 Back
BackInnate Immunity: Nonspecific Defenses of the Host – Study Notes
Study Guide - Smart Notes

Innate Immunity: Nonspecific Defenses of the Host
The Concept of Immunity
Immunity is the ability of an organism to resist infection or disease. The immune system is divided into two main branches: innate immunity and adaptive immunity. Innate immunity provides immediate, nonspecific defense against pathogens, while adaptive immunity is slower but highly specific and has memory.
Innate Immunity: Present at birth, rapid response, recognizes common pathogen features.
Adaptive Immunity: Develops after exposure, slower response, specific to particular pathogens, has memory.
Toll-like receptors (TLRs): Proteins on host cells that recognize pathogen-associated molecular patterns (PAMPs) and trigger immune responses.
Cytokines: Small proteins released by cells that regulate immune responses, including the recruitment and activation of other immune cells.
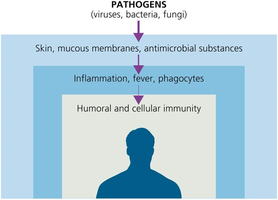
First Line of Defense: Skin and Mucous Membranes
The first line of defense consists of physical and chemical barriers that prevent pathogen entry.
Physical Factors
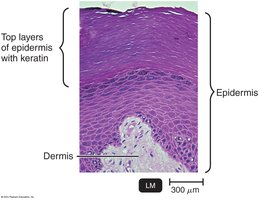
Skin: Composed of the dermis (connective tissue) and epidermis (tightly packed epithelial cells with keratin). Shedding and dryness inhibit microbial growth.
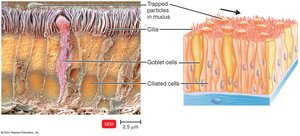
Mucous Membranes: Line the gastrointestinal, respiratory, and genitourinary tracts. Mucus traps microbes and prevents tract drying.
Lacrimal Apparatus: Produces tears that wash the eye.
Ciliary Escalator: Moves mucus and trapped microbes away from the lungs.
Other Mechanisms: Earwax, urine flow, vaginal secretions, peristalsis, defecation, vomiting, and diarrhea help expel microbes.
Chemical Factors
Sebum: Forms a protective film and lowers skin pH (3–5).
Lysozyme: Enzyme in perspiration, tears, saliva, and urine that destroys bacterial cell walls.
Gastric Juice: Low pH (1.2–3.0) destroys most bacteria and toxins.
Vaginal Secretions: Low pH (3–5) inhibits microbes.
Normal Microbiota and Innate Immunity
Microbial Antagonism: Normal microbiota compete with pathogens for space and nutrients, produce substances harmful to pathogens, and alter environmental conditions.
Commensalism: One organism benefits, the other is unharmed.
Opportunistic Pathogens: Normal microbiota that can cause disease under certain conditions (e.g., E. coli, S. aureus).
Probiotics: Live microbes administered for health benefits.
Prebiotics: Nutrients that promote the growth of beneficial microbes.

Second Line of Defense: Cellular and Molecular Components
If pathogens bypass the first line, the second line of defense includes various cells and proteins that attack invaders.
Formed Elements in Blood
Erythrocytes: Red blood cells, transport oxygen.
Leukocytes: White blood cells, key players in immunity.
Platelets: Involved in blood clotting.
All formed in red bone marrow via hematopoiesis.
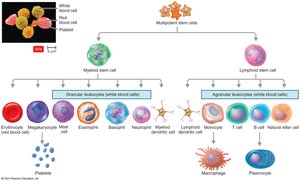
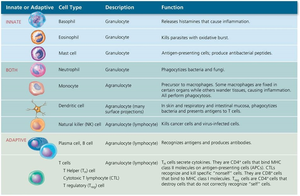
Leukocyte Classification
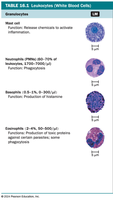
Granulocytes: Visible granules in cytoplasm.
Neutrophils: Highly phagocytic, first responders to infection.
Basophils: Release histamine, involved in allergic responses.
Eosinophils: Attack parasites and helminths, some phagocytosis.
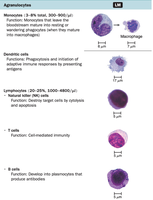
Agranulocytes: No visible granules.
Monocytes: Mature into macrophages, phagocytic.
Dendritic Cells: Phagocytic, present antigens to T cells.
Lymphocytes: T cells, B cells, and NK cells; involved in adaptive immunity.
