 Back
BackMicrobiology Study Guide: Infectious Disease, Epidemiology, Host-Microbe Interactions, and Immunity
Study Guide - Smart Notes

Disease Terminology and Epidemiology
Basic Concepts in Infectious Disease and Epidemiology
Understanding infectious disease and epidemiology is fundamental to microbiology. Infectious diseases are illnesses caused by pathogens, while epidemiology involves monitoring and controlling disease occurrence to promote public health.
Pathogens: Include prions, viruses, bacteria, protozoans, helminths, and fungi.
Opportunistic pathogens: Cause disease only when the host is weakened.
True pathogens: Cause disease in healthy hosts.
Sporadic cases: Isolated infections in a population.
Endemic infections: Routinely detected in a population or region.
Epidemic: Widespread outbreak in a region during a specific time frame.
Pandemic: Epidemic that spreads to numerous countries.
Emerging pathogens: Newly identified or expanding pathogens.
Reemerging pathogens: Previously controlled agents resurfacing.
Zoonotic diseases: Spread from animals to humans; many are noncommunicable.
Communicable diseases: Transmit from human to human.
Contagious diseases: Easily transmitted between hosts.
Signs: Objective indicators (e.g., fever, rash).
Symptoms: Subjective experiences (e.g., pain, fatigue).
Latent infections: Asymptomatic periods.
Acute diseases: Rapid onset and progression.
Chronic diseases: Slower onset and progression.
Koch’s Postulates and Their Limitations
Koch’s postulates are a set of criteria used to establish the causative relationship between a microbe and a disease. They have been instrumental in identifying pathogens but have limitations.
Koch’s Postulates:
The same organism must be present in every case of the disease.
The organism must be isolated and grown as a pure culture.
The isolated organism should cause disease when inoculated into a susceptible host.
The organism must be re-isolated from the inoculated, diseased animal.
Limitations: Not applicable to noninfectious diseases, obligate intracellular pathogens, latent diseases, or pathogens that do not infect nonhuman hosts.
Sources and Transmission of Pathogens
Pathogens originate from various sources and are transmitted through multiple modes. Reservoirs are habitats where pathogens are naturally found, while sources disseminate pathogens to new hosts.
Endogenous source: Pathogen originates from the host’s own body.
Exogenous source: Pathogen is external to the host.
Transmission modes: Person-to-person, animal, environment, vertical (mother to child), airborne, vehicle (fomites, food, water), vector (biological and mechanical).
Stages of Infectious Disease
General Stages of Disease Progression
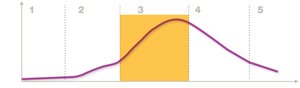
Infectious diseases progress through five general stages, each characterized by specific pathogen levels and symptoms.
Incubation period: Time between infection and earliest symptoms.
Prodromal phase: Early symptoms develop.
Acute phase: Peak of disease.
Period of decline: Replication is controlled; symptoms resolve.
Convalescent phase: Recovery; pathogen may remain latent.
Epidemiology Essentials
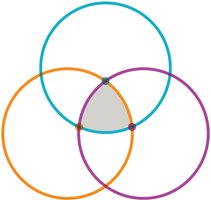
The Epidemiological Triangle
The epidemiological triangle links the host, etiological agent, and environment, providing a framework for understanding disease dynamics.
Host factors: General health, sex, lifestyle, age, ethnicity, occupation.
Etiological agent: Fungi, bacteria, virus, parasite, or prion.
Environmental factors: Climate, geographic location, vector availability, water and food sources.
Public Health Strategies
Strategies to break the epidemiological triangle include public education, quarantine, and vector control.
Hand washing, avoiding intravenous drug use, and drinking clean water are personal habits that lower risk.
Preventing disease in vulnerable populations (babies, elderly, organ transplant recipients) is crucial.
Host–Microbe Interactions and Pathogenesis
Host–Microbe Dynamics
Host–microbe interactions are complex and not always harmful. Normal microbiota colonize various body sites and interact with the immune system.
Dysbiosis: Disruption of microbiota balance.
Opportunistic pathogens: Cause disease under certain circumstances.
Tropism: Pathogen preference for specific host tissues.
Pathogenicity and Virulence
Pathogenicity is the ability of a microbe to cause disease, while virulence describes the degree of disease caused. Virulence factors help pathogens overcome host defenses.
Virulence factors: Mechanisms for adhesion, invasion, immune evasion, and nutrient acquisition.
Damage host cells directly or provoke dangerous immune responses.

Five Steps to Infection
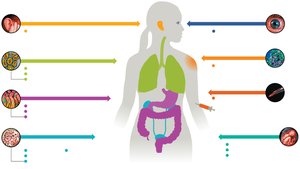
To establish infection, pathogens must complete five tasks: enter the host, adhere to tissues, invade and obtain nutrients, replicate while evading immune defenses, and transmit to a new host.
Portals of entry: Respiratory mucosa, skin, ocular, transplacental, parenteral, urogenital, GI mucosa, otic.
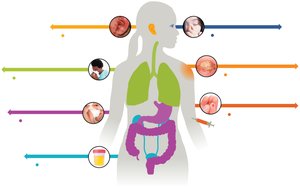
Portals of Exit
Pathogens exit the host through specific routes, often the same as their entry portals. Transmission is facilitated by symptoms such as sneezing, coughing, and diarrhea.
Portals of exit: Feces, urine, blood, wound drainage, saliva, mucus, semen.
Innate Immunity
Classification of Immune Responses
The immune system is divided into innate and adaptive branches. Both recognize pathogens, eliminate invaders, and discriminate self from foreign antigens.
