 Back
BackMicrobial Mechanisms of Pathogenicity: Study Notes
Study Guide - Smart Notes

Microbial Mechanisms of Pathogenicity
Portals of Entry
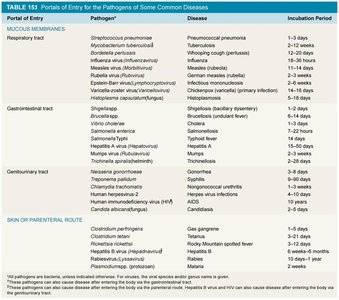
Pathogens must enter the host through specific portals to initiate infection. The main portals of entry include mucous membranes, skin, and parenteral routes. Each portal is associated with particular pathogens and diseases, and the incubation period varies depending on the organism and route.
Mucous Membranes: Includes respiratory, gastrointestinal, and genitourinary tracts. Common diseases: pneumonia, tuberculosis, influenza, cholera, salmonella, STIs.
Skin: Some pathogens grow on unbroken skin or enter through conjunctiva.
Parenteral Route: Entry via punctures, wounds, injections. Diseases: hepatitis, rabies, tetanus, malaria.
Portal of Entry | Pathogen | Disease | Incubation Period |
|---|---|---|---|
Respiratory tract | Streptococcus pneumoniae | Pneumococcal pneumonia | 1–3 days |
Gastrointestinal tract | Vibrio cholerae | Cholera | 2–3 days |
Genitourinary tract | Neisseria gonorrhoeae | Gonorrhea | 2–7 days |
Skin/Parenteral | Clostridium tetani | Tetanus | 1–5 days |
Skin/Parenteral | Plasmodium spp. | Malaria | 7–30 days |
Additional info: | See image_1 for a detailed table of pathogens, diseases, and incubation periods. | ||
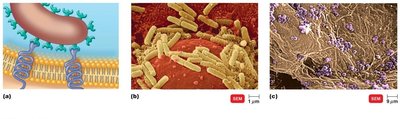
Adherence
Adherence is the process by which pathogens attach to host tissues. This is a critical step in pathogenesis, as it allows microbes to colonize and resist removal by host defenses.
Adhesins (ligands): Surface molecules on pathogens that bind to specific receptors on host cells.
Structures involved: Glycocalyx, fimbriae, and formation of biofilms.
Biofilms: Communities of microbes that share nutrients and are resistant to immune responses.
Penetration of Host Defenses
Bacterial pathogens employ various strategies to penetrate or evade host defenses, including capsules, cell wall components, enzymes, antigenic variation, and penetration into host cells.
Capsules: Glycocalyx layer impairs phagocytosis (e.g., Streptococcus pneumoniae).
Cell Wall Components: M protein in Streptococcus pyogenes increases attachment; mycolic acid in Mycobacterium resists digestion.
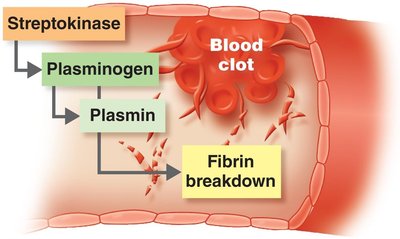
Enzymes: Coagulases, kinases, hyaluronidase, collagenase, and IgA proteases facilitate invasion and spread.
Antigenic Variation: Pathogens alter surface antigens to evade immune detection (e.g., influenza, gonorrhea).
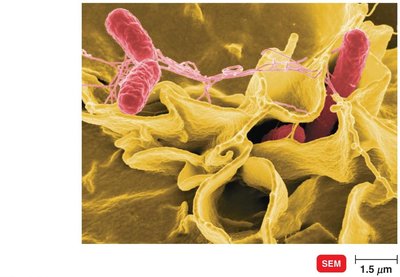
Penetration into Host Cells: Invasins rearrange actin filaments, causing membrane ruffling and facilitating entry (e.g., Salmonella).
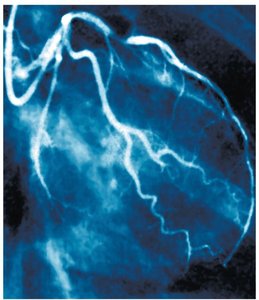
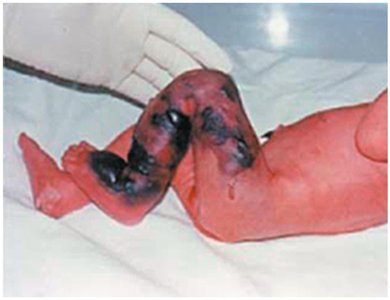
Damage to Host Cells
Pathogens damage host cells by using host nutrients, causing direct damage, producing toxins, and inducing hypersensitivity reactions.
Siderophores: Proteins that bind iron more tightly than host molecules, depriving host cells of essential iron.
Direct Damage: Disruption of host cell function, nutrient usage, waste production, and cell rupture.
Toxins: Poisonous substances that cause fever, shock, and other symptoms. Includes exotoxins and endotoxins.
Exotoxins
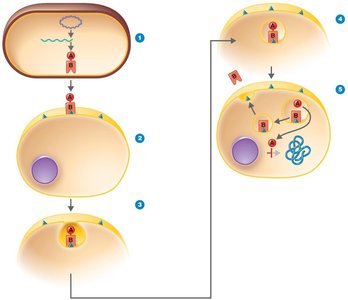
Exotoxins are proteins secreted by bacteria, often highly specific and potent. Types include A-B toxins, membrane-disrupting toxins, superantigens, and genotoxins.
