 Back
BackInteractions Between Microbes and Humans: Pathogenesis, Virulence, and Disease Progression
Study Guide - Smart Notes

Interactions Between Microbes and Humans
Introduction
This chapter explores the complex interactions between microbes and humans, focusing on the processes of colonization, infection, and disease. It covers the human microbiome, mechanisms of microbial pathogenesis, virulence factors, and the progression of infectious diseases, including reservoirs and transmission.
Colonization, Infection, and Disease
Definitions and Distinctions
Colonization: The presence and growth of microbes on or within the body without causing disease. These microbes are often part of the normal flora and are kept in check by the host's defenses.
Infection: Occurs when microbes overcome host defenses, enter tissues, and begin to multiply.
Disease: A deviation from health resulting from the cumulative effects of infection that damage or disrupt tissues and organs, leading to symptoms.
Infectious Disease: A pathologic state caused directly by microorganisms or their products.

The Human Microbiome
Normal Flora and Its Roles
Human Microbiome: The total collection of microbes found on and in a normal human. Most resident microbiota colonize us long-term and do not cause disease.
Benefits:
Antagonism against pathogens
Prevention of pathogen attachment and growth
Development of the immune response
Risks: Opportunistic infections can occur if microbes are introduced into unusual sites, if the immune system is suppressed, or if the normal microbiota is disrupted.
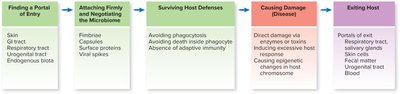
Steps in Microbial Pathogenesis
Overview of Disease Progression
Microbes must complete several steps to cause disease in a host:
Finding a portal of entry
Attaching firmly to host cells
Surviving host defenses
Causing damage (disease)
Exiting the host
Portals of Entry
Mucous Membranes: Respiratory tract (most common), gastrointestinal tract, genitourinary tract, conjunctiva.
Skin: Entry via insect bites, wounds, or injections.
Placenta: Some pathogens can cross the placenta (TORCHES: Toxoplasma gondii, Rubella virus, Cytomegalovirus, Herpes simplex virus, HIV, Syphilis, and others).
Exogenous vs. Endogenous: Exogenous pathogens come from outside the body; endogenous originate from within the host.
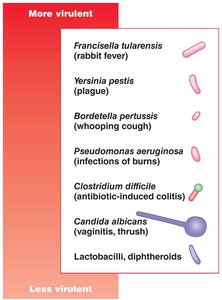
Infectious Dose (ID)
Infectious Dose (ID): The minimum number of microbes required to cause infection. Microbes with a lower ID are considered more virulent.
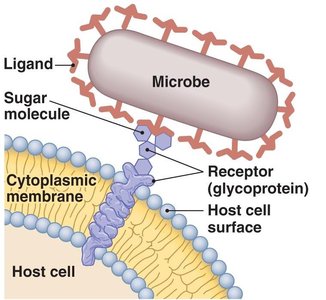
Adhesion to Host Cells
Adhesion: The process by which microbes attach to host tissues, often via specific interactions between microbial ligands and host cell receptors.
Mechanisms: Fimbriae (pili), surface proteins, adhesive slimes or capsules (bacteria, fungi, protozoa); specialized receptors (viruses).
Importance: Firm attachment is usually required for infection, as the body has mechanisms to flush out unattached microbes.
Pathogenicity and Virulence
Definitions
Pathogenicity: The ability of a microorganism to cause disease.
Virulence: The degree of pathogenicity; often determined by the presence of virulence factors.
Virulence Factors: Traits that contribute to a microbe's ability to cause disease, including adhesion factors, biofilms, extracellular enzymes, toxins, and antiphagocytic factors.
Surviving Host Defenses
Antiphagocytic Factors
Phagocytes: Host cells that engulf and destroy pathogens.
Microbial Strategies:
Leukocidins: Kill phagocytes directly.
Capsules: Inhibit phagocytosis.
Intracellular Survival: Some bacteria survive inside phagocytes.
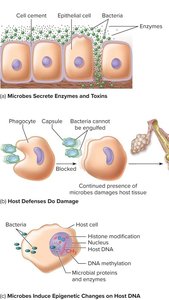
Causing Disease: Mechanisms of Tissue Damage
Virulence Factors and Host Damage
Direct Damage: Enzymes and toxins produced by microbes can directly harm host tissues.
