 Back
BackChapter 15
Study Guide - Smart Notes

Innate Immune System
Overview and General Purpose
The innate immune system is the body's first line of defense against invading pathogens. It provides immediate, non-specific responses to a wide variety of threats, including bacteria, viruses, fungi, and parasites. Unlike the adaptive immune system, the innate system does not require prior exposure to a pathogen and does not generate immunological memory.
Purpose: Prevent entry and rapidly eliminate pathogens.
Components: Physical, chemical, and biological barriers; cellular and soluble factors.
Organization: Involves barriers, recognition, alarm, inflammation, cell recruitment, and effector functions.
Comparison: Innate vs. Adaptive Immune Systems
Innate Immunity: Immediate, non-specific, no memory, uses pattern recognition (e.g., airport security).
Adaptive Immunity: Delayed, highly specific, generates memory, tailored responses (e.g., FBI investigation).
Pathogen Detection and Recognition
The innate immune system detects pathogens by recognizing Pathogen-Associated Molecular Patterns (PAMPs) using Pattern Recognition Receptors (PRRs). These receptors are found on immune cells and in soluble form in the blood.
PAMPs: Conserved molecular structures unique to microbes (e.g., bacterial cell wall components, viral RNA).
PRRs: Include Toll-like receptors (TLRs), NOD-like receptors (NLRs), and soluble factors like complement proteins.
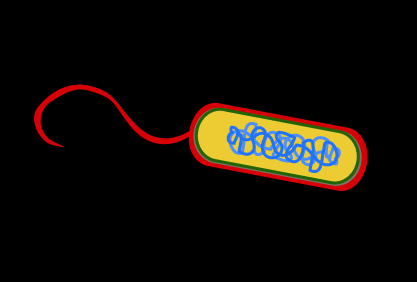
Barriers to Entry: The First Line of Defense
Physical, Chemical, and Biological Barriers
The body employs several barriers to prevent pathogen entry:
Physical: Skin, mucous membranes, cilia, tears.
Chemical: Acidic pH, enzymes (lysozyme, pepsin), bile, antimicrobial peptides (defensins).
Biological: Normal flora (commensal microbes) outcompete pathogens.
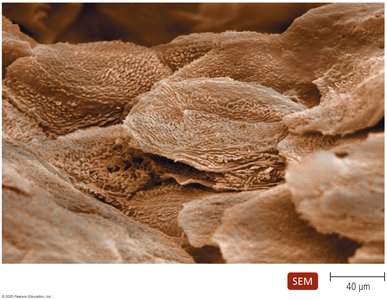
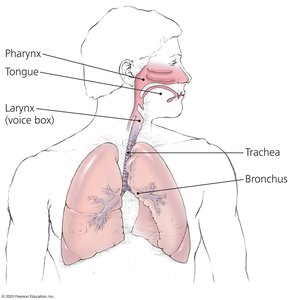
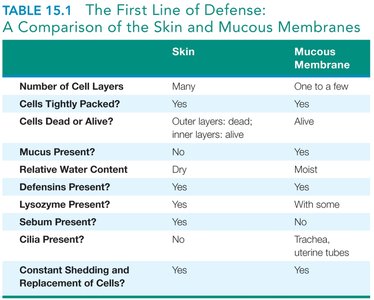
Comparison of Skin and Mucous Membranes
Skin | Mucous Membrane | |
|---|---|---|
Number of Cell Layers | Many | One to a few |
Cells Tightly Packed? | Yes | Yes |
Cells Dead or Alive? | Outer layers: dead; inner layers: alive | Alive |
Mucus Present? | No | Yes |
Relative Water Content | Dry | Moist |
Lysozyme Present? | Yes | With some |
Defensins Present? | Yes | Yes |
Sebum Present? | Yes | No |
Cilia Present? | No | Trachea, uterine tubes |
Constant Shedding and Replacement of Cells? | Yes | Yes |
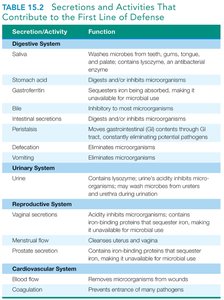
Secretions and Activities Contributing to Defense
Secretion/Activity | Function |
|---|---|
Saliva | Washes microbes from teeth, gums, tongue, and palate; contains lysozyme |
Stomach acid | Digests and/or inhibits microorganisms |
Bile | Inhibitory to most microorganisms |
Defecation, Vomiting, Urine | Eliminates microorganisms |
Vaginal secretions | Acidity inhibits microorganisms |
Menstrual flow | Cleanses uterus and vagina |
Blood flow, Coagulation | Removes or prevents entry of pathogens |
Pattern Recognition and Immune Activation
Pattern Recognition Receptors (PRRs) and PAMPs
PRRs are crucial for the detection of pathogens. They recognize PAMPs, which are conserved microbial molecules not found in host cells.
Cellular PRRs: Located on the surface or inside immune cells (e.g., TLRs, NLRs).
Soluble PRRs: Circulate in blood (e.g., complement proteins).
Toll-Like Receptors (TLRs)
TLRs are a family of PRRs that recognize specific PAMPs. They are found on the cell surface or within endosomal compartments of immune cells.