A-B Toxins: Consist of an active (A) component and a binding (B) component. Example: diphtheria toxin.
Membrane-Disrupting Toxins: Lyse host cells by disrupting plasma membranes (e.g., hemolysins).
Superantigens: Cause intense immune responses by stimulating T cells.
Genotoxins: Damage DNA, leading to mutations and cancer.
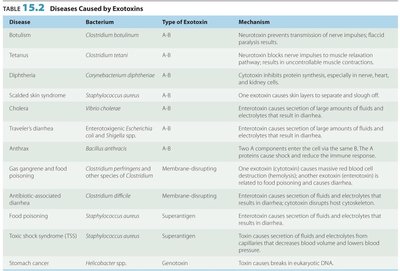
Disease | Bacterium | Type of Exotoxin | Mechanism |
|---|---|---|---|
Botulism | Clostridium botulinum | A-B | Neurotoxin prevents transmission of nerve impulses; flaccid paralysis results. |
Tetanus | Clostridium tetani | A-B | Neurotoxin blocks nerve impulses to muscle relaxation; muscle spasms result. |
Diphtheria | Corynebacterium diphtheriae | A-B | Cytotoxin inhibits protein synthesis, especially in nerve, heart, and kidney cells. |
Additional info: | See image_10 for more diseases caused by exotoxins. | ||
Endotoxins
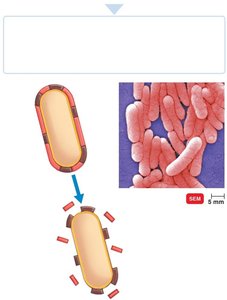
Endotoxins are lipid components of the outer membrane of gram-negative bacteria, released upon cell lysis. They cause general symptoms such as fever, weakness, and shock.
Lipid A: The toxic component of lipopolysaccharides (LPS).
Release: Occurs during bacterial multiplication or death.
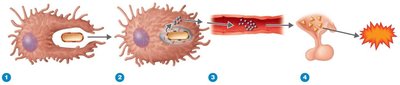
Effects: Stimulate cytokine release, cause disseminated intravascular coagulation.
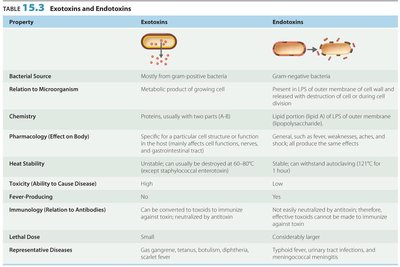
Property | Exotoxins | Endotoxins |
|---|---|---|
Bacterial Source | Mostly gram-positive | Gram-negative |
Relation to Microorganism | Metabolic product | Part of cell wall |
Chemistry | Proteins, usually A-B | Lipid (LPS) |
Pharmacology | Specific effects | General effects |
Heat Stability | Unstable | Stable |
Toxicity | High | Low |
Fever-Producing | No | Yes |
Immunology | Can be converted to toxoids | Not easily neutralized |
Lethal Dose | Small | Large |
Representative Diseases | Gas gangrene, tetanus, botulism, diphtheria, scarlet fever | Typhoid fever, urinary tract infections, meningococcal meningitis |
Pathogenic Properties of Viruses
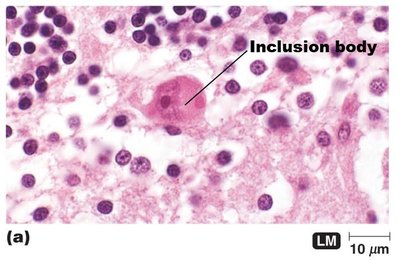
Viruses cause disease by evading host defenses and inducing cytopathic effects (CPEs). CPEs are visible changes in host cells due to viral infection.
Cytocidal Effects: Cell death.
Noncyticidal Effects: Cell damage without death.
Examples of CPEs: Stopping cell synthesis, lysosome release, inclusion bodies, syncytium formation, chromosomal changes, antigenic changes, loss of contact inhibition, blocking interferons.
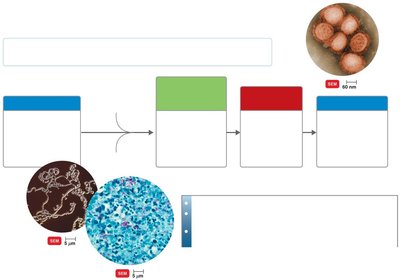
Pathogenic Properties of Fungi, Protozoa, Helminths, and Algae
These organisms cause disease through toxic products, allergic responses, and tissue damage.
Fungi: Produce toxins (e.g., aflatoxin, ergot), provoke allergies, and resist phagocytosis.
Protozoa: Cause symptoms via waste products, digest host cells, antigenic variation.
Helminths: Use host tissue for growth, produce masses, and cause cellular damage.
Algae: Some produce neurotoxins (e.g., saxitoxin).
Portals of Exit
Pathogens exit the host through specific portals, often the same as their entry points. This is essential for transmission to new hosts.
Respiratory tract: Coughing, sneezing.
Gastrointestinal tract: Feces, saliva.
Genitourinary tract: Urine, genital secretions.
Skin: Direct contact.
Blood: Arthropod bites, needles.
Key Concepts
Several factors are required for a microbe to cause disease: entry, adherence, penetration/evasion, and damage.
Pathogens usually leave the body via specific portals of exit, which are generally the same sites as entry.