Innate immunity: Inborn, nonspecific, generalized responses.
Adaptive immunity: Specific, matures over time, exhibits memory, requires days to activate.
First-Line Defenses
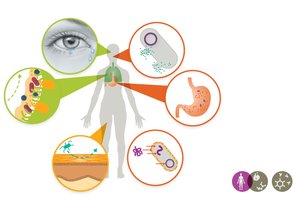
First-line defenses prevent pathogen entry and are categorized as mechanical, chemical, and physical barriers.
Mechanical barriers: Flushing, rinsing, trapping (e.g., tears, urine, saliva, mucus membranes).
Chemical barriers: Molecules that attack microbes or create hostile environments (e.g., lysozyme, stomach acid, fatty acids).
Physical barriers: Structures that block entry (e.g., skin, mucociliary escalator).
Leukocytes and Lymphoid Tissues
Leukocytes are essential for immune responses. Primary lymphoid tissues produce and mature leukocytes, while secondary tissues filter lymph and sample antigens.
Primary lymphoid tissues: Thymus, bone marrow.
Secondary lymphoid tissues: Lymph nodes, spleen, MALT.
Types of Leukocytes
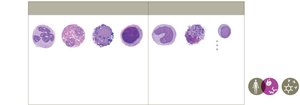
Leukocytes are classified as granulocytes or agranulocytes, each with distinct functions in immunity.
Granulocytes: Neutrophils, eosinophils, basophils, mast cells.
Agranulocytes: Monocytes, dendritic cells, lymphocytes (NK cells, B cells, T cells).
Cytokines and Complement System
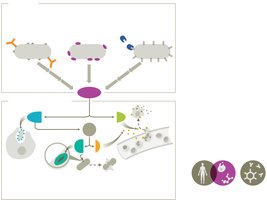
Cytokines are signaling proteins that coordinate immune actions. The complement system is a cascade of proteins that enhances immune responses.
Cytokine storm: Exaggerated response causing tissue damage.
Complement outcomes: Opsonization, inflammation, cytolysis.
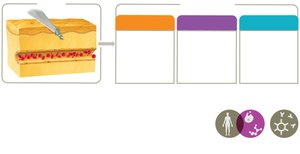
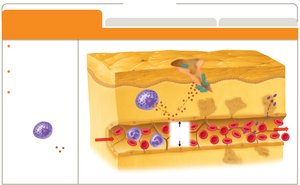
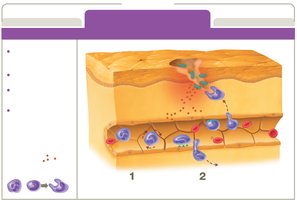
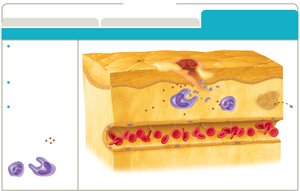
Inflammation
Inflammation is a key innate response to tissue injury, with three main goals: recruit immune defenses, limit pathogen spread, and promote tissue recovery.
Phases: Vascular changes, leukocyte recruitment, resolution.
Fever
Fever is a systemic innate response that enhances antiviral effects, increases phagocyte efficiency, limits pathogen growth, and promotes tissue repair.
Immune System Disorders
Primary and Secondary Immune Deficiencies
Immune deficiencies can be primary (genetic) or secondary (acquired). Primary deficiencies affect immune factors from birth, while secondary deficiencies result from aging, disease, or medical interventions.
Primary immunodeficiencies: Selective IgA/IgG deficiencies, SCID, DiGeorge syndrome.
Secondary immunodeficiencies: Caused by age, infectious agents, medical interventions, systemic disorders.
Autoimmunity and Hypersensitivities
Autoimmunity is an attack against self-tissues, leading to chronic disorders. Hypersensitivities are inappropriate immune responses classified into four types (ACID mnemonic).
Type I (Allergy): IgE mediated, can lead to anaphylaxis.
Type II (Cytotoxic): IgG/IgM mediated, involves cell lysis.
Type III (Immune Complex): IgG/IgM complexes lodge in tissues.
Type IV (Delayed): T cell mediated, delayed response.
Transfusion Compatibility and Rh Factor
Blood typing prevents transfusion reactions. Rh incompatibility during pregnancy can lead to hemolytic disease of the newborn.
Rh– mother exposed to Rh+ fetus: Maternal IgG antibodies attack fetal red blood cells.
Transplant Rejection and Graft Types
Transplant rejection occurs if T cells detect foreign tissue. Grafts are classified as autografts, isografts, allografts, or xenografts. Immune-privileged sites are least likely to be rejected.
Graft-versus-host disease: Occurs in bone marrow transplants; graft attacks host tissues.
Diagnosing Allergies and Hypersensitivities
Allergy diagnosis involves blood tests for IgE titers and skin tests. Hypersensitivity reactions are classified using the Gell and Coombs system.
Summary Table: Types of Hypersensitivity Reactions
Type | Mechanism | Examples |
|---|---|---|
I (Allergy) | IgE mediated | Anaphylaxis, hay fever |
II (Cytotoxic) | IgG/IgM mediated, cell lysis | Hemolytic anemia, transfusion reactions |
III (Immune Complex) | IgG/IgM complexes | Lupus, rheumatoid arthritis |
IV (Delayed) | T cell mediated | Type I diabetes, transplant rejection |
Key Equations
Lethal Dose-50 (LD50): Amount of toxin needed to kill 50% of affected hosts.
Infectious Dose-50 (ID50): Number of cells or virions needed to establish infection in 50% of exposed hosts.
Additional info: Academic context and expanded explanations were added to ensure completeness and clarity for exam preparation.
