 Back
BackChapter 15_Microbial Mechanisms of Pathogenicity: Study Notes
Study Guide - Smart Notes

Microbial Mechanisms of Pathogenicity
Definitions and Key Concepts
Understanding how microbes cause disease is fundamental in microbiology. Pathogenicity is the ability of a microorganism to cause disease by overcoming host defenses, while virulence refers to the degree or extent of pathogenicity. Microbial toxins, such as exotoxins and endotoxins, play a crucial role in disease development.
Toxin: Substance that contributes to pathogenicity.
Toxigenicity: Ability to produce a toxin.
Toxemia: Presence of toxin in the host’s blood.
Toxoid: Inactivated toxin used in a vaccine.
Antitoxin: Antibodies against a specific toxin.
Mechanisms of Pathogenesis
For a microbe to cause disease, it must satisfy four conditions and have an exit strategy:
Gain entry into the host
Adhere and colonize (avoid dislodging/multiply in tissue)
Resist the defenses of the host
Invade and spread
Exit from host and survive (to regain entry)
Portals of Entry
Main Portals of Entry
Microbes enter the host through specific portals:
Mucous membranes: Respiratory, gastrointestinal, genitourinary tracts, conjunctiva
Skin: Through abrasions, wounds, hair follicles, sweat ducts
Parenteral route: Non-oral entry (e.g., intramuscular, subcutaneous, intravenous)
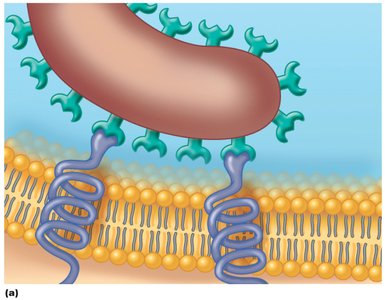
Adherence to Host Cells
Microbes use surface molecules called adhesins or ligands to bind specifically to complementary surface receptors on host cells. This interaction is highly specific and is essential for colonization.
Glycocalyx: Streptococcus mutans
Fimbriae: Escherichia coli
M protein: Streptococcus pyogenes
Biofilm formation further enhances adherence and colonization.
Virulence Factors
Cell Wall Components and Capsules
Microbial surface structures contribute to pathogenicity by resisting host defenses:
Capsules: Prevent phagocytosis (Klebsiella pneumoniae, Streptococcus pneumoniae)
M protein: Resists phagocytosis (Streptococcus pyogenes)
Opa protein: Inhibits T helper cells (Neisseria gonorrhoeae)
Mycolic acid: Resists digestion (Mycobacterium tuberculosis)
Antigenic Variation
Microbes can alter their surface antigens to evade the immune system. This process, known as antigenic variation, is seen in viruses (e.g., influenza) and bacteria (e.g., Borrelia recurrentis).
Enzymes as Virulence Factors
Bacterial enzymes facilitate invasion and spread by degrading host tissues:
Coagulases: Clot fibrinogen in plasma, protecting bacteria from phagocytosis
Kinases: Digest fibrin clots, allowing spread
Hyaluronidase: Degrades hyaluronic acid, aiding tissue penetration
Collagenase: Digests collagen, facilitating spread through connective tissue
IgA proteases: Destroy IgA antibodies
Penetration into Host Cell Cytoskeleton
Some bacteria use invasins to rearrange actin filaments of the host cell cytoskeleton, facilitating entry and movement within and between cells (e.g., Salmonella, Listeria).
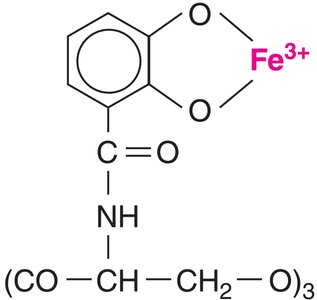
Using Host Nutrients: Siderophores
Bacteria secrete siderophores to scavenge iron from host iron-binding proteins, which is essential for their growth and survival.
Host Damage and Toxins
Direct Damage
Bacteria can cause direct damage by multiplying inside host cells, disrupting cell function, and producing waste products.
