 Back
BackMicrobial Diseases of the Digestive System: Pathogenesis, Agents, and Clinical Features
Study Guide - Smart Notes

Infections of the Digestive System
Overview of the Digestive System
The digestive system is a complex organ system responsible for the breakdown and absorption of nutrients. It is composed of the gastrointestinal (GI) tract, which extends from the mouth to the anus, and accessory organs such as the liver, gallbladder, pancreas, and salivary glands. The GI tract is constantly exposed to microorganisms, making it a major site for infectious diseases. Approximately 70% of the immune system is located in the intestinal tract, primarily as gut-associated lymphoid tissue (GALT).
Major function: Digestion and absorption of nutrients
Accessory organs: Secrete digestive juices
Common route of infection: Fecal-oral transmission
Immune defense: GALT provides immune surveillance and response
Dental Diseases
Dental Caries (Cavities)
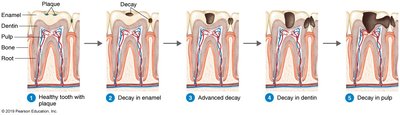
Dental caries are localized destruction of tooth enamel caused by bacterial metabolism. Streptococcus mutans metabolizes sucrose to produce lactic acid, which demineralizes enamel. The bacteria form a biofilm (plaque) composed of bacteria and dextran, a sticky polysaccharide. The biofilm protects bacteria and acid, allowing progressive decay.
Key agents: Streptococcus mutans (initiates caries), Lactobacillus (progresses caries)
Process: Plaque formation → acid production → enamel demineralization → dentin/pulp involvement
Periodontal Disease
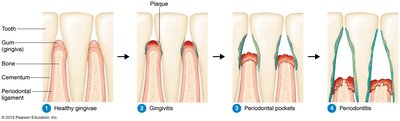
Periodontal diseases affect the supporting structures of the teeth. Gingivitis is inflammation of the gums, often progressing to periodontitis, where bone and tissue are destroyed, potentially leading to tooth loss. Porphyromonas gingivalis is a common causative agent.
Gingivitis: Gum inflammation and bleeding, reversible with oral hygiene
Periodontitis: Destruction of bone and connective tissue, formation of periodontal pockets, possible tooth loss
Bacterial Diseases of the Lower Digestive System
Types of GI Infections
Infections: Pathogen multiplies in GI tract; symptoms delayed, often with fever
Intoxications: Ingestion of preformed toxins; symptoms rapid, usually without fever
Common symptoms: Diarrhea, dysentery (bloody/mucous diarrhea), nausea, vomiting, abdominal cramps
Major concern: Diarrhea is a leading cause of infant mortality in developing countries; rehydration therapy is critical
Staphylococcal Food Poisoning
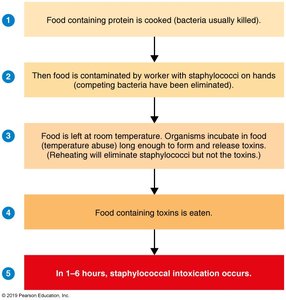
Caused by intoxication with enterotoxin produced by Staphylococcus aureus. The organism is heat- and salt-tolerant, and the toxin is heat-stable. Symptoms appear 1–6 hours after ingestion and include nausea, vomiting, abdominal cramps, and diarrhea, but usually no fever.
Transmission: Contamination of cooked food by handlers, followed by temperature abuse
Prevention: Proper refrigeration to prevent toxin formation
Shigellosis (Bacillary Dysentery)
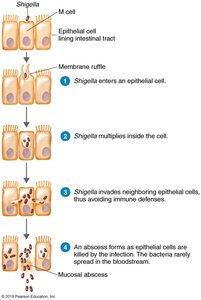
Shigellosis is caused by Shigella species and is characterized by severe, often bloody diarrhea. The bacteria invade M cells in the intestinal lining, multiply intracellularly, and spread to neighboring cells, evading immune defenses. Shiga toxin damages tissues, leading to mucosal abscesses.
Incubation: 12 hours to 2 weeks
Symptoms: Severe diarrhea, abdominal cramps, fever
Transmission: Person-to-person (no animal reservoir)
Salmonellosis
Caused by Salmonella spp., these bacteria invade the intestinal mucosa and can disseminate to other organs. Infection is commonly associated with contaminated poultry, eggs, and meats, as well as reptiles. Symptoms include abdominal pain, fever, and diarrhea, typically lasting 3–5 days.
Transmission: Ingestion of contaminated food or contact with reptiles
Shedding: Infected individuals may shed bacteria for months
Typhoid Fever
Caused by Salmonella Typhi, this severe systemic infection is transmitted only by humans. The bacteria multiply in phagocytes and spread to organs. Symptoms include high fever, headache, and later diarrhea. Chronic carriers may harbor the bacteria in the gallbladder.