White Blood Cell Counts
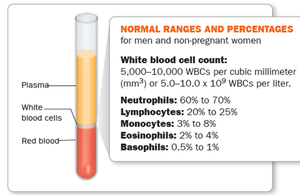
Normal WBC Count: 5,000–10,000 WBCs/mm³ (5.0–10.0 × 10⁹/L).
Differential WBC Count: Measures the relative numbers of each type of WBC.
High WBC: May indicate bacterial infection, autoimmune disease, or medication side effects.
Low WBC: May indicate viral infection, severe bacterial infection, or cancer.
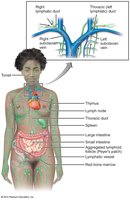
The Lymphoid System
The lymphoid system is a network of tissues and organs that help rid the body of toxins and pathogens. It includes lymph, lymphatic vessels, lymph nodes, spleen, thymus, tonsils, and Peyer's patches.
Lymph: Fluid that carries microbes to lymph nodes for immune surveillance.
Lymphoid Tissue: Contains lymphocytes and phagocytic cells.
Lymph Nodes: Sites where immune cells encounter and destroy pathogens.
Phagocytes and Phagocytosis
Phagocytes are cells that ingest and destroy microbes and debris. The process of phagocytosis involves several steps:
Chemotaxis: Phagocytes are attracted to infection sites by chemical signals.
Adherence: Phagocyte attaches to the microbe via PAMPs and TLRs; opsonization enhances this step.
Ingestion: Pseudopods engulf the microbe, forming a phagosome.
Phagolysosome Formation: Lysosome fuses with phagosome, forming a phagolysosome.
Digestion: Enzymes and toxic substances destroy the microbe.
Excretion: Indigestible material is expelled from the cell.
Inflammation
Inflammation is a local defensive response to tissue damage, characterized by redness, heat, swelling, pain, and loss of function. It serves to contain and eliminate injurious agents and repair tissue.
Stages of Inflammation:
Vasodilation and increased vascular permeability
Phagocyte migration and phagocytosis
Tissue repair
Chemicals Involved: Histamine, kinins, prostaglandins, leukotrienes, cytokines.
Chronic Inflammation: Can contribute to chronic diseases and systemic effects.
Fever
Fever is an abnormally high body temperature, often caused by infection. It is triggered by cytokines that reset the hypothalamic thermostat. Fever enhances immune function but can be dangerous if too high or prolonged.
Benefits: Inhibits pathogen growth, increases immune cell activity, speeds up tissue repair.
Risks: Tachycardia, dehydration, seizures, coma.
Antimicrobial Substances
The body produces several antimicrobial substances as part of innate immunity:
Complement System: Over 30 serum proteins that enhance immune responses via a cascade. Three activation pathways:
Classical Pathway: Triggered by antibodies bound to antigens.
Alternative Pathway: Triggered directly by microbial surfaces.
Lectin Pathway: Triggered by lectins binding to microbial carbohydrates.
Outcomes: Cytolysis (membrane attack complex), opsonization, inflammation.
Interferons (IFNs): Cytokines with antiviral activity; induce production of antiviral proteins in neighboring cells.
Iron-Binding Proteins: Sequester iron to limit microbial growth (e.g., transferrin, lactoferrin, ferritin, hemoglobin).
Antimicrobial Peptides (AMPs): Short peptides that disrupt microbial membranes and inhibit cell wall synthesis.
Summary Table: Major Leukocytes and Their Functions
Cell Type | Description | Function |
|---|---|---|
Neutrophil | Granulocyte | Phagocytizes bacteria and fungi |
Basophil | Granulocyte | Releases histamine (inflammation) |
Eosinophil | Granulocyte | Kills parasites with oxidative burst |
Monocyte/Macrophage | Agranulocyte | Phagocytosis; antigen presentation |
Dendritic Cell | Agranulocyte | Phagocytosis; antigen presentation |
Lymphocyte (T cell, B cell, NK cell) | Agranulocyte | Adaptive immunity (T/B); cytolysis (NK) |
Key Equations and Concepts
Complement Activation (Classical Pathway):
Opsonization: Coating of microbes with proteins (e.g., C3b) to enhance phagocytosis.
Phagocytosis Steps: Chemotaxis → Adherence → Ingestion → Digestion → Excretion
Additional info: These notes integrate foundational concepts from Chapter 16 of a standard microbiology textbook, focusing on innate immunity and its cellular and molecular mechanisms.
