 Back
BackInnate Immunity: Nonspecific Defenses of the Host
Study Guide - Smart Notes

Chapter 16: Innate Immunity – Nonspecific Defenses of the Host
Introduction to Immunity
Immunity refers to the ability of an organism to resist infection or disease. The immune system is divided into innate (nonspecific) and adaptive (specific) defenses. Innate immunity provides immediate, general protection against pathogens, while adaptive immunity targets specific invaders and develops memory for future responses.
Immunity: Ability to ward off disease.
Susceptibility: Lack of resistance to a disease.
Innate Immunity: Defenses present at birth, rapid, and nonspecific.
Adaptive Immunity: Specific, slower to respond, and has memory.
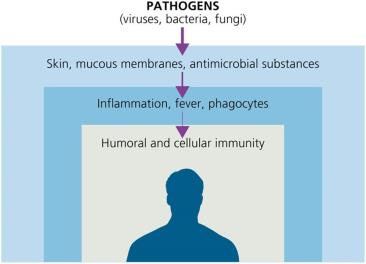
Physical and Chemical Barriers
Physical Barriers
Physical barriers are the body's first line of defense, preventing pathogen entry.
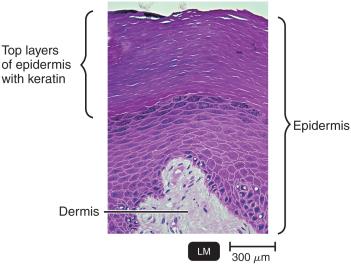
Skin: Composed of the dermis (connective tissue) and epidermis (tightly packed epithelial cells with keratin). Shedding and dryness inhibit microbial growth.
Mucous Membranes: Line the gastrointestinal, respiratory, and genitourinary tracts. Mucus traps microbes and prevents drying.
Lacrimal Apparatus: Drains tears, washing the eye.
Ciliary Escalator: Moves mucus and trapped microbes away from the lungs.
Other Mechanisms: Epiglottis, earwax, urine flow, vaginal secretions, peristalsis, defecation, vomiting, and diarrhea help expel pathogens.
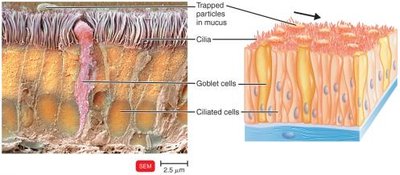
Chemical Barriers
Chemical factors enhance the effectiveness of physical barriers by creating hostile environments for pathogens.
Sebum: Forms a protective film and lowers skin pH (3–5).
Lysozyme: Enzyme in perspiration, tears, saliva, and urine that destroys bacterial cell walls.
Gastric Juice: Low pH (1.2–3.0) destroys most bacteria and toxins.
Vaginal Secretions: Low pH (3–5) inhibits microbes.
Normal Microbiota and Innate Immunity
Normal microbiota protect the host by competing with pathogens for nutrients and space, producing substances harmful to pathogens, and altering environmental conditions. They also play a role in immune system development.
Commensalism: One organism benefits, the other is unharmed.
Opportunistic Pathogens: Normal microbiota that can cause disease under certain conditions (e.g., E. coli, S. aureus).
Probiotics: Live cultures administered for beneficial effects.
Prebiotics: Nutrients that promote growth of beneficial bacteria.
Cells and Formed Elements in Blood
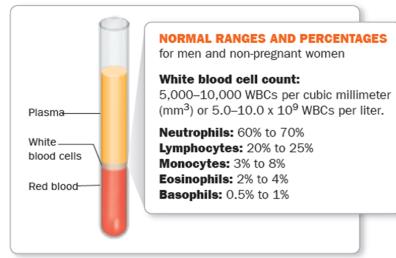
Blood contains cells and cell fragments suspended in plasma. These include erythrocytes (red blood cells), leukocytes (white blood cells), and platelets. All are produced in red bone marrow via hematopoiesis.
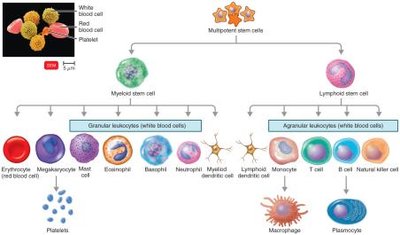
Leukocytes (White Blood Cells)
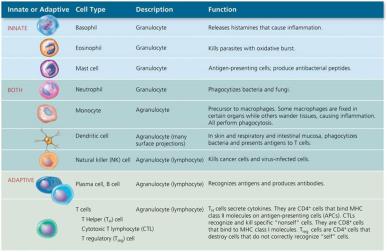
Leukocytes are divided into granulocytes and agranulocytes, each with specialized functions in immunity.
