Back
BackMicrobial Cardiovascular and Systemic Diseases: Structure, Pathogenesis, and Clinical Features
Study Guide - Smart Notes

Microbial Cardiovascular and Systemic Diseases
Structures of the Cardiovascular System
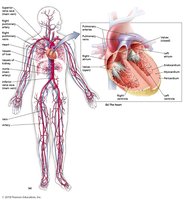
The cardiovascular system is essential for transporting blood, nutrients, and immune cells throughout the body. It consists of the heart, blood, and blood vessels, and is closely linked to the lymphatic system.
Heart: Pumps blood into arteries, which are connected to veins via capillaries.
Arteries: Carry blood away from the heart.
Veins: Return blood to the heart.
Blood composition: Includes serum (liquid portion) and formed elements (erythrocytes, leukocytes, platelets).
Movement of Blood and Lymph
Blood circulates through the heart, lungs, and body tissues, while the lymphatic system collects leaked fluid and returns it to the bloodstream. Blood is normally axenic (germ-free), but breaches in skin or mucous membranes can allow microbial entry, potentially leading to systemic diseases.
Bacterial Cardiovascular and Systemic Diseases
Septicemia, Bacteremia, and Toxemia
These conditions involve the presence of microbes or their toxins in the blood, leading to systemic illness.
Septicemia: Any microbial infection of the blood causing illness.
Bacteremia: Presence of bacteria in the blood.
Toxemia: Toxins released by bacteria at a fixed site enter the bloodstream.
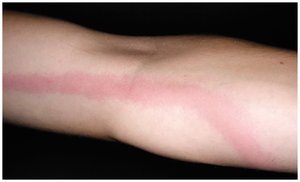
Lymphangitis: Infection and inflammation of lymphatic vessels, often seen as red streaks under the skin.
Signs and Symptoms
Fever, chills, nausea, vomiting, diarrhea, malaise
Septic shock (dangerously low blood pressure)
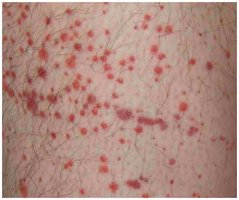
Petechiae (small hemorrhagic lesions)
Osteomyelitis (bone infection)
Symptoms of toxemia depend on the toxin (exotoxins vs. endotoxins)
Pathogens and Virulence Factors
Many bacteria can cause septicemia or toxemia, often as opportunistic or healthcare-associated infections.
Gram-negative bacteria are more commonly associated with severe septicemia due to endotoxin (Lipid A) release.
Virulence factors include capsules (resist phagocytosis) and siderophores (acquire iron).
Pathogenesis and Epidemiology
Direct inoculation of bacteria into blood (e.g., medical procedures, nonsterile needles, or infections elsewhere).
Immunocompetent individuals rarely develop septicemia.
Endotoxin triggers widespread inflammatory responses.
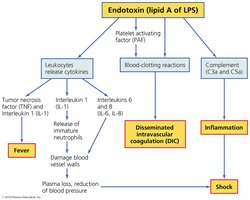
Diagnosis, Treatment, and Prevention
Diagnosis is primarily clinical; blood cultures may not always detect bacteria.
Treatment involves prompt antimicrobial therapy.
Prevention includes immediate treatment of infections, especially in immunocompromised individuals.
Endocarditis
Endocarditis is the inflammation of the endocardium, often due to bacterial infection. Vegetations (masses of platelets and clotting proteins) can form, protecting bacteria from immune defenses.
Signs and symptoms: Fever, fatigue, malaise, difficulty breathing, tachycardia, heart murmurs.
Pathogens: Often caused by normal microbiota (e.g., Viridans streptococci) entering the blood via wounds or dental procedures.
Risk factors: IV drug use, abnormal heart structure.
Diagnosis: Based on symptoms and echocardiogram visualization of vegetations.
Treatment: Intravenous antibacterial drugs; prophylactic antibiotics for high-risk patients.
Brucellosis
Brucellosis is a zoonotic disease caused by Brucella melitensis. It is transmitted via contaminated dairy products or contact with animal fluids.
Signs and symptoms: Fluctuating fever, arthritis, splenomegaly, endocarditis, meningitis.
Diagnosis: Serological tests and fever history.
Treatment: Combination antibiotics; animal vaccine available.
Tularemia
Tularemia is caused by Francisella tularensis, a highly infectious Gram-negative bacterium. It is transmitted via tick bites or contact with infected animals.
Signs and symptoms: Skin lesions, swollen lymph nodes, lymphangitis.
