 Back
BackImmune System Disorders: Immunodeficiencies, Autoimmunity, and Hypersensitivity Reactions
Study Guide - Smart Notes

Immune System Disorders
Overview
Immune system disorders encompass a range of conditions where the immune system is either underactive (immunodeficiency), overactive (hypersensitivity), or misdirected against self-tissues (autoimmunity). Understanding these disorders is crucial for microbiology students, as they illustrate the balance required for effective immune defense and the consequences of immune dysregulation.
Immunodeficiency
Primary and Secondary Immunodeficiencies
Immunodeficiency refers to the lack of a properly functioning immune system. These conditions can be classified as:
Primary immunodeficiency: Genetic or congenital defects present from birth, affecting one or more immune factors. Over 300 disorders are known, with varying severity and treatment options.
Secondary immunodeficiency: Acquired later in life due to aging, infections (e.g., HIV), medical interventions, or systemic diseases (e.g., diabetes, malnutrition).
Primary immunodeficiencies are further classified based on the affected immune component:
B cell/antibody deficiencies (e.g., X-linked agammaglobulinemia, selective IgA deficiency)
T cell deficiencies (e.g., DiGeorge syndrome, SCID)
Phagocyte defects (e.g., chronic granulomatous disease)
Complement protein deficiencies (e.g., C2, C4, C9 deficiencies)
Treatment options include bone marrow transplants, antibody administration, cytokine therapies, and experimental approaches such as gene therapy.
Secondary Immunodeficiencies
Secondary immunodeficiencies are more common and often reversible if the underlying cause is addressed. Causes include:
Age-related decline
Infectious agents (e.g., HIV targets CD4+ T cells, leading to AIDS)
Immunosuppressive drugs (e.g., corticosteroids, immunosuppressants for transplants)
Chronic diseases (e.g., diabetes, malnutrition)
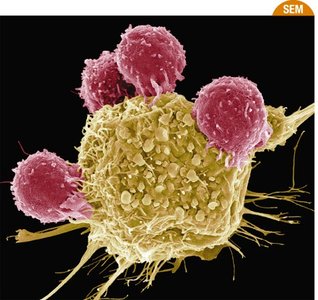
Immunodeficiencies can increase susceptibility to infections and certain cancers, as the immune system also surveils for malignant cells.
Autoimmunity
Mechanisms and Examples
Autoimmunity occurs when the immune system attacks healthy self-tissues, leading to autoimmune disorders. These conditions may be systemic (affecting multiple organs) or localized (targeting specific tissues). Genetics and environmental triggers, such as infections, contribute to their development.
Examples: Type 1 diabetes, multiple sclerosis, rheumatoid arthritis, systemic lupus erythematosus (SLE), Hashimoto's thyroiditis, celiac disease.
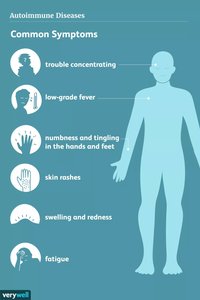
Common symptoms include joint and muscle pain, fatigue, rash, organ dysfunction, and low-grade fever.
Diagnosis and Management
Diagnosis involves detecting self-reactive immune cells or autoantibodies, along with clinical evaluation and laboratory tests. Management focuses on suppressing the immune response and reducing inflammation, but often leads to secondary immunodeficiency. There are currently no cures for autoimmune diseases.
Hypersensitivity Reactions
Classification and Mechanisms
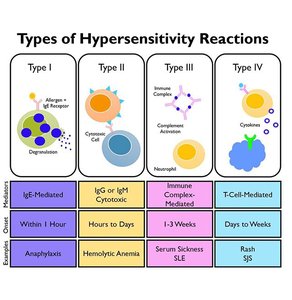
Hypersensitivities are inappropriate or exaggerated immune responses to harmless antigens or self-antigens. The Gell and Coombs classification system divides hypersensitivities into four types:
Type | Mechanism | Onset | Examples |
|---|---|---|---|
I (Immediate) | IgE-mediated, mast cell degranulation | Within 1 hour | Allergies, anaphylaxis |
II (Cytotoxic) | IgG/IgM bind to cell surface antigens, complement activation | Hours to days | Hemolytic anemia, blood transfusion reactions |
III (Immune Complex) | IgG/IgM-antigen complexes deposit in tissues | 1–3 weeks | SLE, serum sickness |
IV (Delayed) | T cell-mediated, cytokine release | Days to weeks | Contact dermatitis, multiple sclerosis |
Type I Hypersensitivity (Immediate, IgE-Mediated)
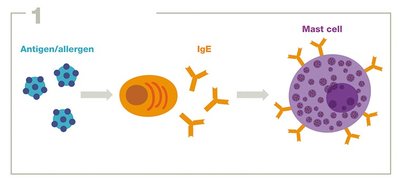
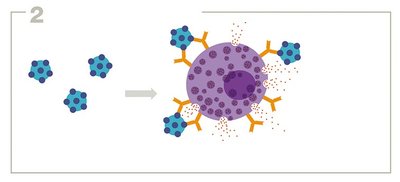
Type I reactions involve IgE antibodies binding to allergens, leading to mast cell or basophil degranulation and release of inflammatory mediators. Common manifestations include allergies (e.g., hay fever, food allergies) and anaphylaxis.
