 Back
BackInnate Immunity: The Body’s First and Second Lines of Defense
Study Guide - Smart Notes

Innate Immunity
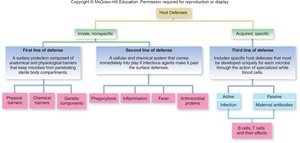
Overview of Host Defenses
Innate immunity represents the body’s nonspecific defense mechanisms, always present and ready to respond to pathogens. It is distinct from acquired (adaptive) immunity, which is specific and develops after exposure to antigens.
First Line of Defense: Physical, chemical, and genetic barriers that prevent pathogen entry.
Second Line of Defense: Cellular and chemical responses that act when pathogens breach the first line.
First Line of Defense
Physical and Chemical Barriers
The first line of defense includes structures and secretions that block pathogen entry. These barriers are constitutive, meaning they do not improve with repeated exposure.
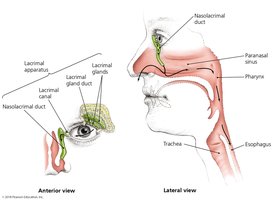
Physical Defenses: Skin, mucous membranes, and associated structures.
Chemical Defenses: Antimicrobial peptides, lysozyme, sebum, and acidic pH.
Phagocytic Defenses: Epidermal dendritic cells and other phagocytes in tissues.
Inflammatory Defenses: Initial response to tissue damage.
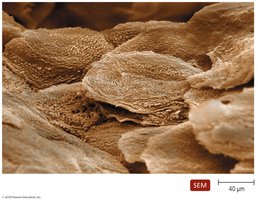
The Skin as a Barrier
The skin is composed of two major layers: the epidermis and dermis. The epidermis consists of tightly packed cells, making it difficult for pathogens to penetrate. Shedding of dead skin cells removes microorganisms, and dendritic cells phagocytize pathogens. The dermis contains collagen fibers that resist abrasions.
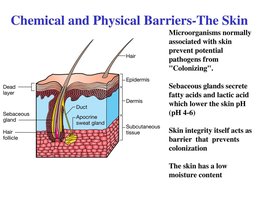
Chemical Defenses of the Skin
Perspiration: Contains salt, antimicrobial peptides, and lysozyme, which inhibit microbial growth and destroy bacterial cell walls.
Sebum: Secreted by sebaceous glands, keeps skin pliable and lowers pH, inhibiting many bacteria.
Mucous Membranes
Mucous membranes line all body cavities open to the environment. They consist of tightly packed cells and continually shed cells to remove microorganisms. Dendritic cells phagocytize pathogens, and goblet and ciliated columnar cells help remove invaders.
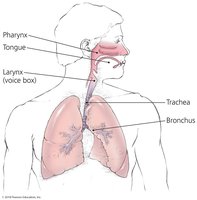
Comparison of Skin and Mucous Membranes
Skin and mucous membranes differ in structure and function, but both serve as effective barriers against pathogens.
Feature | Skin | Mucous Membrane |
|---|---|---|
Number of Cell Layers | Many | One to a few |
Cells Tightly Packed? | Yes | Yes |
Cells Dead or Alive? | Outer layers dead | Alive |
Mucus Present? | No | Yes |
Relative Water Content | Dry | Moist |
Defensins Present? | Yes | Yes |
Lysozyme Present? | Yes | With some |
Sebum Present? | Yes | No |
Cilia Present? | No | Trachea, uterine tubes |
Constant Shedding and Replacement of Cells? | Yes | Yes |
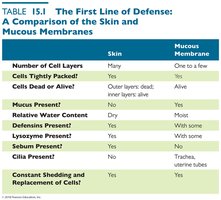
Lacrimal Apparatus
The lacrimal apparatus produces and drains tears, which wash the surface of the eye. Lysozyme in tears destroys bacteria.
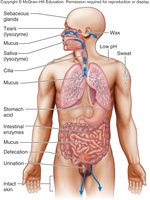
Secretions and Activities Contributing to Defense
Various organs secrete chemicals with antimicrobial properties, contributing to the first line of defense.
