 Back
BackInfection, Infectious Diseases, and Epidemiology: Structured Study Notes
Study Guide - Smart Notes

Infection, Infectious Diseases, and Epidemiology
Symbiotic Relationships Between Microbes and Their Hosts
Microbes interact with their hosts in various symbiotic relationships, ranging from harmless coexistence to pathogenicity. The human microbiome consists of organisms that colonize the body’s surfaces without normally causing disease, also known as normal microbiota, normal flora, or indigenous microbiota.
Resident microbiota: Mostly commensal, non-pathogenic organisms that are permanently established.
Transient microbiota: Microbes that remain in the body for a short period and are found in the same regions as resident microbiota but cannot persist due to competition, elimination by defense cells, or changes in the body.
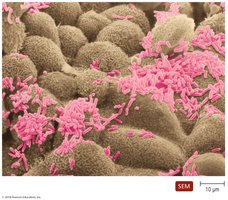
Normal Microbiota in Hosts
The acquisition of the microbiome begins during the birthing process, as the womb is typically free of microorganisms. Much of one’s resident microbiota is established during the first months of life.
Competition: Resident microbiota compete with transient microbiota, preventing their persistence.
Elimination: Body defense cells and chemical/physical changes remove transient microbes.
Distribution of Resident Microbiota
Resident microbiota are distributed throughout various body systems, each with characteristic genera and ecological notes.
Body System | Genera | Notes |
|---|---|---|
Upper Respiratory Tract | Actinomyces, Haemophilus, Lactobacillus, Moraxella, Streptococcus, Staphylococcus, Neisseria, Candida | This area is near the end of the respiratory system and hosts unique microbiota. The microbiota of the nostrils and mouth are sparse compared to those of the nose and mouth. |

Body System | Genera | Notes |
|---|---|---|
Upper Digestive Tract | Actinomyces, Bacteroides, Corynebacterium, Fusobacterium, Lactobacillus, Neisseria, Streptococcus, Treponema | Microbes colonize surfaces of teeth, gums, cheeks, and pharynx; they have been identified in large numbers. |
Lower Digestive Tract | Bacteroides, Clostridium, Enterococcus, Escherichia, Lactobacillus, Proteus, Streptococcus | Bacteria are mostly anaerobic, though some facultative anaerobes are also present. |

Body System | Genera | Notes |
|---|---|---|
Female Urinary and Reproductive Systems | Actinomyces, Candida, Lactobacillus, Staphylococcus, Streptococcus | Microbiota change as activity in the vagina changes during menstrual cycles. The flow of urine prevents colonization of the urinary bladder or urethra. |
Male Urinary and Reproductive Systems | Actinomyces, Lactobacillus, Staphylococcus, Streptococcus | The flow of urine prevents colonization of the urinary bladder or urethra. |

Body System | Genera | Notes |
|---|---|---|
Eyes and Skin | Staphylococcus, Micrococcus, Propionibacterium, Streptococcus, Candida | Microbiota live on the outer dead layers of the skin and in hair follicles and pores of glands. The deeper layers (dermis and hypodermis) are sterile. |