TLR | PAMP (Microbial Molecule) |
|---|---|
TLR1 | Bacterial lipopeptides and certain proteins in multicellular parasites |
TLR2 | Peptidoglycan, lipoteichoic acid (Gram-positive cell wall), yeast cell wall |
TLR4 | Lipid A in LPS (Gram-negative bacteria) |
TLR5 | Flagellin (bacterial flagella) |
TLR3 | Double-stranded RNA (viruses) |
TLR7, TLR8 | Single-stranded viral RNA |
TLR9 | Unmethylated CpG DNA (bacterial/viral DNA) |
The Complement System
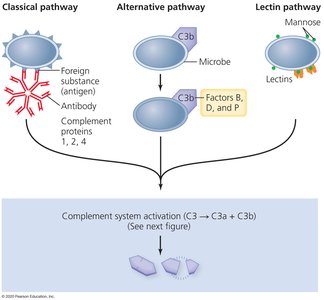
Activation Pathways
The complement system is a cascade of plasma proteins that enhances the ability of antibodies and phagocytic cells to clear microbes. It can be activated by three pathways:
Classical Pathway: Triggered by antibodies bound to antigens.
Alternative Pathway: Triggered directly by microbial surfaces.
Lectin Pathway: Triggered by lectin binding to microbial carbohydrates.
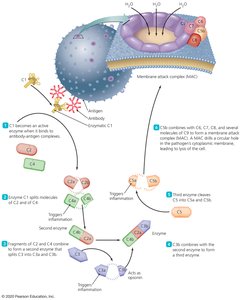
Functions of Complement
Opsonization: Tags pathogens for phagocytosis.
Chemotaxis: Recruits immune cells to infection sites.
Direct Killing: Forms the Membrane Attack Complex (MAC) to lyse pathogens.
Inflammation and Cellular Recruitment
Inflammatory Response
Inflammation is a hallmark of innate immunity, characterized by heat (calor), pain (dolor), redness (rubor), and swelling (tumor). It is triggered by cytokines and chemokines released from immune cells.
Vasodilation: Increases blood flow to the area.
Increased Permeability: Allows immune cells and proteins to enter tissues.
Extravasation: Movement of white blood cells from blood to tissues.
Recruitment of Innate Immune Cells
Key innate immune cells include neutrophils, macrophages, dendritic cells, natural killer (NK) cells, eosinophils, and basophils. Chemotactic signals and adhesion molecules guide these cells to infection sites.
Neutrophils: First responders, phagocytose bacteria, form pus.
Macrophages: Engulf pathogens, present antigens, secrete cytokines.
Dendritic Cells: Bridge innate and adaptive immunity by presenting antigens to T cells.
NK Cells: Kill virus-infected and cancerous cells.

Effector Functions of Innate Immunity
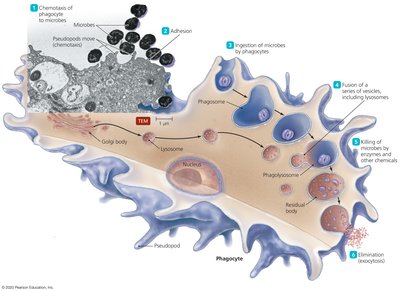
Phagocytosis and Microbial Killing
Phagocytic cells (macrophages, neutrophils, dendritic cells) ingest and destroy pathogens. They may use lysosomal enzymes or generate reactive oxygen and nitrogen species (respiratory burst) for microbial killing.
Reactive Oxygen Species: Superoxide (O2-), hydrogen peroxide (H2O2), bleach (OCl-).
Antimicrobial Peptides: Defensins disrupt microbial membranes.
Natural Killer (NK) Cells
NK cells recognize and kill infected or abnormal host cells using a balance of activating and inhibitory receptors. They are important for early defense against viruses and tumors.
The Lymphatic System and Hematopoiesis
Lymphatic System Structure and Function
The lymphatic system drains excess fluid from tissues, transports immune cells, and provides sites for immune cell interactions. It includes primary lymphoid organs (bone marrow, thymus) and secondary lymphoid organs (lymph nodes, spleen, MALT).
Lymph: Fluid containing immune cells and proteins.
Lymph Nodes: Sites for immune cell activation and proliferation.
Hematopoiesis and Leukocyte Lineages
All blood cells originate from pluripotent stem cells in the bone marrow. Major leukocyte lineages include:
Granulocytes: Neutrophils, eosinophils, basophils/mast cells.
Monocytes/Macrophages: Circulate in blood, mature in tissues.
Dendritic Cells: Antigen-presenting cells, initiate adaptive immunity.
Lymphocytes: B cells (antibody production), T cells (helper and cytotoxic), NK cells.
Summary Table: Key Innate Immune Components
Component | Function |
|---|---|
Physical Barriers | Prevent pathogen entry (skin, mucosa) |
Chemical Barriers | Destroy/inhibit microbes (acid, enzymes) |
Phagocytes | Ingest and destroy pathogens |
NK Cells | Kill infected/cancerous cells |
Complement | Opsonization, chemotaxis, direct killing |
Cytokines/Chemokines | Coordinate and recruit immune responses |
Example: When bacteria breach the skin, PRRs on resident macrophages recognize PAMPs, triggering cytokine release, inflammation, and recruitment of neutrophils to eliminate the invaders.