Sensitization: Initial exposure triggers IgE production, which binds to mast cells.
Re-exposure: Allergen cross-links IgE, causing degranulation and symptoms.
Diagnosis and Management
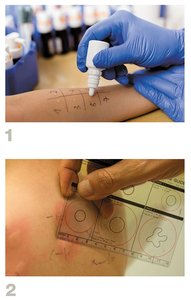
Blood tests for allergen-specific IgE
Skin prick tests to identify allergens
Desensitization therapy for some allergens
Epinephrine for anaphylaxis
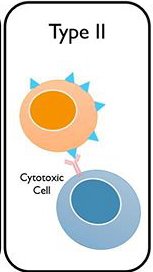
Type II Hypersensitivity (Cytotoxic, Antibody-Mediated)
Type II reactions occur when IgG or IgM antibodies bind to antigens on cell surfaces, leading to cell destruction via complement activation or phagocytosis. Examples include blood transfusion reactions, hemolytic disease of the newborn, and some autoimmune diseases.
Blood Groups and Transfusion Reactions
Blood types are determined by carbohydrate (A, B, O) and protein (Rh) antigens on red blood cells. Incompatible transfusions can cause hemolytic reactions, which are life-threatening.
Blood Type | Antigens Present | Can Receive From |
|---|---|---|
AB+ | A, B, Rh | All types (universal recipient) |
O− | None | O− only (universal donor) |
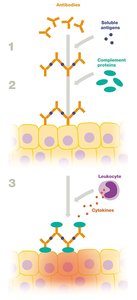
Type III Hypersensitivity (Immune Complex-Mediated)
Type III reactions involve the formation of antigen-antibody complexes that deposit in tissues, activating complement and causing inflammation. This can lead to tissue damage in diseases such as systemic lupus erythematosus and rheumatoid arthritis.
Type IV Hypersensitivity (Delayed, T Cell-Mediated)
Type IV reactions are mediated by T cells rather than antibodies. They manifest 12–72 hours after antigen exposure and are responsible for conditions such as contact dermatitis (e.g., poison ivy), graft rejection, and autoimmune diseases like multiple sclerosis and type 1 diabetes.
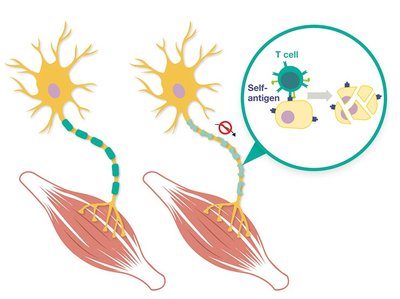
Non-Autoimmune Type IV Hypersensitivities
Examples include contact dermatitis from poison ivy, nickel, or latex. Therapies focus on reducing T cell responses and inflammation.
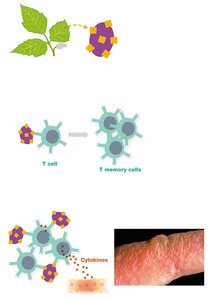
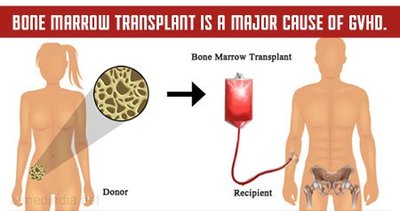
Transplant Rejection and Graft-versus-Host Disease (GVHD)
Transplant rejection occurs when T cells recognize transplanted tissue as foreign. GVHD is a complication of bone marrow transplants, where donor immune cells attack the recipient's tissues.
Visual Summary
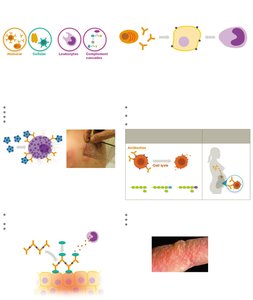
Key Terms
Immunodeficiency: Impaired immune function, either congenital or acquired.
Autoimmunity: Immune response against self-antigens.
Hypersensitivity: Exaggerated or inappropriate immune response to antigens.
Anaphylaxis: Severe, systemic allergic reaction.
Graft-versus-host disease (GVHD): Immune attack by transplanted cells on the recipient.