Normal Microbiota Can Become Opportunistic Pathogens
Normal microbiota may cause disease under certain circumstances, especially in individuals with weakened or depressed immune responses. These are termed opportunistic pathogens.
Conditions for opportunism: Introduction into unusual sites, immune suppression, changes in normal microbiota, and stressful conditions.
Reservoirs of Infectious Diseases of Humans
Pathogens require reservoirs to survive outside their host. Reservoirs are sites where pathogens are maintained as sources of infection.
Animal reservoirs: Diseases naturally spread from animal hosts to humans (zoonoses).
Human carriers: Asymptomatic infected individuals can transmit pathogens.
Nonliving reservoirs: Soil, water, and food contaminated by feces or urine.
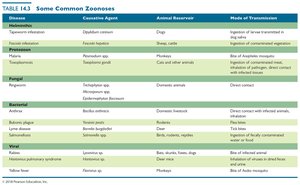
Common Zoonoses
Zoonoses are diseases that spread from animals to humans via direct contact, ingestion, or bloodsucking arthropods. Humans are often dead-end hosts, and zoonoses can be difficult to eradicate.
Disease | Causative Agent | Animal Reservoir | Mode of Transmission |
|---|---|---|---|
Rabies | Rabies virus | Dogs, cats, other animals | Bite of infected animal |
Lyme disease | Borrelia burgdorferi | Deer, rodents | Bite of infected tick |
Ringworm | Microsporum | Domestic animals | Direct contact with infected animal |
Salmonellosis | Salmonella spp. | Reptiles, birds | Ingestion of contaminated food |
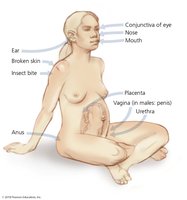
Portals of Entry
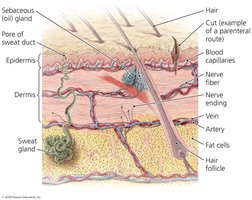
Pathogens enter the body through specific portals, including skin, mucous membranes, and placenta. The parenteral route circumvents these portals, typically via injection.
Skin: Acts as a barrier; pathogens may enter through cuts or by burrowing.
Mucous membranes: Line body cavities; respiratory tract is the most common site.
Placenta: Usually a barrier, but some pathogens can cross and infect the fetus.
Parenteral route: Pathogens deposited directly into tissues beneath skin or mucous membranes.
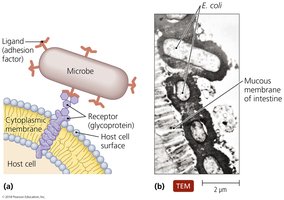
The Role of Adhesion in Infection
Adhesion is the process by which microorganisms attach to host cells, a critical step for establishing colonies. Adhesion factors include specialized structures and attachment molecules.
Attachment proteins: Found on viruses and bacteria; bind host cell receptors.
Host cell specificity: Determined by ligand-receptor interactions.
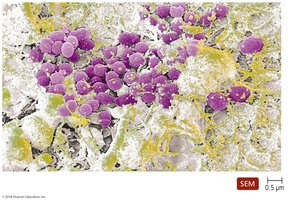
Biofilms: Some bacteria attach to each other, forming biofilms (e.g., dental plaque).
The Nature of Infectious Disease
Infection is the invasion of the host by a pathogen. Disease results if the pathogen alters normal body functions, referred to as morbidity.
Symptoms, Signs, and Syndromes
Symptoms: Subjective characteristics felt only by the patient.
Signs: Objective manifestations observed or measured by others.
Syndrome: Combination of symptoms and signs characterizing a disease.
Asymptomatic (subclinical) infections: Lack symptoms but may have signs.
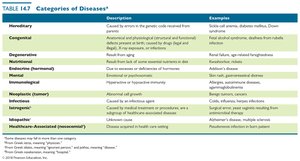
The Cause of Disease: Etiology
Etiology is the study of the cause of disease. Diseases have various causes, including infectious agents, genetic factors, and environmental influences.
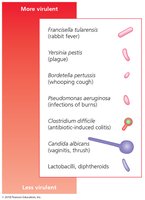
Virulence Factors of Infectious Agents
Pathogenicity is the ability of a microorganism to cause disease, while virulence is the degree of pathogenicity. Virulence factors include adhesion, biofilms, extracellular enzymes, toxins, and antiphagocytic factors.
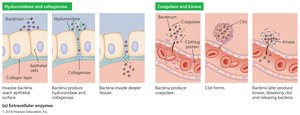
Extracellular Enzymes
Pathogens secrete enzymes that dissolve structural chemicals in the body, aiding infection, invasion, and evasion of defenses. Mutant species lacking these enzymes are often avirulent.
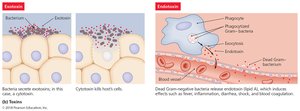
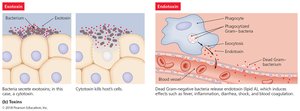
Toxins
Toxins are chemicals that harm tissues or trigger damaging immune responses. Toxemia refers to toxins in the bloodstream.
Exotoxins: Secreted proteins, typically from Gram-positive bacteria.
Endotoxins: Structural components (LPS) of Gram-negative bacteria.
Characteristic | Exotoxins | Endotoxins |
|---|---|---|
Source | Mainly Gram-positive and Gram-negative bacteria | Gram-negative bacteria |
Chemical Nature | Protein or short peptide | Lipid A of LPS |
Toxicity | High | Low |
Effect on Host | Varies (cytotoxic, neurotoxic, enterotoxic) | Fever, shock, blood coagulation |

