 Back
BackInnate Immune System: Structure, Function, and Response
Study Guide - Smart Notes

Innate Immune System
General Purpose, Components, and Organization
The innate immune system is the body's first line of defense against pathogens, providing immediate, non-specific responses. It consists of physical, chemical, and biological barriers, as well as cellular and soluble components that recognize and respond to common pathogen-associated molecular patterns (PAMPs).
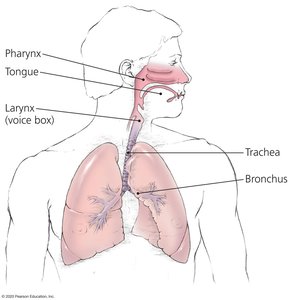
Physical Barriers: Skin, mucous membranes, cilia, tears
Chemical Barriers: Acid, enzymes (pepsin, lysozyme), bile, defensins
Biological Barriers: Normal flora
Cellular Components: Phagocytes (macrophages, neutrophils), dendritic cells, innate lymphocytes
Soluble Components: Complement proteins, cytokines, chemokines
Comparison of Innate and Adaptive Immune Systems
The immune system is divided into two overlapping compartments: innate and adaptive immunity. The innate system responds immediately and non-specifically, while the adaptive system is highly specific, slower to respond, and generates immunological memory.
Innate Immunity: Immediate, non-specific, no memory, recognizes general patterns
Adaptive Immunity: Delayed (3-5 days), highly specific, generates memory, recognizes specific antigens

Detection and Recognition of Pathogens
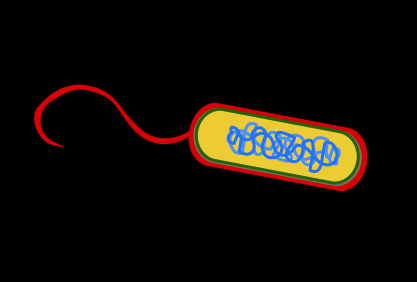
Pathogens are detected by the immune system through pattern recognition. Cells and soluble factors recognize PAMPs using pattern recognition receptors (PRRs), including Toll-like receptors (TLRs) and NOD-like receptors (NLRs).
PAMPs: Molecules expressed by pathogens but not by host cells (e.g., lipopolysaccharide, flagellin, viral RNA)
PRRs: Cellular and soluble receptors that bind PAMPs and activate immune responses
Pattern Recognition Receptors (PRRs) and Toll-Like Receptors (TLRs)
PRRs are found on the surface and inside immune cells. TLRs are a major family of PRRs, each recognizing specific microbial molecules. Some TLRs are located on the cell surface, others in intracellular compartments.
Cell Surface TLRs: Detect extracellular pathogens
Intracellular TLRs: Detect intracellular pathogens (e.g., viruses)
NOD-Like Receptors: Detect intracellular bacterial components
TLR | PAMP (Microbial Molecule) |
|---|---|
TLR1 | Bacterial lipopeptides and certain proteins in multicellular parasites |
TLR2 | Peptidoglycan, lipoteichoic acid (Gram-positive cell wall), cell wall of yeast |
TLR4 | Lipid A in LPS (Gram-negative bacteria) |
TLR5 | Flagellin (bacterial flagella) |
TLR6 | Bacterial lipopeptides, lipoteichoic acid, cell wall of yeast |
TLR10 | Unknown component of influenzaviruses |
TLR3 | Double-stranded RNA (viruses) |
TLR7 | Single-stranded viral RNA |
TLR8 | Single-stranded viral RNA |
TLR9 | Unmethylated cytosine-guanine pairs of viral and bacterial DNA |

Complement System
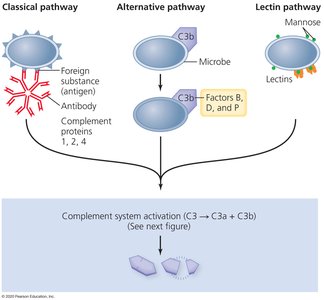
The complement system is a cascade of plasma proteins that can be activated by three pathways: classical (antibody-bound), alternative (direct microbe binding), and lectin (lectin binding to microbial carbohydrates). Activation leads to the formation of the membrane attack complex (MAC), which lyses pathogens, and to opsonization and recruitment of immune cells.
Classical Pathway: Activated by antibody-antigen complexes
Alternative Pathway: Activated directly by microbial surfaces
Lectin Pathway: Activated by lectin binding to microbial carbohydrates
MAC: Forms pores in pathogen membranes, leading to cell lysis
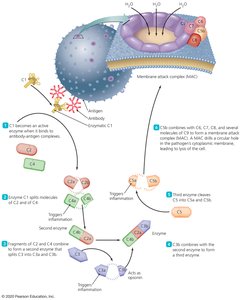
Innate Immune Response: Sequence of Events
Innate immune responses follow a characteristic sequence: recognition, alarm, inflammation, cell recruitment, and effector functions.
Recognition: Detection of pathogens by PRRs
Alarm: Release of cytokines and chemokines to activate and localize immune cells
Inflammation: Vasodilation, increased permeability, extravasation of white blood cells, stimulation of pain receptors
Cell Recruitment: Phagocytes, neutrophils, natural killer cells, eosinophils, basophils, monocytes/macrophages
Effector Functions: Phagocytosis, cytotoxicity, production of reactive oxygen species, antimicrobial peptides, destructive enzymes



