 Back
BackMicrobial Mechanisms of Pathogenicity: How Microbes Cause Disease
Study Guide - Smart Notes

Microbial Mechanisms of Pathogenicity
Overview of Pathogenicity
Pathogenicity refers to the ability of a microorganism to cause disease in a host organism. The process involves several steps, including entry into the host, evasion of host defenses, damage to host cells, and exit from the host to infect new individuals.
Portals of Entry: Microbes enter the host through specific routes such as mucous membranes, skin, or the parenteral route (direct deposition beneath the skin).
Penetration/Evasion of Host Defenses: Microbes use various mechanisms to avoid destruction by the host immune system.
Damage to Host Cells: Pathogens can damage host cells directly or through the production of toxins.
Portals of Exit: Microbes leave the host via routes similar to their entry, facilitating transmission to new hosts.
Portals of Entry
Mucous Membranes
Mucous membranes line body cavities open to the exterior and are common entry points for pathogens.
Respiratory tract: Easiest and most frequently used; e.g., Influenza, common cold viruses.
Gastrointestinal tract: Entry via contaminated food, water, or hands; e.g., Vibrio cholerae.
Genitourinary tract: Entry for most sexually transmitted diseases; e.g., Neisseria gonorrhoeae, Treponema pallidum.
Conjunctiva: Membrane covering the eyes; e.g., pathogens causing pink eye.
Skin
Unbroken skin is a formidable barrier, but some microbes can enter through hair follicles, sweat glands, or by direct penetration (e.g., hookworm, dermatophytes).
Parenteral Route
Microbes can be deposited directly into tissues beneath the skin or mucous membranes via punctures, bites, injections, or wounds.
Preferred Portal of Entry
Many pathogens must enter through a specific portal to cause disease. For example, Streptococcus pneumoniae causes pneumonia if inhaled but not if ingested.
Number of Invading Microbes
LD50 (Lethal Dose 50): Number of microbes required to kill 50% of test hosts.
ID50 (Infectious Dose 50): Number of microbes required to cause infection in 50% of test hosts.
Colonization and Adherence
Colonization
The first stage of infection is colonization, where pathogens establish themselves at the portal of entry, often at mucosal surfaces.
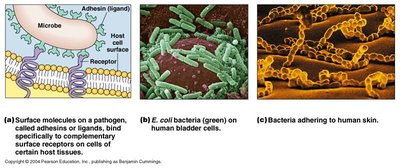
Adherence to Mucosal Surfaces
Bacterial adherence requires interaction between microbial adhesins (ligands) and host cell receptors (often carbohydrates or peptides).
Adhesins: Structures such as pili, fimbriae, capsules, or viral coat proteins that facilitate attachment.
Receptors: Specific molecules on host cells that bind adhesins.
Penetration or Evasion of Host Defenses
Capsules
Capsules are polysaccharide layers that protect bacteria from phagocytosis, increasing virulence (e.g., Streptococcus pneumoniae).
Cell Wall Components
M protein: Resists phagocytosis (Streptococcus pyogenes).
Opa protein: Inhibits T helper cells (Neisseria gonorrhoeae).
Mycolic acid: Waxy lipid that resists digestion (Mycobacterium tuberculosis).
Enzymes (Exoenzymes)
Pathogens produce enzymes that break down host defenses and tissues, aiding invasion and spread.
Leukocidins: Destroy phagocytic white blood cells.
Hemolysins: Lyse red blood cells.
Coagulases: Clot fibrinogen, protecting bacteria from immune attack.
Hyaluronidase: Digests connective tissue, aiding spread.
Necrotizing factors: Kill body cells.
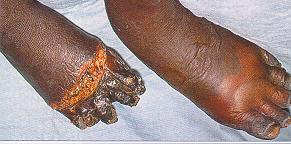
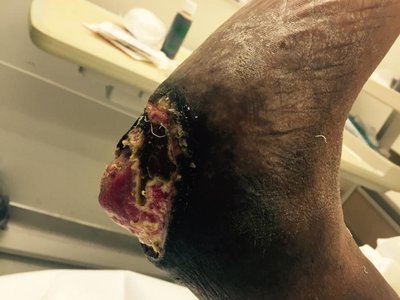
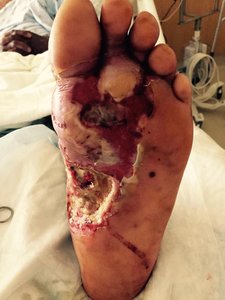
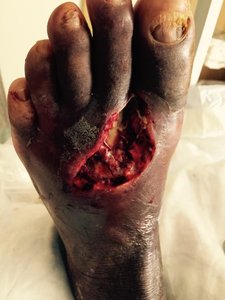
Invasins
Surface proteins that alter host cell actin, allowing bacteria to enter cells (e.g., Salmonella, E. coli).
Damage to Host Cells
Direct Damage
Pathogens can directly damage host cells by multiplying inside them or by triggering immune responses that harm host tissues.
Hypersensitivity Reactions
Excessive immune responses (e.g., anaphylaxis) can cause tissue damage.
Toxins
Overview of Toxins
Toxins are poisonous substances produced by microorganisms. They are classified as exotoxins (proteins, secreted) or endotoxins (lipid A of LPS, released upon cell lysis).
Toxigenicity: Ability to produce toxins.
Toxemia: Presence of toxins in the blood.
Toxoids: Inactivated toxins used for immunization.
Antitoxins: Antibodies against specific toxins.