Incubation: 2–3 weeks
Complications: Intestinal ulceration and perforation
Prevention: Vaccination for high-risk populations
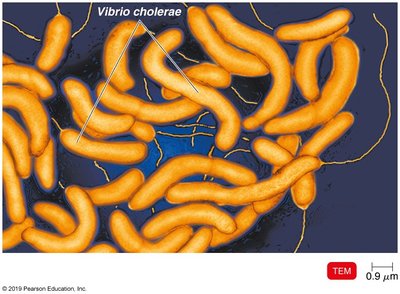
Cholera
Cholera, caused by Vibrio cholerae, is a life-threatening diarrheal disease. The cholera toxin induces massive secretion of electrolytes and water, resulting in 'rice water stools' and severe dehydration. Rapid fluid loss can lead to shock and death if untreated.
Reservoir: Brackish and fresh water
Symptoms: Profuse watery diarrhea, dehydration, thickened blood, organ damage
Treatment: Intravenous fluids are most effective; untreated mortality is high
Escherichia coli Gastroenteritis
Pathogenic E. coli Strains
While most Escherichia coli strains are harmless, some produce toxins that cause gastroenteritis. Enterohemorrhagic E. coli (EHEC), such as O157:H7, secrete Shiga-like toxins and can cause hemolytic uremic syndrome (HUS). Enteropathogenic (EPEC) and enterotoxigenic (ETEC) strains are major causes of diarrhea, especially in developing countries and travelers.
EHEC: Bloody diarrhea, HUS (kidney failure risk)
EPEC: Destroys microvilli, causes diarrhea in children
ETEC: Produces cholera-like toxin, causes traveler's diarrhea
Treatment: Oral rehydration; antibiotics in severe cases

Campylobacteriosis
Campylobacteriosis is the leading cause of bacterial diarrhea in the U.S., primarily caused by Campylobacter jejuni. Most cases are linked to contaminated poultry. Symptoms include fever, cramping, abdominal pain, and diarrhea. A rare complication is Guillain-Barré syndrome, an autoimmune condition causing temporary paralysis.
Transmission: Undercooked poultry, unpasteurized milk
Complication: Guillain-Barré syndrome (immune-mediated nerve damage)
Peptic Ulcer Disease
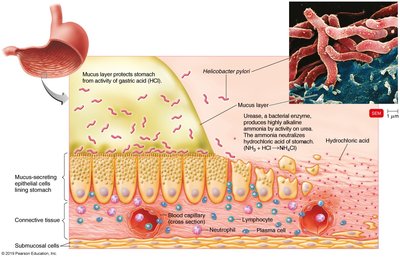
Peptic ulcers are primarily caused by Helicobacter pylori, which survives stomach acid by producing urease, converting urea to ammonia and raising local pH. Infection can lead to ulcers and, in some cases, gastric cancer. Type O blood individuals are more susceptible. Treatment includes antibiotics and bismuth compounds.
Mechanism: Urease production neutralizes stomach acid, allowing colonization
Complications: Ulcers, increased cancer risk
Treatment: Antibiotics, Pepto-Bismol
Clostridial Gastroenteritis
Clostridium perfringens Gastroenteritis
This common cause of gastroenteritis is associated with meat dishes. The bacteria grow in low-oxygen environments and produce exotoxins causing abdominal pain and diarrhea. Proper refrigeration prevents outbreaks.
Incubation: 8–12 hours
Prevention: Refrigerate cooked meats promptly
Clostridium difficile–Associated Diarrhea
Clostridium difficile is an opportunistic pathogen, often following antibiotic therapy. It produces exotoxins that cause mild diarrhea to severe colitis, which can progress to bowel perforation. It is a major cause of hospital-acquired infections.
Risk factor: Recent antibiotic use
Symptoms: Diarrhea, colitis, possible perforation
Viral Infections of the Digestive System
Rotavirus
Rotavirus is the most common cause of viral gastroenteritis in children. It is transmitted via the fecal-oral route and is highly infectious. Symptoms include low-grade fever, diarrhea, and vomiting. Vaccination is available.
Prevention: Vaccine
Treatment: Rehydration therapy
Norovirus
Noroviruses are non-enveloped, highly resistant viruses causing outbreaks of gastroenteritis. The infectious dose is extremely low, and symptoms include vomiting and diarrhea, usually self-limiting within 2–3 days.
Transmission: Fecal-oral
Treatment: Rehydration (IV if severe)
Mumps
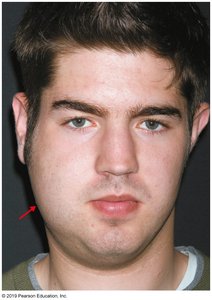
Mumps is a viral infection transmitted via saliva and respiratory droplets. The virus multiplies in the respiratory tract and spreads to organs such as the salivary glands, testes, ovaries, and pancreas. Complications include orchitis (inflammation of testes), meningitis, and pancreatitis. Vaccination (MMR) is effective prevention.