Phagocytic Cells and Their Functions
Phagocytic cells, including macrophages, neutrophils, and dendritic cells, ingest and destroy pathogens. They may use lysosomes or activate a respiratory burst to generate reactive oxygen and nitrogen species.
Macrophages: Patrol tissues, ingest pathogens, key in both innate and adaptive immunity
Neutrophils: Phagocytize bacteria and debris, form pus, use NETs
Dendritic Cells: Professional antigen-presenting cells, bridge innate and adaptive immunity
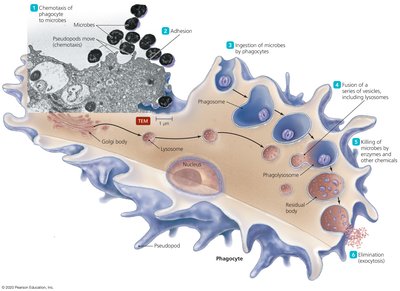
Lymphatic System and Hematopoiesis
The lymphatic system drains excess fluid and proteins from tissues and transports them to the blood. It includes primary and secondary lymphoid tissues, where lymphocytes mature and interact with pathogens. Hematopoiesis is the development of blood cells from pluripotent stem cells in the bone marrow.
Primary Lymphoid Tissue: Thymus, bone marrow
Secondary Lymphoid Tissue: Lymph nodes, MALT, spleen, tonsils, adenoids
Lymph Node: Site for immune cell interaction and activation
Hematopoiesis: Formation of all blood cells, including leukocytes
Leukocyte Lineages
Leukocytes (white blood cells) are divided into granulocytes, monocytes/macrophages, dendritic cells, and lymphocytes, each with distinct roles in immunity.
Granulocytes: Neutrophils, basophils/mast cells, eosinophils
Monocytes/Macrophages: Circulate in blood, mature in tissues, phagocytosis
Dendritic Cells: Antigen presentation, initiate adaptive response
Lymphocytes: B cells (antibody production), T cells (helper and cytotoxic), natural killer cells (innate cytotoxicity)
Summary Table: Skin vs. Mucous Membranes
The skin and mucous membranes serve as the first line of defense, each with unique structural and functional properties.
Skin | Mucous Membrane | |
|---|---|---|
Number of Cell Layers | Many | One to a few |
Cells Tightly Packed? | Yes | Yes |
Cells Dead or Alive? | Outer layers: dead; inner layers: alive | Alive |
Mucus Present? | No | Yes |
Relative Water Content | Dry | Moist |
Lysozyme Present? | Yes | With some |
Defensins Present? | Yes | Yes |
Sebum Present? | Yes | No |
Cilia Present? | No | Trachea, uterine tubes |
Constant Shedding and Replacement of Cells? | Yes | Yes |
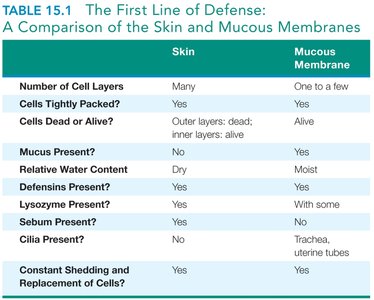
Summary Table: Secretions and Activities Contributing to First Line of Defense
Secretion/Activity | Function |
|---|---|
Saliva | Washes microbes from teeth, gums, tongue; contains lysozyme |
Stomach acid | Digests and/or inhibits microorganisms |
Bile | Inhibits microorganisms |
Intestinal secretions | Digests and/or inhibits microorganisms |
Defecation | Eliminates microorganisms |
Urine | Contains lysozyme; acidity inhibits microorganisms |
Vaginal secretions | Acidity inhibits microorganisms |
Menstrual flow | Cleanses uterus and vagina |
Blood flow | Removes microorganisms from wounds |
Coagulation | Prevents entrance of many pathogens |
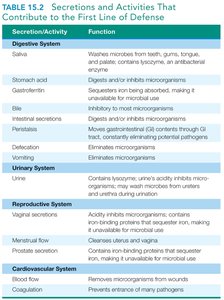
Practice and Application
Understanding the innate immune system is essential for recognizing how the body responds to infection and for diagnosing immune-related diseases. The presence and activity of specific immune cell types in tissues can indicate immune system activity and disease states.
Example: Increased neutrophil recruitment is a hallmark of acute bacterial infection, while eosinophil accumulation is associated with parasitic infections and allergies.
Additional info: The innate immune system is evolutionarily conserved and forms the basis for many therapeutic interventions, including vaccines and immunomodulatory drugs.
