 Back
BackMicrobial Mechanisms of Pathogenicity: Study Notes
Study Guide - Smart Notes

Microbial Mechanisms of Pathogenicity
Pathogenicity and Virulence
Pathogenicity refers to the ability of a microorganism to cause disease, while virulence describes the degree of pathogenicity. Understanding these concepts is fundamental to microbiology and infectious disease.
Pathogenicity: The capacity of a microbe to cause disease in a host.
Virulence: The relative severity or harmfulness of a pathogen.
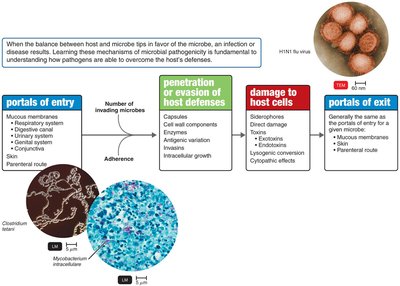
Portals of Entry
Microorganisms must enter the host through specific portals to initiate infection. Most pathogens have a preferred portal of entry.
Mucous membranes: Includes respiratory tract (most common), digestive canal, genitourinary system, and conjunctiva.
Skin: Usually impenetrable unless through hair follicles or sweat gland ducts.
Parenteral route: Direct deposition into tissues via punctures, injections, bites, cuts, wounds, or surgery.
Numbers of Invading Microbes: ID50 and LD50
The number of microbes required to cause infection or death is measured by ID50 and LD50.
ID50: Infectious dose for 50% of a sample population; measures virulence.
LD50: Lethal dose for 50% of a sample population; measures toxin potency.
Example: Bacillus anthracis has different ID50 values depending on the portal of entry.
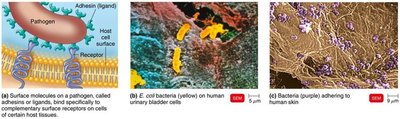
Adherence
Adherence is the process by which pathogens attach to host tissues, a critical step in infection.
Adhesins (ligands): Molecules on pathogens that bind to host cell receptors.
Examples: Glycocalyx of Streptococcus mutans (adheres to teeth), fimbriae of Actinomyces, viral spikes (e.g., SARS-CoV-2 binding to ACE2).
Penetration or Evasion of Host Defenses
Pathogens employ various strategies to evade host defenses and establish infection.
Capsules: Glycocalyx layer impairs phagocytosis (e.g., Streptococcus pneumoniae).
Cell wall components: M protein (resists phagocytosis), Opa protein (attachment), mycolic acid (resists digestion).
Enzymes: Coagulases (coagulate fibrinogen), kinases (digest fibrin clots), hyaluronidase (digests hyaluronic acid), collagenase (breaks down collagen), IgA proteases (destroy IgA antibodies).
Antigenic variation: Pathogens alter surface antigens to evade immune response (e.g., influenza virus).
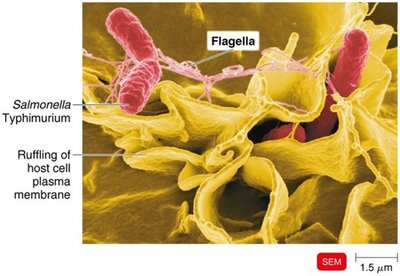
Invasins: Surface proteins that rearrange actin filaments, causing membrane ruffling and bacterial entry (e.g., Salmonella).
Biofilms: Bacterial communities resistant to antibiotics and phagocytosis.
How Bacterial Pathogens Damage Host Cells
Bacterial pathogens damage host cells through nutrient acquisition, direct damage, and toxin production.
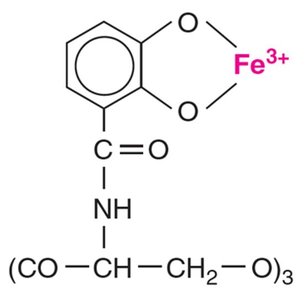
Siderophores: Proteins that bind iron more tightly than host proteins, facilitating iron acquisition.
Direct damage: Disruption of host cell function, nutrient use, waste production, and cell rupture.
Toxins: Poisonous substances causing fever, shock, and other symptoms.
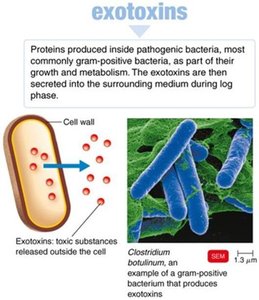
Exotoxins
Exotoxins are proteins secreted by bacteria, often highly specific and potent.
Antitoxins: Antibodies against exotoxins.
Toxoids: Inactivated exotoxins used in vaccines.
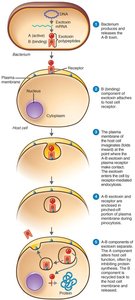
A-B toxins: Consist of an active (A) and binding (B) component (e.g., diphtheria toxin).
Membrane-disrupting toxins: Lyse host cells (e.g., hemolysins).
Superantigens: Cause intense immune response via cytokine release.