Symptoms: Parotitis (swelling of salivary glands), fever, dysphagia
Complications: Sterility, meningitis, pancreatitis
Hepatitis Viruses
Hepatitis A
Hepatitis A virus (HAV) is an RNA virus transmitted via the fecal-oral route. It causes acute liver inflammation, with symptoms such as anorexia, malaise, nausea, and jaundice. The virus is shed before symptoms appear, making outbreaks difficult to trace. Vaccination is available.
Incubation: 2–6 weeks
Prevention: Vaccine
Hepatitis B
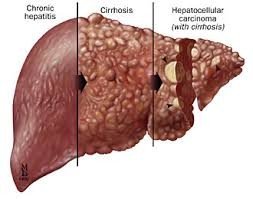
Hepatitis B virus (HBV) is a DNA virus transmitted through blood, sexual contact, or perinatally. Acute infection can progress to chronic hepatitis, cirrhosis, or liver cancer. Chronic carriers are at risk for long-term complications. Vaccination is effective prevention.
Symptoms: Fatigue, malaise, jaundice (acute); chronic infection may lack jaundice
Prevention: Vaccine, safe practices
Treatment: Alpha interferon for chronic cases
Hepatitis C
Hepatitis C virus (HCV) is a bloodborne RNA virus. It is often asymptomatic for decades but can lead to chronic hepatitis, cirrhosis, and liver cancer. There is no vaccine, but antiviral drug combinations are available for treatment.
Transmission: Bloodborne
Complications: Chronic hepatitis, cirrhosis, liver cancer
Fungal Diseases of the Digestive System
Mycotoxins
Certain fungi produce mycotoxins that can contaminate food. Claviceps purpurea causes ergot poisoning, which can lead to gangrene and hallucinations. Aspergillus flavus produces aflatoxin, a potent carcinogen found on peanuts and grains.
Ergot poisoning: Vasoconstriction, hallucinations
Aflatoxin: Liver cirrhosis, cancer risk


Protozoan Infections of the Digestive System
Giardiasis
Caused by Giardia intestinalis, giardiasis results in prolonged, foul-smelling diarrhea. Transmission is fecal-oral, often via contaminated water. The cysts are resistant to chlorine disinfection.
Symptoms: Smelly diarrhea, gas, prolonged illness
Prevention: Water filtration, boiling
Cryptosporidiosis
Caused by Cryptosporidium spp., this infection leads to diarrhea lasting 10–14 days. It is more severe in immunocompromised individuals. Cysts are chlorine-resistant.
Symptoms: Diarrhea, dehydration
Prevention: Water treatment, hygiene
Helminthic Infections of the Digestive System
Tapeworms
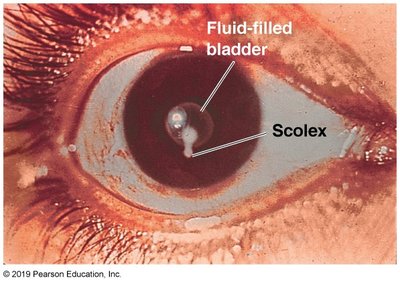
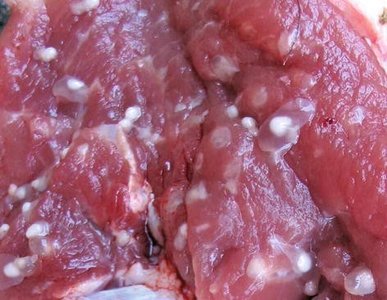
Tapeworms, mainly Taenia spp., have a life cycle involving humans and livestock. Humans ingest larvae in undercooked meat, which mature in the intestines. Eggs are shed in feces, continuing the cycle. Cysticercosis can occur if eggs are ingested, leading to larval cysts in tissues, including the eye and brain.
Transmission: Ingestion of undercooked meat containing cysticerci
Complications: Ophthalmic and neurocysticercosis
Hookworms
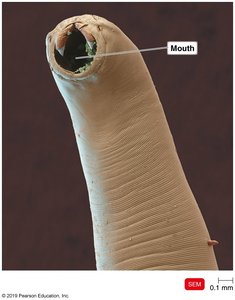
Hookworm infections are caused by several species and are acquired by direct contact with contaminated soil. The worms attach to the intestinal wall and feed on blood, causing anemia and fatigue. Improved sanitation and footwear reduce incidence.
Symptoms: Anemia, fatigue, pica (craving non-food substances)
Prevention: Sanitation, wearing shoes
Pinworms
Pinworm infection (Enterobius vermicularis) is common in children. Female worms lay eggs around the anus, causing itching. Diagnosis is by collecting eggs with tape and viewing under a microscope.
Symptoms: Perianal itching, disturbed sleep
Diagnosis: Tape test
