 Back
BackMicrobial Control: Principles, Methods, and Applications
Study Guide - Smart Notes

Basic Principles of Microbial Control
Terminology of Microbial Control
Understanding the terminology is essential for distinguishing between different microbial control strategies. These terms define the scope, effectiveness, and application of various methods used to control microbial growth.
Term | Definition | Examples | Comments |
|---|---|---|---|
Antisepsis | Reduction in the number of microorganisms and viruses, particularly potential pathogens, on living tissue | Iodine; alcohol | Antiseptics are frequently disinfectants whose strength has been reduced to make them safe for living tissues. |
Aseptic | Refers to an environment or procedure free of pathogenic contaminants | Preparation of surgical field; flame sterilization of laboratory equipment | Scientists, laboratory technicians, and health care workers use aseptic techniques. |
-cide/-cidal | Suffixes indicating destruction of a type of microbe | Bactericide; fungicide; germicide; virucide | Germicides include ethylene oxide, propylene oxide, and aldehydes. |
Degerming | Removal of microbes by mechanical means | Handwashing; alcohol swabbing | Chemicals play a secondary role to the mechanical removal of microbes. |
Disinfection | Destruction of most microorganisms and viruses on nonliving tissue | Phenolics; alcohols; aldehydes; soaps | Term is used primarily in relation to pathogens. |
Pasteurization | Use of heat to destroy pathogens and reduce the number of spoilage microorganisms in foods and beverages | Pasteurized milk and fruit juices | Heat treatment is brief to avoid altering taste. |
Sanitization | Removal of pathogens from objects to meet public health standards | Washing tableware in scalding water in restaurants | Standards of sanitization vary among governmental jurisdictions. |
-stasis/-static | Suffixes indicating inhibition, but not complete destruction, of a type of microbe | Bacteriostatic; fungistatic | Chemicals, refrigeration, and freezing are used to control growth. |
Sterilization | Destruction of all microorganisms and viruses on or in an object | Preparation of microbiological culture media and canned food | Typically achieved by steam under pressure, incineration, or ethylene oxide gas. |

Action of Antimicrobial Agents
Antimicrobial agents act by targeting essential cellular structures and functions. Their effectiveness depends on the type of microorganism and the environmental conditions.
Alteration of cell walls and membranes: Damaging the cell wall can cause cells to burst due to osmotic effects. Damaging the cytoplasmic membrane leads to leakage of cellular contents.
Damage to proteins and nucleic acids: Protein function depends on its three-dimensional shape, which can be disrupted by heat or chemicals. Nucleic acids can be altered or destroyed by chemicals, radiation, or heat, leading to fatal mutations or halted protein synthesis.
Nonenveloped viruses: These viruses are more tolerant of harsh conditions compared to enveloped viruses.
The Selection of Microbial Control Methods
Ideal Properties of Control Agents
Effective microbial control agents should be inexpensive, fast-acting, stable during storage, and capable of controlling microbial growth without harming humans, animals, or objects.
Factors Affecting Efficacy
Site to be treated: The method chosen depends on whether the site is a living tissue, medical instrument, or fragile object.
Relative susceptibility of microorganisms: Microbes vary in their resistance to antimicrobial agents. Germicides are classified as high, intermediate, or low effectiveness.
High-level germicides: Kill all pathogens, including endospores.
Intermediate-level germicides: Kill fungal spores, protozoan cysts, viruses, and pathogenic bacteria.
Low-level germicides: Kill vegetative bacteria, fungi, protozoa, and some viruses.

