 Back
BackInnate Immunity, Inflammation, and Immune System Disorders
Study Guide - Smart Notes

Leukocytes and Their Roles in Immunity
Granulocytes and Agranulocytes
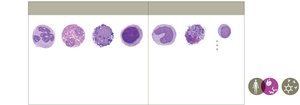
Leukocytes, or white blood cells, are essential components of the immune system, classified into granulocytes and agranulocytes based on the presence of cytoplasmic granules. Each type plays a distinct role in immune defense.
Granulocytes:
Neutrophils: Highly phagocytic; primary responders to bacterial and viral infections.
Eosinophils: Moderately phagocytic; attack allergens and parasites.
Basophils: Involved in allergic responses and defense against parasites; granules contain histamine.
Mast cells: Reside in tissues; attack bacteria, allergens, and parasites; moderately phagocytic.
Agranulocytes:
Monocytes: Mature into macrophages; highly phagocytic; activate adaptive immune responses.
Dendritic cells: Highly phagocytic; serve as antigen-presenting cells to activate adaptive immunity.
Lymphocytes: Include NK cells (innate immunity), B cells, and T cells (adaptive immunity).
Inflammation: Phases and Mechanisms
Overview and Importance
Inflammation is a critical innate immune response that develops when tissues are damaged by trauma or infection. It is essential for healing but can cause tissue damage if unregulated.
Functions of Inflammation:
Recruit immune defenses to the site of injury
Limit the spread of infectious agents
Deliver oxygen, nutrients, and chemical factors for tissue recovery
Phases of Inflammation
Inflammation occurs in three general phases: vascular changes, leukocyte recruitment, and resolution.
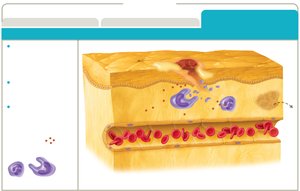
Vascular Changes: Blood vessels dilate and become more permeable due to chemical signals (e.g., kinins, eicosanoids, histamines) released by damaged cells and leukocytes. This allows plasma proteins and immune cells to enter the tissue.
Leukocyte Recruitment: Cytokines recruit neutrophils and monocytes to the site. These cells exit the bloodstream (margination and diapedesis) and perform phagocytosis.
Resolution: Inflammatory signals decrease, tissue repair is initiated, and excess leukocytes undergo apoptosis, forming pus.
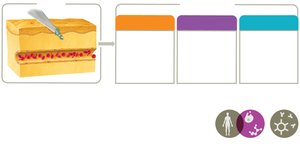
Vascular Changes in Detail
Vasoactive molecules such as kinins, eicosanoids, and histamines increase blood flow and vessel permeability. Exudate, containing plasma proteins like complement, seeps into tissues, causing swelling.
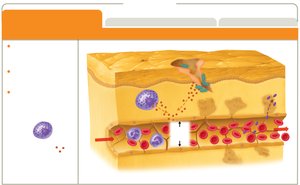
Leukocyte Recruitment in Detail
Cytokines and other chemoattractants guide neutrophils and monocytes to the inflamed tissue. Leukocytes slow down (margination), adhere to the vessel wall, and squeeze through (diapedesis) to reach the site of injury. Monocytes mature into macrophages, and both cell types phagocytize invaders and release more cytokines.
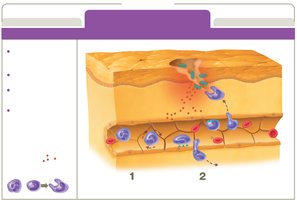
Resolution Phase in Detail
As the threat subsides, capillaries return to normal, and chemical signals promote healing. Unneeded leukocytes die by apoptosis, contributing to pus. Swelling decreases as exudate is drained by lymphatic vessels.
Fever as a Systemic Innate Immune Response
Role and Benefits of Fever
Fever is a systemic response that enhances the effectiveness of interferons, increases phagocyte efficiency, boosts leukocyte production, limits pathogen growth, and promotes tissue repair.
Mechanisms: Hormonal changes, shivering, and increased metabolism raise body temperature, while blood vessels constrict to reduce heat loss.
Immune System Disorders
Primary and Secondary Immunodeficiencies
Immunodeficiencies are conditions where the immune system's ability to fight infections is compromised.
Primary (Congenital) Immunodeficiencies: Genetic defects affecting immune factors, e.g., SCID, DiGeorge syndrome, selective IgA deficiency.
Secondary (Acquired) Immunodeficiencies: Result from aging, infections (e.g., HIV), medical interventions, or systemic disorders (e.g., diabetes, malnutrition).
Treatments: Bone marrow transplants, antibody administration, cytokine therapies, and experimental treatments.
Autoimmunity and Autoimmune Disorders
Autoimmunity occurs when the immune system attacks self-tissues, leading to diseases such as lupus, rheumatoid arthritis, type I diabetes, and multiple sclerosis. Symptoms vary depending on the affected tissues and may include joint pain, fatigue, rash, and organ dysfunction.
Hypersensitivity Reactions
Hypersensitivities are inappropriate immune responses classified into four types (Gell and Coombs classification):
Type I (Allergy): IgE-mediated; rapid response to allergens; can cause anaphylaxis.
Type II (Cytotoxic): IgG or IgM-mediated; targets cells for lysis (e.g., transfusion reactions, hemolytic disease of the newborn).
Type III (Immune Complex): Antigen-antibody complexes deposit in tissues, causing inflammation (e.g., lupus, serum sickness).
Type IV (Delayed): T cell-mediated; delayed response (e.g., tuberculin skin test, transplant rejection, contact dermatitis).
Mnemonic: ACID (Allergy, Cytotoxic, Immune complex, Delayed)
Transplantation and Graft Rejection
Transplanted tissues may be rejected if recognized as foreign by T cells. Grafts are classified as:
Autografts: From self; no rejection.
Isografts: From identical twin; minimal rejection.
Allografts: From same species; risk of rejection depends on MHC similarity.
Xenografts: From different species; high risk of rejection.
Immune-privileged sites (e.g., eye, brain) are less likely to reject grafts. Graft-versus-host disease (GVHD) can occur in bone marrow transplants when donor immune cells attack the recipient.
Blood Typing and Transfusion Reactions
Blood typing is essential to prevent transfusion reactions. Incompatibility can lead to hemolysis and severe immune responses. Rh factor incompatibility during pregnancy can cause hemolytic disease of the newborn if maternal antibodies attack fetal red blood cells.
Visual Summary: Innate and Adaptive Immunity
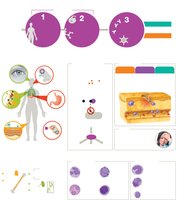
The immune system is organized into three lines of defense:
First-Line Defenses: Physical, chemical, and mechanical barriers (e.g., skin, mucous membranes, lysozyme, stomach acid).
Second-Line Defenses: Cellular and molecular defenses (e.g., phagocytes, inflammation, fever, complement proteins).
Third-Line Defenses: Adaptive immunity (B cells, T cells, antibodies).
Key Terms: Phagocytosis, cytokines, complement, antigen-presenting cells, apoptosis, hypersensitivity, autoimmunity, immunodeficiency, MHC, graft rejection, transfusion reaction, Rh factor