Secretion/Activity | Function |
|---|---|
Digestive System | Saliva, stomach acid, intestinal enzymes, defecation remove or destroy microbes |
Urinary System | Urine washes microbes from urethra |
Reproductive System | Acidity and mucus inhibit microbes |
Cardiovascular System | Blood removes pathogens from wounds |

Second Line of Defense
Blood Components
When pathogens penetrate the first line, the second line of defense is activated. Blood contains plasma (water, electrolytes, proteins), cells, and platelets. Plasma contains iron-binding compounds, complement proteins, and antibodies.
Hematopoiesis: Production of Blood Cells
Blood cell production begins in the yolk sac during embryonic development, then shifts to the liver and lymphatic organs, and finally to the bone marrow.
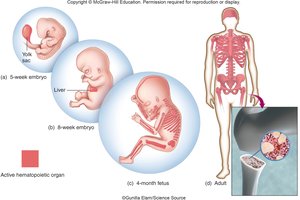
Types of Blood Cells
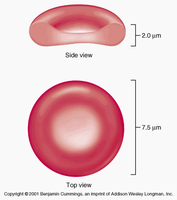
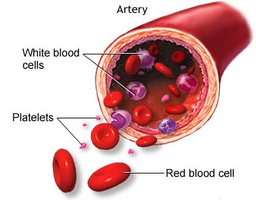
Erythrocytes (RBCs): Transport oxygen and carbon dioxide; do not have immune function.
Platelets: Cell fragments involved in blood clotting and inflammation.
Leukocytes (White Blood Cells): Key players in immune defense.
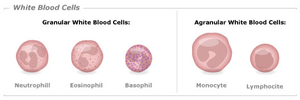
Classification of White Blood Cells
Granulocytes: Neutrophils, eosinophils, basophils; contain granules and have lobed nuclei.
Agranulocytes: Monocytes, lymphocytes; have unlobed, rounded nuclei.
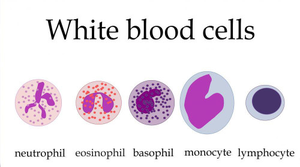
Functions of White Blood Cells
Neutrophils: Phagocytosis and production of toxic chemicals.
Eosinophils: Attack large eukaryotic pathogens (e.g., worms).
Basophils: Involved in inflammatory responses and histamine production.
Monocytes/Macrophages: Phagocytic cells, fixed or wandering in tissues.
Lymphocytes: Major component of specific immunity (T cells and B cells).
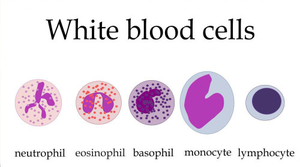
Phagocytosis
Phagocytosis is the process by which phagocytes ingest and destroy pathogens. It involves chemotaxis, binding, ingestion, lysosomal fusion, killing, and waste elimination.
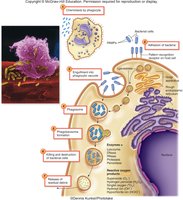
Mechanisms of Killing by Phagocytes
Enzymatic Hydrolysis: Lysozyme, lipases, proteases, nucleases break down pathogens.
Oxidative Burst: Production of strong oxidizers such as superoxide anion, hydrogen peroxide, and hypochlorite.
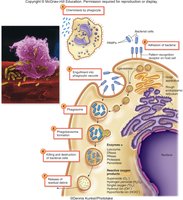
Microbial Evasion of Phagocytosis
Some pathogens possess mechanisms to evade or survive phagocytosis, such as capsules or resistance to lysosomal enzymes.
Nonphagocytic Killing Mechanisms
Eosinophils: Secrete toxins to kill helminths; eosinophilia indicates infestation or allergies.
Neutrophils: Produce chemicals and NETs to kill microbes.
Natural Killer (NK) Cells: Secrete toxins onto infected or tumor cells.
