 Back
BackInnate Immunity: The Body’s First and Second Lines of Defense
Study Guide - Smart Notes

Innate Immunity
Introduction to Immunity
Immunology is the study of the immune system, which protects the body from infection by microorganisms. Immunity refers to the state of having protection against infection. There are two main types of immunity: innate immunity (inborn, nonspecific defenses) and adaptive immunity (specific, acquired defenses).
Innate immunity: Inborn resistance to pathogens, involving nonspecific barriers, cells, and molecules. It includes the first and second lines of defense.
Adaptive immunity: The body’s ability to recognize and defend itself against specific invaders and their products. It is the third line of defense (covered in Chapter 16).
Mechanisms to Prevent Infection
First Line of Defense: Physical and Chemical Barriers
The first line of defense consists of physical and chemical barriers that prevent pathogens from entering the body.
Physical barriers: Skin, lungs, acidity of stomach and vagina, saliva, tears, mucus in the nose and nasopharynx, and intestines.
Chemical barriers: Perspiration (contains salt and antimicrobial peptides), lysozyme (destroys bacterial cell walls), and sebum (lowers skin pH and keeps skin pliable).
Skin: The epidermis and dermis are composed of multiple layers of tightly packed cells. Epidermal dendritic cells phagocytize pathogens, and collagen fibers help resist abrasions.
Mucous membranes: Line all body cavities open to the environment. The epithelium is tightly packed and continually sheds, carrying away microorganisms. Dendritic cells below the epithelium phagocytize pathogens and produce defensive chemicals.
Lacrimal apparatus: Produces and drains tears, which contain lysozyme to destroy bacteria.
Other first-line defenses: Antimicrobial peptides are present in skin, mucous membranes, and neutrophils, acting against a variety of microbes. Many organs secrete chemicals with antimicrobial properties.
The Microbiome in Innate Immunity
The microbiome competes with potential pathogens through microbial antagonism or competitive inhibition. Members of the microbiome:
Consume nutrients, making them unavailable to pathogens
Create environments unfavorable to other microbes
Prevent pathogens from attaching to host cells
Stimulate the body’s second line of defense
Generate antimicrobial compounds and vitamins
Modulate immunity
The Body’s Second Line of Defense
Overview
The second line of defense operates when pathogens penetrate the skin or mucous membranes. It is composed of cells, antimicrobial chemicals, and processes, many of which are found in the blood.
Plasma: Mostly water, containing electrolytes, dissolved gases, nutrients, and proteins (including complement proteins and antibodies).
Serum: Plasma without clotting factors.
Formed elements: Cells and cell fragments in plasma, including erythrocytes (oxygen and carbon dioxide transport), platelets (clotting), and leukocytes (defense).
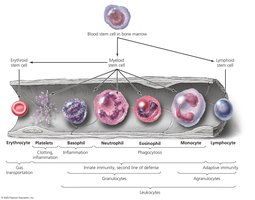
Leukocytes (White Blood Cells)
Leukocytes are divided into two main groups based on the presence or absence of granules:
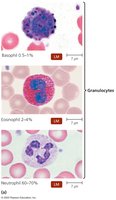
Granulocytes: Basophils, eosinophils, and neutrophils (contain large granules).
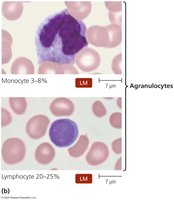
Agranulocytes: Monocytes (mature into macrophages) and lymphocytes (B cells, T cells, and natural killer cells).
Phagocytosis
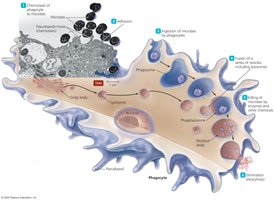
Phagocytosis is the process by which certain cells (phagocytes) engulf and destroy foreign matter. The process can be divided into six stages:
Chemotaxis: Phagocytes are attracted to the site of infection by chemical signals.
Adhesion: Phagocyte adheres to the microbe or particle.
Ingestion: Microbe is engulfed and placed into a phagosome.
Maturation: Phagosome fuses with a lysosome to form a phagolysosome.
Killing: Enzymes and chemicals digest the microbe.
Elimination: Debris is released from the cell or the phagocyte dies.
Nonphagocytic Killing
Eosinophils: Attack parasitic helminths by adhering to their surface and releasing toxins.
Natural killer (NK) cells: Secrete toxins onto the surface of virally infected cells and tumors, distinguishing normal cells by their membrane proteins.
Neutrophils: Can destroy microbes without phagocytosis by producing chemicals that kill nearby invaders.
Nonspecific Chemical Defenses
Toll-like receptors (TLRs): Recognize pathogen-associated molecular patterns (PAMPs) and activate immune responses.
NOD proteins: Detect intracellular pathogens and trigger immune responses.
Interferons: Proteins released by host cells to inhibit viral replication.
Complement system: A group of proteins that enhance immune responses, including opsonization, inflammation, and cell lysis.
Inflammation: A nonspecific response to tissue damage, characterized by redness, heat, swelling, and pain. Acute inflammation is typically beneficial, while chronic inflammation can cause tissue damage.
Fever: An increase in body temperature above 37°C, triggered by pyrogens. Fever can inhibit pathogen growth and enhance immune responses.
Summary Table: Key Components of Innate Immunity
Component | Function |
|---|---|
Skin & Mucous Membranes | Physical and chemical barriers to entry |
Microbiome | Competes with pathogens, produces antimicrobial compounds |
Phagocytes | Engulf and destroy pathogens |
Natural Killer Cells | Kill infected or abnormal cells |
Complement System | Enhances immune responses, lyses pathogens |
Inflammation | Recruits immune cells, promotes healing |
Fever | Inhibits pathogens, enhances immune function |
Additional info: Adaptive immunity, including humoral and cell-mediated responses, is covered in Chapter 16. The exact mechanism of fever is not fully understood, but it is known to be triggered by various pyrogens.