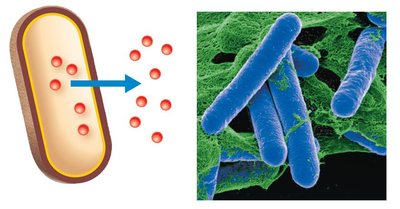
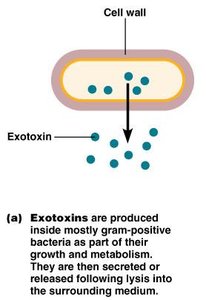
Exotoxins
Exotoxins are proteins secreted by mostly gram-positive bacteria. They are highly toxic, heat-sensitive, and can be neutralized by antitoxins.
Cytotoxins: Kill or damage host cells.
Neurotoxins: Interfere with nerve impulses.
Enterotoxins: Affect the gastrointestinal tract.
Types of Exotoxins
Type I (Superantigens): Overstimulate immune response, causing toxic shock (e.g., TSST-1 from Staphylococcus aureus).
Type II (Membrane-disrupting): Lyse host cells by disrupting membranes (e.g., hemolysins, leukocidins).
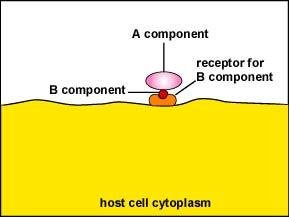
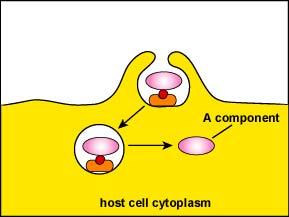
Type III (A-B Toxins): Consist of two parts: A (active) and B (binding). B binds to host cell, A enters and disrupts cell function.
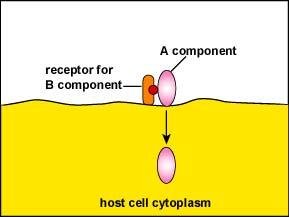
Important Exotoxins
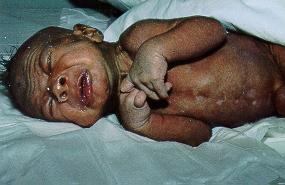
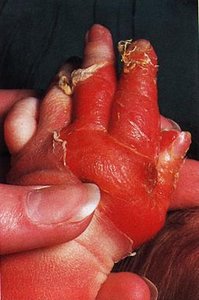
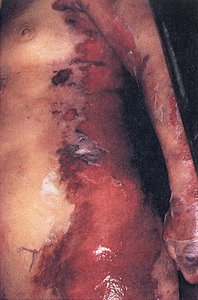
Botulinum toxin: Produced by Clostridium botulinum, causes flaccid paralysis.
Tetanus toxin: Produced by Clostridium tetani, causes muscle spasms.
Vibrio enterotoxin: Produced by Vibrio cholerae, causes massive fluid loss from intestinal cells.
Staphylococcal enterotoxin: Produced by Staphylococcus aureus, causes food poisoning and toxic shock syndrome.
Feature | Exotoxins | Endotoxins |
|---|---|---|
Source | Mostly Gram-positive | Gram-negative |
Chemistry | Protein | Lipid A (LPS) |
Fever? | No | Yes |
Neutralized by Antitoxin? | Yes | No |
LD50 | Small (very toxic) | Large (less toxic) |
Endotoxins
Endotoxins are part of the outer membrane of Gram-negative bacteria (Lipid A of LPS). They are released when bacteria die and the cell wall breaks apart. Endotoxins cause fever, shock, and other systemic effects.
Pyrogenic response: Induces fever by stimulating cytokine release from macrophages, which act on the hypothalamus.
Septic shock: Life-threatening drop in blood pressure due to endotoxin-induced cytokine release.
Detection: Limulus amoebocyte lysate (LAL) assay is used to detect endotoxins in medical equipment and pharmaceuticals.
Pathogenic Properties of Viruses
Mechanisms of Viral Pathogenicity
Viruses cause disease by invading host cells, evading immune responses, and damaging or killing host cells. They can hide from the immune system and attack immune cells directly.
Cytopathic Effects of Viruses
Cytopathic effects are visible changes in host cells due to viral infection. These effects can be cytocidal (cell death) or noncytocidal (cell damage without death).
Inhibition of macromolecular synthesis: Viruses can stop host cell DNA, RNA, or protein synthesis.
Release of lysosomal enzymes: Leads to cell death.
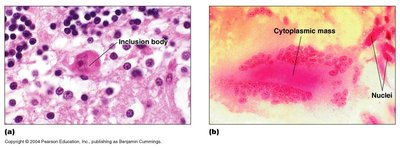
Inclusion bodies: Aggregates of viral or host cell components in the cytoplasm or nucleus, useful for diagnosis (e.g., rabies).
Formation of syncytia: Fusion of infected cells into giant cells (e.g., HIV, measles).
Metabolic changes: Altered hormone or protein production.
Cell-mediated immunity: Immune response can destroy infected cells, sometimes causing tissue damage.
Antigenic changes: Altered cell surface antigens lead to immune destruction.
Chromosomal changes: May include oncogene activation and transformation (loss of contact inhibition).
Portals of Exit
Pathogens exit the host via the same routes as entry, facilitating transmission to new hosts.
Respiratory tract: Coughing, sneezing
Gastrointestinal tract: Feces, saliva
Genitourinary tract: Urine, vaginal secretions
Skin
Blood: Biting arthropods, needles/syringes