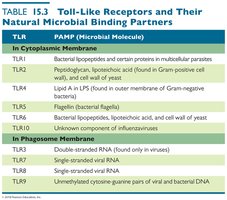
Toll-like Receptors (TLRs)
TLRs are membrane proteins produced by phagocytic cells that bind pathogen-associated molecular patterns (PAMPs) and initiate defensive responses.
TLR | PAMP (Microbial Molecule) |
|---|---|
TLR1 | Bacterial lipoproteins and certain proteins in multicellular parasites |
TLR2 | Peptidoglycan, lipoteichoic acid, cell wall of yeast |
TLR4 | Lipid A in LPS (outer membrane of Gram-negative bacteria) |
TLR5 | Flagellin (bacterial flagella) |
TLR6 | Bacterial lipoproteins, lipoteichoic acid, cell wall of yeast |
TLR7 | Unknown component of influenzaviruses |
TLR3 | Double-stranded RNA (viruses) |
TLR8 | Single-stranded viral RNA |
TLR9 | Unmethylated cytosine guanine pairs of viral and bacterial DNA |
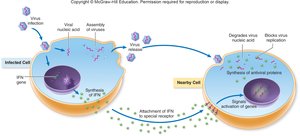
Interferons
Interferons are protein molecules released by host cells to inhibit the spread of viral infections. INF Alpha and Beta stimulate phagocytosis, while INF Gamma regulates T and B cell actions.
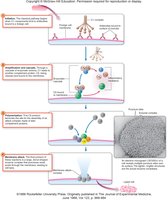
Complement System
The complement system consists of over 30 blood serum proteins that act in a cascade reaction to stimulate inflammation, attract phagocytes, and form membrane attack complexes.
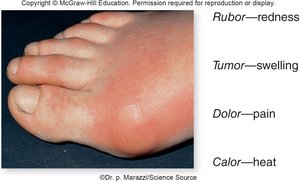
Inflammation
Inflammation is a nonspecific response to tissue damage. The classic signs are rubor (redness), calor (heat), tumor (swelling), and dolor (pain). Vasodilation and increased permeability of blood vessels deliver clotting proteins and facilitate tissue repair.
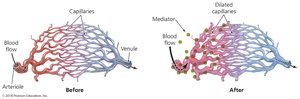
Events of Inflammation
Following a cut and infection, inflammation involves migration of phagocytes, tissue repair, and clearing of debris. Acute inflammation is beneficial and short-lived, while chronic inflammation can cause tissue damage.
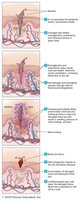
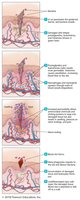
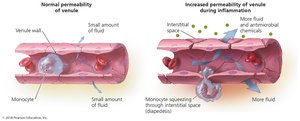
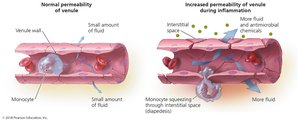
Migration of Phagocytes and Tissue Repair
Phagocytes are recruited to the site of infection by chemotactic factors, attach to blood vessel receptors (marginalization), and squeeze between cells (diapedesis). Delivery of nutrients and oxygen facilitates repair.
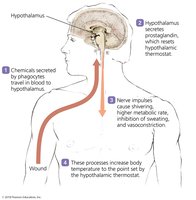
Fever
Fever is a body temperature over 37°C, triggered by pyrogens that stimulate the hypothalamus. Fever enhances interferon effects, inhibits microbial growth, and may enhance phagocyte activity and tissue repair.
Summary Table: Nonspecific Components of Innate Immunity
First Line | Phagocytosis | Extracellular Killing | Complement | Interferons | Antimicrobial Peptides | Inflammation | Fever |
|---|---|---|---|---|---|---|---|
Skin and mucous membranes | Phagocytes ingest pathogens | Eosinophils and NK cells kill pathogens | Components stimulate inflammation and attack pathogens | Increase resistance to viral infections | Interfere with microbial growth | Redness, swelling, pain, heat | Modifies internal environment, inhibits pathogens |