Microbial Death Rate
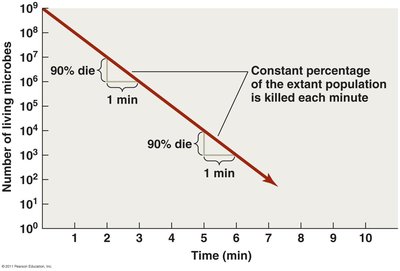
Microbial death rate is a key concept in evaluating the effectiveness of control methods. It describes the constant percentage of a microbial population killed per unit time.
Death rate: Typically follows a logarithmic decline, meaning a constant percentage is killed each minute.
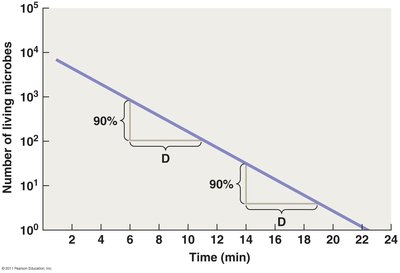
Decimal reduction time (D value): The time required to kill 90% of the population.
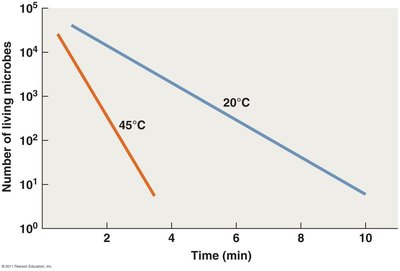
Effect of Temperature
Temperature significantly affects the efficacy of antimicrobial chemicals. Higher temperatures generally increase the rate of microbial death.
Methods for Evaluating Disinfectants and Antiseptics
Phenol Coefficient
The phenol coefficient compares the effectiveness of an agent to phenol. A value greater than 1.0 indicates greater efficacy than phenol.
Use-Dilution Test
Metal cylinders are dipped into bacterial cultures, then immersed in disinfectant dilutions.
Cylinders are washed and placed in growth medium; the most effective agents prevent growth at the highest dilution.
This is the current standard test in the U.S.
Kelsey-Sykes Capacity Test
Bacterial suspensions are added to the chemical being tested.
Samples are removed at intervals and incubated; lack of reproduction indicates effectiveness.
In-Use Test
Swabs are taken from objects before and after disinfectant application.
Swabs are inoculated into growth medium and incubated; growth is monitored to determine efficacy.
Physical Methods of Microbial Control
Heat-Related Methods
Heat is a widely used method for microbial control, acting by denaturing proteins, disrupting membranes, and destroying nucleic acids.
Thermal death point: Lowest temperature that kills all cells in 10 minutes.
Thermal death time: Time to sterilize a volume of liquid at a set temperature.
Moist Heat
Boiling: Kills vegetative cells of bacteria, fungi, protozoan trophozoites, and most viruses. Endospores, protozoan cysts, and some viruses may survive.
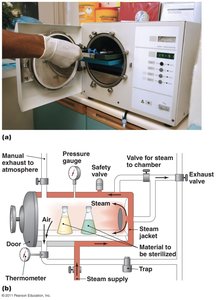
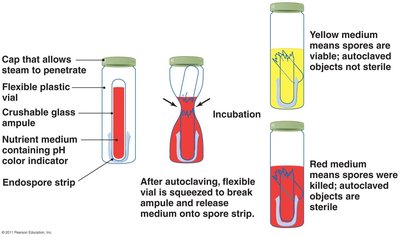
Autoclaving: Uses pressure to increase boiling temperature. Standard conditions: 121ºC, 15 psi, 15 min.
Pasteurization: Used for milk, ice cream, yogurt, and fruit juices. Not sterilization; heat-tolerant microbes survive.
Ultrahigh-temperature sterilization: 140ºC for 1 sec, then rapid cooling. Liquids can be stored at room temperature.
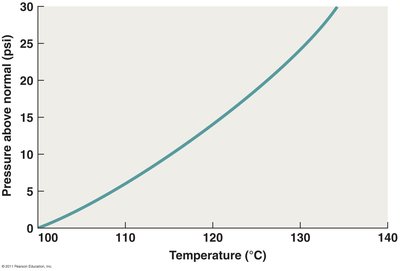
Dry Heat
Used for materials that cannot be sterilized with moist heat.
Denatures proteins and oxidizes chemicals.
Requires higher temperatures and longer times.
Incineration is the ultimate means of sterilization.
Refrigeration and Freezing
These methods decrease microbial metabolism, growth, and reproduction. Psychrophilic microbes can multiply in refrigerated foods, but most pathogens are halted.
Dessication and Lyophilization
Drying inhibits growth by removing water. Lyophilization (freeze-drying) is used for long-term preservation and prevents formation of damaging ice crystals.

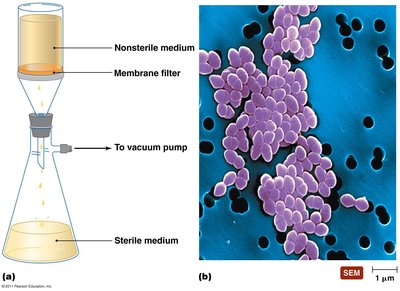
Filtration
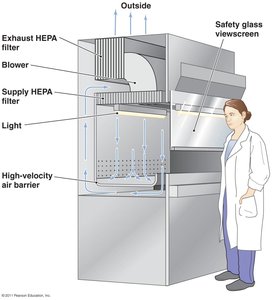
Filtration physically removes microbes from liquids and air. Membrane filters are used for sterilizing heat-sensitive solutions, and HEPA filters are used in biological safety cabinets.
Osmotic Pressure
High concentrations of salt or sugar inhibit microbial growth by causing cells to lose water. Fungi are more tolerant of hypertonic environments than bacteria.
Radiation
Ionizing Radiation
Wavelengths shorter than 1 nm (electron beams, gamma rays).
Creates ions that disrupt molecules and denature DNA.
Electron beams are effective but do not penetrate well; gamma rays penetrate but require longer exposure.