Diagnosis: Serological confirmation (not cultured due to high virulence).
Treatment: Antimicrobials (not beta-lactams); vaccine for at-risk individuals.
Plague
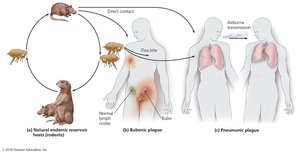
The plague, caused by Yersinia pestis, has two main forms: bubonic and pneumonic. It is transmitted by rodent fleas or direct contact with infected animals.
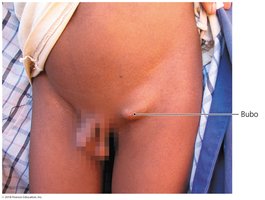
Bubonic plague: Enlarged lymph nodes (buboes), fever, chills, tissue necrosis.
Pneumonic plague: Lung infection, severe respiratory symptoms, nearly 100% fatal if untreated.
Virulence factors: Adhesins, type III secretion systems, capsules, antiphagocytic proteins, endotoxin.
Diagnosis: Based on symptoms; immediate treatment required.
Prevention: Rodent and flea control, hygiene.
Lyme Disease
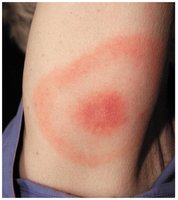
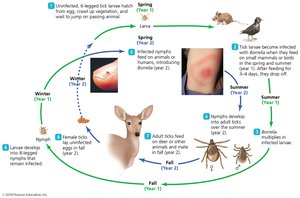
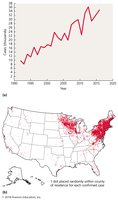
Lyme disease is a vector-borne illness caused by the spirochete Borrelia burgdorferi, transmitted by deer ticks (Ixodes spp.).
Signs and symptoms: Bull’s-eye rash, malaise, neurological and cardiac symptoms, severe arthritis.
Pathogenesis: Bacterium avoids immune detection by altering membrane proteins and does not require iron.
Diagnosis: Based on symptoms and antibody detection.
Treatment: Antimicrobials (early phase); anti-inflammatory drugs for late symptoms.
Prevention: Tick repellents, protective clothing.
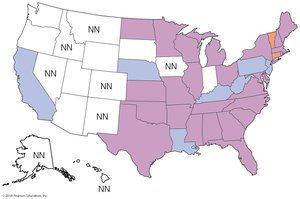
Ehrlichiosis and Anaplasmosis
These emerging tick-borne diseases are caused by Ehrlichia chaffeensis and Anaplasma phagocytophilum, respectively. Both are obligate intracellular parasites.
Signs and symptoms: Flu-like illness, leukopenia, thrombocytopenia.
Pathogenesis: Bacteria replicate in white blood cells, avoiding lysosomal destruction.
Diagnosis: Difficult; based on symptoms and epidemiology.
Treatment: Antimicrobials.
Prevention: Avoid tick-infested areas, use repellents and protective clothing.
Viral Cardiovascular and Systemic Diseases
Yellow Fever
Yellow fever is a mosquito-borne viral disease caused by the yellow fever virus and transmitted by Aedes aegypti mosquitoes.
Signs and symptoms: Three stages: fever, remission, and severe disease with jaundice and hemorrhaging.
Diagnosis: Clinical signs and viral antigen detection.
Prevention: Vaccine and mosquito control.

Infectious Mononucleosis
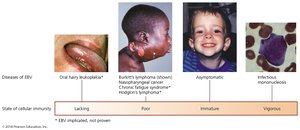
Also known as "mono" or the "kissing disease," this condition is caused by Epstein-Barr virus (EBV, HHV-4). It is transmitted via saliva and infects B lymphocytes.
Signs and symptoms: Severe sore throat, fever, swollen lymph nodes, fatigue, splenomegaly, rash.
Pathogenesis: EBV suppresses apoptosis in B cells, can become latent, and is associated with certain cancers.
Diagnosis: Presence of large, lobed B lymphocytes and neutropenia.
Treatment: Supportive care; avoid contact sports.
Cytomegalovirus Disease
Cytomegalovirus (CMV) is a herpesvirus that can cause severe disease in fetuses, newborns, and immunocompromised individuals. Transmission occurs via bodily secretions.
Signs and symptoms: Asymptomatic in most; severe complications in vulnerable populations.
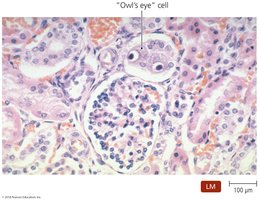
Diagnosis: Identification of "owl's eye" cells.