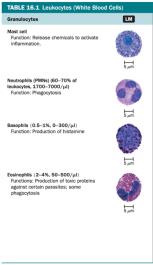
Granulocytes:
Neutrophils: Highly phagocytic, first responders to infection.
Basophils: Release histamine, involved in allergic responses.
Eosinophils: Phagocytic, toxic to parasites and helminths.
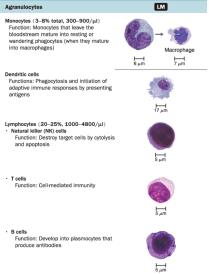
Agranulocytes:
Monocytes: Mature into macrophages in tissues, phagocytic.
Dendritic Cells: Phagocytic, initiate adaptive immune responses.
Lymphocytes: T cells, B cells, and NK cells; key in adaptive immunity.
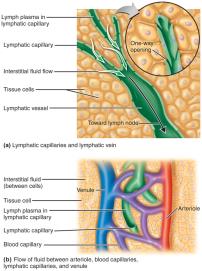
The Lymphoid System
The lymphoid system includes lymph plasma, lymphatic vessels, lymphoid tissues and organs, and red bone marrow. Lymphoid tissue contains lymphocytes and phagocytic cells. Lymph transports microbes to lymph nodes, where immune cells encounter and destroy pathogens.
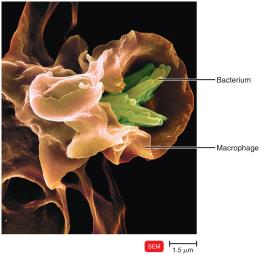
Phagocytosis
Phagocytosis is the process by which certain cells ingest and destroy microorganisms and debris. Professional phagocytes include neutrophils, eosinophils, and macrophages (derived from monocytes). Macrophages can be fixed (residing in tissues) or free (wandering in tissues).
Neutrophils: Predominate early in infection.
Macrophages: Dominate later, cleaning up debris.
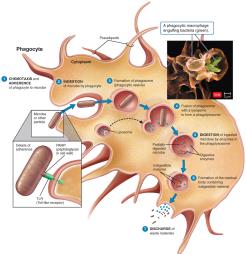
Mechanism of Phagocytosis
The process of phagocytosis involves several steps:
Chemotaxis: Chemical signals attract phagocytes to microbes.
Adherence: Phagocyte attaches to microbe via PAMPs and TLRs; opsonization enhances attachment.
Ingestion: Pseudopods engulf the microbe, forming a phagosome.
Digestion: Lysosomes fuse with the phagosome, forming a phagolysosome; enzymes and toxic products digest the microbe.
Exocytosis: Indigestible material is expelled.
Inflammation
Inflammation is a local defensive response to tissue damage caused by infection, physical, or chemical agents. Its main signs are pain, redness, immobility, swelling, and heat (PRISH). Inflammation destroys or contains injurious agents and initiates tissue repair.
Acute Inflammation: Rapid onset, short duration.
Chronic Inflammation: Slow onset, long duration, may be severe.
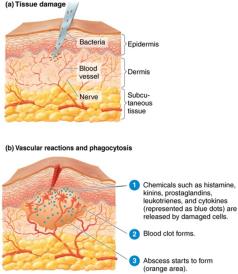
Stages of Inflammation
Vasodilation and Increased Permeability: Blood vessels dilate, increasing blood flow and allowing immune cells to reach the site. Chemicals like histamine, kinins, prostaglandins, and leukotrienes are released.
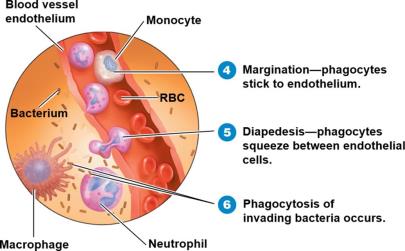
Phagocyte Migration and Phagocytosis: Phagocytes migrate to the site, adhere to endothelium (margination), squeeze through vessel walls (diapedesis), and ingest microbes.
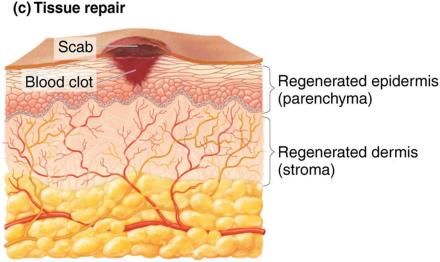
Tissue Repair: Damaged tissue is replaced once harmful substances are removed.