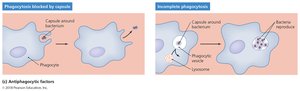
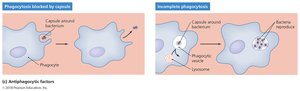
Antiphagocytic Factors
These factors prevent phagocytosis by host cells, allowing pathogens to persist longer. Capsules and antiphagocytic chemicals are common mechanisms.
Bacterial capsule: Composed of chemicals not recognized as foreign; slippery and hard to engulf.
Antiphagocytic chemicals: Prevent fusion of lysosome and phagocytic vesicles; leukocidins destroy phagocytic cells.
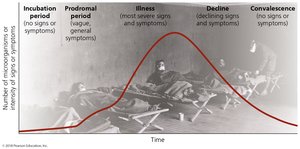
The Stages of Infectious Disease
Infectious diseases typically progress through five stages:
Incubation period: No signs or symptoms.
Prodromal period: Vague symptoms.
Illness: Most severe signs and symptoms.
Decline: Declining signs and symptoms.
Convalescence: No signs or symptoms.
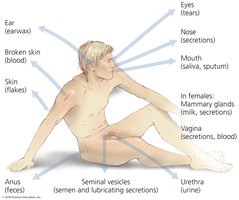
Portals of Exit
Pathogens leave the host through portals of exit, often the same as portals of entry. They are commonly found in materials the body secretes or excretes.
Modes of Disease Transmission
Contact Transmission
Direct contact: Body contact between hosts.
Indirect contact: Spread via fomites (inanimate objects).
Droplet transmission: Spread in droplets of mucus by exhaling, coughing, or sneezing.

Vehicle Transmission
Airborne: Pathogens travel more than 1 m via aerosols.
Waterborne: Spread of gastrointestinal diseases via contaminated water.
Foodborne: Pathogens in or on foods; contamination often from feces.
Bodily fluid: Blood, urine, saliva can carry pathogens.

Vector Transmission
Biological vectors: Biting arthropods transmit pathogens and serve as hosts.
Mechanical vectors: Passively transmit pathogens present on their body.

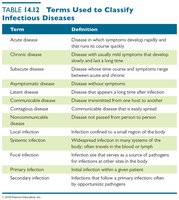
Classification of Infectious Diseases
Diseases can be classified by taxonomic categories, affected body system, longevity and severity, mode of transmission, and population effects.
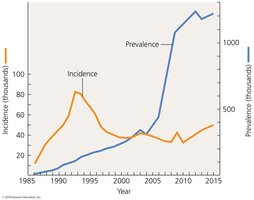
Epidemiology: Frequency of Disease
Disease occurrence is tracked using incidence (new cases) and prevalence (total cases) in a given area and period. Occurrence is also evaluated by frequency and geographic distribution.
Incidence:
Prevalence:
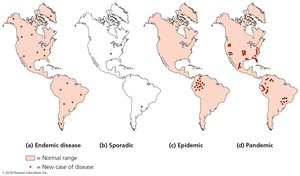
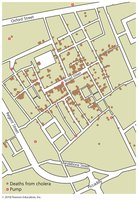
Descriptive Epidemiology
Descriptive epidemiology involves careful tabulation of data concerning a disease, including location, time, and patient information. The goal is to identify the index case (first case) of the disease.
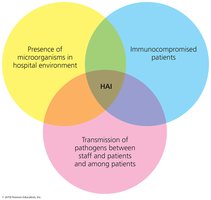
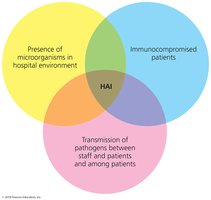
Healthcare-Associated (Nosocomial) Infections (HAI)
HAIs are infections acquired in healthcare settings. They can be exogenous (from the environment), endogenous (from normal microbiota), iatrogenic (from medical procedures), or superinfections (from antimicrobial drug use).
Control: Aggressive measures, especially hand-washing, are essential to reduce HAIs.
Additional info:
Tables and diagrams have been recreated and summarized for clarity and completeness.
Key terms and concepts have been expanded for academic context.
