 Back
BackInnate Immunity: Principles and Mechanisms
Study Guide - Smart Notes

Innate Immunity
Introduction to Immunity
An immune response is a physiological process coordinated by the immune system to eliminate antigens.
Immune: Resistant to a pathogen or microbe.
Susceptible: Not immune; infection may occur.
The immune system is divided into two main branches: innate immunity and adaptive immunity.
Common features
Recognize diverse pathogens
eliminate indentified invaders
discriminate between self and foreign antigens
Classification of Immune Responses
Innate Immunity: Inborn, non-specific, and ancient protection present in all eukaryotes. Provides generalized responses and acts rapidly.
Non-specific immunity
Adaptive Immunity: Found only in vertebrates, matures over time, and tailors responses to specific pathogens. Exhibits memory and typically requires 4–7 days to fully activate.
Immunity is organized into three lines of defense:
Innate immunity:
Barrier defenses
Cellular and molecular defenses
Adaptive immunity:
Adaptive defenses
Normal Microbiota and Immune Function
Role of Normal Microbiota
The normal microbiota plays a crucial role in shaping immune responses and conferring protection.
According to the hygiene hypothesis, reduced diversity and abundance of microbiota may negatively affect immune development.
Studies in germ-free animals show that microbe-free environments lead to underdeveloped immune systems.
Benefits of normal microbiota:
Compete with pathogens for nutrients and space
Produce substances that damage pathogens
Create environments that limit pathogen survival

First-Line Defenses
Overview of First-Line Defenses
First-line defenses
Mechanical barriers: Rinse, flush, or trap pathogens (e.g., tears, urine, saliva, mucus membranes).
Chemical barriers: Directly attack invaders or create hostile environments (e.g., lysozyme, stomach acid, fatty acids in sweat and earwax).
Physical barriers: Structures that physically block pathogen entry (e.g., skin, epithelial tissue).
Mechanical Barriers
Tears wash debris and pathogens from eyes.
Urine flushes microbes from the urinary tract.
Saliva limits microbial adherence in the mouth.
Mucus membranes trap microbes at body entrances and internal surfaces.
Mucociliary escalator sweeps debris from lungs toward the mouth. (e.g sneezing)
Chemical Barriers
May directly attack invaders or establish environments that limit pathogen survival in or on a particular tissue
Lysozyme: found in secretions; Enzyme in tears, mucus, saliva, and breast milk that breaks down bacterial cell walls.
Hydrochloric acid: Stomach acid that destroys pathogens.
Skin: dry, salty, and slightly acidic
Fatty acids: Present in sweat and earwax,
Antimicrobial peptides (AMPs)
AMPs are proteins that destroy a wide spectrum of viruses, bacteria, fungi, and parasites. They are rare targets for microbial resistance and can:
Stimulate leukocytes (modulate inflammation, promote phagocytosis)
Directly disrupt microbial membranes and target intracellular components
Defensins are a key class of mammalian AMPs that rapidly kill invaders by inserting into cell membranes.
Physical Barriers
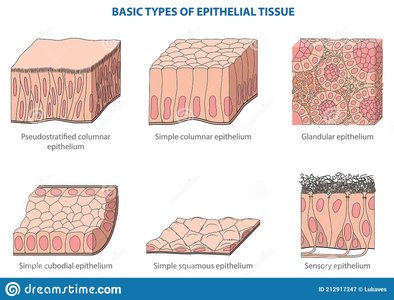
Epithelial tissue: Lines all body cavities and entrances, forming a main physical barrier.
Skin: Composed of tightly packed dead epithelial cells enriched with proteins and lipids, providing a water-resistant layer.
Second-Line Defenses
Leukocytes (White Blood Cells)
When first-line defenses are breached, second-line defenses involving leukocytes and molecular factors are activated.
Leukocytes are classified as:
Granulocytes: Contain visible granules (e.g., neutrophils, eosinophils, basophils, mast cells).
Agranulocytes: Lack visible granules (e.g., monocytes, dendritic cells, lymphocytes).
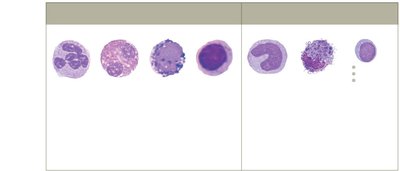
Granulocytes
Neutrophils: Most abundant, first responders, highly phagocytic, release AMPs.
Eosinophils: Less than 5% of WBCs, attack parasites and allergens, moderate phagocytosis.
Basophils: Less than 1% of WBCs, release histamine, involved in allergic responses and combating parasites.
Mast cells: Reside in tissues, release histamine, involved in allergies and parasite defense, capable of phagocytosis.
Agranulocytes
Monocytes: Largest agranular WBCs, mature into macrophages in tissues, highly phagocytic.
Macrophages
Fixed: reside in specific tissues
Wandering: roam through tissues
Dendritic cells: Highly phagocytic, patrol tissues, abundant near body openings, prevent inappropriate immune responses.
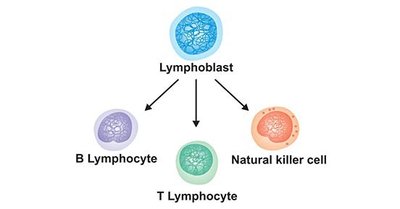
Lymphocytes: Include natural killer (NK) cells (innate immunity), B cells, and T cells (adaptive immunity).
Natural Killer (NK) Cells
NK cells are lymphocytes that provide innate protection against viruses, bacteria, parasites, and tumor cells. They are abundant in the liver and act by recognizing and destroying infected or abnormal cells.