Vasoactive Mediators of Inflammation
Vasoactive Mediator | Source | Effect |
|---|---|---|
Histamine | Mast cells, basophils, platelets | Vasodilation, increased permeability |
Kinins | Blood plasma | Vasodilation, permeability, chemotaxis |
Prostaglandins | Damaged cells | Intensify histamine/kinin effects, help phagocytes move |
Leukotrienes | Mast cells, basophils | Increase permeability, help phagocyte attachment |
Complement | Blood plasma | Stimulates histamine release, attracts phagocytes, promotes phagocytosis |
Cytokines | Macrophages | Vasodilation, increased permeability |
Fever
Fever is an abnormally high body temperature, usually caused by infection. Cytokines reset the hypothalamus to a higher temperature, enhancing immune responses but potentially causing complications if too high.
Benefits: Enhances phagocyte and T cell activity, increases antimicrobial substance production, slows pathogen growth, speeds tissue repair.
Complications: Tachycardia, acidosis, dehydration, seizures, coma, death at very high temperatures.
The Complement System
The complement system consists of over 30 serum proteins that enhance immune responses. It can be activated by three pathways: classical, alternative, and lectin. The main outcomes are cytolysis, opsonization, and inflammation.
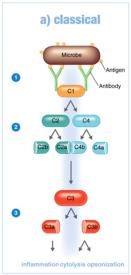
Classical Pathway: Triggered by antibodies binding to antigens.
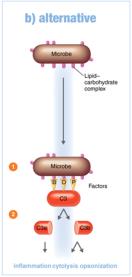
Alternative Pathway: Triggered by complement proteins binding directly to microbial surfaces.
Lectin Pathway: Triggered by mannose-binding lectin binding to microbial carbohydrates.
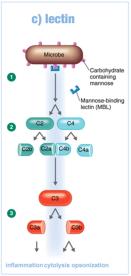
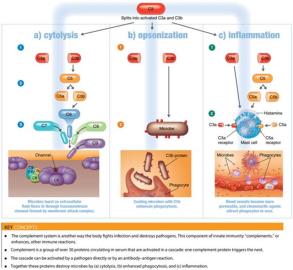
Outcomes of Complement Activation
Cytolysis: Formation of the membrane attack complex (MAC) that lyses microbes.
Opsonization: Coating of microbes to enhance phagocytosis.
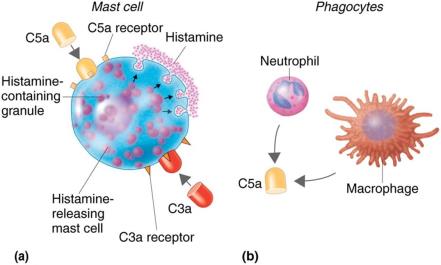
Inflammation: Complement proteins trigger mast cells to release histamine and other mediators.
Regulation and Evasion of Complement
Regulation: Host regulatory proteins prevent excessive complement activation.
Deficiency: Lack of complement proteins increases susceptibility to infection.
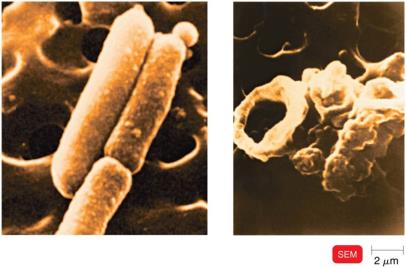
Evasion: Some pathogens evade complement by producing capsules.
Interferons
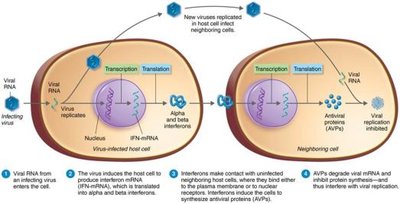
Interferons (IFNs) are cytokines with antiviral activity. Types alpha (IFN-α) and beta (IFN-β) are produced by virus-infected cells and induce neighboring cells to produce antiviral proteins. Gamma interferon (IFN-γ) activates neutrophils and macrophages to kill bacteria.
Other Nonspecific Defenses
Iron-Binding Proteins: Host proteins (transferrin, lactoferrin, ferritin, hemoglobin) sequester iron, limiting pathogen growth. Some bacteria produce siderophores to compete for iron.
Antimicrobial Peptides: Short peptides (e.g., defensins, cathelicidins) produced in response to microbes; inhibit cell wall synthesis, form pores, or destroy nucleic acids.
Genetic Resistance: Certain genetic traits (e.g., sickle cell trait) confer resistance to specific pathogens.
Age and Health Practices: Very young and elderly are more susceptible; healthy practices (hand hygiene, cough etiquette, safe sex) reduce infection risk.