Treatment: Limited; fomivirsen for eye infections.
Dengue Fever
Dengue fever is a mosquito-borne viral disease with two phases and a risk of severe hemorrhagic fever upon reinfection with a different strain.
Signs and symptoms: Fever, pain, rash, and in severe cases, internal bleeding and shock.
Prevention: Vaccine and mosquito control.
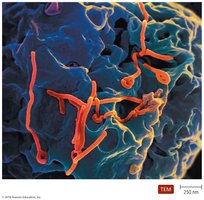
African Viral Hemorrhagic Fevers
Ebola and Marburg viruses cause severe hemorrhagic fevers with high mortality rates. Transmission occurs via contact with infected bodily fluids.
Signs and symptoms: Fever, fatigue, petechiae, severe hemorrhaging, shock, kidney failure.
Diagnosis: Clinical symptoms and virus detection in blood.
Treatment: Supportive; no effective antivirals.
Prevention: Vaccines under study.
Disease | Viral Genus (Family) | Natural Host(s) | Vector | Geographic Distribution |
|---|---|---|---|---|
Yellow fever | Flavivirus (Flaviviridae) | Humans, monkeys | Aedes aegypti mosquito | Africa, South America |
Dengue fever | Flavivirus (Flaviviridae) | Humans, monkeys | Aedes aegypti mosquito | Worldwide, especially tropics |
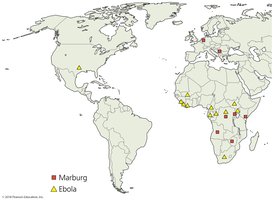
Ebola hemorrhagic fever | Ebolavirus (Filoviridae) | Probably bats | None | Central Africa, research facility in the US |
Marburg hemorrhagic fever | Marburgvirus (Filoviridae) | Probably bats | None | Central Africa, research facility in Europe |

Protozoan and Helminthic Cardiovascular and Systemic Diseases
Malaria
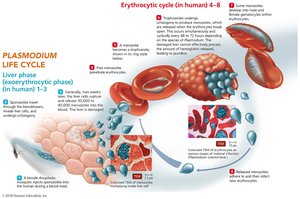
Malaria is a life-threatening disease caused by Plasmodium species, transmitted by Anopheles mosquitoes. The parasite's life cycle involves both liver and erythrocytic stages in humans.
Signs and symptoms: Recurrent fever, chills, anemia, jaundice, fatigue.
Genetic resistance: Sickle-cell trait, hemoglobin C, G6PD deficiency, and lack of Duffy antigens confer resistance.
Diagnosis: Identification of Plasmodium in blood.
Treatment: Antimalarial drugs; some strains are drug-resistant.
Prevention: Mosquito control, nets, protective clothing.
Toxoplasmosis
Toxoplasmosis is caused by the protozoan Toxoplasma gondii, with cats as the definitive host. It is a major concern for immunocompromised individuals and fetuses.
Signs and symptoms: Usually asymptomatic; severe disease in immunodeficient and congenital infections.
Transmission: Undercooked meat, contaminated soil, transplacental.
Diagnosis: Detection of organisms in tissues.
Treatment: Required for high-risk groups.
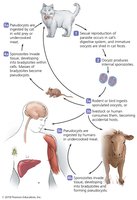
American Trypanosomiasis (Chagas’ Disease)
Chagas’ disease is caused by Trypanosoma cruzi and is endemic in Central and South America. It is transmitted by the bite of "kissing bugs."
Signs and symptoms: Swelling at infection site, chronic complications (cardiac, digestive).
Pathogenesis: Parasite evades immune system by living inside cells and changing surface antigens.
Diagnosis: Microscopic identification or xenodiagnosis.
Treatment: Early treatment is crucial; late stages are untreatable.
Prevention: Avoidance of vector insects.
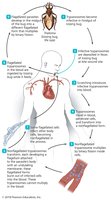
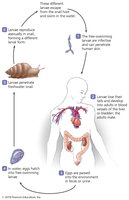
Schistosomiasis (Bilharzia)
Schistosomiasis is caused by blood flukes of the genus Schistosoma. The disease is prevalent in sub-Saharan Africa and involves a complex life cycle with snails as intermediate hosts.
Signs and symptoms: Swimmer's itch, organ damage due to egg deposition.
Diagnosis: Identification of eggs in stool or urine.
Treatment: Praziquantel.
Prevention: Avoid contaminated water, improve sanitation.