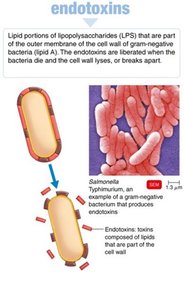
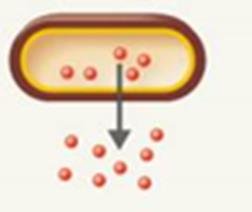
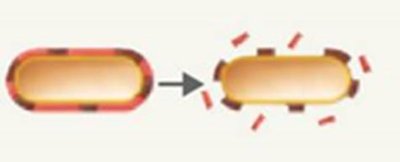
Endotoxins
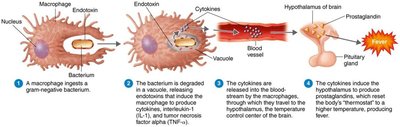
Endotoxins are lipid A components of lipopolysaccharides (LPS) in gram-negative bacteria, released upon cell death.
Effects: Fever, shock, disseminated intravascular coagulation, weakening of blood-brain barrier.
LAL assay: Detects endotoxins using horseshoe crab blood.
Comparison of Exotoxins and Endotoxins
Exotoxins and endotoxins differ in their source, chemistry, effects, and immunological properties.
Property | Exotoxins | Endotoxins |
|---|---|---|
Bacterial Source | Gram-positive and gram-negative | Gram-negative |
Chemistry | Proteins (A-B structure) | Lipid A (LPS) |
Heat Stability | Unstable (destroyed at 60-80°C) | Stable (withstands autoclaving) |
Toxicity | High | Low |
Fever-Producing | No | Yes |
Immunology | Can be neutralized by antitoxin | Not easily neutralized |
Lethal Dose | Small | Large |
Representative Diseases | Tetanus, botulism, diphtheria | Typhoid fever, meningitis |
Plasmids, Lysogeny, and Pathogenicity
Plasmids and lysogenic conversion contribute to microbial pathogenicity by encoding virulence factors and toxins.
Plasmids: Carry genes for toxins, antibiotic resistance, and enzymes.
Lysogenic conversion: Incorporation of prophage genes alters microbial characteristics (e.g., diphtheria toxin).
Pathogenic Properties of Viruses
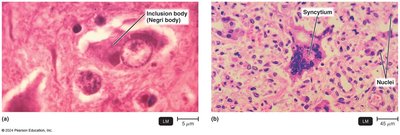
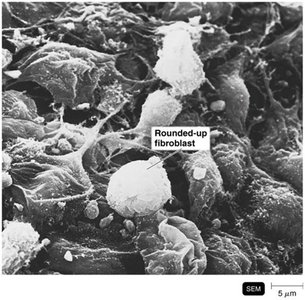
Viruses cause disease through cytopathic effects (CPE), which are visible changes in host cells.
Cytocidal effects: Kill host cells.
Noncytocidal effects: Cause cell damage without death.
Examples: Inclusion bodies (Negri bodies in rabies), syncytium formation (measles), transformation (cancer).
Interferons: Alpha and beta interferons protect neighboring cells from viral infection.
Virus (Genus) | Cytopathic Effect |
|---|---|
Poliovirus (Enterovirus C) | Cytocidal (cell death) |
Genital warts virus (Alphapapillomavirus) | Acidophilic inclusion bodies in nucleus, transformation |
Adenovirus (Mastadenovirus) | Basophilic inclusion bodies in nucleus |
Rabies (Lyssavirus) | Acidophilic inclusion bodies in cytoplasm |
CMV (Cytomegalovirus) | Acidophilic inclusion bodies in nucleus and cytoplasm |
Measles virus (Morbillivirus) | Cell fusion |
HIV (Lentivirus) | Destruction of T cells |
SARS-CoV-2 (Betacoronavirus) | Syncytia, cilia shrinkage, altered junctions |
Pathogenic Properties of Fungi, Protozoa, Helminths, and Algae
These eukaryotic pathogens cause disease through toxins, tissue damage, and immune evasion.
Fungi: Produce toxic metabolites, provoke allergies, inhibit protein synthesis, and prevent phagocytosis with capsules.
Protozoa: Cause symptoms via waste products, digest host cells, grow in phagocytes, and undergo antigenic variation.
Helminths: Use host tissue for growth, produce large masses, and release waste products causing symptoms.
Algae: Some produce neurotoxins (e.g., saxitoxin) causing paralytic shellfish poisoning.
Portals of Exit
Microorganisms exit the host through specific portals, often the same as their entry points.
Respiratory tract: Coughing and sneezing.
Gastrointestinal tract: Feces and saliva.
Genitourinary tract: Urine and genital secretions.
Skin
Blood: Via arthropod bites or needles.
 Additional info: These notes expand on brief points with academic context, definitions, and examples to ensure completeness and clarity for exam preparation.
Additional info: These notes expand on brief points with academic context, definitions, and examples to ensure completeness and clarity for exam preparation.