Bacterial Toxins
Bacterial toxins are classified as exotoxins and endotoxins:
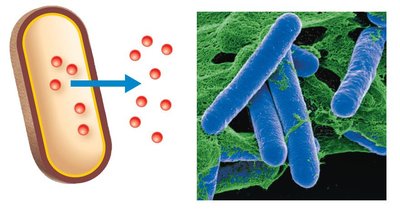
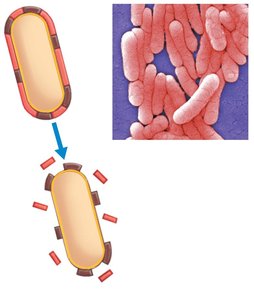
Exotoxins: Secreted proteins, highly toxic, heat labile, produced mainly by Gram-positive bacteria
Endotoxins: Lipid A component of LPS in Gram-negative bacteria, released upon cell death, heat stable
Exotoxin Types and Mechanisms
A-B toxins: Consist of an active (A) and binding (B) component; the A component alters cell function, often by inhibiting protein synthesis
Membrane-disrupting toxins: Cause cell lysis by disrupting plasma membranes
Superantigens: Trigger excessive immune response by binding to MHC II and T cells, causing massive cytokine release
Exotoxin Classification
Diphtheria toxin: A-B toxin
Botulinum toxin: A-B neurotoxin
Tetanus toxin: A-B neurotoxin
Vibrio enterotoxin: A-B enterotoxin
Staphylococcal enterotoxin: Superantigen
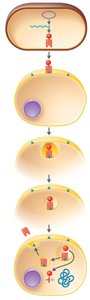
Lysogeny and Pathogenicity
Some bacteria acquire toxin genes via lysogenic conversion, where a bacteriophage integrates its DNA into the bacterial genome, conferring new virulence properties.
Endotoxins and the Pyrogenic Response
Mechanism of Endotoxin Action
Endotoxins stimulate macrophages to release cytokines (IL-1, TNF-α), which travel to the hypothalamus and induce fever by triggering prostaglandin production.
Comparison of Exotoxins and Endotoxins
Property | Exotoxin | Endotoxin |
|---|---|---|
Source | Mostly Gram-positive | Gram-negative |
Relation to Microbe | By-products of growing cell | Outer membrane |
Chemistry | Protein | Lipid A |
Fever? | No | Yes |
Neutralized by Antitoxin? | Yes | No |
LD50 | Small | Relatively large |
Pathogenic Properties of Other Infectious Agents
Fungi
Fungal waste products may cause symptoms
Chronic infections provoke allergic responses
Trichothecene toxins inhibit protein synthesis (Fusarium)
Proteases (Candida, Trichophyton)
Capsule prevents phagocytosis (Cryptococcus)
Ergot toxin (Claviceps purpurea), aflatoxin (Aspergillus), neurotoxins (phalloidin, amanitin)
Protozoa
Waste products cause symptoms
Evade host defenses by growing in phagocytes (Toxoplasma) and antigenic variation (Giardia, Trypanosoma)
Helminths
Use host tissue and interfere with host function
Metabolic waste causes symptoms (e.g., elephantiasis by Wuchereria bancrofti)
Algae
Produce neurotoxins (e.g., saxitoxin from dinoflagellates causing paralytic shellfish poisoning)
Portals of Exit
Portal of Exit
Microbes exit the host through the same portals as entry: mucous membranes, skin, parenteral route. This is essential for transmission and survival.
Summary Diagram: Microbial Pathogenicity
The balance between host and microbe determines infection outcome. Mechanisms include portals of entry, penetration/evasion of host defenses, damage to host cells, and portals of exit.
Nosocomial Infections: MRSA
MRSA (Methicillin Resistant Staphylococcus aureus)
Causes life-threatening necrotizing illness due to leucocidin toxin
Resistance to methicillin and vancomycin
USA100 MRSA: 92% infections in healthcare
USA300 MRSA: 89% infections in community
Acquisition of vanA gene from Enterococcus species