Immune Response: Microbes may induce excessive or inappropriate host immune responses, causing tissue damage.
Epigenetic Changes: Some pathogens alter host gene expression to facilitate infection.
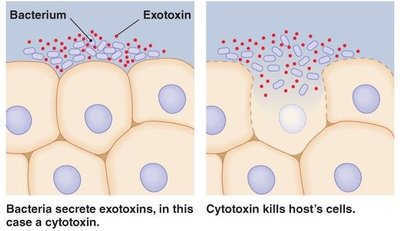
Toxins
Exotoxins: Proteins secreted by bacteria (both Gram-positive and Gram-negative) into the surrounding environment. They are highly potent and have specific effects on host cells.
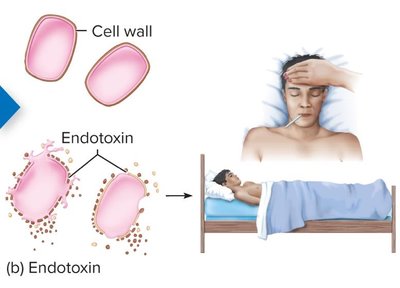
Endotoxins: Components of the outer membrane of Gram-negative bacteria (Lipid A of lipopolysaccharide). Released when bacteria die and are less specific in their effects, often causing fever, shock, and inflammation.
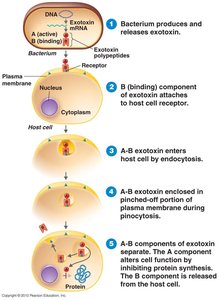
Types of Exotoxins
A-B Toxins: Consist of an active (A) component and a binding (B) component. The B component binds to the host cell, allowing the A component to enter and disrupt cellular function.
Membrane-Disrupting Toxins: Cause cell lysis by forming pores or disrupting membrane phospholipids (e.g., hemolysins, leukocidins).
Superantigens: Non-specifically activate large numbers of T cells, leading to massive cytokine release and potentially fatal immune responses (e.g., toxic shock syndrome toxin).
Enzymes as Virulence Factors
Coagulases: Cause blood clotting, protecting bacteria from phagocytosis.
Kinases: Break down clots, allowing bacteria to spread.
Hyaluronidases: Digest connective tissue, aiding in microbial spread.
Collagenases: Break down collagen in connective tissues.
IgA Proteases: Destroy IgA antibodies on mucosal surfaces.
Progression and Stages of Infectious Disease
Stages of Disease
Incubation Period: Time between initial contact and appearance of symptoms; pathogen is multiplying.
Prodromal Stage: Early, mild symptoms such as malaise and discomfort.
Acute Phase: Pathogen multiplies at high levels; specific symptoms are most pronounced.
Convalescent Period: Symptoms decline; patient recovers, but pathogens may still be present.
Continuation Phase: In some cases, the pathogen or symptoms persist after apparent recovery.
Reservoirs and Transmission of Infectious Agents
Types of Reservoirs
Living Reservoirs: Humans (actively ill or carriers), animals (zoonoses), and arthropods (biological vectors).
Nonliving Reservoirs: Soil, water, and air can harbor pathogens for extended periods.
Zoonosis
Zoonosis: Infections indigenous to animals but naturally transmissible to humans. Many emerging diseases are zoonotic and may involve complex life cycles and multiple hosts.
Healthcare-Associated Infections (HAIs)
Definition and Significance
HAIs (Nosocomial Infections): Infections acquired during a hospital or healthcare facility stay. Affect 0.1–20% of patients, with significant morbidity and mortality.
Common Types: Pneumonia, gastrointestinal illness, urinary tract infections, bloodstream infections, surgical site infections.
Common Pathogens: Clostridioides difficile, Staphylococcus aureus, Klebsiella spp., Escherichia coli, Enterococcus spp.
Prevention and Control
Infection Control Officer: Oversees infection prevention practices, outbreak tracking, and staff training.
Universal Precautions: All bodily fluids are treated as potentially infectious; strict aseptic techniques are enforced.
Key Disease Terms
Sign: Objective evidence of disease (e.g., fever, rash).
Symptom: Subjective evidence as sensed by the patient (e.g., pain, fatigue).
Syndrome: A set of signs and symptoms that characterize a disease.
Septicemia: Microorganisms multiplying in the blood.
Bacteremia/Viremia: Presence of bacteria/viruses in the blood without multiplication.
Asymptomatic/Subclinical: Infection without noticeable symptoms.
