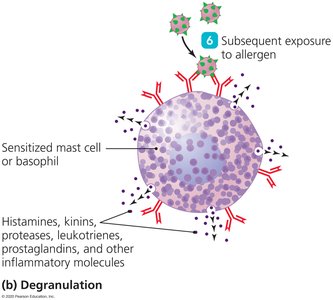
Degranulation: Subsequent exposure causes cross-linking of IgE, leading to release of histamine and other mediators.
Clinical manifestations: Allergic rhinitis, asthma, anaphylaxis.
Examples of Allergens
Pollen grains
Mold spores
House dust mites

Type II (Cytotoxic) Hypersensitivity
Type II hypersensitivity occurs when antibodies target and destroy cells, often with the help of complement. This type is involved in several autoimmune diseases and transfusion reactions.
Mechanism: Antibodies bind to antigens on cell surfaces, leading to cell lysis via complement activation or antibody-dependent cellular cytotoxicity.
Examples:
Destruction of blood cells after incompatible blood transfusion
Hemolytic disease of the newborn (Rh incompatibility)
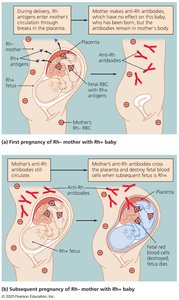
ABO Blood Group Compatibility
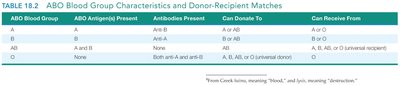
ABO Blood Group | ABO Antigen(s) Present | Antibodies Present | Can Donate To | Can Receive From |
|---|---|---|---|---|
A | A | Anti-B | A or AB | A or O |
B | B | Anti-A | B or AB | B or O |
AB | A and B | None | AB | A, B, AB, or O (universal recipient) |
O | None | Both anti-A and anti-B | A, B, AB, or O (universal donor) | O |

Type III (Immune Complex–Mediated) Hypersensitivity
Type III hypersensitivity is caused by the formation of immune complexes (antigen-antibody complexes) that are not efficiently cleared. These complexes deposit in tissues, triggering inflammation and tissue damage.
Mechanism: Immune complexes activate complement and attract neutrophils, leading to inflammation and tissue injury.
Examples:
Hypersensitivity pneumonitis
Glomerulonephritis
Systemic lupus erythematosus (SLE)
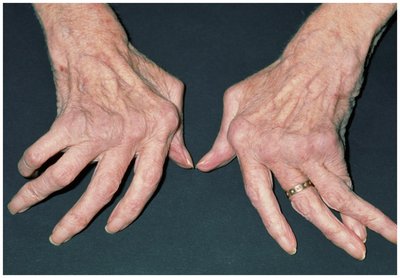
Rheumatoid arthritis (RA)
Type IV (Delayed or Cell-Mediated) Hypersensitivity
Type IV hypersensitivity is mediated by T cells rather than antibodies. The reaction is delayed, typically appearing 12–24 hours after antigen exposure.
Mechanism: Antigen-presenting cells activate T cells, which then mediate inflammation and tissue damage.
Examples:
Tuberculin response (e.g., Mantoux test for tuberculosis)
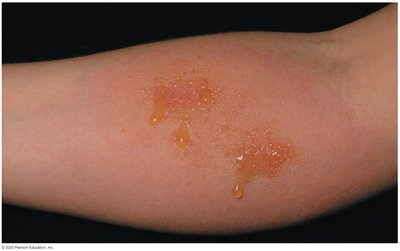
Contact dermatitis (e.g., poison ivy)
Graft rejection
Autoimmune Diseases
Overview and Causes
Autoimmune diseases occur when the immune system mistakenly targets and attacks the body's own tissues. These diseases are more common in the elderly and in women. The exact causes are complex and multifactorial, involving genetic, hormonal, and environmental factors.
Possible causes:
Estrogen may stimulate cytotoxic T cell activity
Maternal or fetal cells crossing the placenta
Environmental triggers (e.g., viral infections)
Genetic predisposition (e.g., certain MHC genes)
Exposure of hidden self-antigens
Molecular mimicry by microorganisms
Failure of immune regulation mechanisms
Examples of autoimmune diseases: Type I diabetes, rheumatoid arthritis, multiple sclerosis, lupus, inflammatory bowel disease (IBD), and possibly Alzheimer's disease.

Criteria for a Good Vaccine
Key Features of Effective Vaccines
A good vaccine should provide long-lasting protection with minimal side effects. It should be safe, stable, and easy to administer.
Induces strong and long-lasting immunity
Safe with minimal adverse effects
Stable and easy to store/transport
Cost-effective and accessible
Capable of inducing both humoral and cellular immune responses
Minimal risk of causing disease in immunized individuals
Summary Table: Hypersensitivity Types
Type | Mechanism | Time Course | Examples |
|---|---|---|---|
I | IgE-mediated degranulation of mast cells/basophils | Seconds to minutes | Allergies, anaphylaxis |
II | Antibody-mediated cell destruction | Minutes to hours | Transfusion reactions, hemolytic disease of the newborn |
III | Immune complex deposition and inflammation | Several hours | SLE, RA, glomerulonephritis |
IV | T cell-mediated tissue damage | 12–24 hours or more | Contact dermatitis, graft rejection |