Nonionizing Radiation
Wavelengths greater than 1 nm (UV light).
Causes formation of pyrimidine dimers in DNA, affecting protein and nucleic acid structure.
Suitable for disinfecting air, transparent fluids, and surfaces.
Biosafety Levels
Laboratories are classified into four biosafety levels based on the pathogens handled:
BSL-1: Handling pathogens not causing disease in healthy humans.
BSL-2: Handling moderately hazardous agents.
BSL-3: Handling microbes in safety cabinets.
BSL-4: Handling microbes causing severe or fatal disease.

Chemical Methods of Microbial Control
Overview
Chemical agents affect cell walls, membranes, proteins, or DNA. Their effectiveness varies with environmental conditions and is often greater against enveloped viruses and vegetative cells.
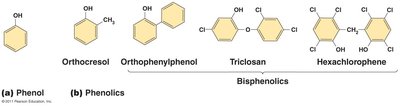
Phenol and Phenolics
Intermediate- to low-level disinfectants.
Denature proteins and disrupt membranes.
Effective in presence of organic matter; remain active for prolonged periods.
Commonly used in healthcare, labs, and homes.
Alcohols
Intermediate-level disinfectants.
Denature proteins and disrupt membranes.
More effective than soap for hand hygiene.
Used for skin preparation prior to injection.
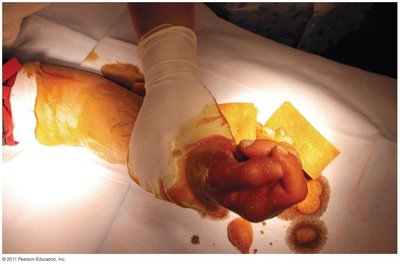
Halogens
Intermediate-level antimicrobial chemicals.
Damage enzymes via oxidation or denaturation.
Used in iodine tablets, chlorine treatment, bleach, and bromine disinfection.
Oxidizing Agents
Peroxides, ozone, and peracetic acid.
Kill by oxidation of microbial enzymes.
High-level disinfectants and antiseptics.
Hydrogen peroxide can disinfect surfaces but is not useful for open wounds due to catalase activity.
Ozone is used for water treatment; peracetic acid is a sporocide for equipment sterilization.
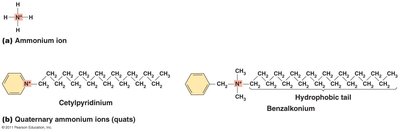
Surfactants
Reduce surface tension of solvents.
Soaps have hydrophilic and hydrophobic ends; good degerming agents but not antimicrobial.
Detergents are positively charged organic surfactants; quats are low-level disinfectants ideal for medical and industrial applications.
Heavy Metals
Denature proteins; low-level bacteriostatic and fungistatic agents.
1% silver nitrate prevents blindness from Neisseria gonorrhoeae.
Thimerosal preserves vaccines; copper controls algal growth.
Aldehydes
Compounds with terminal –CHO groups.
Cross-link functional groups to denature proteins and inactivate nucleic acids.
Glutaraldehyde disinfects and sterilizes; formalin is used in embalming and room disinfection.
Gaseous Agents
Microbicidal and sporicidal gases used in closed chambers.
Denature proteins and DNA by cross-linking functional groups.
Used in hospitals and dental offices; can be hazardous, explosive, poisonous, and potentially carcinogenic.
Enzymes
Antimicrobial enzymes act against microorganisms.
Lysozyme in human tears digests peptidoglycan cell wall.
Lysozyme reduces bacteria in cheese; prionzyme removes prions from medical instruments.
Antimicrobials
Includes antibiotics, semi-synthetic, and synthetic chemicals.
Typically used for disease treatment; some are used for microbial control outside the body.
Development of Resistant Microbes
Overuse of antiseptic and disinfectant products can promote the development of resistant microbes. There is little evidence that these products add to human or animal health.