Molecular Defenses
Cytokines
Cells release chemicals to communicate
Cytokines are signaling proteins that mediate and regulate immunity, inflammation, and hematopoiesis. They are produced by various cells, including innate immune cells, liver, epithelial cells, and adaptive immune cells.
Stimulate inflammation and fever
Recruit leukocytes
Promote tissue repair and immune regulation
Include chemokines, interleukins, interferons, and tumor necrosis factors
Chemokines
Recruit the cell towards an area that has damage
• Cytokines that act as signaling proteins that attract white blood cells to areas where they are needed
• Induce chemotaxis
• Aid in wound healing, blood vessel formation and repair, lymphoid tissue development, and activation of innate and adaptive immune responses
Interleukins (Ils)
• Activate adaptive and innate immune responses
• Stimulate hematopoiesis (blood cell formation)
• IL-1 family regulates inflammation, stimulates innate and adaptive immune responses, and generates fever
• IL-2 family are central to T cell development, self tolerance, triggering apoptosis
Interferon (IFNs)
• Virus-infected cells make IFN-α and IFN-β as alarms that stimulate nearby uninfected cells to mount antiviral defenses
• Small proteins that act as signaling molecules
• Signal when pathogens or tumor cells are detected
• Up-regulates interferon-stimulated genes (ISGs) (apoptosis, anti-viral response
Tumor necrosis factors (TNFs)
• Signaling protein
• TNF-α
• Made primarily by macrophages
• Stimulates inflammation, kills tumor cells, and stimulates fever
• TNF inhibitors are approved by U.S. Food and Drug Administration (FDA) to treat a variety of conditions, including rheumatoid arthritis (RA), psoriatic arthritis, inflammatory bowel disease (IBD) and ankylosing spondylitis.
Iron-Binding Proteins
Iron is essential for both host and microbial cells.
The host limits free iron availability using proteins such as
hemoglobin
ferritin
lactoferrin
transferrin.
Some pathogens counteract this by producing siderophores or lysing red blood cells to access iron.
Siderophores- organic molecules that pull iron from our proteins
Hemolytic bacteria- break down RBCs to get the iron-rich hemoglobin inside
Complement System REFER TO LECTURE
The complement system consists of proteins produced by the liver that circulate in an inactive state. Activation occurs via three pathways:
Classical pathway: Triggered by antibodies bound to microbes.
Lectin pathway: Triggered by mannose-binding lectin binding to microbial carbohydrates.
Alternative pathway: Triggered directly by microbial surfaces.
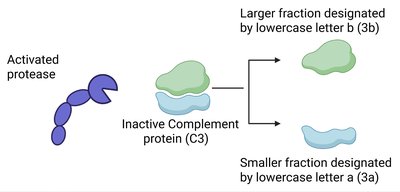
All pathways converge to activate C3, leading to three main outcomes:
Opsonization: Tagging invaders for phagocytosis.
Membrane Attack Complex (MAC): Direct lysis of target cells.
Inflammation: Recruitment of immune cells and enhancement of inflammatory responses.
Inflammation and Fever
Inflammation
Inflammation is an innate immune response to tissue damage or infection. Its main goals are to recruit immune defenses, limit pathogen spread, and promote tissue repair. The process occurs in three phases:
Vascular changes: Increased blood flow and vessel permeability.
Leukocyte recruitment: Leukocytes exit blood vessels (margination and diapedesis) and migrate to the site of injury.
Resolution: Inflammation subsides, tissue repair begins, and excess leukocytes undergo apoptosis.
Chronic Inflammation
Chronic inflammation occurs when the response is prolonged, leading to tissue damage and contributing to diseases such as atherosclerosis, cancer, and neurodegenerative disorders. Treatment includes NSAIDs and steroidal anti-inflammatory drugs.
Fever (Pyrexia)
Fever is a systemic innate immune response characterized by an elevated body temperature. It is triggered by pyrogens (e.g., bacterial toxins, cytokines) that signal the hypothalamus to raise the body's temperature set point.
Enhances antiviral effects of interferons
Increases phagocyte efficiency and leukocyte production
Limits growth of certain pathogens
Promotes tissue repair
Low-grade fever is generally protective, while high-grade fever (>40.5°C) is life-threatening and requires medical intervention.
Summary Table: Key Components of Innate Immunity
Component | Function | Example |
|---|---|---|
Mechanical Barriers | Physically remove pathogens | Tears, urine, mucociliary escalator |
Chemical Barriers | Destroy or inhibit pathogens | Lysozyme, stomach acid, AMPs |
Physical Barriers | Block pathogen entry | Skin, epithelial tissue |
Leukocytes | Phagocytosis, immune signaling | Neutrophils, macrophages, dendritic cells |
Cytokines | Coordinate immune responses | Interleukins, interferons, TNF-α |
Iron-Binding Proteins | Limit microbial access to iron | Transferrin, lactoferrin |
Complement System | Opsonization, cytolysis, inflammation | C3, MAC |
Fever | Enhances immune function | Pyrogens, hypothalamic regulation |
Key Equations and Concepts
Opsonization: Tagging of pathogens for enhanced phagocytosis by immune cells.
Diapedesis: The process by which leukocytes squeeze through blood vessel walls to reach infected tissues.
Pyrogens: Fever-inducing agents that act on the hypothalamus.
SUMMARY OF THE WHOLE LECTURE
1. Innate Immunity is a non-specific immunity, fast to act and protects the host from a microbial threat.
2. Innate Immunity consists of mechanical barrier, chemical barrier, cells of innate immune system, cytokines, iron-binding proteins, complement system, and fever (to a certain extent)
3. Interferons protect the host from viral agents.
4. Inflammation is part of host immunity that plays a role in recruiting various immune cells at the site of infection or tissue damage, and is involved in tissue healing
